Atrophic glossitis: An often-overlooked oral condition
Atrophic glossitis (AG) is an often-overlooked oral condition affecting up to 10% of the population. It’s characterized by the partial or complete absence of filiform and fungiform papillae on the dorsal surface of the tongue.1 This results in a smooth, red tongue with a diminished ability to taste. It is more prevalent in older adults and people with underlying medical conditions.2,3 Oral care professionals need to be aware of the signs and symptoms of AG so it can be diagnosed and treated promptly. An early diagnosis and treatment can help to prevent serious health consequences and improve oral health.
Why it’s important to know about AG
AG can indicate nutritional deficiencies, such as vitamin B12, iron, and zinc. These deficiencies can have serious health consequences, so it's important to address them promptly.
Second, atrophic glossitis can complicate certain medical conditions, such as Sjögren's syndrome, celiac disease, and diabetes. Identifying atrophic glossitis may lead to the diagnosis of an underlying medical condition that would otherwise go undetected.
You might also be interested in: Conditions of the tongue that may suggest a more serious systemic story
Third, AG can make eating and speaking difficult if symptomatic, leading to weight loss, malnutrition, and social isolation.
Finally, it can increase the risk of developing other oral health problems, such as candidiasis and leukoplakia.
Classification of atrophic glossitis
AG can be classified based on its underlying cause:
- Nutritional atrophic glossitis: caused by a vitamin B12, iron, vitamin B2, vitamin B3, vitamin B6, folic acid, iron, zinc, and vitamin E deficiency4
- Hyposalivation-associated atrophic glossitis5
- Candidiasis-associated atrophic glossitis
- Medication-induced atrophic glossitis: caused by certain medications, such as chemotherapy drugs and radiation therapy
- Systemic disease-associated atrophic glossitis: caused by underlying medical conditions such as diabetes mellitus, HIV/AIDS, and autoimmune diseases6
- Idiopathic atrophic glossitis: cause of unknown origin
Pathogenesis
Its exact pathogenesis has yet to be fully understood. However, it is thought that the loss of filiform and fungiform papillae is due to a combination of factors that will cause a decreased production of keratin, with an increased inflammation of the tongue mucosa that, in some cases, may allow the overgrowth of Candida albicans.7,8
Clinical signs and symptoms
A smooth, red tongue is the most common clinical sign of atrophic glossitis. The tongue may also be dry and sore. In some cases, patients may also experience a burning sensation in the mouth or difficulty tasting food.
Evaluation and treatment
The diagnosis of atrophic glossitis is based on a clinical tongue examination. The dentist or oral pathologist may also order blood tests to check for vitamin B12, iron, and folate deficiencies.
Treatment of atrophic glossitis depends on the underlying cause. If a vitamin B12 deficiency causes the condition, treatment involves administering vitamin B12 supplements. If the condition is caused by xerostomia, treatment may involve using artificial saliva or other measures to increase salivary production. If it’s caused by candidiasis, treatment involves antifungal medications.
Prognosis and complications
The prognosis for atrophic glossitis is generally good. The tongue papillae can often regrow with appropriate treatment, and the condition can improve. However, the tongue papillae may sometimes not regrow completely, and the condition may persist.
In rare cases, atrophic glossitis can lead to complications such as difficulty eating and swallowing and a higher risk of Infection.
Differential diagnosis
The differential diagnosis for atrophic glossitis includes other conditions that can cause a smooth, red tongue, such as candidiasis, geographic tongue, lichen planus, pemphigus vulgaris, and squamous cell carcinoma of the tongue.
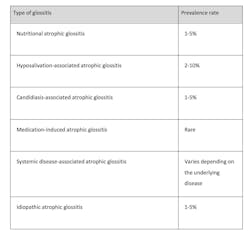
Click for a comparison chart of different types of glossitis and their prevalence rate
Conclusion
Atrophic glossitis is a common condition caused by various factors. The condition is characterized by a smooth, red tongue with a diminished ability to taste. Treatment of atrophic glossitis depends on the underlying cause, but in most cases, the condition can be improved with appropriate treatment.
References
- Chiang CP, Chang JY, Wang YP, Wu YH, Wu YC, Sun A. Atrophic glossitis: etiology, serum autoantibodies, anemia, hematinic deficiencies, hyperhomocysteinemia, and management. J Formos Med Assoc. 2020;119(4):774-780. doi:10.1016/j.jfma.2019.04.015
- Chi AC, Neville BW, Krayer JW, Gonsalves WC. Oral manifestations of systemic disease. Am Fam Physician. 2010;82(11):1381-1388.
- Reamy BV, Derby R, Bunt CW. Common tongue conditions in primary care. Am Fam Physician. 2010;81(5):627-634
- Chen GY, Tang ZQ, Bao ZX. Vitamin B12 deficiency may play an etiological role in atrophic glossitis and its grading: a clinical case-control study. BMC Oral Health. 2022;22(1):456. doi:10.1186/s12903-022-02464-z
- Pellicano R. Is chronic atrophic gastritis the missing link between atrophic glossitis, gastric parietal cell antibody positivity and hematological deficiencies? J Formos Med Assoc. 2020;119(5):1004-1005. doi:10.1016/j.jfma.2020.01.003
- Nakamura S, Okamoto MR, Yamamoto K, et al. The Candida species that are important for the development of atrophic glossitis in xerostomia patients. BMC Oral Health. 2017;17(1):153. doi:10.1186/s12903-017-0449-3
- Li C, Wu Y, Xie Y, et al. Oral manifestations serve as potential signs of ulcerative colitis: a review. Front Immunol. 2022;13:1013900. doi:10.3389/fimmu.2022.1013900
- R AN, Rafiq NB. Candidiasis. In: StatPearls [Internet]. StatPearls Publishing; 2023.
About the Author

Andreina Sucre, MSc, RDH
Andreina Sucre, MSc, RDH, is an international dentist, oral pathology, and oral surgery specialist practicing dental hygiene in Miami, Florida. A passionate advocate for early pathological diagnosis, she empowers colleagues through lectures focused on oral pathologies. Andreina is the founder of The Patho RDH, a published author for RDH magazine, and a selected speaker at RDH Under One Roof 2026. Committed to community outreach, she educates non-native English-speaking children on oral health and actively volunteers in dental initiatives.