Comparing surgical and pharmacological interventions for trigeminal neuralgia pain
Trigeminal neuralgia is a chronic and debilitating condition.1 It is characterized by severe, stabbing, and recurrent pain, lasting from some seconds to many minutes.1-6 Studies show that many of these patients have episodes of spontaneous pain that have a short duration.2,6 The pain clears up between attacks, and it does not happen when a person is asleep.2
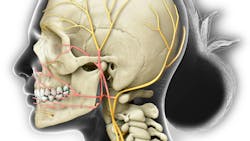
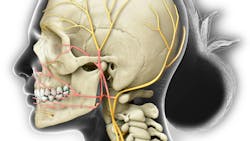
This condition affects one or more branches of the trigeminal nerve, and it is the most common neuralgia.2,3,6 There are usually two varieties: type 1 (intermittent pain) and type 2 (constant pain).2 It is often classified as classical or idiopathic, meaning that there is no known cause of the symptoms.2
Neurovascular conflict is the most accepted etiological theory.2 This theory states that an artery or vein is compressing the trigeminal nerve, which injures the myelin sheath and causes hyperactive function of the nerve.2 The consequences of demyelination are that it can cause increased electrical hyperexcitability in the trigeminal nerve.2 Also peripheral pathologies at the root, other dysfunctions of the brain stem, and intracranial lesions can cause trigeminal neuralgia.1,2 The Gasserian ganglion, from where the trigeminal nerve separates, can undergo structural and biochemical changes, which contribute to demyelination and axonal degeneration, thereby causing discomfort.2
It is estimated that the yearly incidence of trigeminal neuralgia is 12.6 per 100,000 persons per year.1 This condition commonly happens after the age of 50, and it is uncommon in young adults.1,2,5 It is more common in females; however, some data shows that 60% of patients with trigeminal neuralgia are female.1,2,5 It is also commonly unilateral, affecting one side of the face.1
Trigeminal neuralgia can often be implicated in dentistry because it causes extreme pain in the jaw, lips, and face.2-5 Patients can feel sharp stabbing pains in the mouth, which can be brought on by chewing, speaking, or brushing teeth.7 It can be challenging to treat patients with trigeminal neuralgia.7 A simple touch can make the nerve fire off and cause pain; also, there can be specific trigger points or zones that may be in the same division of the trigeminal nerve.7 The condition can be mistaken for tooth pain.7
The purpose of this review is to evaluate current treatments for Trigeminal neuralgia and determine if one is more effective than the other. This literature review asks the following research question: In patients with trigeminal neuralgia, are surgical interventions compared with pharmacological treatment more effective in decreasing pain symptoms?
Effective surgical treatments
To treat trigeminal neuralgia, there are many different forms of surgical options. They include gamma knife surgery, percutaneous balloon compression, glycerol rhizotomy, peripheral nerve section, partial sensory root section, microvascular decompression, endoscopic vascular decompression, internal neurolysis, percutaneous trigeminal radiofrequency thermocoagulation, and coblation.2, 7, 11-14 The following treatments are effective in different studies.
Gamma knife surgery, which is also known as stereotactic radiosurgery, is a noninvasive technique.5,6 It uses a focused beam of radiation at the trigeminal root in the posterior fossa.5,6 This technique uses radiation to block nerve conduction, which leads to less pain.3 It is reported that initial pain relief is 77-96%, with long-term results from this surgery leading to 50%.2,15
Percutaneous balloon compression is a surgical procedure that penetrates the foramen ovale and then uses the compression of a balloon that is inflated into Meckle’s cave.6 This procedure avoids injury to the corneal reflex, and it is reported that it is used in patients with multiple sclerosis and significant medical comorbidities. 1 Studies show that this safe and simple method gives patients 90% of pain relief.2,5
Glycerol rhizotomy is another type of procedure that enters the foramen ovale and then uses a chemical injection of glycerol thereby killing the nerve fibers.6 Studies show the immediate success rate of this procedure is 95%, with a 50-60% recurrence in two years.2
The peripheral nerve section procedure is a surgery distal to the Gasserian ganglia, and it blocks or destroys portions of the trigeminal nerve.6,15 With this procedure, it has been reported that 90% of patients receive relief from pain.3 In one year, 68-85% are pain-free, and at three years, it drops to 54-64%.2,6 Other studies show 50% recurrence after one year.5
One of the most common surgical procedures is microvascular decompression.5 This is a major neurosurgical procedure that involves craniotomy.5 It is often described as the most effective treatment for early and continuing pain control.10 Vessels that compress the trigeminal nerve are located and then moved to avoid contact with the trigeminal nerve.5,7,16 This procedure is indicated in patients with type 1 and type 2 forms of trigeminal neuralgia.2 Microvascular decompression is acceptable for elderly patients in suitable health for this procedure.10
It is reported that this method has better results than gamma knife surgery because it provides higher pain relief, and the most extended duration of pain freedom.2,6,10 Studies report that the early outcome of this surgery is typically 90-95%, which drops to 75% at 5-year follow-up.2,4,6 It is reported that 18-34% of patients have a recurrence of pain.6
Endoscopic vascular decompression is a type of surgery that is minimally invasive.2 This technique allows better visualization during the procedure.2 This procedure identifies new nerve-vessel conflicts in 7.5%-33% of cases.2 Studies claim that this procedure is safe, improves pain relief, and the complications are lower when compared to microvascular decompression.2
Effective pharmacological treatments
Many different medications are recommended to help patients find relief from their symptoms including carbamazepine, oxcarbazepine, topiramate, subcutaneous sumatriptan, lidocaine and local anesthetics, clonazepam, gabapentin, phenytoin, tizanidine, topical capsaicin, valproate, baclofen, lamotigene, and pimozide.3,6,17
Carbamazepine is one of the most common medications used for trigeminal neuralgia.1,6 It is a sodium channel blocker which keeps voltage-gated sodium channels in an inactive state.6,18 Carbamazepine has been established as a first-line treatment, and it is also an anticonvulsant5,8,19, 20 Anticonvulsants are effective in acting on the neurons that are repeatedly firing, effecting the networks, action of neurotransmitters, and effecting neuronal ionic transport.3
Carbamazepine studies have shown significant improvement in pain intensity, spontaneous attacks, and prevention of triggers, which precede the attacks.1,3 Studies show that it is effective in 75% of patients under long term treatment.1 However, it has poor tolerability and side effects.6 Side effects include drowsiness, dizziness, nausea, headache, vomiting, abdominal cramps, dysuria, tinnitus, and vertigo.3,18,20-22 Some studies have shown effectiveness when carbamazepine has been combined with other medications such as baclofen, gabapentin, pregabalin, lamotrigine, clonazepam, sodium valproate, phenytoin sodium, or opiates.1,7,23 However a study showed that when carbamazepine was combined with baclofen, it was most effective in reducing pain than compared with carbamazepine alone.8, 24
Oxcarbazepine is another sodium channel blocker and an anticonvulsant.3,6 It is a second-line treatment.3 It is at times chosen over carbamazepine because it is more easily tolerated and it has fewer side effects.5,7,23 Studies show that 88% of the patients taking oxcarbazepine had a reduction in pain attacks by more than 50%.7
Gabapentin is another medication used to treat trigeminal neuralgia, its effectiveness has been reported in several studies.25 It is also a second-line treatment, anticonvulsant, and GABA receptor agonist.3,25 A GABA receptor agonist inhibits excitatory neurotransmitters from being released, thereby inhibiting pain.25 Studies have shown good response in 71.4% of patients after 15 days when the patient is taking 900mg/day.25 One hundred percent of patients reported good response in 3 months after the dose was increased to 1800mg/day.25
Gabapentin has many advantages. It does not interact with other drugs, does not cause skin reactions, and it has mild side effects.25 The side effects include mild somnolence, dizziness, headache, nausea, and edema in the ankles.25 The appeal of these mild side effects is that it makes gabapentin a safer drug for elderly patients to take.25 Compared with carbamazepine, gabapentin is well-tolerated and doesn’t have serious side effects.25 One study suggested that gabapentin is effective as a first- or second-line treatment because of its ability to be more tolerable.25 It also suggested that gabapentin would be effective in resistant cases of trigeminal neuralgia that do not respond favorably to other treatments.25
Comparing surgical and pharmacological options
Medical and surgical treatment options are available to patients and help alleviate their symptoms.1Treatment with medications is considered simple whereas surgical treatment is considered as being more complex.1 Additionally, surgical options may be limited depending on the location.23 Typically, the first line of treatment is pharmacological options, whereas surgery is offered when medication options have been exhausted.1,18
Several medications that are prescribed for trigeminal neuralgia are sodium channel blockers.1,3 As stated before, the benefit of sodium channel blockers is that they keep the voltage-gated sodium channel in an inactivated state.18 These medications have been shown to significantly lower pain intensity.3
Carbamazepine is considered the gold standard when treating patients.9 This medication is also the most studied and the drug of choice for symptoms.1,18,19,21,25 At times, carbamazepine has to be combined with other drugs to increase effectiveness and alleviate pain.8 Additionally, carbamazepine is an anticonvulsant drug, but other anticonvulsant drugs are readily available.2 However, many of these medications cause side effects, making it hard for patients to carry out day-to-day tasks. The side effects of medications that are used to treat trigeminal neuralgia include drowsiness, dizziness, nausea, headache, vomiting, abdominal cramps, dysuria, tinnitus, and vertigo.3,18,20-22 This can pose a more significant concern for those that are elderly due to issues of balance and side effects.6 Because of these side effects, patients may be unable to tolerate taking these different medications.
When patients cannot tolerate medications or do not respond to these medications, then surgery is recommended.1,6,7 Several surgical options are available, and these treatments have a high success rate.14 Most patients that have had surgery would have preferred to have it earlier.1 Microvascular decompression is a mainstay of treatment.11 Studies have shown that this surgical procedure has the most extended duration of pain freedom and the highest pain relief.2, 6, 10,11 The outcomes for classic trigeminal neuralgia relief after microvascular decompression are impressive at 83.5-96.7%, with no recurrence with long term follow up.4 This procedure is performed beneath a microscope, and Teflon is placed to relieve nerve compression.4 Another study presented that neurosurgical treatment offers better long-term control of pain.17 The same study showed that 70% of patients who had microvascular decompression were pain-free after 19 years of treatment.17 Microvascular decompression is recommended in younger patients and healthy elderly.2
Many surgeries are safe, simple, and effective.2. However surgical options have some side effects. When undergoing different surgical procedures, there is the risk of sensory disturbances and hypaesthesia.5 Depending on where the surgery is, a patient can have lasting numbness, sensory loss, trauma, and complications.1,2,12 However, as stated before, most patients that have surgery would have preferred to have it earlier.1
Conclusion
Medications and surgical treatments are both recommended for Trigeminal Neuralgia patients. They both have their benefits and also have side effects. Medications are chosen first because they are readily available. However, when patients are unable to tolerate different medications, then surgical options are available. Many patients have said that they would have preferred to have surgery earlier. This being said, the option to treat with surgery first, should be offered to patients. Some patients fear surgery and would benefit from a proactive approach of patient education to inform them of what safe surgical interventions are available. However, no studies have shown that surgery is more effective than medication. Thus, the conclusion is that more research needs to be done on this topic to determine if surgical treatments are more effective than pharmacological options. Further research will allow clinicians and patients to make the best decision when choosing a treatment that is most effective.
Editor's note: This article appeared in the March 2024 print edition of RDH magazine. Dental hygienists in North America are eligible for a complimentary print subscription. Sign up here.
References
- Yadav S, Mittal HC, Sachdeva A, Verma A, Dhupar V, Dhupar A. A retrospective study of 72 cases diagnosed with idiopathic trigeminal neuralgia in Indian populace. J Clin Exp Dent. 2015;7(1):e40-e44. doi:10.4317/jced.51771
- Yadav YR, Nishtha Y, Sonjjay P, Vijay P, Shailendra R, Yatin K. Trigeminal neuralgia. Asian J Neurosurg. 2017;12(4):585-597. doi:10.4103/ajns.AJNS_67_14
- Peterson-Houle GM, AbdelFattah MR, Padilla M, Enciso R. Efficacy of medications in adult patients with trigeminal neuralgia compared to placebo intervention: a systematic review with meta-analyses. J Dent Anesth Pain Med. 2021;21(5):379-396. doi:10.17245/jdapm.2021.21.5.379
- Wu A, Doshi T, Hung A, et al. Immediate and long-term outcomes of microvascular decompression for mixed trigeminal neuralgia. World Neurosurg. 2018;117:e300-e307. doi:10.1016/j.wneu.2018.06.016
- Rashid A, Pintea B, Kinfe TM, Surber G, Hamm K, Boström JP. LINAC stereotactic radiosurgery for trigeminal neuralgia-retrospective two-institutional examination of treatment outcomes. Radiat Oncol. 2018;13(1):153. doi:10.1186/s13014-018-1102-2
- Cruccu G, Gronseth G, Alsksne J, et al. AAN-EFNS guidelines on trigeminal neuralgia management. Eur J Neurol. 2008;15(10)1013-1028. doi:10.1111/j.1468-1331.2008.02185.x
- Jainkittivong A, Aneksuk V, Langlais RP. Trigeminal neuralgia: a retrospective study of 188 Thai cases. Gerodontology. 2012; 29(2):e611-e617. doi:10.1111/j.1741-2358.2011.00530.x
- Puri N, Rathore A, Dharmdeep G, et al. A clinical study on comparative evaluation of the effectiveness of carbamazepine and combination of carbamazepine with baclofen or capsaicin in the management of trigeminal neuralgia. Niger J Surg. 2018;24(2):95-99. doi:10.4103/njs.NJS_8_18
- Zakrzewska JM, Akram H. Neurosurgical interventions for the treatment of classical trigeminal neuralgia. Cochrane Database Syst Rev. 2011;2011(9):CD007312. doi:10.1002/14651858.CD007312.pub2
- Amagasaki K, Watanabe S, Naemura K, Shono N, Nakaguchi H. Safety of microvascular decompression for elderly patients with trigeminal neuralgia. Clin Neurol Neurosurg. 2016;141:77-81. doi:10.1016/j.clineuro.2015.12.019
- Ko AL, Ozpinar A, Lee A, Raslan AM, McCartney S, Burchiel KJ. Long-term efficacy and safety of internal neurolysis for trigeminal neuralgia without neurovascular compression. J Neurosurg. 2015;122(5):1048-1057. doi:10.3171/2014.12.JNS14469
- Lin Y, Ni J, Zuo X, et al. Efficacy of coblation versus radiofrequency thermocoagulation for the clinical treatment of trigeminal neuralgia. Wideochir Inne Tech Maloinwazyjne. 2020;15(4):620-624. doi:10.5114/wiitm.2020.92409
- Wei Y, Zhao W, Pu C, et al. Clinical features and long-term surgical outcome in 39 patients with tumor-related trigeminal neuralgia compared with 360 patients with idiopathic trigeminal neuralgia. Br J Neurosurg. 2017; 31(1):101-106. doi:10.1080/02688697.2016.1233321
- Heinskou TB, Maarbjerg S, Wolfram F, et al. Favourable prognosis of trigeminal neuralgia when enrolled in a multidisciplinary management program – a two-year prospective real-life study. J Headache Pain. 2019;20(1):23. doi:10.1186/s10194-019-0973-4
- Albano L, Agosta F, Basaia S, et al. Alterations of brain structural MRI are associated with outcome of surgical treatment in trigeminal neuralgia. Eur J Neurol. 2022; 29:305-317. doi:10.1111/ene.15105
- Guo H, Song G, Wang X, Bao Y. Surgical treatment of trigeminal neuralgia with no neurovascular compression: a retrospective study and literature review. J Clin Neurosci. 2018;58:42-48. doi:10.1016/j.jocn.2018.10.066
- Ibrahim S. Trigeminal neuralgia: diagnostic criteria, clinical aspects and treatment outcomes. A retrospective study. Gerodontology. 2014;31(2):89-94. doi:10.1111/ger.12011
- Tariq R, Janjua OS, Mehmood S, Khalid MU, Zafar KJ, Hameed S. Comparison of effectiveness of carbamazepine versus topiramate for the management of trigeminal neuralgia. Pakistan Armed Forces Med J. 2021;71(4):1360-13633.
- Ayele BA, Mengesha AT, Zewde YZ. Clinical characteristics and associated factors of trigeminal neuralgia: experience from Addis Ababa, Ethiopia. BMC Oral Health. 2020; 20(1):244. doi:10.1186/s12903-020-01227-y
- Sathasivam HP, Ahmad AR, Hin LS. A retrospective study of the clinical characteristics of Malaysian trigeminal neuralgia (TGN) patients seen at the Oral Medicine Clinic, Kuala Lumpur general hospital. Malaysian Dent J. 2012;34(1):8-12.
- Besi E, Boniface DR, Cregg R, Zakrzewska JM. Comparison of tolerability and adverse symptoms in oxcarbazepine and carbamazepine in the treatment of trigeminal neuralgia and neuralgiform headaches using the Liverpool Adverse Events Profile (AEP). J Headache Pain. 2015;16:563. doi:10.1186/s10194-015-0563-z.
- Coats RO, Crossley KL, Conlin N, et al. Cognitive and sensorimotor function in participants being treated for trigeminal neuralgia pain. J Headache Pain. 2020;21(1):91. doi:10.1186/s10194-020-01156-9
- Ariyawardana A, Pallegama R, Sitheeque M, Ranasinghe A. Use of single- and multi-drug regimens in the management of classic (idiopathic) trigeminal neuralgia: an 11-year experience at a single Sri Lankan institution. J Investig Clin Dent. 2012;3(2):98-102. doi:10.1111/j.2041-1626.2011.00109.x
- Danyluk H, Andrews J, Kesarwani R, et al. The thalamus in trigeminal neuralgia: structural and metabolic abnormalities, and influence on surgical response. BMC Neurol. 2021;21(1):290. doi:10.1186/s12883-021-02323-4
- Kaur B, Dhir P. Evaluation of the efficacy of carbamazepine and gabapentin in the management of trigeminal neuralgia: a clinical study. J Indian Acad Oral Med Radiol. 2018;30(3):253.
Sheila Britten, BSDH, RDH, has been a dental hygienist for over 17 years. She first started as a dental assistant in 1997. Wanting to have more one-on-one time with patients, she decided to attend dental hygiene school. She graduated from hygiene school in 2006, and finished her bachelor’s degree in 2022. She practices dental hygiene four days a week and enjoys volunteering and writing in her spare time.
About the Author

Sheila Britten, BSDH, RDH
Sheila Britten, BSDH, RDH, has been a dental hygienist for over 17 years. She first started as a dental assistant in 1997. Wanting to have more one on one time with patients, she decided to attend dental hygiene school. She graduated from hygiene school in 2006, and finished her bachelor’s degree in 2022. She practices dental hygiene four days a week and enjoys volunteering and writing in her spare time.