Careful questioning of patients to determine the origin of a burn
Since changes in oral tissues occur over time, patients may not even be aware of them until a dental professional notices or the pain becomes extreme enough that patients seek assistance. Careful questions will elicit answers that lead you closer to learning the origin of oral tissue irritations, burns, and chemical injuries.
Determining a specific cause of redness, whiteness, taste alteration, vesicles, or pigmentation can be a daunting task for a clinician. The art of questioning patients about dental products used, foods consumed, and lifestyle practices is not straightforward in most cases. Patients often do not remember what they consumed yesterday or the day before. Changes in the oral tissues occur over time, and patients may not even realize that changes are present until they are either noticed by a dental professional or become painful, causing patients to seek assistance. Sometimes, patients take it upon themselves to solve their pain issue by using over-the-counter products to self-medicate.
The offenders of changes in oral tissue may be dental products, food products, or self-induced irritation from devices, suicide attempts, the persistence of chronic habits, or perhaps recreational drugs (cocaine). The list of common products involved in tissue changes is long, and includes dental products, foods, mechanical devices, chemicals in household products, and medications. Hydrogen peroxide, silver nitrate, phenol, endodontic materials, and certain medications are known to promote tissue damage. Gasoline, turpentine, rubbing alcohol, and eugenol have been reported to cause injuries to the oral tissues as well.1
To assist in a clinical assessment, a recent article by researchers resulted in an algorithm for the treatment of intraoral burns, citing that there is no standard of care for guidelines specific to intraoral burns.2 Burns are divided into four categories: thermogenic, cryogenic, chemical, and electrical.2 The algorithm, based on the GRADE system (used to grade the strength of recommendations), is designed to assist the clinician toward a path that will address a net benefit, quality of evidence, values, and preferences as well as the cost of an action. The chemical burn is divided into two paths: one for acid-induced and one for alkali-induced causes. In cases when there is significant destruction of tissue, further steps in treatment would be needed, such as surgical debridement and antibiotics to assist in more rapid recovery.
The four scenarios listed below have been documented for some time and known to cause irritation to the oral tissues or worse. Many reports exist, but sometimes these causes are not recognized as problems or they are forgotten as possibilities unless a careful assessment is made.
Aspirin burns
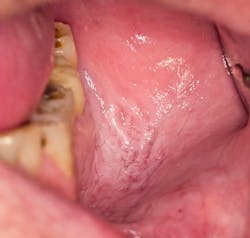
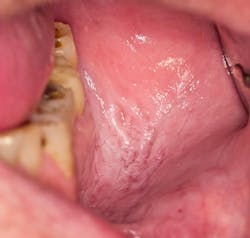
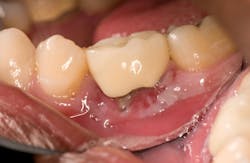
A long-held belief that patients may practice is to place an aspirin tablet directly on the tooth to relieve tooth pain. Patients may also crush an aspirin tablet and apply it directly on the tissue next to the affected tooth. The result is depicted in Figure 1. Patients may not divulge this practice to the clinician unless specifically asked about it.1,3
Garlic burns
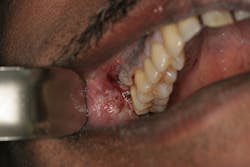
In many cases, the clinician may not even consider asking about the use of crushed garlic. A case of a 49-year-old Middle Eastern man presented seeking care for pain of the maxillary right posterior molar region.4 The lesion, as depicted in Figure 2, shows a grayish white sloughing plaque with irregular borders located on the attached gingiva and alveolar mucosa. The authors reported the palatal mucosa, soft palate, and tonsillar pillar of this area as having no erythema or necrosis. The patient reported pain in the tooth area of No. 3, but he was not aware of the extent of tissue necrosis and erythema. Although a chemical burn was suspected, careful questioning and a differential diagnosis to rule out more ominous findings occurred as well. It was subsequently determined that the patient placed crushed raw garlic on the lesion throughout the day to combat pain. Family members told the patient about the benefits of placing raw garlic adjacent to the tooth to relieve pain. The patient had taken acetaminophen for pain prior to the use of garlic, but after using all of his available supply, he placed the garlic in the tooth region and then sought treatment after four days when the tooth and tissue continued to get worse. A thorough assessment was made, and because of bone loss, apical sclerosis, irreversible pulpitis, and severe gingival recession, tooth No. 3 was extracted. The extraction of tooth No. 2 and residual roots of No. 1 were also treatment planned. The patient was told to discontinue the crushed garlic and return for follow-up evaluation.
Garlic has been used throughout history for medicinal purposes. Egyptians, Romans, and many cultures have relied on the health benefits of garlic. The use of garlic has been a part of many cultures for thousands of years, and its use has been passed down through generations.5 Allicin is the product that is released when the garlic clove is crushed. Allicin is found in leeks, shallots, onions, and Chinese chives as well. When crushing a garlic clove, an enzyme called alliinase catalyzes the formation of allicin. It then breaks down to form organosulfur compounds. Current research at Oregon State University is being conducted on the many health benefits of garlic.6 However, placement of crushed garlic on oral tissue is not a health benefit, as evidenced in the case reported by Vargo et al.4
Burns from cinnamon products
Cinnamon use and cinnamic aldehyde allergy are widely reported, but without careful questioning of patients, it is difficult to diagnose. Cinnamon may be hidden in dental products and food, and some patients may be using large amounts of cinnamon on cereals, oatmeal, and even breads. Cinnamon may also be found in chewing gums, sodas, condiments, and candies. Patients may need to keep a diet diary to determine what they are using or consuming and how often. A new toothpaste, dental product, or mouth rinse (figure 3) may cause a reaction for patients. Further, a combination of foods or products should be considered. After the possible products are identified, discontinuing those offending flavoring agents and/or chemicals will usually clear up any irritation. Keeping a food and product diary for one week, followed by a two-week period of time after discontinuing use of a product, will confirm a cinnamon-related allergy.7
Burns from smokeless tobacco
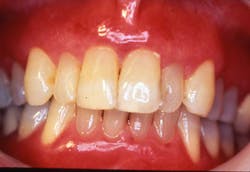
Smokeless tobacco continues to cause oral damage to the tissues over time, and its association with oral cancer is well documented (figure 4). Discontinuation of tobacco products is needed with follow-up visits to evaluate the tissue. The harmful chemicals and constant irritation to the tissue promote the possibility of oral cancer and tissue destruction.1,3
Related products such as Toumbak,8 predominately used in areas of Sudan, and betel quid products, used in many countries, are part of the current trend in tobacco use. Many other chemicals and additives are found within these products. As a reminder, these products should be considered in determining the cause of burns and tissue irritation when questioning patients, especially when tobacco use is thought to be involved. Careful questioning of patients is needed to determine what is being used, how often, and the amount of usage.
Conclusion
Asking good questions is crucial in determining the cause of burns or chemical injuries in the mouth. Without proper questioning, patients may not even remember what product they have used. Additionally, patients could be embarrassed that they used a particular chemical or product. Patients should be questioned about herbal use, alternative medicine products, and home remedies. Depending upon the offending substance, there could be other areas involved, such as the nasal or esophageal tissues. All areas of the head and neck region should be considered in a comprehensive evaluation. As always, remember to listen to your patients and ask good questions.
References
1. Neville BW, Damm DD, Allen CM, Chi AC. Oral and Maxillofacial Pathology. 4th ed. St. Louis, MO: Elsevier; 2016: 264-266.
2. Kang S, Kufta K, Sollecito TP, Panchal N. A treatment algorithm for the management of intraoral burns: A narrative review. Burns. 2018;44(5):1065-1076. doi:10.1016/j.burns.2017.09.006.
3. DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. 3rd ed. Philadelphia, PA: Wolters Kluwer, Lippincott, Williams & Wilkins; 2018.
4. Vargo RJ, Warner BM, Potluri A, Prasad JL. Garlic burn of the oral mucosa: A case report and review of self-treatment chemical burns. J Am Dent Assoc. 2017;148(10):767-771. doi:10.1016/j.adaj.2017.02.053.
5. Bagga S, Thomas BS, Bhat M. Garlic burn as self-inflicted mucosal injury—a case report and review of the literature. Quintessence Int. 2008;39(6):491-494.
6. Higdon J. Garlic and organosulfur compounds. Linus Pauling Institute. Micronutrient Information Center. Oregon State University website. https://lpi.oregonstate.edu/mic/food-beverages/garlic. Published 2005. Updated July 2008 by Drake VJ. Updated September 2016 by Delage B. Reviewed December 2016 by Reid K.
7. Burkhart NW. Toothpaste allergy. RDH magazine website. 2007;27(6):86,107-108. http://www.rdhmag.com/articles/print/volume-27/issue-6/columns/oral-exams/toothpaste-allergy.html. Published June 1, 2007.
8. Sami A, Elimairi I, Burkhart NW. Toumbak, the new king of smokeless tobacco. Presented at: American Academy of Oral Medicine 2018 Annual Meeting; April 12, 2018; San Antonio, TX.
About the Author
Nancy W. Burkhart, EdD, MEd, BSDH, AAFAAOM
NANCY W. BURKHART, EdD, MEd, BSDH, AAFAAOM, is an adjunct professor in the Department of Periodontics-Stomatology, College of Dentistry, Texas A&M University, Dallas, Texas. She is founder and cohost of the International Oral Lichen Planus Support Group (dentistry.tamhsc.edu/olp/) and coauthor of General and Oral Pathology for the Dental Hygienist, now in its third edition. Dr. Burkhart is an academic affiliate fellow with the American Academy of Oral Medicine, where she also serves as chair of the Affiliate Fellowship Program Committee. She was awarded the Dental Professional of the Year in 2017 through the International Pemphigus and Pemphigoid Foundation, and she is a 2017 Sunstar/RDH Award of Distinction recipient. Her professional interests are in the areas of oral medicine and the relationship between oral and whole-body health, with a focus on mucosal disease and early oral cancer detection. Contact her at [email protected].