How to perform a head and neck oral/ oropharyngeal cancer screening
Important: Use loupes and operatory lighting for optimal visualization.
Preliminary
- Assess for any abnormal movement, speech, or asymmetry upon greeting the patient.
- Obtain an updated dental, medical, and social history.
- Ask pertinent questions related to potential signs and symptoms during evaluation:
- Persistent (two weeks or longer) sore throat, cough, or hoarseness
- A change in voice
- Numbness or pain
- Unilateral earache
- Fatigue or exhaustion
- Difficulty swallowing or sensation of something caught in throat
- Unexplained weight loss
- Swollen, painless lymph node
Intraoral
- For optimal visualization, the clinician stands with the patient reclined at 45-degree angle, and patient chair raised to optimal level.
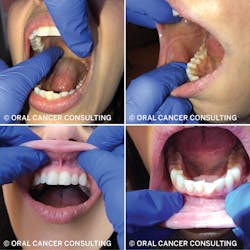
- Oral cavity (figures 1 and 2)
- Use mouth mirror to visualize all tissues and structures.
- Visualize and palpate lips, buccal mucosa, maxillary and mandibular labial and gingival tissue, vestibules, frenums, commissures, hard and soft palate, and retromolar trigone.
- Tongue
- Assess mobility: tongue extended, move side to side, up and down.
- Assess tongue tie: Patient opens mouth wide and touches tip of tongue just behind incisive papilla.
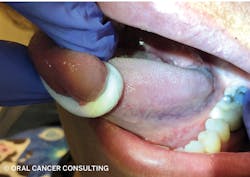
- Grasp tongue with moistened, rolled 2x2 gauze, firmly pulling tongue up and to side to visualize lateral borders, ventral surface, posterior third, and lingual tonsils. Palpate all surfaces visualized; repeat other side. Without gauze, palpate sides, tip, and dorsal surface.
- Entire floor of mouth: palpate intra- and extraorally simultaneously.
- Assess parotid and sublingual salivary flow, gently stimulating ducts with cotton tip.
Oropharynx
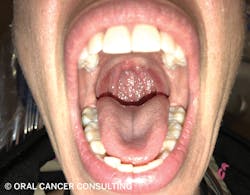
- Comprised of the palatine tonsils, soft palate, uvula, posterior third base of the tongue, lingual tonsils, posterior wall (figures 3 and 4).
- Place mirror on dorsal surface posterior third of tongue and depress firmly. The patient says “ahh.” Visualize uvula, soft palate, palatine tonsils, anterior and posterior tonsillar pillars, posterior wall, and glossotonsillar sulcus. Place salt on tongue for gagging.
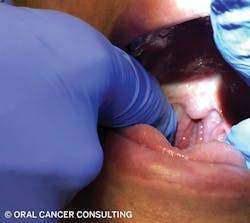
- Palpate glossotonsillar sulcus (where palatine tonsil meets posterior base of tongue). Slide finger in gently from retromolar trigone or anterior pillar.
- Assess palatine tonsils for symmetry in size and color. Document tonsil size (Brodsky score). Lingual tonsils assessed with tongue.
- Assess and document Mallampati score (classification of oropharyngeal structures; learn more at bit.ly/mallampati).
- Assess uvula for abnormalities in color, shape, deviations, swelling, and lesions.
Extraoral
- Patient sits upright.
- Face the patient; assess symmetry of head and neck.
- Examine skin, hairline, part in hair, facial hair, ears, nose, lips, vermilion border.
- Assess temporomandibular joint (TMJ) for crepitus, deviation, pain, popping, and limitations on opening.
- Palpate lymph nodes and muscles with circular compression using pad of fingers.
- Palpate occipital nodes with the patient’s head tilted forward.
- Palpate pre- and postauricular and facial nodes, parotid gland, and temporalis, buccinator, and masseter muscles with the patient’s teeth clenched.
- Palpate submandibular and submental nodes, pressing firmly against mandible.
- Rolling tissue over mandible, palpate sublingual and submandibular nodes with tongue at roof of mouth.
- With the patient’s head turned to one side and chin lowered and resting in the clinician’s hand, palpate sternocleidomastoid muscle and anterior and posterior cervical chains, then palpate clavicular nodes with the shoulder on same side raised slightly. Repeat on other side.
- Palpate thyroid and assess for symmetry during swallowing. For a helpful video by Stanford Medical School explaining the examination of the thyroid, visit bit.ly/RDHthyroid.
Editor's note: View Susan Cotten's companion article to this reference sheet here.
Susan Cotten, BS, RDH, OMT, is a passionate speaker, consultant, and subject-matter expert on HPV and the head and neck oral/oropharyngeal cancer exam. She is owner of Oral Cancer Consulting. She developed the “Cotten Method,” a comprehensive office system specific to oral cancer, assisting dental providers in early detection while reducing risk for liability. She is a 2018 recipient of the Sunstar/RDH Award of Distinction and Colorado Dental Hygienists’ Association Outstanding Contribution award.
About the Author

Susan Cotten, BSDH, RDH, OMT
Susan Cotten, BSDH, RDH, OMT, is dentistry’s oral cancer coach, 2018 Sunstar/RDH Award of Distinction recipient, and developed The Cotten Method™ of Screening for oral, oropharyngeal cancer, and other head and neck concerns. With more than 30 years as an RDH, Susan provides in-office training, speaking, and hands-on workshops to deepen confidence in a comprehensive screening, reduce liability, and increase early detection. Determined to have a world Oral Cancer Free™, her course is available online through the National Network of Healthcare Hygienists. Reach her at [email protected].