Antral pseudocyst
BY NANCY W. BURKHART, BSDH, EdD
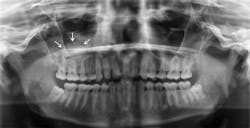
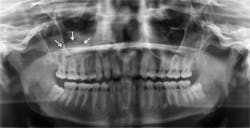
Your patient today is Carl, a 33-year-old engineer who has a six-month maintenance appointment. Carl has not had a Panorex film made for a number of years, and it is suggested to him. Upon evaluation of the film, you note a broad-based, weakly opaque, dome-shaped entity in the right maxillary sinus.
The patient reports no symptoms and has no discomfort in the right region of the sinus. You do not note any swelling either intraorally or extraorally on the right side of the face. A complete intraoral exam is performed, and there are no significant findings. The patient is taking no prescription medications but does report seasonal allergies. Upon a complete evaluation, it is determined to be a classic antral pseudocyst (AP).
Etiology and pathogenesis: The research reported in regard to antral pseudocysts suggests that the entity is composed of serous exudates that evolve under the maxillary sinus. Antral pseudocyst has been interchanged with a sinus mucocele and mucous retention cyst of the sinus.
Antral pseudocyst is the most accurate term. The mucocele is destructive and requires surgery while the AP does not require intervention and will dissipate. In a classic paper by Gardner (1984), in an attempt to clarify the terms that add to the confusion of APs, a differentiation with other entities is made. Sinus mucoceles present with accumulation of mucin, including the expansion and destruction of bone. Retention cysts present with a blockage of a duct and surrounded by epithelium. Both have been interchanged incorrectly with APs.
Gardner describes the AP as occurring because of focal inflammatory exudates that lift the epithelial lining of the sinus and the periosteum from the underlying bone, producing a domelike appearance. It is thought to be the result of a previous odontogenic infection, a sinus infection, or an infection that caused irritation to the sinus lining. The AP has been confused with the mucous retention cyst (that is an epithelial lined true cyst) and antral mucocele, which, according to Gardner, rarely occurs in the maxillary sinuses.
Epidemiology: Previous studies of large radiographic evaluations place the occurrence of the antral pseudocyst at anywhere from 1.5% to 10% of the general population (Neville et al., 1994). The AP can occur in any age group.
Extraoral characteristics: The antral pseudocyst usually produces no expansion of bone and no extraoral swelling. Other cysts that do promote expansion and bone destruction will eventually have extraoral swelling with pain or discomfort. The antral pseudocyst does have the capability of growth and most will dissipate without any damage or intervention.
Radiographic distinguishing characteristics: The classic antral pseudocyst presents as a dome-shaped lesion on the maxillary sinus floor. Most have a very faint, opaque appearance on a radiograph. The lesion is usually well delineated (see Figure 1). There is sometimes confusion with the AP and polyps. Polyps are irregular in shape when compared to the AP. The fluid in polyps is in the loose connective tissue of the lamina propria of the lining of the sinonasal tract, and the mucosa is thickened by edema.
Histology: The antral pseudocyst does not contain an epithelial lining and is composed of a serous fluid. The AP cannot be removed intact since the fluid will gush out while the polyp will be intact and the surgeon is able to remove it. These pseudocysts usually rupture on their own.
Differential diagnosis: Fine-needle aspiration is sometimes necessary to differentiate the AP from other entities when an abnormal pattern or appearance may cause suspicion of other types of cysts or pathology (Sett-Dias AC et al. 2013). The antral pseudocyst was originally confused with the sinus mucocele that contains mucin and is epithelial lined. Radiographically, the entire sinus will appear cloudy when the lesion is a sinus mucocele (Neville et al. 1995). Tumors and tooth-related cysts appearances may cause some diagnostic confusion in certain instances.
Dental implications: Testing of the pulp vitality is completed, and the teeth should test vital. The patient should be followed and evaluated for any increase, decrease, or future infection of the general area of the sinus.
Treatment and prognosis: Generally, no treatment is needed. The patient should be evaluated at periodic appointments. If there is any question regarding the diagnosis, the fluid may be removed and the specimen histologically examined. A procedure called Caldwell-Luc is performed on any lesion with noted expansion, destruction, or symptoms indicating possibly etiology other than the classic antral pseudocyst. This surgical procedure is used to enter the cyst and clean out the affected area.
The antral pseudocyst is routinely just monitored until it dissipates. The main problem would be misdiagnosis of a more destructive lesion resulting in overtreatment.
As always, continue to ask good questions and always listen to your patients. RDH
References
1. Cortes AR, et al. 2012 file://localhost/J Craniofac Surg. 2012 Nov%3B23(6)/e535-7. doi/ 10.1097:SCS.0b013e31825aaff8. Evaluation of a maxillary sinus floor augmentation in the presence of a large antral pseudocyst. Cortes AR1, Corrêa L, Arita ES.
2. Gardner DG. file://localhost/Pseudocysts and retention cysts of the maxillary sinus. Gardner DG. Oral Surg Oral Med Oral Pathol. 1984 Nov%3B58(5)/561-7.
3. Neville BW, et al. Oral and Maxillofacial Pathology. W.B. Saunders Co., Philadelphia. 231-232, 1994.
4. Sette-Dias AC, et al. 2013. file://localhost/Stomatologija. 2013%3B15(3)/92-4. Differential diagnosis of antral pseudocyst. A case report. Sette-Dias AC1, Naves MD, Mesquita RA, Abdo EN.
5. Haring JI. Case Study. http://www.rdhmag.com/articles/print/volume-22/issue-1/columns/case-study/case-study.html
6. Gardner DG. Pseudocysts and retention cysts of the maxillary sinus.
7. Gardner DG. Oral Surg Oral Med Oral Pathol. 1984 Nov; 58(5): 561-7. file://localhost/Oral Surg Oral Med Oral Pathol. 1984 Nov%3B58(5)/561-7. Pseudocysts and retention cysts of the maxillary sinus. Gardner DG.
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. Her website for seminars on mucosal diseases, oral cancer, and oral pathology topics is www.nancywburkhart.com.