By Lynne Slim, RDH, BSDH, MSDH
More than two years have passed since my last visit to the densely populated Manhattan, and this time I took a train to Penn Station, followed by the New York subway to my eventual destination near the theater district. My great friend, Fay Brown, RDH, guided me through the maze, and it was actually a lot of fun. Unlike previous memories from childhood when NYC subways were considered dangerous, the subway system is clean and I felt relatively safe.
I was in New York City to attend a continuing education course for physicians and oral health-care professionals (primarily oral surgeons). The course consisted of an update on bisphosphonate and rank-l inhibitor (denosumab) associated osteonecrosis of the jaws. The presenters for the all-day conference were Dr. Robert Marx, chief of the division of oral and maxillofacial surgery at the University of Miami, and Dr. Richard Kraut, professor and director of oral and maxillofacial surgery at Albert Einstein College of Medicine.
-----------------------------------------------------
More articles by Lynne Slim
- Influx of Baby Boomers
- Educating patients about the biofilm phenotype
- Grading evidence concerning bidirectional diabetes
-----------------------------------------------------
Bisphosphonate-induced osteonecrosis of the jaws (BIONJ) was first introduced by Marx and Stern in 2002. Marx described it as exposed, nonhealing bone that worsened with debridement. At that time, all of the patients in the 2002 report were being given pamidronate (Aredia, Novartis) to control malignant tumor deposits in bone.1
I've already published several articles about Victorian era (mid to late 1800s) match factory workers whose working conditions were dangerous and who were exposed to poisonous fumes that resulted in "phossy jaw." It took the financial generosity of the public and some press support — in addition to forming a trade union — to improve working conditions. But it was many more years before these workers stopped using the dangerous phosphorous vapors that contributed to osteonecrosis of the jaws (ONJ).2
Cases of osteonecrosis of the jaws have returned and are on the increase, according to Marx and Kraut, and we cannot turn a blind eye to this debilitating drug-induced side effect.
As a review, today's oral nitrogen-containing bisphosphonates and intravenous nitrogen-containing bisphosphonates circulate around the body the same way as the phosphorous vapors, and are absorbed into bone and ingested by osteoclasts. When this unique binding process of bisphosphonates to bone occurs, osteoclasts are poisoned, and this reduces or eliminates bone turnover. Alveolar bone in the mandible and maxilla turns over more rapidly than in long bones, so the jaws are a better target for bisphosphonate toxicity.2
What began as a positive correlation in 2002 between the bisphosphonate class of drugs (oral and IV) and ONJ has now changed to include new drugs:
- Prolia, an osteoporosis drug
- Xgeva, a cancer drug
Both of these drugs have been implicated in ONJ pathogenesis and have added more uncertainty concerning prevention, management, and resolution of directed treatments.3 In addition, the anti-angiogenic drug bevacizumab (Avastin) and the tyrosine kinase inhibitor sunitinib (Sutent), both cancer drugs, are associated with ONJ (based on case reports). But both of these drugs have too few cases and a low incidence to date of developing it.3,4 Even so, the risk of developing ONJ has been issued an advisory by the Food and Drug Administration and committee of the American Association of Oral and Maxillofacial Surgeons (AAOMS) who wrote the 2014 position paper expressing concern about a similar potential risk associated with several other medications within the same drug class that have a similar mechanism of action.4
Names for ONJ that are associated with bisphosphonates such as BRONJ, BON, BONJ, and BIONJ have now been replaced by the American Medical Association with the name DIONJ (drug-induced ONJ), and there is even a site-specific ICD-9 code of 733.45.3 The AAOMS recently recommended changing the nomenclature of BRONJ to medication-related osteonecrosis of the jaw (MRONJ), and they have a new position paper that discusses risk estimates and gives clinicians management strategies for patients treated with these drugs.4
It took me a while to wrap my head around these new drugs. So I have customized a table showing drug name, classification, action, dose, and route (see Table I).
Prolia and Xgeva are inhibitors of RANKL, which inhibits osteoclast function and associated bone resorption. When Prolia is administered by subcutaneous injection every six months, there is a reduction of risk of vertebral, nonvertebral, and hip fractures in patients with osteoporosis.4
Xgeva is effective in reducing skeletal events related to metastatic bone disease from solid tumors and is administered monthly.4
The only risk factor for DIONJ is the offending drug, according to the authors of the University of Miami position paper, and oral health-care professionals need to become familiar with the list of bisphosphonate drugs for osteoporosis and new drugs for the treatment of cancer complications and metastasis.3 Diagnosing DIONJ requires ruling out a history of radiotherapy to the jaws or osteomyelitis (bone infection) that can mimic DIONJ. Osteopetrosis can also mimic DIONJ as can cement-osseous dysplasia. Osteopetrosis is limited to women of African heritage in the 30- to 50-year age range.3
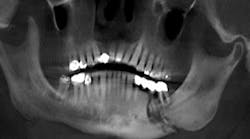
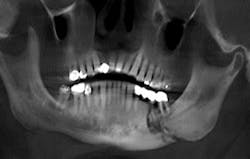
The presence of exposed bone may be subtle and may at first appear as a fistula or periodontal defect when probing, or granulation tissue covering over unhealed exposed bone.3 In reviewing the database from the University of Miami, 29% of cases of exposed bone develop spontaneously without any initiating insult to the alveolar bone, and 61.6% are initiated by extraction. Dental implant surgery accounts for 2.2%, bone biopsy 1.1%, and periapical surgery is an initiating event in only 0.5% of cases.3 Affected alveolar bone is often seen by observing sclerosis of the lamina dura in a radiograph or radiographic identification of a more diffuse sclerosis in the alveolar bone.3
Exposed necrotic bone is becoming more common in today's general and specialty dental practices. Hygienists and dentists must take detailed medical histories and carefully examine patients at risk for DIONJ. Create a list of all bisphosphonate drugs (oral and IV) and new drugs, paying close attention to the potency of the drug and its route of administration. The length of time the drug has been taken plus the drug's half-life in bone is important information to record in the patient's chart.3
In a future column, I will cover prevention and management strategies for patients who are treated with drugs strongly associated with DIONJ.
Table I | New Drugs Implicated in DIONJ* | |||
Drug | Classification | Action | Dose | Route |
Prolia (denosumab) | Monoclonal antibody | Osteoclast inhibitor | 60 mg/ 6 months | Injection |
Xgeva (denosumab) | Monoclonal antibody | Osteoclast inhibitor | 120 mg/mo | IV |
*Avastin (bevacizumab) and Sutent (sunitinib) are also associated with ONJ, but both drugs, to date, have few cases and a low incidence. | ||||
LYNNE SLIM, RDH, BSDH, MSDH, is an awardwinning writer who has published extensively in dental/dental hygiene journals. Lynne is the CEO of Perio C Dent, a dental practice management company that specializes in the incorporation of conservative periodontal therapy into the hygiene department of dental practices. Lynne is also the owner and moderator of the periotherapist yahoo group: www.yahoogroups.com/group/periotherapist. Lynne speaks on the topic of conservative periodontal therapy and other dental hygiene-related topics. She can be reached at [email protected] or www.periocdent.com.
References
1. Marx RE. (2011) Oral and Intravenous Bisphosphonate-Induced Osteonecrosis of the Jaws (2nd.ed.). Quintessence Publishing Co., Inc.
2. http://www.rdhmag.com/articles/print/volume-29/issue-7/feature/the-return-of-the-dreaded-145phossy-jaw146.html
3. Marx RE, Broumand V, Tursun R. University of Miami, Division of Maxillofacial Surgery. Position paper on drug induced osteonecrosis of the jaws. April 15, 2014. (unpublished)
4. American Association of Oral and Maxillofacial Surgeons. Medication-related osteonecrosis of the jaw- 2014 update. (position paper).
Past RDH Issues