Thyroid issues: Goiters and other conditions pinpoint the thyroid gland's effect on the body
By Nancy Burkhart, BSDH, EdD
The thyroid gland is a butterfly-shaped gland and is found in the lower portion of the neck below the thyroid cartilage. Palpation of this area is always part of the extraoral exam. Normally, the thyroid gland is not visible clinically in the healthy individual, but may be palpated as a soft tissue mass.
The thyroid gland develops in the area at the base of the tongue at the foramen cecum. During normal development, it migrates into the neck along the thyroglossal duct tract. When the migration does not occur, the gland remains at the base of the tongue and is known as a lingual thyroid. This tissue mass may be mistaken for a growth that needs to be biopsied or removed. However, when thyroid hormone deficiency is suspected, it could be the only functioning thyroid tissue the patient may have in the body, so careful evaluation is needed.
Any abnormal growth or enlargement in the thyroid area should alert the health-care provider to the possibility of thyroid cancer until proven otherwise. Sometimes larger masses of tissue may be observed in the neck, and these can become quite large, surprisingly undetected in some cases, and referred to as a goiter.
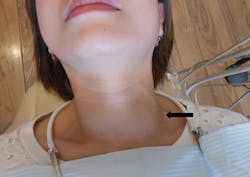
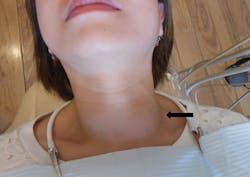
Goiters are clinically observed when performing the extraoral exam (see Figure 1). The size and rubbery consistency of the goiter will usually become noticeable when palpated. A common cause of goiter worldwide is the lack of iodized salt.
This has even become a problem in Western cultures since rock salt has often replaced the iodized salt that was once used. Iodine allows the body to produce an adequate amount of the thyroid hormone that is needed to perform daily cellular functions. Many salts today do not have the iodine that was added in the past, and a reduction of salt in the average diet has occurred because of the association with hypertension.
But in countries where iodized salt is readily available, goiters are usually due to nodules that develop in the gland because of either over- or underproduction of the hormones that are associated with the thyroid. Other factors that can cause the thyroid to enlarge are Graves' disease, Hashimoto's disease, multinodular goiter, solitary thyroid nodules, inflammation, and pregnancy.
Figure 1: In office of: Dr. Carol Jin San Ramon, CA. Narrative: Upon palpitation, it is firm, raised approximately 1", and measures 3" by 3" in a circular formation. Courtesy of Carol Perkins, RDH.
Detection during the dental exam
According to the American Thyroid Association, an estimated 20 million Americans have some form of thyroid disease. Up to 60% of those with thyroid disease are unaware of their condition. Women are eight times more likely than men to develop a thyroid problem, and one woman in eight will develop a thyroid condition in her lifetime.
Stewart (2001) expressed two solid reasons for checking the patient's thyroid during a dental exam. The first is to aid in diagnosis, and the second reason is to avoid any serious complications during the actual dental treatment.
The dentist or hygienist is often the first person to notice a change in the neck region and refer the patient to a physician for treatment. The earlier a definitive diagnosis is made, the less damage will occur to the patient and the systems of the body. Malignancy can occur and needs to be ruled out as a cause for the mass increase. Thyroid cancer accounts for 3.8% of new cancers, and 64,300 new cases of thyroid cancer will be diagnosed in 2016 (NIH, National Cancer Institute Seer data).
In some countries, cretinism (congenital hypothyroidism) is rising due to hypothyroidism in the mother. Birth defects such as heart, brain, and kidney problems are documented in babies born to women with untreated hypothyroidism. Children may have a higher risk of cleft palate and intellectual developmental problems as well. Thyroid problems can occur because of two reasons: an excess of thyroid hormone or a deficiency in thyroid hormone. An imbalance in hormones will produce varying symptoms.
Myxedema occurs in hypothyroidism in adults, and this edema causes water retention and facial changes. Enlarged gingiva associated with edema may also occur in uncontrolled and prolonged hypothyroidism. Hypothyroidism laboratory results indicate elevated thyroid-stimulating hormone levels (TSH) with reduced levels of thyroxine. Prolonged hypothyroidism may result in a dull expression, puffy eyelids, coarse skin, dry hair, slowed mental and physical activity, anemia, and secondary cardiovascular effects may occur. Dental effects of prolonged hypothyroidism are gingival enlargement, macroglossia, glossitis, salivary enlargement, and dysgeusia. As the tissue enlarges in the thyroid area, there may be difficulty in swallowing and breathing, and increased coughing may be noted as well.
The thyroid gland produces three hormones, T3 (triiodothyronine) and T4 (thyroxine) and calcitonin. These hormones control the metabolism of almost all the cells in the body. Follicular cells in the thyroid gland produce the thyroid hormones thyroxine and triiodothyronine. Thyroxine and triiodothyronine regulate basal metabolic rates and body temperature, lipid metabolism, carbohydrate metabolism, and all aspects of linear growth. They are crucial in brain development before and after birth; regulate heart rate, contractibility, and output; and regulate vasodilation, respiratory rate, gastrointestinal activity, libido, and fertility (Delong & Burkhart, 2013).
Calcitonin is produced by parafollicular cells in the gland. It inhibits the release of calcium from the bones into blood and other fluids, as well as regulates serum calcium and phosphorus levels. As you can see, the thyroid hormones are essential for all normal bodily functions and good health.
The thyroid gland has an effect on every system in the body. In the case of hyperthyroidism, palpitations, tremors, tongue tremors, and bone loss are reported. Graves' disease is a result of hyperthyroidism in some cases. The symptoms of both increased and decreased thyroid function often produce bodily complaints that can be very vague and may even be attributed to medications and other disease states. There is a period of trial and error in attempting to diagnose these complaints. The patient may exhibit frustration in the lack of a diagnosis that may send the patient to multiple health-care providers in search of answers.
Hashimoto thyroiditis is an autoimmune disease in which the body treats the thyroid tissue as an antigen, and this results in inflammation and a slow destruction of the thyroid gland. High levels of antibodies against thyroglobulin and the enzyme thyroid peroxides (TPO test) play a role in the production of thyroid hormones and are diagnostic in Hashimoto thyroiditis (Burkhart, 2013).
Routinely, the normal thyroid levels are tested through TSH levels: For most labs that number is 0.3-3.0 mIU/L. Some physicians like to see the upper limit at 2.5 mIU/L. Higher levels of TSH mean that the pituitary gland is producing thyroid stimulation to compensate for low levels of thyroxin in the bloodstream in order to stimulate the thyroid gland to produce more thyroid hormone. This causes chronic enlargement of the gland as it attempts to produce enough thyroid hormone to "turn off" the release of TSH by the pituitary gland. Since the cells that produce the thyroid hormones T3 and T4 are incapable of decreased hormone production, they must adapt to the increased demand by becoming hyperplastic or hypertropic (DeLong & Burkhart, 2013).
Treatment for hypothyroidism is thyroid replacement hormones such as Levoxyl, Synthroid, Cytomel, Thyrolar (containing both T3 and T4), or Armour Thyroid (made from pigs). Some physicians do not recommend Armour Thyroid since there may be a slight risk of disease transmitted by animal tissue, and this is under investigation. There is also a difference in the animal tissue with the ratio of T3 to T4 compared to humans and may raise the risk of bone and heart problems.
The oral manifestations may vary depending upon the extent and length of the deficiency. Restoring and maintaining the euthyroid (normal thyroid balance) is the long-term goal of medical treatment. Vital signs should be taken, and medication dosage and pertinent questions should be asked of the patient.
Oral medicine considerations
An estimated 20 million Americans suffer from hypothyroidism and as many as 60 million may be undiagnosed, because the symptoms mimic other diseases/disorders (American Thyroid Association). Patients often complain of fatigue; sensitivity to cold; constipation; puffiness in the face; changes in voice; elevated blood cholesterol level (LDL level); fluid retention and weight gain; muscle aches; tenderness in the hips and shoulders; joint pain; pale, dry, coarse skin; changes in hair; forgetfulness; and a slowing of the thought process in general with possible depression.
Some patients may experience some or all of these symptoms to varying degrees. However, other common disorders have similar complaints such as obesity, diabetes, sleep apnea, depression, kidney problems, heart disorders, and the list goes on. So it is difficult to rely on symptoms to make a diagnosis. Only blood tests can diagnose thyroid hormone levels. Other tests for further diagnosis include antibody tests, ultrasonography, thyroid scans, and biopsy. Stress appears to heighten thyroid issues.
Patients who have noted uncontrolled hypothyroid issues may be more susceptible to problems with local anesthesia and retraction cord soaked with epinephrine. The effect of epinephrine is increased when a patient has thyroid issues. Consultation with the patient's physician is suggested when doubt exists regarding the status of the patient.
Some foods also act as goitrogens and can interfere with thyroid hormone production, thereby slowing down the thyroid function. Foods in the cruciferous category such as cabbage, broccoli, cauliflower, radishes, rutabagas, and turnips may inhibit the body's ability to use iodine. Some physicians suggest using these vegetables in moderation or to minimize their use depending upon the severity and cause of the hypothyroidism. Additionally, certain medications may interact with thyroid medications. Taking thyroid medication on an empty stomach and several hours before or after other medications is suggested.
Keep listening to your patients and always ask good questions. RDH
How to document an enlarged thyroid gland
Clinically, when noting a goiter or undiagnosed enlarged thyroid, the health-care provider should document the size, shape, mobility, and consistency of the growth. Clinical images are always optimal for documentation along with written descriptions.
Having the patient turn to one side and then to the other often allows the clinician a clear outline of the gland. Using the fingers of both hands to palpate will determine the lower extension of the growth. Associated lymph nodes should be palpated as well. Ask the patient to swallow to observe the movement of the thyroid tissue. There should be follow-up with an internist or an endocrinologist (Glick, 2015). Nodules that are noted may be varying types of goiters, metastatic disease, lymphoma, and even masses of thyroid cancer.
What questions should you ask your patient about any neck abnormality or previous thyroid treatment?
- Have you noticed a change in your neck?
- Have you ever been told that you have a thyroid problem?
- When were you aware of any thyroid issues?
- What was the diagnosis? For example: a cyst, goiter, or other.
- What signs or symptoms did you have that caused your physician to test you? What were your original complaints?
- How often do you see your physician?
- What is the long-term plan for your condition?
- Have you fainted or passed out at any time since you last saw your physician?
- What medications do you take? Has your physician increased or decreased your medication dosage recently? If so, why?
- Are you on medication long term?
- Do you currently have other medical problems such as diabetes or heart disease?
- Do you find yourself weaker and more lethargic than you were a few months ago?
- What type of problems are you having in your mouth? Enlarged tongue, dry mouth, difficulty in swallowing, swollen salivary glands, hoarseness, inflammation, difficulty breathing or pain?
References
1. Burkhart NW. Hashimoto's thyroiditis. RDH. 2013; 33(3): 66-68.rdhmag.com/articles/print/volume-33/issue-3/columns/hashimotos-disease-hypothyroidism-is-autoimmune-disease.html.
2. Hubbard S. The head and neck exam: Only 25% of dental hygienists provide the service. Why? RDH Magazine, April 36:4.2016.
3. DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist, 2nd ed. Wolters Kluwer Health/Lippincott, Williams & Wilkins. Baltimore, 2013. Pg. 165-68.
4. Glick M. Burket's Oral Medicine. 12th ed. People's Medical Publishing House USA, Shelton CT, 2015.
5. Little JW. Thyroid disorders. Part ll: hypothyroidism and thyroiditis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006; 102(3): 275-80.
6. McGrogan A, Seaman HE, Wright JW, de Vries CS. The incidence of autoimmune thyroid disease: a systematic review of the literature. Clin Endocrinol 2008;69(5):687-96.
7. Nobuyuki A, Tada H, Hidaka Y, Hashimoto K. Hashimoto's disease and Dr. Hakaru Hashimoto. Endocrine J. 2002; 49(4), 393-7.
8. Radziewicz LC. RDH, Hashimoto's Disease. rdhmag.com/articles/print/.../hashimotorsquos-disease.html
9. Rees TD. Endocrine and Metabolic Disorders from Clinical Care in Oral Health. 2012.
10. Silverman S, Eversole LR, Truelove EL. Essentials of Oral Medicine. Dr. Carol M. Stuart. Chapter 9. London:BC Decker Inc; 2001 96-99.
11. The ADA Practical Guide to Patients with Medical Conditions, First Edition. Edited by Lauren L. Patton. 2012; John Wiley & Sons, Inc.
12. Beck M. Doctors hear patients' calls for new approaches to hypothyroidism. WSJ, April 11, 2016. wsj.com/articles/doctors-hear-patients-calls-for-new-approaches-to-hypothyroidism-146040111
Website Information
1. hormone.org or call 1-800-HORMONE.
2. American Thyroid Association. thyroid.org, accessed May 3rd 2016.
3. National Graves' Disease Foundation, ngdf.org.
4. seer.cancer.gov/statfacts/html/thyro.html.
5. video.about.com/thyroid/The-Difference-Between-Hashimoto-s-Disease-and-Hypothyroidism.htm.
6. The Mayo Clinic,mayoclinic.org/diseases-conditions/hypothyroidism/symptoms-causes/dxc-20155382
7. thyroidawareness.com/neck-check
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics/stomatology, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was awarded a 2016 American Academy of Oral Medicine Affiliate Fellowship (AAOMAF). She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. She can be contacted at [email protected].