Chipping Away At Unresolved Pocket Depth
The incorporation of PerioChip into periodontal maintenance provides a treatment option for frustrating cases where periodontitis continues to linger.
Terri S.I. Tilliss, RDH, MS, MA, and
Kimberly Krust Bray, RDH, MS
Jennifer has been practicing for many years. Her practice schedule has varied from two to five days per week, depending on what was happening in her life, but she has consistently practiced and has been in only two office settings during all those years. Jennifer feels that she has reaped the rewards of her career. She would not hesitate to choose dental hygiene again if she were just beginning college. She finds great satisfaction in helping her clients attain and maintain oral health.
Yet, something has been bothering Jennifer for a long time. It nags at her almost every workday. She rationalizes that it is just a part of being a dental hygienist, part of the limitations in treating periodontal disease. When she views it this way, she can push it to the back of her mind for short periods. But the nagging thoughts do not ever really go away.
Jennifer`s unease pertains to the periodontal maintenance of her clients. She enjoys greeting and treating these clients every three or four months. In fact, she finds that welcoming back these long-term clients every few months is one of the real pleasures of clinical dental hygiene. There are not many professions, she feels, where one can spend an hour every few months with people who have become friends.
Jennifer knows, both empirically and from an evidence-based perspective, that her regular scaling and root-planing procedures coupled with her clients` varying degrees of compliance with an oral hygiene regimen does make a difference. She knows that, in general, frequent debridements can maintain periodontal conditions.
Why does Jennifer often feel frustrated? The frustration occurs when measuring and documenting probe readings. Jennifer finds that, appointment after appointment, some areas improve while others stay the same. To her dismay, some probing depths get even worse.
Many of Jennifer`s clients have isolated 4 mm or 5 mm pockets. Others even have scattered 6 mm or 7 mm pockets. Although Jennifer has educated clients about the option of periodontal surgery, only a handful seriously consider it. In addition, she encourages a variety of oral hygiene aids or well-designed manual brushes or power brushes. She also frequently suggests newer dentifrices and mouthwashes developed to address gingival conditions.
But nothing ever seems to change in a substantial way. Jennifer believes that this is due not only to the limitations of these products, but also to compliance issues. The products and techniques that she recommendeds require her clients to change their behavior - often an insurmountable feat. Therein lies Jennifer`s frustration. She just doesn`t feel right debriding and documenting probe readings time after time without seeing much significant improvement. Sometimes the pockets are even deeper than they were previously. She`s pretty well given up on the idea of getting some of these individuals to take their periodontitis seriously; they just seem resistant to the idea.
One day, about a year ago, Jennifer was reading a journal during her lunch hour. She saw an article which addressed chemotherapeutics and periodontal disease. The article focused on a new antimicrobial product called the PerioChip® (2.5 mg. chlorhexidine gluconate). Manufactured by Perio Products Ltd., in Jerusalem, Israel (and distributed by Astra Zeneca, L.P., in Westborough, Mass.), the product consisted of a "wafer" - actually, a "biodegradable gelatin matrix" impregnated with chlorhexidine.
All that was needed was to slip the chip into the pocket and chlorhexidine would bathe the area for seven to 10 days. She was glad to learn that there was no need to remove the chip; it would simply dissolve away. Jennifer knew that chemotherapeutics can help control plaque and kill pathogens in the tissues and crevices. After retrieving the original reference from the dental school library describing the PerioChip, she was convinced this product offered good results for clients who sounded just like hers.
The exciting part to Jennifer was that this approach didn`t require any active compliance on the part of the patient. She also didn`t have to be convinced about chlorhexidine; she knew it was the "gold standard" in antimicrobials.
She knew, though, that in-office irrigation with chlorhexidine wasn`t the answer. The chlorhexidine does not remain in the pocket long enough, and studies fail to show that irrigation really helps. Certainly, she`d gotten many of her clients over the years to rinse at home with it, but the taste and staining often affected compliance.
Since the chip is 5 mm long, she knew that it could only be placed in pockets of 5 mm or more. She had plenty of those in her practice!
After enthusiastically discussing PerioChip with her employer, Dr. O, they talked it over with the periodontist who manages their referred patients. The periodontist spoke favorably about PerioChip and suggested that they try it.
Jennifer recommended that it would be important to routinely document the periodontal status of all patients. They decided to start by treating a few patients with PerioChip and to follow their outcomes. Jennifer selected two patients with 5 mm to 7 mm pockets. She followed the documentation outlined in the study so that she could track the results.
Jennifer was excited about beginning a new therapy. She felt sure that the clients she had in mind would be receptive for three main reasons:
- They had tired of hearing her call out pocket depth readings that changed only slightly, not at all, or even got worse.
- They wouldn`t have to add anything to their usual oral hygiene regimen.
- The PerioChip procedure would not be overly costly.
She knew that thorough scaling and root planing would still be necessary, as she`d always done. Yet, she also knew that local delivery systems using antimicrobials could provide an additional opportunity to affect the bacteria that scaling and root planing may leave behind. With the local delivery of antimicrobials, the re-population of pockets with bacteria would be delayed. Maybe this would make a difference for her clients. In essence, it could extend the benefits of the debridements that she was providing.
Jennifer considered the clients in her practice with pocketing that never seemed to resolve. She selected two who fit the criteria for PerioChip use and should benefit from the procedure.
The first client: Paul
The first to return for a maintenance visit was Paul, who is 65 years old. Reviewing his medical history, Jennifer saw that he had mild hypertension, arthritis, and cancer/prostate surgery. He also had depression, which is controlled by Prozac, his only regular medication. He used to smoke, but hasn`t for the past 20 years.
Paul`s only oral hygiene practice is brushing once daily. He`d never quite adopted the practice of flossing or using any other device interproximally. He had quadrant scaling/root planing five years ago. He doesn`t always make it in for three-month maintenance visits.
When Paul arrived at the office for his first maintenance appointment, he presented as a Periodontal Case Type III. His pocket depths ranged from 2 mm to 8 mm with generalized bleeding and edematous tissue. He had generalized horizontal bone loss on the right side - the most serious loss of attachment at #2 and #3 - as well as a Class I furcation on the DL of #2. He also had deep pockets on #14 and #15 with a Class II furcation involvement at #14DL.
Jennifer scaled and root planed his right side using anesthesia for the maxillary molars. This was all the scaling she planned to complete at this appointment. The remainder of the time was spent working with Paul on his oral hygiene and explaining about the PerioChip therapy that she had in mind. She assured Paul that Dr. O was in complete agreement with her about the need for PerioChip. After Paul understood that the PerioChip was non-invasive, painless, and not overly expensive, he agreed to try it.
Jennifer completed the left side two days later, again with anesthesia for the maxillary molars. At this appointment, after thoroughly drying the areas, she placed a PerioChip at the ML #2 and DB #14, the two sites she had selected for initial treatment with the PerioChip. She was pleased at how easily and effortlessly the chip slipped into the pockets. She reminded Paul not to floss for 10 days at the PerioChip sites, knowing that this would be no great hardship; floss rarely found its way into Paul`s mouth under any circumstances! He could continue to brush normally, and there would be no food restrictions.
She eagerly awaited Paul`s return after a three-month interval. After the usual preliminaries, she probed the PerioChip sites. There was a 1 mm pocket depth reduction at #2 ML; it changed from 6 mm to 5 mm. She knew that placement of another PerioChip at this site was indicated since it still measured 5 mm. To her delight, Jennifer found that #14 DB had improved from 7 mm to 4 mm. She completed probing the rest of his mouth, disclosed and reinforced his plaque removal skills, and then scaled his mouth. Last, she placed another chip at #2 ML and again reminded Paul not to floss at this site.
The following three months flew by. When Jennifer looked at the daily schedule, she was amazed that it was time for Paul`s next maintenance appointment. After the usual greetings, Jennifer determined that Paul had begun some flossing. Although he was not regular, by any means, he had begun flossing a "couple of times each week." This was progress!
After performing her other assessments, Jennifer disclosed and reinforced plaque removal techniques at his "trouble spots." She then probed the entire mouth and had some interesting findings. There was still a measurement of 5 mm at #2 ML, so she placed another chip. The 4 mm pocket at #14 DB had stayed stable. Jennifer helped Paul to understand the changes that occurred and reminded him not to floss at #2 ML for 10 days.
When Paul returned nine months after the initial PerioChip placement, Jennifer found that #14 DB, which had received a chip only once nine months ago, was maintaining a 3 mm reduction from baseline. She noticed that #14 DL, which did not receive a chip, also had a 2 mm reduction. She wondered if there could have been some crossover of chlorhexidine from facial to lingual. The ML of #2 had achieved another 1 mm improvement.
In summarizing the nine-month span, Jennifer realized that the chlorhexidine-treated pockets, ML #2 and DB #14, had reduced 2 mm and 3 mm respectively. Just like the original study findings, the areas treated with PerioChip were more likely to show pocket depth reduction >2 mm changes than those that received scaling/root planing alone.
The second client: Sally
The second client approached about treatment with PerioChip was Sally. Sally had joined the practice about 11/2 years ago. At that time, she had four quadrants of scaling and root planing performed due to several scattered 4 mm to 7 mm generalized pockets. She has been on three-month maintenance since then. But, being the busy mother of three small children, the intervals between appointments sometimes would stretch to four to five months. After the scaling and root planing, Sally`s pocket depths had improved slightly in some places, but not consistently enough for Jennifer or Sally to feel content. As Jennifer suspected, Sally was thrilled to have a noninvasive option to try in order to help manage this disease process.
Sally is 38 years old, and her medical history was unremarkable other than an aspirin allergy. She has smoked for 15 years. Sally has had nine posterior teeth extracted over the years, has eight fillings, no new decay, and wears a maxillary partial denture. Her oral hygiene regimen consists of brushing twice daily and occasional use of dental floss.
Sally, like Paul, presented as a Periodontal Case Type III. At today`s appointment, her pocket depths ranged from 2 mm to 6 mm. There was some bleeding on probing. Generalized moderate to advanced bone loss was evident along with 1 mm to 2 mm recession. There was a Class II furcation on #12D.
After completing the perio charting, Jennifer worked with Sally on her oral hygiene. Sally indicated a commitment to use a periodontal aid each day since she has never really "taken to" floss.
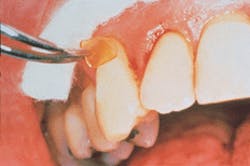
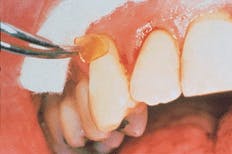
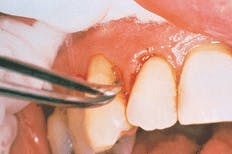
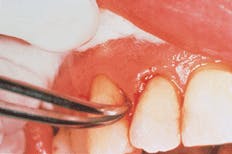
Jennifer then selected sites for the PerioChip. Sally concurred, and Jennifer began the scaling and root planing. She was glad she had budgeted two hours into the schedule. It had been five months since Sally`s last debridement, and there were deep pockets and some newly formed calculus. Then she dried #6 MB and #9 MB and quickly inserted the PerioChip in each site at the 6 mm pocket (see related photographs on the first page of this article). She repeated the same process on #31 ML, which also had a 6 mm pocket. She planned to carefully monitor all of Sally`s pocket depths. After booking an appointment in three months, Sally promised not to floss or use the periodontal aid at the PerioChip sites for 10 days, and promised to try to be diligent about consistently cleaning everywhere else.
At the three-month assessment, Sally arrived curious to see how things had changed with PerioChip, scaling and root planing, and her more diligent home care. After Jennifer conducted her usual examinations, with all findings within normal limits, she evaluated the gingiva and probed. There was resolution of many bleeding sites. Although many areas showed no change, there were several 1 mm to 2 mm reductions in pocket depth. The PerioChip-treated site at #31ML had improved from 6 mm to 4 mm. The 6 mm pocket at the MB#6 was now 4 mm. The MB#9 had improved to 5 mm; so after scaling she placed another PerioChip there. Sally re-appointed for three months later.
Unfortunately, Sally had to cancel the next three-month appointment. By the time she returned to the office it was time for the nine-month assessment. However, she assured the receptionist when she called that she was still practicing good oral hygiene at home. Upon Sally?s return, Jennifer completed the preliminaries and was pleased with the tissue appearance in many areas.
When the probing was complete, it was apparent that several areas stayed the same, some showed improvement, and a few were 1 mm deeper than last time. In looking at the PerioChip treated sites, MB#6 had remained at 4 mm. The 5 mm pocket at MB#9 was now 4, which was a 2 mm improvement from baseline, and the ML #31 also improved by 1 mm since the last visit, changing from 6 mm to 3 mm over the nine-month period.
As Jennifer reviewed Sally?s case over the nine months, she realized that her findings did resemble those in the original study; the PerioChip and scaled/root planed treated sites had pocket depth reductions of 2 mm or more. While there were some areas treated with scaling/root planing alone that showed a 2 mm reduction (DL#11 and MB#29), many more remained the same or showed a lesser improvement.
A week later, Jennifer and Dr. O sat down over the lunch hour with the charts of Paul and Sally. They reviewed what had transpired over the nine months to evaluate the effects of treatment with PerioChip. What they had hoped would happen ? greater pocket depth reduction ? did happen. Although adult periodontitis is not curable, they decided that the PerioChip could offer a viable and safe option to control disease for many of their clients. Jennifer finally felt like there was a treatment option which would enable her to take a more proactive role in achieving pocket depth reductions, enabling clients to better control plaque and disease.
Terri S.I. Tilliss, RDH, MS, MA, is an associate professor at the University of Colorado Health Sciences Center. Kimberly Krust Bray, RDH, MS, is an associate professor at the University of Missouri, Kansas City.
References available upon request.
Placement of PerioChip for Sally at MB #6.
Charting results for Paul
---------------------------
ML #2 DB #14
Baseline 6 7
3 months 5 4
6 months 5 4
9 months 4 4
Charting results for Sally
----------------------------------
MB #6 MB #9 ML #31
Baseline 6 6 6
3 months 4 5 4
9 months 4 4 3