Vitiligo
by Nancy Burkhart, RDH, EdD
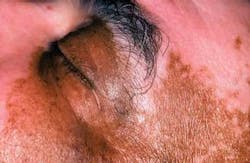
Clinical impressions: Your patient is a 46-year-old African-American male. Upon greeting him in the waiting area, you notice that he has heavy pink, pigmented areas on his face, hands, and neck region. You vaguely remember reading about this condition while in college. So, during the health history segment, you ask the patient if he is under treatment for the skin condition. As he begins to describe his condition, you slowly remember what you thought you had forgotten about vitiligo (see Figure 1).
Diagnosis: Vitiligo
Pathogenesis: Poliosis (the absence of or lessening of pigmentation) in the hair, scalp, brows, or lashes is due to a lack of pigment production. The pigment producing cells in the body are termed melanocytes. The melanocytes migrate to the basal cell layer of the tissues and, through dendritic processes of the melanocytes, allow granules to be transferred by melanosomes that extend close to the keratinocytes in the cell layers. The actual pigmentation process is determined by the process of the melanocytes and not by the increase in the number of the melanocytes. Vitiligo is a progressive disease of the epidermis (leukoderma). In vitiligo, the melanocyte is destroyed or absent. Therefore, the pigmentation process does not occur. Vitiligo may be localized or generalized with several subtypes.
Etiology: Generally, vitiligo is presented as a disorder of multifactorial etiology, associated with environmental, genetic propensity, and immunologic factors. The loss of pigmentation may be due to three causes: autoimmunity, autocytotoxic factors, or a neural hypothesis. Generally, a multifactorial etiology is accepted.
- Autoimmunity directed by antibodies with a possible breakdown in the immune surveillance system and, ultimately, melanocyte destruction
- Autocytotoxic factors such as chemical exposure may be toxic to melanocytes
- The neural crest theory is based on the origination of the melanocytes from the neural crest and the fact that certain disorders such as neurofibromatosis and tuberous sclerosis exhibit hypopigmentation.
Epidemiology: An estimated 1 to 2 percent of the world’s population has vitiligo. Vitiligo may occur in all age groups from infancy to older individuals. Studies by Dogra, et al. (2005) indicate a mean age of onset at 55+ years in a group of 182 patients. Handa and Kaur (1999) reported a mean age of 25 years in a group of 1,436 patients. The head and neck were reported as the most common site of occurrence followed by the upper limbs. No sex predilection is reported, but it is believed that more women seek treatment because of cosmetic concerns.
Method of transmission: There is no transmission factor associated with vitiligo. Vitiligo is an acquired disorder.
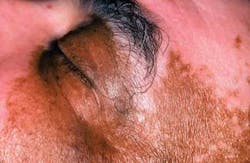
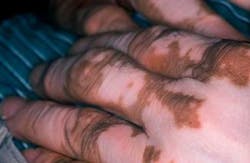
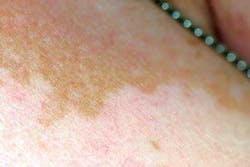
Extraoral characteristics: Vitiligo results from a loss of melanocytes in the involved skin areas. As seen in Figure 2, there is a distinct difference in his normally dark pigmentation in comparison to the less pigmented areas that appear as light pink. In contrast, the loss of pigmentation seen in Figure 3 is less noticeable in the skin of a Caucasian individual who has much lighter skin tones. The slightly tanned area of skin is her normal skin color with the lighter tones representing vitiligo. Vitiligo may go unnoticed in lighter skinned individuals in many instances due to the lack of contrast between areas of vitiligo and normal skin color. Vitiligo may present as single patches of depigmentation or more generalized whole body loss of skin pigmentation. Additionally, some patients report pruritic symptoms with vitiligo that result in inflammation or redness due to scratching.
Perioral and intraoral characteristics: Oral and perioral vitiligo is seldom reported in the dental literature. Perioral and lip vitiligo, however, may be relatively more common. Some authorities believe that oral vitiligo may be present more often than is actually reported. Because of the lighter mucosal color, the contrast is not as evident as the appearance seen on the skin. Oral mucosa is sparsely populated by melanocytes accounting for the lighter color. Additionally, there is a sun exposure factor related to the advancement of cutaneous vitiligo and, of course, sun exposure is not a factor in the oral mucosa.
Distinguishing characteristics: The stark difference in the pigmentation of the skin is usually the factor that sends the patient to a dermatologist in search of answers. Depending upon the skin’s appearance, the cosmetic factor can produce extreme self-esteem issues. Pinto (2005) addressed the self-esteem issues in children and cosmetic procedures are often warranted in these cases.
Differential diagnosis: Vitiligo may be associated with other autoimmune type diseases, hypothyroidism, diabetes mellitus, pernicious anemia, Addison’s disease, and alopecia areata. Several disorders may be considered in a differential diagnosis: cheilitis, traumatic scarring, and some mucosal disease states such as lichen planus.
Treatment: Cutaneous vitiligo is advanced by sun exposure so the use of a high SPF sunscreen is prescribed and limiting sun exposure is highly suggested. Vitiligo is progressive so carefully monitoring the patient is necessary.
Tattooing, skin grafts, topical PUVA, and laser treatment are often used in treatment and cosmetic procedures. Mediations such as calcipotriene, tacrolimus (Protopic), trioxsalen, prednisone, or triamcinolone may be used depending upon the severity. No one treatment works for all patients, therefore, the treatment must be individualized.
Prognosis: The correct diagnosis and follow-up is crucial. Since other autoimmune disease states may occur, the patient is carefully monitored.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor in the Department of Periodontics at Baylor College of Dentistry and Texas A & M Health Science Center in Dallas. Nancy is also a co-host of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She is the co-author of General and Oral Pathology for Dental Hygienists, published by Lippincott Williams & Wilkins in Baltimore in October 2007. She can be contacted at [email protected].
References
- Dogra S, Parsad D, Handa S, Kanwar AJ. Late onset vitiligo: as study of 182 patients. Int J Dermatol. 2005 Mar; 44(3):193-6.
- Handra s, Kaur I. Vitiligo: clinical findings in 1436 patients. J Dermatol. 1999 Oct; 26 (10):653-7.
- Kar PK. Vitiligo: as study of 120 cases. Indian J Dermatol Venereol Leprol. 2001 Nov-Dec; 67(6):302-4.
- Mahajan BB, Garg G, Gupta RR. Evaluation of cosmetic tattooing in localized stable vitiligo. J Dermatol. 2002 Nov; 29(11):726-30.
- Pinto A. Pediatric soft tissue lesions. Dent Clin North Am. 2005 Jan; 49(1):241-58.
- Regezi J.A, Sciubba J.J., Jordan R. C .K. Oral Pathology: Clinical Pathologic Correlations. Saunders, St. Louis MO. 2003
- Spritz RA. The genetics of generalized vitiligo and associated autoimmune diseases. J Dermatol Sci, 2006 Jan; 41(1):3-10.