Second nature: Incorporating natural, biocompatible products into your periodontal protocol
As lifelong learners, dental hygienists are positioned to incorporate the most recent best practices into their periodontal protocol and restructure how procedures are delivered in specific clinical settings. This article will examine recent findings that suggest changes are needed in the use of traditional products used in periodontal therapy, and look at the ingredients, indications, and modes of action for several nontoxic, biocompatible agents that are potential alternatives.
Current practices and challenges
Nonsurgical periodontal therapy remains a critical component of dental hygiene practice. Patients rely on dental hygienists to deliver thorough instrumentation; provide education surrounding the importance of sound self-care practices; and recommend adjunctive therapies that will promote optimal treatment outcomes: namely, a reduction in bleeding and probing depths. Following nonsurgical periodontal therapy, it is customary for clinicians to place a variety of chemotherapeutic agents into periodontal pockets to reduce bacteria, thereby creating an environment conducive to healing. While the primary goals of periodontal therapy have remained unchanged in recent years, the latest research has demonstrated that some off-label uses of previously popular agents are contraindicated, as will be discussed further below.
Natural products provide a potential solution to this challenge. Among the general public, natural products continue to gain popularity, and dental manufacturers have responded to this trend. However, as natural products become more available, it is important for dental hygienists to adapt while still using evidence-based research to provide the highest standard of care.
Recent findings
For decades, dental hygienists have delivered in-office nonsurgical periodontal therapy by irrigating or mechanically placing chemotherapeutic agents into periodontal pockets. As the American Academy of Periodontology states, “These agents may be used to reduce, eliminate, or change the quality of microbial pathogens; or alter the host response through local or systemic delivery of appropriate agent(s).”1 One such agent is a 0.12% chlorhexidine gluconate rinse, which has been used to irrigate gingival tissues immediately following instrumentation. While chlorhexidine can still be prescribed to reduce gingival inflammation (its official use), it is contraindicated for irrigation immediately following scaling and root planing due to its tendency to inhibit reattachment of the junctional epithelium. In the article, “The Effect of Chlorhexidine Treatment of Root Surfaces on the Attachment of Human Gingival Fibroblasts In Vitro,” the authors caution against using chlorhexidine for irrigation purposes due to its role in preventing reattachment: “Exposure of root surfaces to chlorhexidine significantly inhibits subsequent fibroblast attachment which may interfere with regeneration of the periodontium. Hence, the data suggest that efforts should be made to minimize Chlorhexidine contact with the root surface with physical barriers.”2
Considering this recent research, nontoxic products that are free of allergens have garnered more attention by dental professionals. Many clinicians have accepted that anti-inflammatory irrigants used in periodontal therapy are not “one size fits all,” but there remains uncertainty regarding the selection of the appropriate agent for each patient. Below is a closer look at several natural, or more holistic, products that have been used for irrigation, rinsing, and postsurgical wound healing.
Xylitol
Botanicals
The three herbs used in PeriActive are:
- Centella asiatica (gotu kola), which has been shown to increase effective collagen and is used in wound healing;5
- Sambucus nigra (black elderberry), which inhibits proinflammatory properties of two periodontal pathogens (Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans);6 and
- Echinichia purpurea (purple coneflower), which has antiviral, antibacterial, and anticytotoxic effects.7
The manufacturers of PeriActive rinse outline the recommended uses as “for those have who to tendency or/and gingivitis periodontitis, surgically post implant-placement, after periodontal surgery or surgical extractions, and for under inflammation around or dentures implants.”8
StellaLife
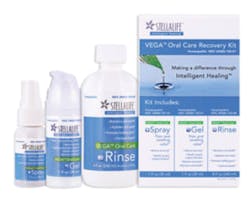
Major shifts in postoperative pain management have led to the use of homeopathic therapies in clinical practice. StellaLife’s Vega Oral Care Recovery Kit (figure 4), as well as other rinses and gels, have been adopted by many practices as adjunctive aids that promote wound healing following third molar extraction and periodontal surgery.
As alternatives to the prescription of narcotic pain medications, nonsteroidal anti-inflammatory drugs, acetaminophen, and a homeopathic recovery kit have been used for pain management for patients undergoing various oral surgery procedures.13 Tatch concluded that “The Vega Oral Care Recovery Kit may provide a natural alternative to steroids and narcotic pain medications while accelerating healing in patients undergoing various dental procedures.”14
Conclusion
As lifelong learners, dental hygienists must tailor their recommendations according to recent literature and individual patient presentation. Products that demonstrate potential benefits for our patients following the delivery of initial periodontal therapy are continuously changing and evolving. Many agents that are more natural in composition are beginning to attract both consumers and dental professionals due to their potential benefits. Recommendations regarding appropriate agent selection have transformed in recent years. However, the usage of newer agents is less than widespread at present. The conversation must continue for dental hygienists to stay current and maintain a working knowledge of the safety and efficacy of new products. Ultimately, a working knowledge of available homeopathic agents will strengthen trust between patients and providers.
References
- American Academy of Periodontology. Guidelines for periodontal therapy. J Periodontal. 2001;72(11):1624-1628. https://doi.org/10.1902/jop.2001.72.11.1624
- Alleyn CD, O’Neal RB, Strong SL, Scheidt MJ, Van Dyke TE, McPherson JC. The effect of chlorhexidine treatment of root surfaces on the attachment of human gingival fibroblasts in vitro. J Periodontal. 1991;62(7):434-438.
- Goldstep F. Oral rinses for periodontal health: Simplified. Oral Health website. https://www.oralhealthgroup.com/features/oral-rinses-for-periodontal-health-simplified/. Published December 1, 2014. Accessed November 29, 2019.
- Park E, Na HS, Kim SM, Wallet S, Cha S, Chung J. Xylitol, an anticaries agent, exhibits potent inhibition of inflammatory responses in human THP-1-derived macrophages infected with Porphyromonas gingivalis. J Periodontal. 2014;85(6):e212-223.
- Shetty BS, Udupa SL, Udupa AL, Somayaji SN. Effect of centella asiatica L (Umbelliferae) on normal and dexamethasone-supressed would healing in wistar albino rats. Int J Low Extr Wound. 2006;5(3):137-143.
- Harokopakis E, Albzreh MH, Haase EM, et al. Inhibition of proinflammatory activities of major periodontal pathogens by aqueous extracts from elder flower (Sambucus nigra). J Periodontol. 2006;77(2):271-279.
- Woelkart K, Marth E, Suter A, et al. Bioavailability and pharmacokinetics of Echinacea purpurea preparations and their interaction with the immune system. Int J Clin Pharm Th. 2006;44(9):401-408.
- The Izun PeriActive Oral Rinse: a breakthrough treatment for gingivitis. Izun Oral Care website. http://izunoralcare.com/media/downloads/PeriActive-White-Paper.pdf. Accessed November 22, 2019.
- Tatch W. Natural adjunct to post-operative management after third molar surgery. Oral Health website. https://www.oralhealthgroup.com/features/natural-adjunct-post-operative-management-third-molar-surgery/. Published June 30, 2017. Accessed December 1, 2019.
- Seeley BM, Denton AB, et.al. Effect of homeopathic Arnica montana on bruising in face-lifts: results of a randomized, double blind, placebo-controlled clinical trial. Arch Facial Plast Surg. 2006;8(1):54-59.
- Akhtar N, Zaman SU, Khan BA, Amir MN, Ebrahimzadeh MA. Calendula extract: effects on mechanical parameters of human skin. Acta Pol Pharm. 2011;68(5):693-701.
- Srivastava JK, Pandey M, Gupta S. Chamomile, a novel and selective Cox-2 inhibitor with anti-inflammatory activity. Life Sci. 2009;85:663-669.
- Tatch W. Opioid prescribing can be reduced in oral and maxillofacial surgery practice. J Oral Maxil Surg. 2019;77(9):1771-1775.
- Tatch W. Natural adjunct to post-operative management after third molar surgery. Oral Health website. https://www.oralhealthgroup.com/features/natural-adjunct-post-operative-management-third-molar-surgery/. Published June 30, 2017.
Lauren Haperman, BSDH, RDH, PHDHP, is a practicing dental hygienist in Richmond, Virginia. She is currently pursuing a master of science degree in dental hygiene through the University of Bridgeport. Her passions include promoting diversity, equity, and inclusion within the profession; periodontal therapy; and public health. She welcomes your feedback and may be reached at [email protected].
About the Author

Lauren Hapeman, BSDH, RDH, PHDHP
Lauren Hapeman, BSDH, RDH, PHDHP, is a practicing dental hygienist in Richmond, Virginia. She is currently pursuing a master of science degree in dental hygiene through the University of Bridgeport. Her passions include promoting diversity, equity, and inclusion within the profession; periodontal therapy; and public health. She welcomes your feedback and may be reached at [email protected].
Updated February 4, 2020