Removing stains from teeth: A guide for clinicians and patients
Part of the dental hygienist’s clinical assessment is determining what type of stain the patient presents with and how best to remove it. Clinicians should understand the etiology and appearance of the various types of stains. This will help them determine whether a stain can or cannot be removed through powered and/or manual instrumentation and polishing. This can also be communicated to patients to aid in their oral self-care regimens at home.
Classification of stains
Stains and other discolorations happen in one of three ways: 1) adhering directly to the tooth surface, 2) found within the calculus or soft deposit itself, or 3) found directly inside the tooth or restorative materials. The former two types of stains can be removed through scaling and polishing; the latter type of stain requires other methods or cannot be removed at all. Some of these stains might be prevented by changes in the patient’s home-care and dietary habits.
Stains are primarily a cosmetic problem. Any negative effect on teeth or gingiva is related to the biofilm or calculus on which the stain occurs. Thick deposits of stain could provide a rough surface on which biofilm can collect, while certain stains provide a means of evaluating oral cleanliness and the patient’s habits.
Stains can be classified by location (extrinsic or intrinsic) and source (exogenous and endogenous).1-3 Extrinsic stains occur on the external surface of the tooth and can be removed by self-care methods (such as brushing and flossing) and scaling and polishing (traditional or air polishing).1-4 Intrinsic stains occur on the internal surface of the tooth and cannot be removed by self-care methods.1,4 Exogenous stains originate from sources outside of the tooth and may be extrinsic or intrinsic.1-4 Endogenous stains originate from within the tooth and are always intrinsic;1,3 endogenous stain is usually discolored dentin reflected through the enamel.1
Exogenous extrinsic stains
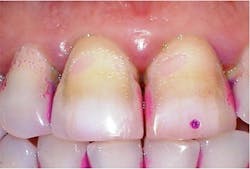
The most common extrinsic stain is yellow stain.1 Clinically, it appears as a dull, yellowish discoloration of plaque (figure 1). Its distribution on tooth surfaces can be generalized or localized. It can be found in people of all ages and is most commonly noted when the patient’s oral hygiene is poor or neglected. The yellow color can be attributed to food pigments.1 Yellow stain can be removed through powered and manual instrumentation as well as polishing procedures. Improved oral self-care can lead to reduction in its accumulation.
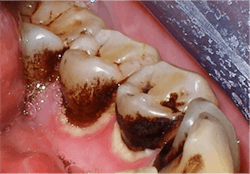
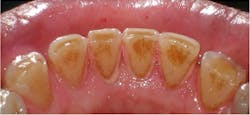
The second most common stain is brown stain.1 Clinically, it may range in appearance from light to dark brown or black and may appear leathery. Brown stain is distributed primarily on the cervical third of lingual tooth surfaces but may extend to the middle third. The deposits increase with poor oral self-care or neglect. Brown stain is primarily caused by smoking or chewing tobacco, hookah, and marijuana use1-4 (figure 2). Other brown stains are caused by stannous fluoride, foodstuffs (coffee, tea, soy sauce), betel nut chewing, swimmer’s stain (from frequent exposure to chlorinated or brominated pool water), and antiplaque agents (chlorhexidine gluconate mouth rinse) (figure 3).1,3,4 The best way to prevent brown stain is to reduce or eliminate the cause of the stain. It can also be reduced by improved oral self-care. Removal is accomplished with powered and manual instrumentation as well as polishing.
Fun fact: Betel nut has a caries-inhibiting effect, but the oral cancer risk outweighs any possible advantage.1
Green stain can be very difficult to remove. Its clinical appearance ranges from light or yellowish green to very dark green stain embedded in plaque. It may be found on the gingival crest, enamel grooves, or the entire facial surface, but it is mainly found on the facial third of maxillary anterior teeth. Green stain is primarily found in children, but it may occur at all ages. Green stain is attributed to poor oral self-care, resulting in the accumulation of chromogenic bacteria and fungi, as well as blood pigments from hemoglobin being decomposed by bacteria.1-4 It may be removed through powered and manual instrumentation and polishing procedures. Improved oral self-care can lead to reduction of green stain.
Fun fact: Stain from marijuana may appear to have a grayish-green hue.1
Black line stain, also known as mesenteric stain, is most common in women and children, but can occur at all ages. It is composed primarily of gram-positive rods.1 Clinically, it appears as a continuous fine black line (with no appreciable thickness) that follows the gingival crest; the rest of the mouth is clean, and the gingiva is healthy.1,3 It is found mainly on the lingual and proximal surfaces of maxillary posterior teeth. Its etiology is thought to be related to a natural tendency; the stain’s attachment to the tooth is by a pellicle-like structure, possibly related to body chemistry. Black line stain may be reduced with improved oral self-care.
Orange and red stains are rare, with red stains being rarer than orange stains, and occur from antibiotic use.1,3 The antibiotics alter the normal flora, allowing chromogenic bacteria to grow and accumulate at the cervical third on the facial and lingual of anterior teeth, resulting in the orange and/or red stain. Orange and red stains can be removed through mechanical instrumentation and reduced by improved oral self-care.
Stains from metals can have different clinical appearances. Copper or brass stains will appear green or bluish green, while iron may present as brown to greenish brown or black. Nickel appears as green, cadmium as yellow or golden brown, with lead ranging from gray to black. Metal stain is usually found on the cervical third of anterior teeth. The stain is caused by the inhalation of dust or metallic salts from working in the metal industry; workers should wear masks to protect themselves from exposure. Metal stain can also be attributed to the topical effect of some drugs, such as liquid iron consumption. Taking the medication through a straw or in tablet/capsule form will minimize direct contact with the teeth.1-4
Exogenous intrinsic stains
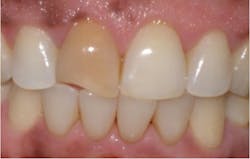
When intrinsic stains come from an outside source, the stain is called exogenous intrinsic. Exogenous extrinsic stains from tobacco, tea, coffee, wine, and green stains can become exogenous intrinsic over time, especially if the stain is not removed regularly. Restorative materials such as amalgam (figure 4), silver nitrate, and other endodontic materials, can become intrinsic.1-4 Topically applied stannous fluoride may stain pits and grooves of posterior teeth and the cervical thirds of the facial surfaces of anterior teeth, penetrating through and become intrinsic. Dark green stain can sometimes become embedded in the surface enamel. This enamel may become demineralized due to cariogenic biofilm. In these instances, appropriate fluoride treatment is recommended.
Endogenous intrinsic stains
Not all pulpless teeth discolor, but those that do may have a light yellow-brown, slate gray, reddish-brown, dark brown, bluish-black, orange, or greenish tinge (figure 5). The color comes from the decomposed pulp, usually caused by trauma.1,2 Other endogenous intrinsic stains may be caused by imperfect tooth development due to either genetic abnormalities or environmental influences.
Genetic abnormalities that lead to endogenous intrinsic stains include amelogenesis imperfecta, in which the tooth enamel is missing because of ameloblast disturbance and the teeth become yellow-brown or gray-brown, and dentinogenesis imperfecta (figure 6), in which odontoblastic disturbances cause the teeth to fracture easily and the teeth appear translucent and opalescent, varying in color from gray to bluish-brown.1,4
Enamel hypoplasia can cause endogenous intrinsic stains presenting as generalized or local hypoplasia. Systemic hypoplasia is white spots and/or pits in the enamel caused from a disturbance in the formation of the organic matrix (figure 7). It can be from systemic causes such as syphilis; high fever diseases such as measles, chicken pox, or scarlet fever; malnutrition; premature birth; or idiopathic causes.1,3,4 The spots usually occur on the first molars and canines. When congenital syphilis is the cause, it may alter the shape of the teeth, forming peg laterals called Hutchinson’s incisors, or mulberry molars. Local hypoplasia usually occurs from trauma to a developing tooth bud, resulting in white spots and/or pits on the tooth affected. The white spots may stain easily.1,3
Dental fluorosis is caused by the ingestion of excessive fluoride ion in drinking water (more than 2 parts per million) during tooth formation. The enamel is altered because fluoride is toxic to ameloblasts.1,2,4 Important to note is that fluorosis cannot occur if the teeth are already formed. Severity of fluorosis is related to the age of the patient when exposed and the dose of the fluoride exposure. Optimal fluoride levels can range from 0.7 to 1.2 parts per million (ppm), depending on the climate (the colder the climate, the higher the concentration). Today, 0.7 ppm is the generally accepted optimal level.
Tetracycline use can result in endogenous intrinsic staining of the teeth when the drug is administered during the third trimester of pregnancy or to a child during infancy or early childhood.1-4 The severity of the stain depends on the dosage and length of time the tetracycline was ingested. Tetracycline stain is limited to the parts of the teeth that were developing at the time of the drug’s administration.
Having a working knowledge of the various types of dental stains can assist the clinician in determining the best way to remove the stains and in educating the patient in stain prevention methods. Exogenous extrinsic stains can be removed by the patient and the clinician; endogenous intrinsic stains cannot by removed by traditional stain removal methods. The clinician and the patient working as cotherapists can determine the best way for patients to minimize stain production.
Editor's note: This article appeared in the April 2022 print edition of Dental Economics magazine. Dentists in North America are eligible for a complimentary print subscription. Sign up here.
References
1. McConnell CA. Dental soft deposits, biofilm, calculus, and stains. In: Boyd LD, Mallone LF, Wyche CJ. Wilkins’ Clinical Practice of the Dental Hygienist. 13th ed. Jones & Bartlett; 2021:293-299.
2. Stefan SA. Biofilm, calculus, and stain. In: Henry R, Goldie MP. Dental Hygiene Applications to Clinical Practice. FA Davis Company; 2016:235-236.
3. Francis B, Barnes CM. Cosmetic and therapeutic polishing. In: Daniel SJ, Harfst SA, Wilder RS. Mosby’s Dental Hygiene Concepts, Cases, and Competencies. 2nd ed. Elsevier, Inc.; 2008:600-607.
4. Watts A, Addy M. Tooth discolouration and staining: a review of the literature. BDJ. 2001;(19):309-316.
About the Author

Becky Smith, EdD, CRDH, FADHA
Becky Smith, EdD, CRDH, FADHA, worked as a public health dental hygienist on a Native American Indian reservation for 10 years before moving to private practice. Currently, Dr. Smith is a professor at Miami Dade College, where she has been teaching since 2005. Her areas of specialty are periodontology and preclinical and clinical dental hygiene. She enjoys all things Disney, reading, movies, traveling, and being a mom to her daughter Arielle and her four-legged family members.