Dealing with Benefit Denials
BY DIANNE GLASSCOE WATTERSON, RDH, BS, MBA
Dear Dianne,
I've been a hygienist for 20 years in the same office. Our doctor is great to work with, plus he does excellent dentistry. However, one of the most frustrating realities today is that so many of our patients want only what insurance will pay for.
Recently, I had a patient with early periodontal disease around her mandibular molars with bleeding and 5 mm pockets. When we did the insurance pre-authorization, the treatment was denied.
How do these insurance companies get away with denials like this? And what options are left for me as a hygienist to help this patient? I really care for my patients, and I know what needs to be done to bring this problem under control. But it seems like our hands have been tied by this third party entity that has never even looked in this patient's mouth. Any suggestions?
Janice, RDH
Dear Janice,
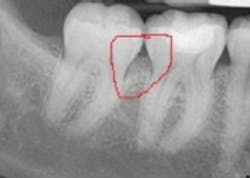
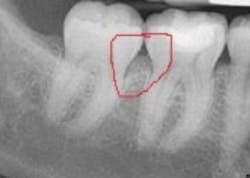
Recently, I was consulting in an office, and the insurance coordinator brought to me a situation almost identical to the one you have described. The hygienist had identified early periodontitis around some posterior teeth with 5 mm pocketing and bleeding. The patient's benefit carrier had denied coverage, stating insufficient bone loss. When I looked at the radiographs, I noticed the loss of bone definition in the molar areas, which is indicative of early periodontitis. There were not blatant vertical defects, yet the bone loss was evident. The X-ray is shown below.
Sometimes, we can help our patients by becoming their advocate. So, I helped the insurance coordinator compose a letter of appeal to the benefits carrier. We called attention to the obvious lack of bone definition in the interproximal areas in question. We also made our case that successful intervention in early stages is a far superior option vs. waiting until bone loss advances to deeper levels. The areas in question needed definitive periodontal care in order to intercept the disease process now rather than later.
According to Dr. David Pettigrew, here are the top 10 reasons that insurance claims are denied:
1. Incomplete/inaccurate/unreadable claim information. This is by far the No. 1 reason for claims being denied, delayed, and returned. |
2. Missing tooth clause. Once treatment extends beyond simple restorative to crowns, fixed or removal prosthesis, implants, etc., it is best to file a predetermination so everyone knows his/her fiduciary responsibility up front. |
3. Contractual clinical denials. Some dental contracts just do not cover certain services. |
4. Contractual limitation denials. These are nonclinical circumstances that do not allow payment of benefits. Examples include age of the patient, frequency, and waiting periods. |
5. Unreadable documentation. X-rays and charting that are difficult to read or interpret cause many claims to be delayed or denied. |
6. Student verification. Many claims are delayed because of inadequate documentation of a student's status. |
7. Nonresponse from office. Ensure that your office has a process that tracks and addresses insurance company inquiries in a timely manner. |
8. No explanation for replacement. Just because a crown or fixed or removable bridge is over the contractual frequency time limit does not mean that it is eligible for replacement. |
9. Incorrect CDT coding. If you use any other codes, or old discontinued codes, expect those services to be denied. |
10. Duplicate service. Inquire about the old claim rather than file a new one to prevent the second one being processed as a duplicate of the first and not paid. |
Amazingly, the benefits carrier approved the treatment following our letter of appeal.
Benefit providers hire people to review claims. Sometimes the reviewers are dentists that work either full or part-time reviewing claims or pre-authorizations. If the reviewer has a large caseload, claims may not get a thorough review or even a close scrutiny of documentation. In the aforementioned case, the bone loss does not appear as a clear vertical defect, but rather as a "fuzzy" area in the interproximal space. In the early stages of periodontitis, early bone loss will show up as loss of bone definition (such as loss of lamina dura).
Unfortunately, fraudulently reporting of periodontal treatment when bone loss is not evident radiographically is far too common. Just check out a few of the state board websites to see what disciplinary actions have been taken, and you are sure to find fraudulent reporting of periodontitis when the actual treatment rendered was a prophylaxis. Insurance consultants are always on the alert for situations involving "upcoding."
-------------------------------------------------
Other articles by Watterson
-------------------------------------------------
As a result of a few bad apples, the trend is to deny benefits for anything that is not blatant. Early periodontitis is not blatant; it is subtle clinically and radiographically.
When benefit carriers deny coverage for procedures, sometimes it is necessary to get the patient involved. Patient complaints to an employer-sponsored benefits coordinator may carry more weight than complaints from dental professionals.
My personal experience involved payment for a crown I had done on #30. The tooth in question hurt every time I bit down on something. There was no radiographic evidence of decay or fracture, and it was not temperature sensitive. However, there was a large amalgam filling. My dentist suspected a fracture and recommended a crown. After the crown was placed, I had no more biting pressure pain. However, my benefits carrier refused payment, citing no evidence of decay or fracture.
I wrote a personal letter, stating the former pain associated with biting was completely eliminated after having the crown done. The claim was paid the following week! If I had not complained, there's no doubt the claim would have never been paid by my benefits carrier.
The past few years have brought some striking changes in our relationship with third party payers. We've evolved (or devolved) into an adversarial relationship, and many have come to view third party payers as the enemy. Our love affair with "dental insurance" has turned into an "abusive lover" situation that goes so far as to mandate what we can charge if we want to be one of "their" providers.
Reimbursement rates have not kept pace with rising costs associated with providing high-quality dental care, and some reimbursements have even been reduced. We've allowed the payers to intrude into our practices and dictate care. Not only do they engage in denying treatment, but they lead our patients to feel that we are overcharging them when they state on the estimate of benefits statement "the provider's fees exceed the reasonable and customary." The patient is often caught in the middle of a continual struggle between the dentist and benefit payer. It's a sad state of affairs, and it seems to be getting worse instead of better.
When patients are insurance dependent, and the insurance denies a necessary treatment such periodontal therapy, here are my suggestions:
• Write a letter of appeal on behalf of the patient to the benefits carrier.
• Get the patient involved.
• Ramp up the patient's home care routine by implementing a Water Pik for twice daily use. Instruct the patient to put a few drops of sodium hypochlorite in the water two to three times weekly to help with microbial control, and direct the spray into the sulcus.
• Increase the patient's professional care to every three months.
• Take time to discuss the progression of this chronic infection to help the patient understand the urgency of interceptive treatment now rather than allowing the disease process to continue. If your patient fully understands, he may opt to pay out-of-pocket.
All the best,
Dianne RDH
DIANNE GLASSCOE WATTERSON, RDH, BS, MBA, is a professional speaker, writer, and consultant to dental practices across the United States. Dianne's new book, "The Consummate Dental Hygienist: Solutions for Challenging Workplace Issues," is now available on her website. To contact her for speaking or consulting, call (301) 874-5240 or email [email protected]. Visit her website at www.professionaldentalmgmt.com.