Another tool to help reduce gingivitis: Toothpaste encourages gingival health prior to restorations
By Todd C. Snyder, DDS, AAACD
Virtually every type of restorative dentistry performed requires a healthy and dry environment in which to work. Everything from sealants, composites, indirect restoration preparations, impressions, cementation, root canals, and more require some type of moisture control measures to be implemented for the highest level of success. Various fluid contaminants that constantly challenge restorative therapies consist of saliva and crevicular fluids.
These are some of the most prevalent and yet easiest fluids to control. Blood, however, is probably one of the most challenging fluids to manage during many treatment modalities. Sometimes bleeding is due to iatrogenic trauma during a procedure and often could have been avoided. Gingivitis and periodontal disease are to blame for many of the fluid management issues that dentists typically deal with when it comes to bleeding during restorative dental work. There are numerous different ways to combat bleeding, such as the use of different medications, cautery devices, lasers, and local astringents.
The majority of patients who come into dental practices have at minimum some localized gingivitis. Research states that 75% of Americans have some form of either gingivitis or periodontal disease.1 Many of these patients may require only routine cleanings two to three times a year while others need more aggressive periodontal therapies.
Dental professionals, in addition to using hand instruments and technological devices, may use localized antibiotics, prescribe various types of oral rinses (some of which can stain teeth), or recommend prescription-strength dentifrices to reduce or eliminate gingivitis. Prior to starting restorative care, a patient ideally should have a healthy periodontal status and absence of gingivitis near the treatment area so as to decrease bleeding when placing direct or indirect adhesive restorations, or taking impressions for indirect restorations.
The benefit of maintaining healthy gingival tissues while in provisional restorations means it is significantly easier to place indirect restorations without having to manage bleeding. I was introduced to a new modality this year, Premier's Enamelon preventive treatment gel. I've been evaluating Enamelon's ability to assist with the treatment of gingivitis in my patients. We are also conducting research to evaluate Enamelon's ability to protect teeth from acid attacks and tooth decay.
New patients often receive an exam and cleaning at their first appointment. Many offices offer oral hygiene instructions and a complimentary bag containing a toothbrush, floss, and toothpaste. Our office has been implementing the use of Enamelon for some of our new patients, and we've been seeing improvement in the health of the gum tissues during restorative dental work.
As dentists, we typically provide many cosmetic and restorative dentistry services that require provisional restorations to be placed for weeks at a time. We want to have healthy tissues to facilitate better composite bonding, impressions, adhesion, and seating of restorations. Enamelon appears to help minimize the level of gingival inflammation during provisionalization on restorative procedures such as veneers and crowns in both the posterior restorations and anterior cosmetic area.
First Case Study
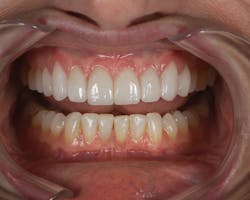
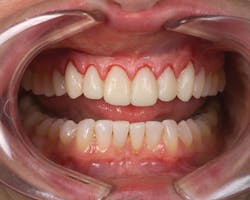
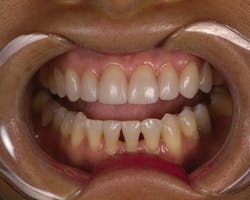
Here is an example of one of our many restorative cases in which a patient with existing veneers presented with very irritated and bulky tissues (Figure 1) that actually got healthier during the provisionalization. Typically cases get worse while patients are wearing provisionals because of the inability to floss and clean well.
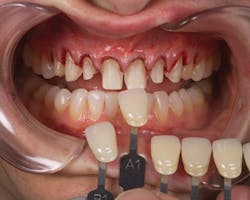
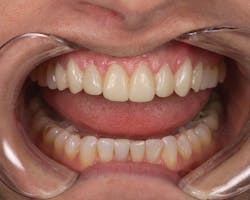
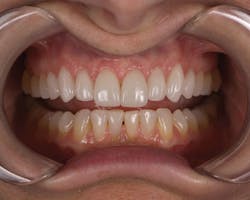
After the prep and temporization appointment (Figures 2, 3), the patient was instructed to use the Enamelon toothpaste in place of his existing dentifrice and to use the preventive treatment gel once a day (typically at bedtime) after brushing.
Figure 1
Figure 2
Figure 3
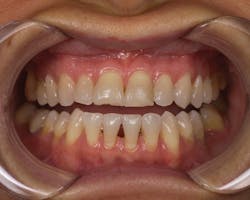
Figure 4
Figure 5
Upon evaluation of the patient at the delivery appointment (Figure 4), the tissues were actually healthier and substantially less inflamed around the provisional, making the delivery process far easier than it would have been had there been bleeding and inflamed tissues.
Figure 5 shows the final veneers cemented in place, and the photo was taken immediately after delivery. Notice the lack of gingival bleeding or irritation as compared to that in Figure 1.
Second Case Study
We have found in many of our large cases, such as the one mentioned here, as well as our everyday simple fillings and single-crown restorations, that we have less bleeding and irritated tissues to contend with after implementing Enamelon into our hygiene department's treatment protocols.
Figures 6 and 7 show a pre- and postop photo of another veneer case in which Enamelon was recommended for daily home use after the preparations, impressions, and temporization. One can easily see how much tighter and healthier the tissue appears in figure 7 after the patient used Enamelon for at least two weeks, which makes the veneer delivery appointment more predictable, efficient, and esthetic.
Figure 6
Figure 7
Performing dental procedures and placing various types of restorations typically require a contaminant-free environment for materials to perform optimally. To that end we always want to have a healthy periodontium prior to beginning restorative therapy-not that it is always possible, but in a perfect world it would be great to work with healthy tissues. There are many different ways in which to obtain a healthier periodontium-various types of in-office cleanings, lasers, antibiotics, medications, oral rinses, pastes, etc.
Most of these modalities have to be used under the care of a dentist at his or her facility or via a prescription. Electric toothbrushes, dental floss, and oral rinses can be enough to minimize the risks of bleeding by decreasing or even eliminating gingivitis. Premier has gone a step further to create a toothpaste that has been reported to help reduce gingivitis. RDH
Todd C. Snyder, DDS, received his doctorate in dental surgery at the University of California at Los Angeles School of Dentistry. It is there that he co-developed and co-directed the first and only comprehensive two-year postgraduate program in esthetic and contemporary restorative dentistry. Dr. Snyder is a member of Catapult Elite, an international speakers consortium. He lectures nationally and internationally on numerous aspects of dental materials, techniques, occlusion, technology, and practice management. Dr. Snyder has been on the faculty at UCLA, and is currently on the faculty at Esthetic Professionals. Additionally, Dr. Snyder is a consultant for numerous dental manufacturing companies and has had the opportunity to research and recommend changes for many of the materials now being used in dentistry.
References
1. http://www.nytimes.com/health/guides/disease/gingivitis/risk-factors.html