Oral Health Solutions with Clear Aligner Therapy: Three case studies show benefits of proper tooth alignment
Three case studies show benefits of proper tooth alignment
BY Ben Miraglia, DDS, and Lauren Gueits, RDH, BS
Orthodontics is an essential component of comprehensive care. The following cases demonstrate how patients benefit from providing orthodontic solutions to orthodontic problems. Hygienists are an integral component to instilling the value of tooth alignment and proper occlusion to patients. Orthodontics has become a readily acceptable option for adult patients due to the availability of clear aligner therapy. The value of the therapy is not based on the obvious esthetic benefits of "straight" teeth, but rather the functionality of a healthy occlusion. Doctors have been very successful in treating patients with clear aligner therapy to prevent the possible consequences of malocclusion: occlusal wear, abfractions, incipient decay, periodontal disease, and even TMD symptoms.
The authors collaborated to share remarkable case studies below, which exemplify patients' success, good health, and improved well-being. Clear aligner therapy started as a result of a team approach during hygiene treatment.
Dr. Miraglia: First aha moment
One patient has impacted me more than any other during my 22 years in private practice. His name is Evin, and he first visited our office on Oct. 17, 2005. He had not received dental care for five years. He had a two-hour session with my hygienist. The first hour was for diagnostic records. The second hour began his necessary dental hygiene protocols.
---------------------------------------
Related articles
- Orthodontic tooth movement with clear aligners: seeing results with the invisible
- Invisalign in the PPO general practice: How a reluctant provider earned $300,000 in 9 months
- Thursday Troubleshooter: Can this dental office upcharge on a PPO fee for Invisalign?
---------------------------------------
I prescribed nonsurgical periodontal therapy. At five weeks into our hygiene care, Evin was beginning to heal, thanks to the removal of the plaque and calculus and his excellent home care. Evin's next step would be a consultation to discuss his malocclusion.
Evin returned for the consultation, and we discussed his original periodontal condition, his bleeding gums, recession, calculus, and pocket depths. We also discussed the improvements he was experiencing due to his hygienist's efforts and his much improved home care. Then I taught Evin about his bite and explained that his teeth were connecting in ways that contributed to his periodontal condition.
Evin learned that his bite was poor and destructive to the teeth, gums, bone, jaw joint, and surrounding muscles. We learned that Evin never had braces as a teenager. I explained that utilizing orthodontics to position the teeth and bite correctly would make a significant difference in the overall health, stability, and longevity of his teeth and gums. We discussed the existing damage and could not guarantee a full recovery. Evin was advised that he might need to be referred to the periodontist for any residual recession of tooth No. 23.
At age 23, braces were not appealing to Evin, so our discussion turned toward the benefits of clear aligner therapy to correct his bite. Evin accepted the treatment recommended, and we acquired the necessary impressions, submitting his case for aligner manufacturing. From the start, our intent was to move all 28 teeth into proper position and achieve a good overbite and overjet, and intercuspation of the posterior teeth with no interferences.
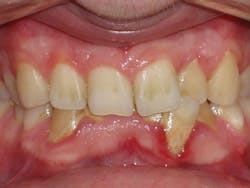
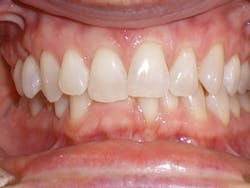
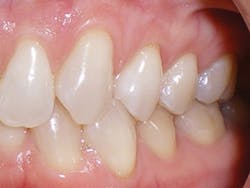
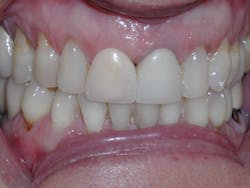
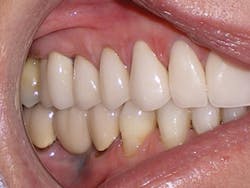
Four weeks later, Evin began his clear aligner treatment (see Figure 1). He was seen for follow-up clear aligner visits at six-week intervals until his treatment was completed. During his clear aligner treatment, Evin maintained three-month recalls with the hygienist. His home care was excellent, in part due to the benefit of aligners being removable.
The six-week follow-up visits with Evin were eye-opening! I had the opportunity to observe his periodontal condition improve at each interval. After 30 aligners, or 15 short months, Evin's clear aligner orthodontic treatment was completed and final photos were taken. His bite was checked to confirm we had achieved our initial goal. Evin now had the appropriate overbite, overjet, and class I occlusion with proper posterior intercuspation with no interferences.
Figure 1
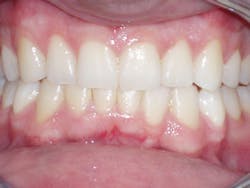
His healthy occlusion was reflected in his gum tissue. Evin finished with nearly a full resolution of his periodontal deterioration. What was originally swollen, inflamed, and bleeding gum tissue that had lost most of its gingival architecture was now very healthy and had regained all components of normal gingival architecture. His gingival tissue was now stippled, clean, pink, tight, and displayed the shallow pocketing of 1-3 mm with no bleeding (compared to his 4-5 mm initial probings). The gingival tissue on the buccal of No. 23 resolved to the level where no further periodontal intervention was recommended. The gingival tissue from teeth Nos. 22-27 had never been touched by a scalpel, laser, or any other periodontal procedure other than the original scaling and root planing, followed by clear aligner therapy.
Retainers, similar to the aligners, but a medical grade heavier, were delivered to Evin and he was advised to wear them nightly.
Evin's treatment was completed in 2006. Fast forward nine years, and Evin schedules six-month preventive recare visits with our hygienist and still follows excellent home care. He has enjoyed nine years of health, comfort, and stability.
When we first met Evin, he was unhappy and generally unhealthy. Evin's treatment with clear aligners taught me how powerful these appliances were and how significant an impact they can have on the periodontal health, stability, and longevity of our patients. Even more powerful is the impact the clear aligner therapy had on Evin's overall health and well-being.
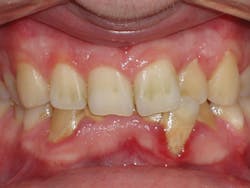
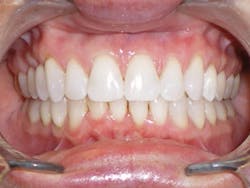
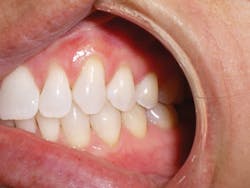
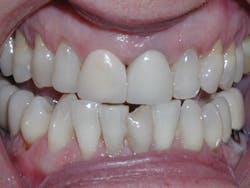
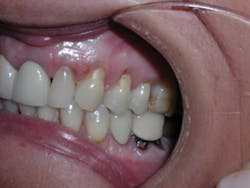
Figure 2
Since treating Evin, I approach all periodontal concerns with an eye for the patient's overall health and happiness as well as their occlusion. Any malocclusion can contribute to the periodontal deterioration of our patients. Correcting the patient's malocclusion is a vital step in established and maintaining lifelong periodontal health as well as generally happy and healthy patients.
Gueits: The hygienist's perspective
I saw Evin's case for the first time at a continuing education event I attended in 2006. It helped validate the need to change dentistry's common philosophy of a periodontics / restorative / orthodontics protocol to the more comprehensive protocol of periodontics / orthodontics / restorative.
Orthodontics is fundamental to oral health and should not be considered an afterthought - rather, a standard of care. Imagine if Evin did not go to a dentist such as Dr. Miraglia. If orthodontics was not part of Evin's treatment, he would have been a victim of costly and painful dental procedures geared toward treating symptoms rather than providing solutions.
I share Evin's case with my patients to show them firsthand the consequences of malocclusion and to instill the value of properly aligned teeth, using the following analogies:
• Imagine building your house on beams that are tilted. Would you want to invest in a house built on that foundation? Imagine the consequences of improper forces! The teeth are no different. Teeth that are in the proper inclination will provide a solid foundation for oral health. Simply stated: "Teeth that fit together last longer" and subsequently will need less costly dentistry in the future. Most importantly, there's nothing like your own teeth!
• Imagine Evin's lateral incisor, tooth No. 23, as a pole in the ground. Imagine that pole being "hammered" constantly throughout the day. What would happen? The pole would exhibit fracturing and splintering, and the dirt around the pole would dissipate, forming a "well" around the pole, leading to loss of stability. The same thing happens with the tooth in the periodontium.
• Picture a shoebox. The upper teeth are the "lid," and the bottom teeth are the "box." The upper teeth should slide over the bottom like a shoebox lid fits over the box. Teeth should be "sliding, not colliding."
All three analogies demonstrate traumatic occlusion. When teeth are not hitting properly, they create excessive forces. Teeth are not special; they do not get to bypass the laws of physics. The periodontal ligament cannot act as the cushion or shock absorber. If the teeth are constantly in trauma, as I have routinely warned patients, "Something's gotta give." What gives? Two things:
• Hard tissue: loss of enamel and bone
• Soft tissue: loss of attachment, clefting, recession, leading to potential abfraction formation
The solution is clear. If patients present with an orthodontic problem, shouldn't we provide an orthodontic solution? Shouldn't we consider taking our patients' teeth out of trauma rather than continue to address the symptoms of malocclusion? How do we do that? When patients are given the option of long-term solutions with orthodontics, they have the advantage of:
• Keeping the integrity of their own teeth, reinforcing minimally invasive dentistry
• Preventing future consequences of malocclusion (recession, abfraction, hypersensitivity, wear facets, crowns, potential TMD symptoms
• Having functional occlusion to prevent future wear and fracturing
• Improved well-being. Let's not forget the "swagger factor" that patients experience by having an esthetically pleasing outcome, leading to higher self-esteem and oral health motivation as portrayed in Evin's case.
• Realizing that they don't have "bad" or "crooked" teeth.
Evin is a perfect example of this. He always had beautiful teeth. Dr. Miraglia could see that they were just in the wrong place! Insufficient space, as a result of improper arch forms is the cause of crowding, not "crooked" teeth (see Figure 1).
Have you ever seen an anatomically crooked tooth? Dr. Miraglia and I have never seen a crooked tooth. Crooked roots? Yes, but not a single crooked tooth. We have to stop thinking about fixing crooked teeth and start focusing on the root cause.
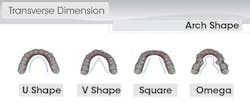
The natural solution was to provide Evin with a U-shaped arch to create space allowing for proper tooth alignment. There was no removal of tooth structure. Many refer to clear aligner therapy as a prime example of "organic" dentistry.
Dr. Miraglia: How the hygienist addresses malocclusion
A primary role for the hygienist is as educator or patient advocate. The hygienist has the advantage of time with the patient, and this helps to build a strong relationship, enabling the hygienist to spend a few minutes during a recall appointment to educate and, more importantly, resonate!
Our focus has always been on two key issues. The first is the difference between aligned teeth and crowded teeth. Our hygienists teach the patients that crowded teeth are harder to keep clean, and, as a result, they collect more plaque and calculus. Over time, this accumulation will irritate the gum tissue. The short-term result is puffy, red-to-purple bleeding gum tissue with deeper pockets.
The reality is that the repeating pattern of plaque accumulation, then removal at six-month intervals can be a slow deterioration process. The long-term consequence is gingival recession followed by bone loss. The hygienist has the opportunity to explain that properly aligned teeth collect less plaque and calculus because they are easier to clean. As a result, aligned teeth experience less deterioration over time.
Finally, the hygienist can introduce clear aligner therapy as a technique that can easily align the patient's crowded teeth. This simple educational technique can help patients connect the dots from crowded teeth to unhealthy, and from aligned teeth to health and longevity.
The second issue is the difference between a good bite and a bad bite. Professionals use the word malocclusion; however, this word doesn't register with most of our patients. Hygienists should be able to teach their patients the difference. Hygienists should feel comfortable describing a good bite as being protective and a bad bite as being destructive. A good bite exists when the teeth come together and contact one another where they were designed to contact. As Lauren explained, "Teeth should be sliding, not colliding." This concept is simple for a hygienist to teach, and patients are very receptive to this type of language and description. Lauren presents the solution to her patients as: "We really need to consider taking your teeth out of trauma" and then offers clear aligner therapy as the vehicle to do so.
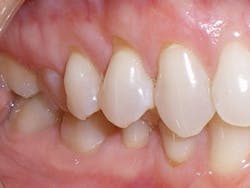
Compare the inclination of the long axis of teeth on #12 before and after treatment.
When I come in for the exam, I reinforce the hygienist's findings and the good news that braces are not the only option for adult patients. Clear aligner therapy happens to be an amazing option for adults to use to convert their malocclusion into healthy, stable, functional, and comfortable occlusion.
These two issues can be explained to any patient in a matter of minutes during a standard recall visit. We have had great success in sharing Evin's case with our patients when educating them on the health benefits of tooth alignment. "Show and tell" actually saves time since a picture is worth a thousand words. Consider accessing case studies at Invisalign.com (or Google "align tech case studies" for impressive before and after cases.)
Usually, I have very little to do, thanks to the efforts of my hygienist! The patient is already prepared for me, and I am there to answer any questions the patient might have. These conversations are most impactful when supportive and cooperative relationships exist between the hygienist and the dentist. When my hygienist and I are on the same page, the patient benefits from sound, caring treatment.
Three of the most obvious indications of malocclusion are the presence of clefting, recession, and abfractions. Both dentists and hygienists are capable of diagnosing areas of buccal recession and abfraction. However, too many times toothbrush abrasion is diagnosed. We need to evaluate the positioning of the teeth and the buccal/lingual inclination prior to jumping to conclusions that patients are brushing too aggressively.
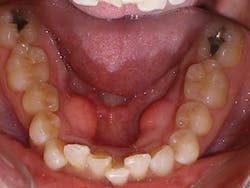
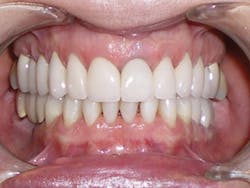
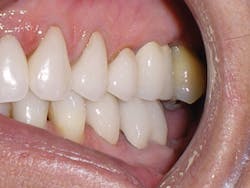
Figure 3
We find these areas of clefting, recession, and abfraction most often on the buccals of the canines and premolars, as well as occasionally on the buccals of the first molars as a result of lingual inclination. Dentists have made a routine practice of restoring the abfracted missing tooth structure with composite resin restorations. Dentists have also made it a practice to refer these patients to the periodontist for possible grafting procedures to replace the receded gingival tissues. These composite resin restorations and periodontal grafting procedures are classic examples of treating the symptoms instead of treating the cause.
The cause of the recession and abfractions is the patient's malocclusion. Specifically, it is the resulting horizontal force placed on the teeth from the malocclusion. Malocclusions deliver horizontal forces to the posterior teeth, and the result is early recession and abfractions that will continue to deteriorate until the cause is treated.
When composites are placed in areas of buccal abfractions, we expect the margins to be sealed and smooth. As the years pass, we detect the margins opening as the abfraction process continues both gingivally and occlusally to the composite. Eventually the composite will fall out and the patient will need a new, larger restoration.
Abfractions are merely a symptom of the horizontal forces generated by the underlying malocclusion. Treating the symptoms does not offer long-term health and stability because the cause of the problem is still present. The best way to care for our patients is to offer long-term orthodontic solutions that actually address the cause of the problem. In the case of recession and abfractions, the priority should be to correct the malocclusion. Sandra is a perfect case example:
Dr. Miraglia: Fixing Sandra's 'crooked' teeth
Sandra is a common example of a patient having a malocclusion that is the direct cause of her recession, and abfractions. When we first examined Sandra, her chief complaint was her smile (see Figure 3). She was unhappy with her smile and "crooked" teeth and had the desire to fix them.
Sandra expressed to us that she looked into clear aligner therapy but was told she was not a candidate. She was told she would need two years in braces and possibly some teeth extracted. These treatment options were undesirable, so she chose to do nothing. We assured her that she was an excellent candidate for clear aligner therapy, and her treatment time would be 14 months with no extractions.
Sandra was happy to hear the news. After collecting a full set of diagnostic records, performing the necessary scaling, root planing, polishing, and completing a comprehensive examination, Sandra was scheduled for consultation.
At the consultation, Sandra's photos were used to teach. The photo of the lower crowding with the lingual plaque and calculus was used to teach Sandra the difference between crowded teeth and aligned teeth. We also informed her that her teeth are not actually "crooked" (her chief complaint). The mandibular occlusal view pointed out her V-shaped arch provided no room for her teeth to fit within the arch.
The remaining photos were used to teach the difference between a good bite and a bad bite. Sandra learned about clefting, recession, abfractions, and the visible areas of enamel wear on multiple teeth. Sandra understood that clear aligner therapy would change her bad bite to a good bite, resulting in a beautiful, healthy smile. My goal went further than that. I knew the benefits of aligned teeth include increased longevity, a healthy periodontium, and proper occlusion for her to enjoy a lifetime of oral health.
Sandra was excited to begin treatment. So her case was submitted, developed, and delivered in short order. Her treatment involved 24 aligners, which took exactly 12 months of treatment time.
Upon completion of treatment, she had a healthy, stable, and functional occlusion. Notice the clefting, recession, and abfraction improvements in the photographs related to her case. This validates my objection to the current standard of care of "waiting and watching" for conditions to worsen. Instead, my hygienists and I educate patients on the long-term solutions of clear aligner therapy so they can make educated choices regarding their oral health.
Data about malocclusion and patient health
Approximately three out of four Americans have some type of malocclusion.1 The American Academy of Periodontology (AAP) released a statement on Comprehensive Periodontal Therapy in 2011 that was a call to action for hygienists to include occlusion in the comprehensive periodontal exam. Furthermore, the AAP stated treatment procedures, when indicated, should include occlusal therapy that may include tooth movement. A recommendation has been made upon completion of planned periodontal therapy for the correction of any tooth positioning considered to be contributing to the periodontal disease process.2
In 2012, the Centers for Disease Control and Prevention (CDC) released statistics stating that 47.2% of the American population has periodontitis3 (that is not including gingivitis, rather actual bone and clinical attachment loss). This statistic jumps to 70.1% in adults over the age of 65.3 Drs. Staufer and Landmesser have found anterior crowding of 3 mm or more serves as an individual host factor for periodontal disease.4 This is extremely relevant to hygienists' quests to prevent any additional risk factors contributing to periodontal disease.
A study comparing the microbial composition in subgingival plaque of adult crowded vs. noncrowded segments consistently represented more species of periodontopathogens in crowded teeth.5
A review of the oral-systemic connection was introduced, focusing on inflammation as a result of anterior crowding and excessive functional stress.6 Malocclusion and abnormal tooth position are being considered potential contributors to the disease process when they cause occlusal traumatism.7
Noncarious class V lesions and abfraction formation are based on the laws of physics and improper loading of horizontal (non-axial) forces. Gingival clefting may appear as a first sign of faulty tooth positioning. Creating axial (vertical) forces is paramount to tooth longevity.8,9 The idea is to prevent abfractions from forming rather than wait to treat them. Horizontal forces cause excessive strain on the cervical region, which does not allow the force to be absorbed by the periodontal ligament (the shock absorber). Tooth flexion and occlusal stress lead to the breakdown of the enamel rods, which may result in abfraction formation appearing as wedge-shaped notches.10 Orthodontic therapy is referenced as a viable treatment option to prevent recession and potential abfraction formation.11
The current standard of care for treating noncarious class V lesions is: 1. Wait and watch and 2. Class V buccal composites.12 Some controversial treatments for noncarious class V lesions are occlusal adjustments and night guards (occlusal splints).13 If abfractions are suspected, then any decision to carry out destructive, irreversible treatment should be considered very carefully, since inappropriate occlusal adjustments may increase the risk of certain conditions such as caries, occlusal tooth wear, and dentin hypersensitivity.14 Occlusal splints have the potential to reduce non-axial (horizontal) forces. Although they provide a conservative treatment, there is no evidence to support their use for managing suspected abfraction lesions.15
Orthodontics is also the most minimally invasive treatment option! No drilling, no filling, no surgery - just repositioning and arch re-formation. We have been challenged, as our professional responsibility, to identify and recommend appropriate orthodontic solutions.2
Dr. Miraglia: Victoria's long-term history and recovery
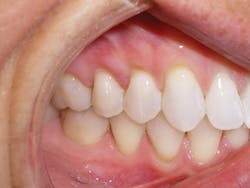
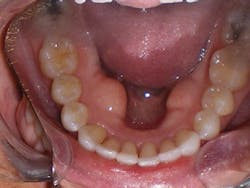
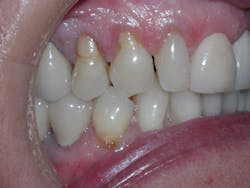
Victoria was similar to Sandra, but had more advanced deterioration. Victoria had a history of recession and abfraction as well as composite resin restorations placed to restore the abfracted areas. Victoria also had her malocclusion for a longer period of time, so she has had the opportunity to have restorations and the continuation of the recession and further abfraction areas occurring around the existing buccal composites (see Figure 4). Eventually, this led to the buccal composites falling out, which is evident in the photos. This process of recession, abfraction, composite filling, more recession and abfraction, and another composite filling, etc. happens for a reason. When we place composites, we are treating the symptoms and not the cause of the abfractions.
Figure 4
Victoria validated this by describing that she had been going to the dentist routinely, always needing something repaired. In Victoria's case, as with many others, the cause was the malocclusion; the indicated treatment was to develop the arch form and width, and to level and align the teeth to deliver a better, protective occlusion.
After taking a full set of records, Victoria's consultation involved using her photographs to teach the extent of the deterioration her malocclusion had caused. We discussed recession, bone loss, periodontal probing depths, abfractions, gingivitis, decay, fractured cusps, worn enamel, failed restorations, and continued deterioration. We taught the difference between a good bite and a bad bite and discussed the opportunities to treat the cause of the deterioration with clear aligners first and then perform the restorative dentistry second.
Victoria agreed to our recommendation. Clear aligner therapy was accomplished with 25 aligners, which took 12 months. Then, full-coverage esthetic restorations were placed on teeth Nos. 3-14 and also teeth Nos. 19 and 20. A lower lingual bar was bonded to all six lower anterior teeth, Nos. 22-27.
Correcting the malocclusion directly contributed to the improvement in the health of the gum tissue. The restorative dentistry was accomplished easily thanks to the gum tissue being pink, healthy, and tight, with shallow pockets. After completing the comprehensive care treatment for Victoria, she was placed on a four-month recall that she continues to maintain. Five uneventful years have passed, and the five-year follow-up photos show stability and health. Victoria enjoys all of the function and strength from her good bite and dental restorations without any deterioration at the five-year mark. The key to periodontal health and restorative success and stability is the correction of the malocclusion. The clear aligner therapy was the cornerstone of this comprehensive treatment plan.
Conclusion
We have both been fortunate to work with professionals who share the same philosophy of orthodontics being paramount to comprehensive care. This shared philosophy is understood and reinforced by the entire team, including assistants and office personnel. This reinforces the office philosophy of orthodontics being integral to comprehensive care and provides consistent messages to our patients.
Prior to clear aligner therapy, adult patients did not have a reasonable option for orthodontics as a viable treatment for the consequences of malocclusion. Many dentists and hygienists were not taught to include orthodontics as a preventive solution to the consequences of malocclusion. A philosophy of orthodontics as a standard of care has provided patients with improved health and well-being. These patients were able to make educated choices on the value of orthodontics as a result of the dentist/hygienist approach in providing clear aligner therapy as a viable long-term solution. Your patients are counting on you not only to improve their smiles, but to be healthy and happy as well. RDH
Disclaimer:
The views presented in this article are independent of Align Technology and Lauren Gueits' role as hygiene education manager for Align Technology. The author is commenting on clinical experiences treating Invisalign patients since 1999, the inception of Invisalign. Dr. Miraglia is a faculty member for Invisalign.
Lauren Gueits, RDH, BS, has been a clinician for more than 20 years, and she is a recipient of the 2010 Sunstar/RDH Award of Distinction. She lectures nationally to health professionals on the oral/systemic and ortho/perio link. NBC and ABC, featured her story on disclosing diabetes through her dental exam. She presented at the 2011 American Association of Diabetes Educators Symposium. She was the first dental professional to produce and simultaneously broadcast live webinars to both diabetes and dental professionals for continuing education through Colgate's Oral Health Network. She received training in orofacial myofunctional therapy through the AOMT in 2013.
Ben Miraglia, DDS, graduated from the State University of New York at Buffalo School of Dental Medicine. He has 19 years of private practice experience in Mt. Kisco, N.Y. Dr. Ben Miraglia has been providing Invisalign with a comprehensive care philosophy for the last 10 years. Since 2008, Dr. Miraglia has been an Invisalign faculty member speaking internationally to thousands of dentists. Dr. Miraglia is a graduate of the United States Dental Institute where he learned his non-extraction and nonsurgical orthodontic philosophy. He was appointed to the USDI faculty in 2008 and teaches nationally for them. Dr. Miraglia was recently honored with a position on the President's Council of Northern Westchester Hospital in Mt. Kisco.
References
1. Brunelle et al. Journal of Dental Research (2/96).
2. The American Academy of Periodontology Statement: Comprehensive Periodontal Therapy. J Periodontal May 2000 (Supplement).
3. Eke PI, Dye BA, Wei L, Thornton-Evans GO, Genco RJ. Prevalence of Periodontitis in Adults in the United States: 2009 and 2010. J Dent Aug 2012.
4. Staufer K, Landmesser H. J Orofac Orthop. 2004 Jan;65(1):13-25.Department of Orthodontics, University of Witten/Herdeke.
5. Chung et al. International Journal of Adult Orthodontics and Orthognathic Surgery.
6. Goldman H, Schluger S, Fox L, Cohen DW. Periodontal Therapy. 7. Philadelphia: W.B. Saunders; 1990. p. 52.
7. Geiger AM. Malocclusion as an etiologic factor in periodontal disease: A retrospective essay. Am J Orthod Dentofacial Orthop 2001 Aug;120(2)112-5.
8. Lee WC, Eakle WS. Possible role of tensile stress in the etiology of cervical erosive lesions of teeth. J Prosthet Dent. 1884;52:374-380.
9. Rees J. The effect of variation in occlusal loading on the development of abfraction lesions: a finite element study. J Oral Rehabil. 1977;4:65.
10. Kassab MM, Cohen RE. J Am Dent Assoc. 2003 Feb;134(2):220-5.
11. Micheal et al. Australian Dental Journal Volume 54, Issue 1. Pages 2-8, March 2009.
12. Onal B, Pamir T. A two-year clinical performance of esthetic restorative materials in noncarious cervical lesions. JADA Vol. 136, No 11, 1547-1555.2005.