Focal epithelial hyperplasia
(Heck’s disease)
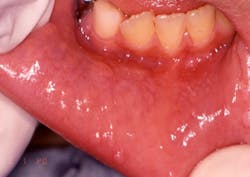
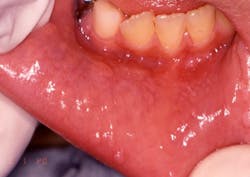
Your patient today is a 10-year-old boy, Jason, who presents to your office with his mother. The mother is concerned about the small papules that are visible on the mucosa along the vestibular areas of lips. The papules appear to be slightly raised, sessile, and almost the same color as the surrounding tissue. Jason reports no pain, but has traumatized the growths several times in the past few months. The mother reports that the growths appear to “come and go” (see Figure 1).
Introduction: Focal epithelial hyperplasia (FEH), also known as Heck’s disease, was described by Estrada in 1956 within a group of Colombian Caramanta Indians and in 1965 as a distinct entity within communities of Native Americans and Alaskan Eskimo children.
Since its discovery, reports have been made from around the world, but FEH is not commonly reported in Europe. Others areas of the world have reported FEH, including Brazil, Mexico, and South Africa, as well as the United States. Another known term for focal epithelial hyperplasia is multifocal epithelial hyperplasia (MEH). In Latin America, the entity is known as multifocal papilloma virus-induced epithelial hyperplasia.
The HPV 13 (human papilloma virus) and 32 (low-risk types that are non-oncogenic) have been implicated in the development of this condition. Some researchers suggest a genetic predisposition, as well as the possibility of household transmission since studies confirm that multiple family members may also have FEH (Lopez-Villanueva, et al. 2011). Communities with close living spaces appear to exhibit more reported cases.
Personal hygiene, nutrition deficiency, and oral hygiene deficiency have been noted as well and may play a role in spreading the virus. The virus is very contagious and easily spread. Reports of an increase in communities in rural South African towns with a high rate of HIV-positive individuals have been noted. The use of highly active antiretroviral therapy for the treatment of HIV is associated with increased frequency of FEH (Feller et al. 2010).
Method of transmission: HPV 13 or 32 is transmitted in a manner similar to that of other human papillomaviruses, by surface contact with the virus through a break in the mucosal barrier. Utensils and saliva contamination have been suggested as possible routes of transmission. This is frequently due to localized trauma and this type of trauma frequently occurs in the lip region.
Epidemiology: Focal epithelial hyperplasia has been identified in many population groups around the world. All ages can be affected, but the condition is somewhat more common in younger age groups. Younger females (78%) are reported to have developed FEH more frequently than males in a study of nine case reports with a mean age of 13.3 years old (Ledesma-Montes, et al. 2005).
Pathogenesis: Introduction of the virus into the mucous membranes causes proliferation of the cells in the stratum spinosum. It is hypothesized that the child may develop maturation of the immune system, and the growths slowly dissipate due to the immune system’s ability to detect the viral particles as it matures. This could be why adults are not usually affected in the same numbers as children.
Perioral and intraoral characteristics: The lesions of focal epithelial hyperplasia display a pink to whitish, somewhat translucent surface that is only slightly cauliflower-like. They are soft on palpation, as they generally have less keratin than the other HPV-related lesions. The lesions most commonly affect the lips, tongue, and buccal mucosa, where they appear as numerous discrete papular or nodular growths that may be singular or in multiple lesions.
Distinguishing characteristics: These lesions may be more generalized within the oral cavity than the other forms of HPV.
Significant microscopic features: The hallmark of focal epithelial hyperplasia is the presence of mitosoid figures (cells in which the nuclear DNA has fragmented, resulting in a cell that appears as if it is undergoing mitosis) in the middle of the spinous layer of the epithelium. These cells are referred to as mitosoid cells, mitosoid bodies or mitosoid figures.
Cells show pyknotic nuclei with vacuolated cytoplasm exhibiting koilocytic cells (indicative of HPV). The tissue demonstrates acanthosis, parakeratosis within the epithelium. The histology will exhibit deep papillomatous projections. All these features will suggest a diagnosis of FEH.
Dental implications: The lesions usually heal spontaneously, but may reappear with trauma. Parents of young children may be especially alarmed when the disorder continues over a long period of time.
Differential diagnosis: Other verrucal or papillary type lesions would be considered in a differential diagnosis such as verruca vulgaris, oral squamous papilloma, and condyloma acuminatum, as well as the oral lesions associated with Cowden syndrome and Crohn’s disease, white sponge nevus. Multiple endocrine neoplasia syndrome type 2B, an autosomal dominant disorder, may have a similar intraoral appearance, and should also be considered as well.
Treatment and prognosis: Treatment is not always necessary. Conservative excision may be performed to establish a definitive diagnosis, and laser ablation may be performed in recurrent cases. These lesions will resolve spontaneously without any treatment in most cases. Regression is noted in many cases because of possible viral recognition and cell-mediated immunity. Malignant transformation is unlikely.
Constant trauma of the tissue may be more of a long-term problem, and tissue trauma or abrasion is certainly not optimal for the patient. But, as stated previously, the patient may develop an immune system ability to recognize and destroy the viral particles. Sometimes methods such as surgery, laser ablation, or topical retinoid acids are used for some growths and, of course, a biopsy to determine the etiology. RDH
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ ADHA award winner. Her website for seminars is www.nancywburkhart.com
References
Abdullah L, Abbas O. Question: Can you identify this condition? Can Fam Physician. 2011 57(12): 1415.
Feller L, Khammissa RAG, Wood NH, Marnewick JC, Meyerov R, Lemmer J. HPV-sssociated oral warts. SADJ. 2010; 65(4): 172-5.
Ledesma-Montes C, Vega-Memije E, Garces-Ortiz M, Cardiel-Nieves M, Juarez-Luna C. Mutifocal epithelial hyperplasia. Report of nine cases. Med Ora Patol Oral Cir Buccal 2005; 10:394-401.
Lopez-Villanueva ME, Conde-Ferraez L, Ayora-Talavera G, Ceron-Espinosa JD, Gonzalez-Losa MDR. Human papillomavirus 13 in a Mexican Mayan community with multifocal epithelial hyperplasia: could saliva be involved in the household transmission? Eur J Dermatol. 2011: 21(3): 396-400.
Puriene A, Rimkevicius A, Gaigalas M. Focal epithelial hyperplasia: Case report. Stomatologija, Baltic Dental and Maxillofacial J. 2011; 13: 102-04.
Past RDH Issues