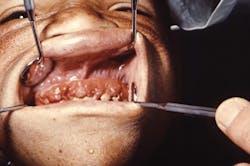
Hashimoto's disease: Hypothyroidism is autoimmune disease
Figure 1: Hypothyroidism. Enlarged gingiva associated with edema from hypothyroidism. (From CDC/Dr. J. Lieberman; Dr. Freideen Farzin, University of Tehran.)
By NANCY W. BURKHART, BSDH, EdD
Your patient today is Alma, a 45-year-old female, who reports that she was recently diagnosed with Hashimoto’s disease. Hashimoto’s disease is an autoimmune disease, and Alma’s health record reminds you that she has a history of Sjogren’s syndrome as well. Often, an additional type of autoimmune disease such as Sjögren’s syndrome, diabetes, or Addison’s disease is associated with Hashimoto’s disease.
Alma has complained about xerostomia and some enlargement of the salivary gland tissue in the past, which is characteristic and is associated with the Sjogren’s syndrome. However these complaints could become exacerbated by the addition of Hashimoto’s thyroiditis.
Alma asks, “what can you tell me about hypothyroidism and hashimoto’s disease? Are they the same?”
In general, the most common cause of hypothyroidism is a lack of iodine in the diet. Iodine allows the body to produce an adequate amount of the thyroid hormone that is needed to perform daily cellular functions. Many salts today do not have the iodine that was found in the past, and a reduction of salt in the average diet has occurred because of the association and emphasis or caution with hypertension. Hypothyroidism in general is estimated to occur 350/100,000 a year in females and approximately 80/100,000 a year in males, and it becomes more common as patients age.
Myxedema occurs in hypothyroidism, and this edema causes water retention and facial changes. Enlarged gingiva associated with edema may also occur in uncontrolled and prolonged hypothyroidism. Hypothyroidism is a condition, and laboratory results indicate elevated thyroid-stimulating hormone levels (TSH) with reduced levels of thyroxine. Prolonged hypothyroidism may result in a dull expression, puffy eyelids, coarse skin, dry hair, mental and physical activity is slowed, anemia, and secondary cardiovascular effects. Dental effects of prolonged hypothyroidism are gingival enlargement (see Figure 1), macroglossia, glossitis, salivary enlargement and dysgeusia (distortion with the sense of taste).
Hashimoto’s thyroiditis is an autoimmune disease where the body sees the thyroid tissue as an antigen, and this results in inflammation and a slow destruction of the thyroid gland. Hakaru Hashimoto, a Japanese medical scientist, discovered the disease in the early 1900s. Hashimoto thyroiditis occurs more frequently in females with a female to male ratio of 20:1 and the age range is usually from age 6 to middle-aged individuals, as is the pattern of other autoimmune diseases. It occurs in 3.7% of the United States population.
It is not uncommon to find several people in one family diagnosed with Hashimoto’s disease such as a mother, daughter, aunt, and grandmother. The immune system mistakes the individual’s own tissue as a health threat or foreign invader and begins to mount a defense against those tissues by producing antibodies toward proteins in the thyroid gland, thus destroying the thyroid gland or rendering it incapable of making the necessary thyroid hormones.
Hashimoto’s disease is the most common cause of hypothyroidism in developed countries such as the United States. The symptoms that are produced are those caused by an underactive thyroid and ultimate destruction of the thyroid over a number of years resulting in hypothyroidism. Lab testing will indicate antibodies against thyroglobulin and thyroperoxidase. Hashimoto’s thyroiditis exhibits early symptoms of this deficiency, but in varying degrees such as depression, anxiety, fatigue, difficulty sleeping, skin changes, and weight gain. Goiters are sometimes developed and are usually clinically observed when performing the extraoral exam. Birth defects such as heart, brain, and kidney problems are documented in babies born to women with untreated hypothyroidism. Children may have a higher risk of cleft palate and intellectual developmental problems as well.
Essentially, the thyroid gland produces three hormones, T3 (triiodothyronine), T4 (thyroxine), and calcitonin. These hormones control the metabolism of almost all the cells in the body. Follicular cells in the thyroid gland produce the thyroid hormone, thyroxine, and triiodothyronine. Thyroxine and triiodothyronine regulate basal metabolic rates and body temperature, lipid metabolism, carbohydrate metabolism, and all aspects of linear growth. They are crucial in brain development before and after birth, regulate heart rate, contractibility and output, regulate vasodilatation, respiratory rate, gastrointestinal activity, and libido and fertility (Delong & Burkhart, 2013).
Calcitonin is produced by what is termed parafollicular cells. The calcitonin inhibits the release of calcium from the bones into blood and other fluids, as well as regulating serum calcium and phosphorus levels.
As you can see, the thyroid hormones are essential for normal bodily functions. As you explain this to Alma, she begins to understand the process and to correlate the symptoms that she has observed for quite some time. She has complained of fatigue, sensitivity to cold, constipation, a puffy face, changes in her voice, an elevated blood cholesterol level (LDL levels), fluid retention and weight gain, muscle aches, tenderness in the hips and shoulders, joint pain, pale, dry, course skin, forgetfulness, and a slowing of the thought process in general with possible depression. Some patients may experience some or all of these symptoms to varying degrees.
High levels of antibodies against thyroglobulin and the enzyme thyroid peroxidase (TPO test) play a role in the production of thyroid hormones and are diagnostic in Hashimoto’s thyroiditis. Routinely, the normal thyroid levels are tested through TSH levels; for most labs, that number is 0.3-3.0. mIU/L. Some physicians like to see the upper limit at 2.5 mIU/L. Higher levels of TSH mean that the pituitary gland is producing thyroid stimulation to compensate for low levels of thyroxin in the bloodstream in order to stimulate the thyroid gland to produce more thyroid hormone.
Treatment for hypothyroidism is thyroid replacement hormones such as Levoxyl, Synthroid, Cytomel, Thyrolar (containing both T3 and T4), or Armour Thyroid (made from pigs). Some physicians do not recommend Armour Thyroid since there may be a slight risk of disease transmitted by animal tissue, and this is under investigation.
Some foods also act as goitrogens and can interfere with thyroid hormone production, thereby slowing down the thyroid function. Foods in the cruciferous category such as cabbage, broccoli, cauliflower, radishes, rutabagas, and turnips, may inhibit the body’s ability to use iodine, and block the actual secretion of the thyroid hormone conversion. Some physicians suggest using these vegetables in moderation or to minimize their use depending upon the severity and cause of the hypothyroidism. Additionally, certain medications may interact with thyroid medications as well. Taking thyroid medication on an empty stomach and several hours before or after other medications is suggested.
Finally, since autoimmune diseases are often reported during times of stress, physicians do tell patients to limit stressful situations and to find stress-reducing activities such as yoga, tai chi, light physical activity, and surrounding yourself with those people that you enjoy being around — those who are uplifting to you!
Keep listening to your patients and always ask good questions. RDH
Discussing Hashimoto’s before treatment
The oral manifestations may vary depending upon the extent and length of the deficiency. Restoring and maintaining the euthyroid (normal thyroid balance) is the long-term goal by the medical community. Vital signs, medication dosage, etc., and pertinent questions should be asked of the patient. An excellent article published in RDH by Lynn Cortese Radziewicz accounts her own lengthy and personal journey to obtaining a diagnosis of Hashimoto’s thyroiditis (see references).
Dr. T.D. Rees (2012) suggested some questions that the dental practitioner needs to ask the patient before rendering treatment:
- When were you first diagnosed?
- What signs or symptoms did you have that caused your physician to test you?
- How often do you see your physician?
- Have you fainted or passed out at any time since you last saw your physician?
- What medications do you take? Has your physician increased or decreased your medication dosage recently? If so, why?
- Do you currently have other medical problems such as anemia or heart disease?
- Do you find yourself weaker and more lethargic than you were a few months ago?
- What type of problems are you having in your mouth? Enlarged tongue, dry mouth, swollen salivary glands?
Source: Patton LL ed. American Dental Association, Chicago IL. 2012. pg89.
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics/stomatology, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. Her website for seminars on mucosal diseases, oral cancer, and oral pathology topics is www.nancywburkhart.com. She can be contacted at [email protected].
References
- DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist, 2nd ed.. Wolters Kluwer Health/Lippincott, Williams & Wilkins. Baltimore, 2013. Pg. 165-68.
- Little JW. Thyroid disorders. Part ll: hypothyroidism and thyroiditis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006; 102(3): 275-80.
- McGrogan A, Seaman HE, Wright JW, de Vries CS. The incidence of autoimmune thyroid disease: a systematic review of the literature. Clin.Endocrinol 2008;69(5):687-96.
- Nobuyuki A, Tada H, Hidaka Y, Hashimoto K. Hashimoto’s disease and Dr. Hakaru Hashimoto. Endocrine J. 2002; 49(4), 393-7.
- Radziewicz LC. RDH, Hashimoto’s Disease. www.rdhmag.com/articles/print/.../hashimotorsquos-disease.html
- The ADA Practical Guide to Patients with Medical Conditions, First Edition. Edited by Lauren L. Patton.É 2012 John Wiley & Sons, Inc. Published 2012 by John Wiley & Sons, Inc. Rees, TD. Endocrine and Metabolic Disorders from Clinical Care in Oral Health. 2012
Websites:
- http://video.about.com/thyroid/What-Is-Hashimoto-s-Disease-.htm
- http://video.about.com/thyroid/What-Is-TSH-.htm
- http://video.about.com/thyroid/The-Difference-Between-Hashimoto-s-Disease-and-Hypothyroidism.htm
- http://thyroid.about.com/b/2006/09/20/dont-like-certain-veggies-it-may-be-your-thyroid-talking.htm
- www.aarda.org