The medically challenging patient needs compassion and education: A case study
Diane has arthritis, Raynaud’s disease, Sjögren’s syndrome, and a form of scleroderma known as CREST syndrome. Due to the difficulty of dental care, she had avoided seeing a dentist for 10 years until pain on No. 31 forced her to make an appointment.
Jamie Collins, RDH, CDA
Recently, I had the honor of treating a medically challenging patient, one whose medical conditions complicated her dental treatments considerably. As part of a periodontal specialty practice, we often see patients who have struggled with periodontal disease complicated by multiple risk factors.
Diane presented with autoimmune disorders and poor personal hygiene care. Diane was referred to our practice by her general dentist for evaluation and treatment of her generalized periodontal condition, and for a prognosis of her remaining dentition. She is 64 years old. Diane had been through breast cancer treatment two years ago, followed by surgery and radiation. She does not drink alcohol or use tobacco products. She takes tamoxifen, vitamin D, biotin, and folic acid daily. She rounds out her health history forms by noting arthritis, Raynaud’s disease, Sjögren’s syndrome, and scleroderma. Due to the difficulty of dental care, she had avoided seeing a dentist for 10 years until pain on No. 31 forced her to make an appointment.
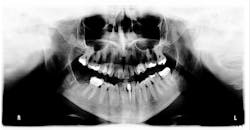
Figure 1: Panoramic x-ray
Scleroderma is an autoimmune disease that affects the connective tissue of the body and can cause thickening of the skin, inflammation, blood vessel disorder, and lack of elasticity in the skin due to fibrosis. It is rare enough that I had only experienced one other patient who had been severely affected by the disease in the past 20 years.
Diane has been diagnosed with a form of scleroderma known as CREST syndrome. Organs that are affected by scleroderma can include the esophagus, which is the problem that plagues Diane. This presents a complication to treating her due to throat dysfunction, making it difficult for Diane to swallow and impossible to place her in a supine position. The disease affects the lower two-thirds of the esophagus and can cause extreme reflux and heartburn, which can also affect oral health from the effects of stomach acid.
One of the most difficult things we encountered in treatment planning was obtaining radiographs, due to the lack of elasticity of the skin. Diane was unable to tolerate any stretching of her cheek and lips to accommodate even a size one pediatric sensor. I was able to get less-than-ideal bitewings and manipulate the area for one periapical film. She was then referred back to her general dentist to obtain a panoramic film, since our office is only capable of taking digital full-mouth series using the sensor or CBCT images.
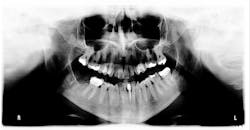
Figure 2: Mandibular arch
Compounding the effects of scleroderma, Diane also suffers from Sjögren’s syndrome, which affects the saliva and mucus-producing glands in the body. She exhibits signs of xerostomia with dry and sticky mucous membranes. Diane presented to her appointment with a large bottle of water that she said “goes everywhere” with her. It is so much a part of her that she has a holster around her waist to hold her water bottle. She was unable to recline more than about 60 degrees in the dental chair without having swallowing issues. As much as it inconvenienced me to treat Diane at this angle, I completely understood that it was related to her medical condition versus simple discomfort.
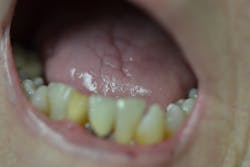
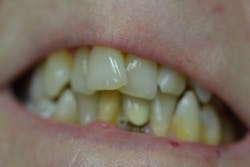
Figure 3: Maxillary anterior right
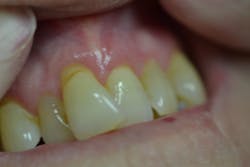
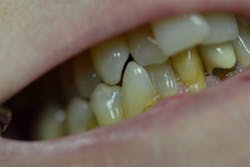
Her periodontal probing depths ranged from 2 mm to 6 mm, with as much as 4 mm of recession noted in some areas. Tooth No. 19 had a fractured off DL cusp to the gumline with decay close to the nerve; No. 29 had deep DO decay that would require endodontic treatment, buildup, and a crown to repair or possibly extraction; and No. 31 was unrestorable with buccal decay to the nerve, through the furcation, and at the bone level (figures 1–6). Faced with that treatment plan, she would also need four quads of scaling and root planing with anesthetic. We were able to coordinate the schedule to extract No. 31 directly after her periodontal treatment while she was still anesthetized.
Administration of anesthetic for Diane was a challenge in itself as we tried to “stretch” the cheek to gain access, all while not being able to recline her more than a 60-degree angle. Once she was anesthetized and comfortable, I proceeded to complete scaling and root planing on the right side prior to the doctor surgically extracting No. 31. She struggled to tolerate the extraction and was emotionally exhausted, as well as extremely nervous and on edge during the entire procedure. The tooth was so severely decayed that it continued to crumble and fracture away. It was an extensive process.
Figure 4: Maxillary anterior left
For future extractions or any periodontal surgeries, it was recommended that Diane complete them with the aid of sedation, which would allow her to relax and allow the dentist easier access. Diane’s next periodontal therapy appointment with me was a little easier because we both knew what to expect from each other. It helped being aware of her physical limitations beforehand.
Addressing the periodontal disease process was just one piece of the puzzle. Education and treating the cause and contributing factors were key. Diane suffers with xerostomia as a result of Sjögren’s, and it’s difficult for her to floss due to the lack of elasticity caused by scleroderma. Her only home-care routine up to that point had been using a manual toothbrush. At times, flare-ups of arthritis can make grasping the brush difficult. I spent some time discussing with Diane her goals for her oral health, and together we found products she felt she could use effectively.
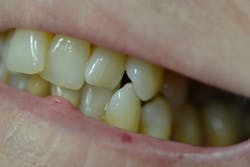
Figure 5: Right side
We talked about the benefits and overall effectiveness of power brushes, and I felt she would be best served with the smaller head size of the Oral-B brush. Diane said she does not floss because getting her hands in her mouth is next to impossible. An oral irrigator to combat the periodontal disease process was a logical choice in this case. With the help of xerostomia home products, we may be able to increase the effectiveness of saliva on a daily basis. With education and compassion, I stressed the need for three-month periodontal visits to maintain her oral health for the future. Diane is motivated to improve her home-care routine and realizes her risks of oral complications due to her medical conditions.
A key point for each of my patients is that I can only do so much on the professional level; it is up to each patient to continue to improve at home through the use of recommended products and by altering daily routines to ensure the odds of success. Through education and compassion, I can tailor recommendations to fit my patients’ individual needs. I can offer encouragement and motivation, but they must take responsibility for their own oral and systemic health at home.
Resources
• Shiel Jr WC. Davis CP, ed. How do health-care professionals classify scleroderma? MedicineNet website. https://www.medicinenet.com/scleroderma/article.htm#how_do_health_care_professionals_classify_scleroderma. Updated September 19, 2018.
• About Sjögren’s. Sjögren’s Syndrome Foundation website. https://www.sjogrens.org/home/about-sjogrens.
Jamie Collins, RDH, CDA, is a practicing clinical hygienist in Idaho and Washington states. She has been in the dental field for nearly 20 years, both as an assistant and hygienist. With a passion for patient care, especially those with higher risk factors, Jamie enjoys sharing the tips and tricks of the dental profession through speaking and writing. In addition to clinical practice, she is also an educator, has contributed to multiple textbooks and curriculum development, and is a key opinion leader. Contact her at [email protected].
CREST syndrome
Calcinosis—the formation of calcium deposits under the skin that may become infected or need to be surgically removed
Raynaud’s syndrome—spasms of the tiny vessels of the fingers, toes, tongue, nose, and ears that can cause them to turn blue or red with cold or emotional distress
Esophageal dysmotility—a dysfunction of the esophagus that can affect swallowing or backflow of stomach juices
Sclerodactyly—thickening and tightening of the skin on the fingers and toes that may limit movement
Telangiectasia—an abnormal dilation of small, red areas on the face, hands, and mouth that blanch when pressed upon, which is a reflection of dilated capillaries