Breaking down the new 2017 periodontal classification system
A lot has changed in dentistry over the last 19 years. The new classification system opens the door to the oral-systemic link, welcomes patients to become more involved in the state of their diseases, allows hygienists to communicate with patients, and leads to better treatment acceptance and understanding.
Jessica Raymond-Allbritten, BASDH, CRDH
The dental profession has used the same periodontal classification system for the last 19 years. Throughout that time, there have been many advancements in dentistry that require an update to the system. In the fall of 2017, a joint workshop was held between the European Federation of Periodontology (EFP) and the American Academy of Periodontology (AAP) to discuss issues with the 1999 periodontal classification system and to develop a new classification system based on current scientific evidence. After extensive discussion and research, the EFP released the new global classification system for periodontal health, diseases, and conditions, as well as peri-implant diseases and conditions in June 2018.
In review, the 1999 classification labeled periodontal disease as chronic, aggressive (localized and generalized), necrotizing, and a manifestation of systemic disease. The old system had several flaws including: considerable overlap in disease categories, no gingival disease component, lack of emphasis on age of onset of disease and rates of progression, and unclear classification factors. During the meeting last fall, four different working groups discussed these flaws and developed individual reports on their findings. The findings in each report were then developed into the new classification system.
In the new classification system, the section “Periodontal diseases and conditions” is broken down into three groups with subcategories. There is now a separate section called “Peri-implant diseases and conditions” that is divided into four groups.1
Periodontal diseases and conditions
Periodontal health, gingival diseases, and conditions
Periodontal health is clearly defined by the absence of clinical detectable inflammation. Clinical gingival health can be found on a periodontium that is intact without clinical attachment loss (CAL) or bone loss, and on a reduced periodontium in either a patient without periodontitis or in a patient who has a history of periodontitis who is clinically stable.
Nondental plaque biofilm–induced gingival diseases include conditions that are not caused by plaque and usually do not resolve after plaque removal. The patient’s medical history should be reviewed for possible oral-systemic conditions. Genetic disorders, infections, immune conditions, endocrine diseases, and traumatic lesions are examples of possible causes.2
Dental plaque‐induced gingivitis presents with red, inflamed, and bleeding gingival tissue and has both local predisposing factors and systemic modifying factors that can affect its location, severity, and progression. Dental plaque‐induced gingivitis can occur on an intact periodontium or on a reduced periodontium in either a patient without periodontitis or in a patient whose periodontitis is currently stable.2 A periodontitis patient with gingival inflammation remains as such; however, it is imperative to determine the cause of the inflammation and reduce it.
Periodontitis
As previously mentioned, the old system categorized periodontal diseases as chronic or aggressive, but now they are grouped under a single category—periodontitis. Periodontitis is then further characterized by a staging and grading system.
Staging is based on the severity of the disease and the complexity of the disease management. When staging a patient, it is important to note that it takes only one complexity factor to shift the diagnosis to a higher stage. If a stage-shifting complexity factor is removed by treatment, the stage will not regress to a lower stage since the original complexity factors should always be considered in maintaining a patient’s oral health.
Grading includes a history-based analysis of the rate of periodontitis progression, assessment of the risk for further progression, analysis of possible treatment outcomes, and assessment of the risks for how the disease or treatment will affect the patient’s general health. When grading a patient, direct evidence is the best; when it isn’t available, indirect evidence can be used. Dental professionals should assume Grade B disease and find evidence to shift toward Grade A or Grade C. Once a grade is established, it can be modified based on present risk factors.2
The category Periodontitis also includes necrotizing periodontitis and periodontitis as a manifestation of systemic disease. Necrotizing periodontal diseases present clinically with papilla necrosis, bleeding, and pain, and are associated with host immune response and impairment. Diagnosis is based on history and whether there is a systemic condition that is altering the patient’s immune response. Periodontitis as a manifestation of systemic disease is a category developed to account for the systemic diseases and conditions that affect the periodontium. There are rare conditions that result in periodontitis, and these should be grouped in this category.2
Other conditions affecting the periodontium
Systemic diseases associated with loss of periodontal-supporting tissues, such as neoplastic diseases, may affect the periodontium independent of dental plaque-induced periodontitis and should be categorized based on the primary systemic disease.
Endodontic-periodontal lesions are bacteria transferred between the pulp and periodontal structures. These lesions are characterized by a deep periodontal pocket extending to the root apex and/or negative/altered response during a pulp vitality test. Evidence of bone loss at the apex or furcation may be present with or without pain, exudate, tooth mobility, and/or fistula.
Periodontal abscess is localized accumulation of exudate within the periodontal pocket resulting in tissue destruction. Periodontal abscesses are further categorized by likely cause and when they occurred.2
Mucogingival conditions, as stated in the report from workgroup three, include two main categories: “Relates to gingival recession and is based on interproximal loss of clinical attachment and also includes an assessment of the exposed root and CEJ. The report presented a new classification system for recession.”4
• “Recession Type 1 (RT1): Gingival recession with no loss of interproximal attachment. Interproximal CEJ is clinically not detectable at both mesial and distal aspects of the tooth.
• Recession Type 2 (RT2): Gingival recession associated with loss of interproximal attachment. The amount of interproximal attachment loss (measured from the interproximal CEJ to the depth of the interproximal sulcus/pocket) is less than or equal to the buccal attachment loss (measured from the buccal CEJ to the apical end of the buccal sulcus/pocket).
• Recession Type 3 (RT3): Gingival recession associated with loss of interproximal attachment. The amount of interproximal attachment loss (measured from the interproximal CEJ to the apical end of the sulcus/pocket) is higher than the buccal attachment loss (measured from the buccal CEJ to the apical end of the buccal sulcus/pocket).”4
• A case without gingival recession can be described as the gingival phenotype (gingival thickness and keratinized tissue width). Findings contributing to the description of this condition might be tooth position, aberrant frenum, or vestibular depth.4
Occlusal trauma and traumatic occlusal forces are the forces that exceed the capacity of the teeth and can result in excessive wear or fractured teeth. It is important to note the report stated that occlusal trauma does not cause attachment loss and does not increase the progression of periodontitis. There is limited evidence that inflammation of the periodontal ligament can increase with occlusal trauma.4
Prosthesis and tooth-related factors are now included in the new classification system. This section was added to the classification system because indirect restorations may cause recession and CAL due to invasion of the supracrestal attached tissue (formally called biological width).4
Peri-implant diseases and conditions
Workgroup four developed a new classification for these four categories: peri-implant health, peri-implant mucositis, peri-
implantitis, and peri-implant soft- and hard-tissue deficiencies.
Peri-implant health presents with a core of connective tissue covered by keratinized or nonkeratinized epithelium and the intrabony part of the implant is in contact with mineralized bone.5
Peri-implant mucositis is indicated by the presence of bleeding on probing and clinical signs of inflammation. It is primarily thought to be caused by plaque as it often resolves with better home care and a proper in-office treatment to reduce biofilm.2
Peri-implantitis is characterized by the presence of bleeding on probing, clinical signs of inflammation, and radiographic bone loss. It is often seen in patients with a history of periodontitis and progresses quickly in a nonlinear pattern.2
Soft- and hard-tissue implant site deficiencies occur after tooth loss and lead to diminished alveolar ridge/process. Prior to tooth removal, if a root fracture, abscess, thin buccal bone plates, or endodontic infection is present, it can result in greater loss of the alveolar ridge/process. Medications and systemic diseases also reduce the amount of natural formed bone. In these cases, further treatment would be indicated prior to implant placement.2
Conclusion
The new periodontal classification system allows clinicians to better categorize patients’ oral health based on clinical and radiographic findings. Now that the oral-systemic link is part of the classification system, it will help patients become more involved in knowing the state of their diseases. Talking to patients about their classification can lead to better treatment acceptance and understanding. The new classification is complex and will take time to fully incorporate into patient care globally. The sidebar included within this article can be printed and kept with this article for easy chairside reference to aid in implementing the new classification system. Insurance companies will soon adopt the new classification system into their EOBs and expect it in the narratives they receive.
References
1. Caton JG, Armitage G, Berglundh T, et al. A new classification scheme for periodontal and peri‐implant diseases and conditions – Introduction and key changes from the 1999 classification. J Clin Periodontol. 2018;45(suppl 20):S1-S8. doi:10.1111/jcpe.12935.
2. Chapple ILC, Mealey BL, Van Dyke TE, et al. Periodontal health and gingival diseases and conditions on an intact and a reduced periodontium: Consensus report of workgroup 1 of the 2017 World Workshop on the Classification of Periodontal and Peri‐Implant Diseases and Conditions. J Clin Periodontol. 2018;45(suppl 20):S68-S77. doi:10.1111/jcpe.12940.
3. Papapanou PN, Sanz M, Buduneli N, et al. Periodontitis: Consensus report of workgroup 2 of the 2017 World Workshop on the Classification of Periodontal and Peri‐Implant Diseases and Conditions. J Clin Periodontol. 2018;45(suppl 20):S162-S170. doi:10.1111/jcpe.12946.
4. Jepsen S, Caton JG, Albandar JM, et al. Periodontal manifestations of systemic diseases and developmental and acquired conditions: Consensus report of workgroup 3 of the 2017 World Workshop on the Classification of Periodontal and Peri‐Implant Diseases and Conditions. J Clin Periodontol. 2018;45(suppl 20):S219-S229. doi:10.1111/jcpe.12951.
5. Araujo MG, Lindhe J. Peri‐implant health. J Periodontol. 2018;89(suppl 1):S249-S256. doi:10.1002/JPER.16-0424.
Jessica Raymond-Allbritten, BASDH, CRDH, practices dental hygiene with Ryan Lepore, DMD, at Lepore Comprehensive Dentistry in Dunedin, Florida. Jessica was a member of the 2015 Colgate Oral Health Advisory Board. She is also a contributing author for the Colgate Oral Health Advisor web page. You may contact her at [email protected].
A quick look
Periodontal disease and conditions can be broken down into three major categories:
1. Periodontal health and gingival diseases
a. Periodontal and gingival health
b. Gingivitis caused by biofilm (bacteria)
c. Gingivitis not caused by biofilm
2. Periodontitis
a. Necrotizing diseases
b. Periodontitis as a manifestation of systemic disease
c. Periodontitis (more detailed explanation below)
3. Other conditions affecting the periodontium
a. Systemic diseases affecting the periodontium
b. Periodontal abscess or periodontal/endodontic lesions
c. Mucogingival deformities and conditions
d. Traumatic occlusal forces
e. Tooth- and prosthesis-related factors
Peri-implant diseases and conditions can be broken down into four major categories:
1. Peri-implant health
2. Peri-implant mucositis
3. Peri-implantitis
4. Peri-implant soft- and hard-tissue deficiencies
Staging of periodontitis
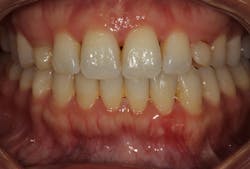
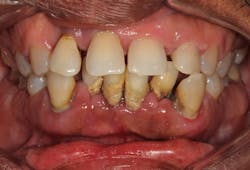
• Stage I (initial): 1–2 mm clinical attachment loss (CAL), less than 15% bone loss (BL) around root, no tooth loss due to periodontal disease, probing depth (PD) 4 mm or less, mostly horizontal BL (figure 1)
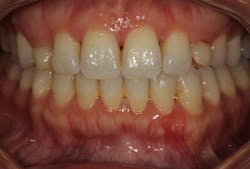
• Stage II (moderate): 3–4 mm CAL, 15%–33% BL, tooth loss, PD 5 mm or less, mostly horizontal BL (figure 2)
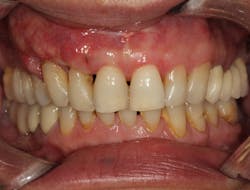
• Stage III (severe with potential for additional tooth loss): 5 mm or more CAL, BL beyond 33%, tooth loss of four teeth or less, with complex issues such as PD 6 mm or more, vertical BL 3 mm or more, Class II–III furcations, and/or moderate ridge defects (figure 3)
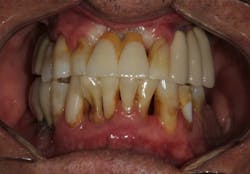
• Stage IV (severe with potential for loss of dentition): Encompasses all of Stage III with additional features that will require the need for complex rehabilitation due to masticatory dysfunction, secondary occlusal trauma, severe ridge defects, bite collapse, pathologic migration of teeth, less than 20 remaining teeth (10 opposing pairs) (figure 4)
Figure 1: Stage I periodontitis
Figure 2: Stage II periodontitis
Figure 3: Stage III periodontitis
Figure 4: Stage IV periodontitis
Photos courtesy of Scott Froum, DDS
Extent and distribution of periodontitis
1. Localized—BL is around less than 30% of teeth in mouth
2. Generalized—BL is around more than 30% of teeth in mouth
3. Molar-incisor—BL is found around molar (usually first) and anterior incisors
Grading of periodontitis
• Grade A (slow progression): No BL or CAL over five years, no smoking, no diabetes, heavy biofilm but no destruction
• Grade B (moderate progression): Less than 2 mm BL or CAL over five years, half pack or less per day smoking, HbA1c less than 7%, biofilm commensurate with destruction
• Grade C (rapid progression): Greater than 2 mm of BL or CAL over five years, half pack or more per day smoking, HbA1c 7% or higher, destruction exceeds amount of biofilm
This sidebar has been adapted from “The new classification of periodontal disease that you, your patient, and your insurance company can understand” by Scott Froum, DDS, originally appearing in Perio-Implant Advisory on August 30, 2018.