Optimizing the diagnostic view of pediatric care
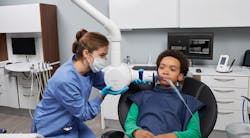
The x-ray is positioned for a pediatric patient. Courtesy of Dentsply Sirona.
When I first graduated from hygiene school, I worked full-time in a busy pediatric office. Our “open bay” layout, which included four dental chairs in a large room, was designed to allow parents, siblings, and other children to engage in the “show-tell-do” systems that ease the inexperienced patient’s anxiety. For the pediatric patient, everything involved in the dental experience is new.
The patient’s first-time experience can be overwhelming due to the sounds alone, such as the high-pitched sound of the polishing handpiece and suction. However, with the gentle touch of a skilled dental hygienist, the patient can overcome the initial fear of the unknown. The role of the pediatric dental hygienist is imperative to the patient’s future success in oral health.
Retaking X-rays
Imagine that you have a patient in your chair who is five-and-a-half years old. During the initial assessment, you notice a dark shadow on the distal of number K. The patient’s sibling is at high risk for tooth decay, the patient’s home care is poor, and her diet includes juice throughout the day.
The patient has never had a radiograph, but has been to the office when her brother had extractions. The patient showed tears during the placement of the lead apron. Her gag reflux is triggered by the plastic cover of the phosphor plate. She bites on the plate instead of the RINN, leaving a bright white artifact on the plate. The clinician must open the lining to expose the phosphor plate, then scan it into the computer. In the meantime, the anxious patient (and parent) wait eagerly for the news. However, the information from the plate cannot be evaluated, and we need to start over.
This exact scenario happened to me many times while working in pediatrics with phosphor plates.
Having multiple sensor sizes is critical to meet the needs of the patients in your office.
Dental Trauma
Due to their active lifestyles and brave spirits, dental trauma in children is common. When trauma happens, a radiograph is needed to determine the severity of that trauma. Despite telling the child that you received the best radiograph award in hygiene school and it will be easy, their dilated pupils and quivering lips say it all.
Frequently, parents and siblings try to prepare the child for their first time taking radiographs. Despite their good intentions, the patient is often left with the thought of something hugely uncomfortable being shoved into the mouth. To be fair, traditional films and phosphor plates are not far off from this dreaded fear. The thin phosphor plates often dig into the floor of the patient’s mouth, causing pain and preventing them from being able to fully close. Without fully closing, the film moves and lacks the information needed to be a diagnostic image.
This experience obviously creates anxiety for the next time the patient needs radiographs. Clinicians often have to retake film, which is not only costly for the office, but it is time consuming for the patient, resulting in more radiation exposure for the child, which no one likes.
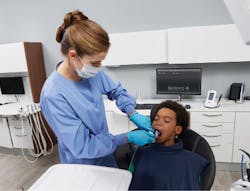
A hygienist carefully positions a sensor for an xray. Courtesy of Dentsply Sirona.
Digital sensors
When my office began implementing digital sensors, we provided higher diagnostic quality images with the first exposure. The instant availability of the image allowed the sensor to be in the child’s mouth for less time, and the child in the chair for less time. The sensors also require less radiation.
Additionally, I would alert the doctor that the image was ready, and the doctor would assess the image on their computer. This allowed the doctor to see the image and diagnose while in the other room, enabling us to save time. The improved image quality allows the parents to see the radiolucency in the tooth more easily, which increased our education abilities and treatment acceptance.
In my experience, the most favorable software I worked with was Dentsply Sirona’s Sidexis 4 because it allows intraoral camera images and 2D radiographic images to be shown on the same screen. This technology improves patient and parent education as cavities are identified two ways, while side by side.
To be successful in the implementation of high-quality digital diagnostic images, having multiple sensor sizes is critical to meet the needs of the patients in your office. Selecting the appropriate sized sensor for the patient’s anatomy will prevent additional trauma and allow the patient to close properly. The Schick 33 digital sensor by Dentsply Sirona is offered in a size 0, which is extremely helpful for pediatric patients. Dentsply Sirona also offers the AimRight positioning adhesive tabs, which lets clinicians place the sensor exactly where it needs to be. The AimRight tabs also allow the clinician to adjust the tab on the sensor wherever it will work best—sticking and re-sticking (if needed) several times with ease. For patients with narrow palates and tori, Edge Ease tabs can be placed on the edges of the sensor for increased comfort.
Providing the proper diagnosis and early intervention of dental decay begins with high-quality diagnostic images. Our ethical responsibility to provide ALARA (as low as reasonably achievable) is more easily achieved with digital sensors. Every office should have multiple sizes of sensors to allow for patient’s anatomy and increase patient comfort along with allowing for proper positioning for diagnostic images. Dentsply Sirona offers a digital radiograph system to meet the pediatric needs every practice has.
Editor's note: This article was originally published in 2018 and has been updated as of August 2025.
About the Author

Amber Auger, MPH, RDH
Amber is a dental hygiene clinician, international speaker, and hygiene director who specializes in nonsurgical periodontal therapy, heart-centered education, and efficiency. Through her signature program, Thrive in the OP and Thrive Chairside Summit, she equips hygienists with evidence-based systems to elevate patient outcomes, confidence, and production. Amber blends clinical expertise with practical strategies to help dental teams implement sustainable, science-driven protocols. She can be reached at amberauger.com.