Update on psychiatric drug use: Medications pose a treatment challenge for dental professionals
By Lisa Dowst-Mayo, RDH, BSDH
According to the Centers for Disease Control, approximately 25% of the U.S. population suffers from mental illness.1 This means one in four of the people who present to your office could be taking a prescription medication for treatment of mental illness. Eight percent of Americans age 12 and older currently suffer from depression, and female patients have higher prevalence than male patients at every age group.2 According to Thomas Insel, MD, former director of the National Institute for Mental Health, "antidepressant use among Americans from 2005-2008 found that more than one in 10 Americans ages 12 and older report taking an antidepressant medication."3 It is likely you will see at least a few patients a week who take either an antidepressant or antipsychotic, and this article will provide a "refresher" for the private practice clinician on the pharmacology of those drug classes.
According to the IMS National Prescription Audit, the most profitable prescription medication in the United States, for the second year in a row, was aripiprazole (Abilify) with $6.9 billion in total sales.4 Aripiprazole is an antipsychotic medication that can be used in the treatment of a variety of disorders. Antipsychotics, through their mechanism of action on dopamine and serotonin, are effective in treating a patient's positive symptoms of mental illness such as hallucinations, delusions, and paranoia, and the negative symptom of emotional withdrawal.5 Duloxetine (Cymbalta), an antidepressant, was the sixth most commonly prescribed medication, and the eighth most profitable at just over $4 billion total sales in the U.S. in 2014.4
There are two major classes of medications used in the treatment of mental illness (e.g., schizophrenia, depression, bipolar disorder): antipsychotics and antidepressants.5,6 Like most other pharmaceutical drugs, these medications come with a variety of side effects due to their diverse actions in the body. The dental provider should be aware that many of these side effects can have adversarial effects on the oral cavity. Since these medications bind nonspecifically to muscarinic, alpha, and histamine receptors all over the body, a patient's heart rate, blood pressure, sense of balance, and muscle control can be affected.5
These side effects can alter the dental professional's management during patient treatment. This article will review the mechanism of action, side effects, and dental office management considerations for patients taking antidepressants and antipsychotics.
Mechanism of action: Antipsychotics
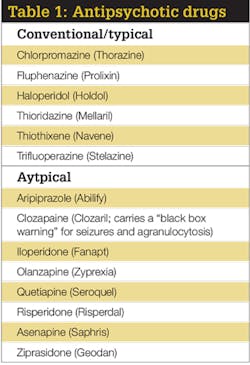
The antipsychotic's main mechanism of action is on the neural pathways involving the cerebral cortex and the limbic system.5 The limbic system is the portion of the brain that deals with emotions, memories, and arousal.5 It is believed that people with psychosis have excessive activity of neurotransmitters such as dopamine and serotonin.5 There are two main classes of drugs in the antipsychotic family: conventional/typical and atypical (see Table 1). Atypical drugs are the newer class and are more commonly prescribed, as they have fewer side effects than conventional/typical antipsychotics.
Dopamine has an important role in the etiology of psychotic disorders such as schizophrenia. Conventional antipsychotic drugs are dopamine antagonists; through their binding to dopamine receptors, mainly the D2 receptor, they decrease the amount of dopamine released into the synaptic nerve gap.5 This action is thought to cause the positive changes in behavior of those suffering from psychosis. However, because these drugs only alter dopamine levels, they are active against only the positive symptoms of the disorder and not the negative.5 Another major drawback to this class is their propensity to excessively block dopamine, which can lead to a severe condition known as extrapyramidal syndrome (EPS); this will be discussed in the next section. 5 (Editor's note: See Glossary for a list of unfamiliar terms such as this one.)
Atypical antipsychotic drugs block not only dopamine receptors, but also serotonin receptors, mainly the 5HT2A receptor.5 Due to this change in mechanism of action, as compared to conventional drugs, atypical antipsychotics are less likely to cause EPS.5 Atypical drugs are active against both the positive and negative symptoms of psychosis.5
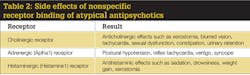
Both classes of antipsychotics bind nonspecifically to receptors in the body that are not their actual target.5 Due to this nonspecificity of receptor binding, these drugs will produce many undesirable side effects that can make compliance an issue for patients. Table 2 lists the receptors antipsychotics will nonselectively bind to and the resulting side effects.
Antidepressants
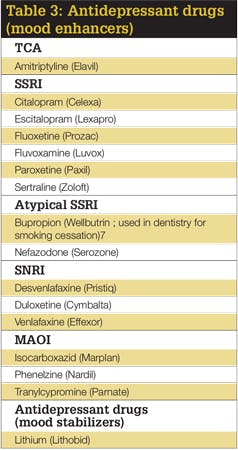
The treatment of depression greatly advanced when medicine developed a deeper understanding of depression and its association with altered serotonin and norepinephrine levels. When these neurotransmitter levels are altered, mental depression or mania occurs. When levels are higher, mania occurs; when they are lower, mental depression occurs.5 Drugs used in the treatment of manic depression (unipolar) generally increase the levels of serotonin, norepinephrine, or both in the synaptic gap by blocking reuptake.5 As a result, there will be an increase in serotonin and norepinephrine available for the body to use. This allows for greater neuronal activity, and alleviates the symptoms of depression. In the treatment of bipolar disorder, mood enhancers will be utilized during periods of depression, and mood stabilizers will be used during periods of mania (see Table 3).
Drug classes that are considered mood elevators are serotonin reuptake inhibitors (SSRIs), atypical SSRIs, selective serotonin norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), and monoamine oxidase inhibitors (MAOIs) (see Table 3). The most common mood stabilizing drug, which is used during periods of bipolar mania, is lithium (Lithobid).5,6 The only class of drugs that does not exert its action directly on serotonin and norepinephrine receptors are the MAOIs. They inhibit the enzyme monoamine oxidase, which is an enzyme that breaks down norepinephrine and epinephrine.5 MAOIs are often used as a last resort because of their many food restrictions and adverse reactions.5 Foods that contain tyramine (e.g., cheese, bananas, raisins, avocados, soy sauce, yogurt, sour cream, bologna, salami, hot dogs, sauerkraut, wine, beer, herring) must be avoided because tyramine causes the release of additional norepinephrine, and this could lead to hypertensive crisis or stroke.5,6
The SSRIs typically have fewer side effects than all other drug classes because they are more selective for their serotonin receptors, and do not bind as readily to nonselect targets.5,6 They were introduced to the U.S. market in 1988 for the treatment of depression, and since then have been used in the treatment of eating disorders, fibromyalgia, premenstrual syndrome, obsessive-compulsive disorder, and panic disorders.6
Side effects
Patients who are taking antipsychotics or antidepressants can experience many side effects. The anticholinergic and antihistaminic effects will predispose a patient to a multitude of issues such as increased heart rate, decreased blood pressure, sedation, xerostomia, weight gain, blurred vision, and gastrointestinal and urinary complications.5,6 If any drug excessively blocks dopamine, EPS can occur.5 This syndrome typically arises in 50-75% of patients who are taking conventional antipsychotics.5 The effects of EPS can become permanent, even after the patient stops taking the drug.5 Extrapyramidal effects include dystonia, parkinsonism, akathisia, and tardive dyskinesia.5
TCA, MAOI, and atypical SSRIs can adversely affect the cardiovascular and central nervous system and also impair the liver.5 Weight gain can be seen in patients taking TCAs and MAOIs.5 Weight loss is common in patients taking SSRIs.5 Sexual dysfunction is more commonly associated with MAOIs, SSRIs, and atypical SSRIs.5 MAOIs cause a wide variety of adverse effects such as blurred vision, tremors, seizures, urinary retention, constipation, and fatal liver damage.5 This contributes to the reason why many doctors consider them last-resort drugs.
Dental office management
The dental professional should use caution when administering dental local anesthesia with vasoconstrictors to patients taking antipsychotics and antidepressants that interact with adrenergic receptors in the body.6 The professional needs to avoid intravascular injections and be sure to aspirate carefully.6 Epinephrine and levonordefrin could cause hypotension and reflex tachycardia, and as such, a cardiac dose (2 carpules or 0.04 mg vasoconstrictor) should be used or avoided completely.6 This is especially true of patients taking antipsychotics and TCAs. There are no special concerns regarding the use of vasoconstrictors in patients taking SSRIs.6
NSAIDs (e.g., ibuprofen, naproxen) should not be recommended to control postoperative pain in patients taking SSRIs or lithium, as these will increase the levels of both drugs systemically.6 If a patient is suffering from extrapyramidal syndrome and experiencing dystonia, the dental professional should inquire if the muscles of the face, tongue, or neck are involved, as this is common in the disorder.5,7 If a patent is experiencing tardive dyskinesia, involuntary movements involving tongue, lips, face, jaw, and extremities are common and can lead to broken teeth, bruxism, tongue trauma, or ulcerations.7 TCAs and SSRIs have been shown to contribute to nocturnal bruxism and nightguards may be indicated as part of a dental hygiene care plan.
Xerostomia is a common side effect with both drug classes. Xerostomia counseling should be provided to patients, including frequent sips of water, salivary substitutes, fluoride use, and avoiding alcohol consumption.6,7 SSRIs generally cause the least amount of xerostomic effects of all antidepressant drugs.6
After reading this article, you should feel more confident in your knowledge of the adverse effects, mechanism of action, body interactions, and precautions indicated for the many patients in your practice who take antidepressants or antipsychotics. Knowledge of these medications will enhance your ability to work effectively with this population. RDH
Lisa Dowst-Mayo, RDH, BSDH, graduated magna cum laude with a degree in dental hygiene sciences from Baylor College of Dentistry in 2002. She is currently pursuing a Master in Healthcare Administration from Ohio University. She is the dental hygiene program director at Concorde Career College in San Antonio where she teaches pharmacology, special needs, and board review. She is a current board member of the Dallas Dental Hygiene Society and is a published author and national speaker. She can be contacted through her website at www.lisamayordh.com.
References
1. CDC Report: Mental Illness Surveillance Among U.S. Adults. CDC website. http://www.cdc.gov/mentalhealthsurveillance/. Updated December 2, 2013. Accessed March 4, 2016. 2. Morbidity and Mortality Weekly Report: QuickStats: Prevalence of current depression among persons aged ≥12 years, by age group and sex - United States National Health and Nutrition Examination Survey, 2007-2010. CDC website. http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6051a7.htm?s_cid=mm6051a7_w#x2013; United States, National Health and Nutrition Examination Survey, 2007-2010. Updated January 6. 2012. Accessed March 4, 2016.
3. Insel T. Director's blog: Antidepressants: A complicated picture. National Institute of Mental Health website. http://www.nimh.nih.gov/about/director/2011/antidepressants-a-complicated-picture.shtml. Published December 6, 2011. Accesssed March 4, 2016.
4. Schumock G, Li E, Suda K, et al. National trends in prescription drug expenditures and projection for 2014. American J Health-Syst Pharm. 2014;71(6):482-499.
5. Hinter H, Nagle B. Pharmacology: An Introduction. 3rd ed. New York: McGraw, 2012. 6. Weinberg M, Theile C, Fine J. Oral Pharmacology for the Dental Hygienist. 2nd ed. Upple Saddle River, New Jersey: Pearson, 2013.
7. Wilkins E. Clinical Practice of the Dental Hygienist. 11th ed. Philadelphia, Pennsylvania: Lippincott Williams & Wilkins Wolters Kluwer Health; 2012