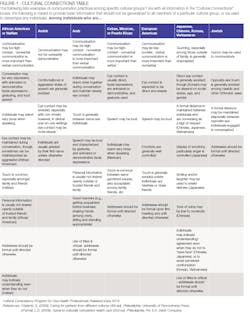
Cultural competency still struggles to be heard in US dental practices
By Elicia Lupoli, RDH, BSDH
Cultural and linguistic competence was introduced in the United States in 1995, when the Office of Minority Health (OMH) and Health and Human Services (HHS) established the Center for Linguistic and Cultural Competence in Health Care (CLCCHC). For years, research demonstrated health disparities in the US.1,2 In 2000, OMH HHS developed a set of national standards entitled “Culturally and Linguistically Appropriate Services” (CLAS) for the health-care field after revising and combining public comments.”3
The decision to develop the original 14 CLAS standards in 2000 was “to respond to the need to ensure that all people entering the health-care system receive equitable and effective treatment in a culturally and linguistically appropriate manner.”3
Due to the nation’s increased diversity, the Affordable Care Act, and other events, in 2013 CLAS was revised as the “enhanced National CLAS Standards,” and a blueprint was established to help implement 15 new standards.”4-6 Public comments were taken prior to issuing the the 2013 final draft. One addition was “encompass a broad definition of culture to include religion and spirituality; lesbian, gay, bisexual, and transgender individuals; deaf and hearing impaired individuals; and blind and vision impaired individuals.”4-6
While CLAS Standards and the accompanying blueprint were lawfully implemented into federally funded organizations,4-6 the guidelines that serve to reduce US health disparities and inequities impact us all if put to use. The combined cost of health disparities and subsequent deaths due to inadequate and/or inequitable care has been estimated to cost the US $1.24 trillion.7 According to the OMH HHS, “one of the most modifiable factors is the lack of culturally and linguistically appropriate services, broadly defined as care and services that are respectful of and responsive to the cultural and linguistic needs of all individuals.”4-6
Martin Luther King, Jr., said, “Whatever affects one directly, affects all indirectly ... I can never be what I ought to be until you are what you ought to be.”
Interpreting the language
“Cultural competency” means to understand the values, beliefs, and behaviors of diverse groups. “Linguistic competency” is the ability to communicate with those groups.4-6 When faced with cultural and linguistic challenges, clinicians may find it difficult to relay important oral health information. Barriers to communicate personal health information are generally present, in one way or another, and may not be immediately identifiable. Clinicians may become frustrated if they believe the patient did not follow their given advice, yet that assumption means the patient clearly understood.
Most practitioners are well aware that one size does not fit all especially with oral and systemic health challenges. The same holds true for communication and perception. By increasing awareness and knowledge of surrounding cultures and learning effective and efficient communication methods, the dental profession can assist in reducing oral health disparities and contribute to patient-centered collaboration.2 The ability to communicate and comprehend from provider to patient and patient to provider reduces the chances for health-care errors and resulting litigations.
Communication can be verbal, written, and nonverbal. A health provider may unknowingly express a variety of meanings without speaking any words. Nonverbal communication styles include paralanguage, which encompasses how words are expressed through tone, volume, and rate.8,9 Nonverbal volume may be indicated when writing or typing words in all capital letters, which has commonly indicated yelling. Two additional nonverbal styles include kinesics, or body language, and proxemics, the space between those communicating.10,11
An open mind to diversity
Aside from linguistic challenges, being open to cultural diversities may help with dental hygiene diagnosis and patient education. Early in my career, I saw many patients of Indian ethnicities with moderate and tenacious brown stain. I referred to my schooling and tried to associate it with bacteria or dietary habits. I found out through communicating in a nonjudgmental manner that they often cook with cumin and cayenne. I did not tell these patients to stop using the spices, but knowing the cause helped me find a way to fight the stains.
I also worked with a few patients of Asian descent. They had severe erosion and were highly sensitive to temperatures, regardless of topical or noninjectable anesthetic. I learned that people in their culture suck on lemons and eat a lot of fresh, raw hot peppers. This information informed me for future patients who may have these signs. I’ve been able to advise them about how to protect their enamel if they must consume acidic foods. This also helped the practice because I was prepared when I saw one of their family members.
My culture tends to communicate in close proximity with others. Often, I use touch by shaking someone’s hand in greeting or upon exiting. Keeping cultural respect in mind, these various types of communication techniques vary from one person to another. There are some who may not want to be more than four feet in proximity from another when communicating. As a health-care profession, learning and developing skills for communicating should be a constant process. Some clinicians are naturally more perceptive than others, whether a gift or years of trial and error. There is no need to be a fortune teller if this is not your forte, but always ask when uncertain. If the patient’s face is scrunched up into a ball, rather than wondering or not doing anything, ask the patient if he or she is OK; learn the patient’s preferences and then please document the preferences for the next clinician.
Linguistics in clude cues, signs, sy mbols, and writing.12 The Occupational Safety and Health Administration’s (OSHA) safety data sheets, previously called material safety data sheets, are a good example of symbols, as is the Wong-Baker FACES pain rating scale.
The OMH HHS advises against using children as interpreters for their parents who are patients.13-15 I have done this many times this many times when I have felt badly for a patient who could not understand me. The reasons to avoid using children as translators are solely for the protection of children. These include “putting the child in the parental role, possibly conveying the wrong message because the child’s emotional or cognitive understanding may not yet be mature, or leaving something out because they fear their parents’ suffering.”13-15 We have to do what is in the best interests of patients. When it comes down to patients not knowing what we are saying or asking their child to help, in my opinion, we should use our best judgment. A simple sentence may be, “Tell your mom it is very important that she have someone who can interpret our recommendations from today and to call us,” and then follow up if you do not receive a call back.
If there is no access to support staff in the language you need, seek out phone or computer interpretation. How many of us pull out our cell phones to use Google Translator? Sometimes it is not on point with the varying dialects, yet in a pinch we do what we can. It is helpful to know the most common languages of your patient population in order to be prepared. If you learn your patient cannot communicate with you, it causes stress to have to troubleshoot during the 30- or 50-minute appointment. This can lead to clinical errors, improper documentation, or losing the patient. There are ways to change the dental and medical histories and consent forms into other languages.16-18 If your practice has not had any instances of cultural and linguistic challenges, this will likely change. “The minority population is projected to rise to 56% of the total population in 2060, compared with 38% in 2014.”19
Communicating with another culture
When we need to educate patients on the state of their oral health, there are some techniques we can use, whether they speak English, have a low oral literacy, or have limited English proficiency. We know that we cannot force anyone to change, yet we cannot make the assumption that they don’t care until we’ve exhausted all methods of communication.
Motivational interviewing is a patient-centered communication method. It incorporates three elements: “Collaboration between you and your patient rather than confrontation; drawing out your patient’s ideas about change rather than imposing ideas; and emphasizing your patient’s autonomy rather than emphasizing your authority.” 21 Positive feedback is an ideal method,22,23 not only with cultural sensitivity, but also with coworkers, children, friends, and families.
The teach-back method is another method introduced for cultural and linguistic communication. This is a “research-based health literacy intervention that promotes adherence, quality, and patient safety.”24 This technique is used to make sure the clinician and patient comprehend what the other is saying. Dental providers should limit how much material they provide, and then have the patient repeat it to make sure the message is properly received.
Digging for answers
As dental hygienists, one of our jobs is leading patients towards health, oral and systemic, through prevention and education. We should not force patients into specific diets or ask them not to consume things they like. Even with smoking, I do my best to educate patients on the havoc it wreaks on their health. When they start hacking, I remind myself that they most likely already know how bad smoking is. I let them know I’m here for them when they’re ready to cease the habit. “Until you are ready to stop, how about you try this (…) to protect what you have left?”
I’ve treated many adolescents of various nationalities with black line stain. They were all swimmers. I learned their exposure to daily chlorine was a contributing factor for their stain. My point is that not every patient has textbook signs and not everything I see is in a textbook. This is why clinical judgment remains the other part of evidence-based dentistry.20 We must sometimes dig for answers, and that’s hard to do with language and cultural differences, as well as with the brief time we are allotted to see these patients.
When people realize that the care you provide is sensitive to their needs and they can communicate with you, their families and friends may also want to become part of the practice. Announce your strengths or current competencies on your website and social media. Make signs that say, “Handicap accessible,” “We cater to multiple languages,” or “Translation or interpretation services here.” Then give these patients a way to find you. Some marketable assets may include elevators for the disabled, room design for wheelchairs, and special lights or glasses for the visually sensitive. For those offices with televisions in the treatment rooms, turning on the closed captioning is a simple way to cater to those with hearing difficulties. Consider offering transportation options such as Uber or community van services. Offer OraVerse for children, or multilanguage educational brochures,25 many of which are free through the National Institute of Dental and Craniofacial Research. Consider changing your office hours to accommodate those with difficult working hours. In 2014, an estimated 70% of dental emergency room visits occurred outside of normal business hours in Maryland.26
Becoming aware of societal changes and cultures will lead to a better understanding of patients and help us to offer an environment more conducive to trust. Many clinicians want to know how to increase patient compliance. First and foremost is making sure that we understand what our patients are communicating. Listening is paramount. Effective communication is a two-way street that means both parties actively talking and listening.
Elicia Lupoli, RDH, BSDH, is on the editorial board for RDH magazine and Hygienetown, as well as an editor for her state association’s quarterly newsletter (ADHA Connecticut). Elicia attributes the start of her writing career to Shirley Gutkowski, RDH, BSDH, and other success to her many mentors.
References
1. National healthcare quality and disparities report and 5th anniversary update on the national quality strategy. (2015). Agency for healthcare research and quality, Rockville, MD. http://www.ahrq.gov/research/findings/nhqrdr/nhqdr15/index.html. Accessed August 11, 2017.
2. Chattophadhyay A. (2008). Oral health disparities in the United States. The dental clinics of North America, 52, 297-318. http://dx.doi.org/10.1016/j.cden.2007.11.001. Accessed August 11, 2017.
3. Office of Minority Health; National Standards on Culturally and Linguistically Appropriate Services (CLAS) in Health Care. https://www.federalregister.gov/documents/2000/12/22/00-32685/office-of-minority-health-national-standards-on-culturally-and-linguistically-appropriate-services. Accessed August 11, 2017.
4. Blueprint national standards for CLAS in health and health care: A blueprint for advancing and sustaining CLAS policy and practice. https://www.thinkculturalhealth.hhs.gov/assets/pdfs/EnhancedCLASStandardsBlueprint.pdf. Accessed August 11, 2017.
5. U.S. Department of Health and Human Services, Office of Minority Health [HHS OMH]. National standards for culturally and linguistically appropriate services in health and health care: A blueprint for advancing and sustaining CLAS policy and practice. http://www.thinkculturalhealth.hhs.gov. Accessed August 11, 2017.
6. National Standards for Culturally and Linguistically Appropriate Services (CLAS) in Health and Health Care. (2013). Federal Register, The daily journal of the United States Government. https://www.federalregister.gov/d/2013-23164. Accessed August 11, 2017.
7. LaVeist TA, Gaskin DJ, Richard P. The economic burden of health inequalities in the United States. Washington, D.C.: Joint Center for Political and Economic Studies.
8. Albert RD, Nelson G. Hispanic/Anglo-American differences in attributions to paralinguistic behavior. International Journal of Intercultural Relations, 17, 19-40.
9. Pennycook A. (1985). Actions speak louder than words: Paralanguage, communication, and education. TESOL Quarterly, 19, 259-282.
10. Shea SC. Psychiatric interviewing: The art of understanding, second edition. Philadelphia, PA: Sanders.
11. Poyatos F. New perspectives in nonverbal communication. Oxford: Pergamon Press.
12. Lusky K. Picture boards help those who can’t speak for themselves. ACP Hospitalist. http://www.acponline.org/hospitalist/jan08/pictures.htm. Accessed August 11, 2017.
13. Flores G, Laws MB, Mayo SJ, Zuckerman B, Abreu M, Medina L, Hardt EJ. Errors in medical interpretation and their potential clinical consequences in pediatric encounters. Pediatrics, 111, 6–14.
14. Campinha-Bacote J, Claymore-Cuny D, Cora-Bramble D, et al. (2006). Transforming the face of health professions through cultural and linguistic competence education: The role of HRSA centers of excellence. Health Resources and Services Administration, U.S. Department of Health and Human Services, Washington, DC.
15. Wilson-Stronks A, Galvez E. (2007). Hospitals, language, and culture: A snapshot of the nation. The Joint Commission website. http://www.jointcommission.org/assets/1/6/hlc_paper.pdf. Accessed August 11, 2017.
16. Basic health history available in translated languages, MetLife oral health library. (n.d.). https://oralfitnesslibrary.com/Multi-Language-Health-History-Forms. Accessed August 11, 2017.
17. Department of Health. Basic consent forms. http://webarchive.nationalarchives.gov.uk/+/http://www.dh.gov.uk/
en/Publichealth/Scientificdevelopmentgeneticsandbioethics/
Consent/Consentgeneralinformation/DH_4015950. Accessed August 11, 2017.
18. University of the Pacific. Basic health history and consent forms, dental practice documents. http://dental.pacific.edu/departments-and-groups/professional-services-and-resources/dental-practice-documents. Accessed August 11, 2017.
19. New Census Bureau report analyzes U.S. population projections. United States Census Bureau. https://www.census.gov/newsroom/press-releases/2015/cb15-tps16.html Accessed August 11, 2017.
20. Kishore M, Panat SR, Aggarwal A, Agarwal N, Upadhyaya N, Alok A. (2014). Evidence Based Dental Care: Integrating Clinical Expertise with Systematic Research. JCDR, 8(2), 259–262. http://doi.org/10.7860/JCDR/2014/6595.4076. Accessed August 11, 2017.
21. Rollnick S, Miller WR, Butler C. (Eds.). Motivational interviewing in health care: Helping patients change behavior. New York: The Guilford Press.
22. Bandura A. Self-efficacy: The exercise of control. New York: Freeman.
23. Sanson-Fisher RW, Campbell EM, Redman S, Hennrikus D. (1989). Patient-provider interactions and patient outcomes. The Diabetes Educator, 15, 134-138. doi: 10.1177/01457217890150020924. The teach-back method. http://www.teachbacktraining.org. Accessed August 11, 2017.
25. National Institutes of Health, National Institute of Dental and Craniofacial Research (NIDCR). Order free brochures. https://catalog.nidcr.nih.gov/OrderPublications/default.aspx?_ga=1.79332118.302370058.1419349565. Accessed August 11, 2017.
26. Nasseh K, Vujicic M, Romaine D. Diverting emergency department dental visits could save Maryland’s Medicaid program $4 million per year. Health Policy Institute Research Brief, American Dental Association. http://www.ada.org/~/media/ADA/Science%20and%20Research/HPI/Files/HPIBrief_1114_2.ashx. Accessed August 11, 2017.