Reassuring the anxious patient: Needle-free anesthetic options decrease sensitivity or pain during hygiene procedures
By Lory Laughter, RDH, MS
Every dental professional has experienced the fearful or anxious patient. The individual’s first words to you are, “I hate going to the dentist.” Dental fear or apprehension is a leading reason why appointments are not made, pain is self-treated, and why, even after all of your education efforts, patients do not return to complete care.
Six years ago, I met my first patient with real dental phobia. He didn’t tell me how much he disliked being in my presence. Instead we spent one full appointment talking about exactly what might happen in the dental chair. It took him seven tries to call and book the appointment, even though he knew some of the staff members personally.
He actually drove by the building or into the parking lot a number of times before he could come inside. This was a level of patient discomfort I had never witnessed. Thankfully, I worked in an environment where providing care was more important than production goals.
After rapport was built and the patient agreed to treat his periodontal infection, the biggest contributing factor to his fear emerged. He was worried about pain and severely afraid of needles. It has been reported that almost one-half of American adults experience dental fear of at least a moderate level. In fact, 5% to 10% of adults report avoiding dental care due to fear.1
A quick search of online blogs and chat groups highlight two issues discussed most prominently for why people do not seek treatment for dental problems - discomfort/pain and fear of needles. We practice in an exciting time where both barriers can be addressed successfully and easily.
Even patients who may not be anxious but experience sensitivity during preventive appointments are resistant to injected anesthetic. The objections can range from numbness interfering with work or other activities to simply not wanting local anesthetic when no drilling is taking place.
While these reasons may seem frivolous or minor to the dental hygienist, patients can have strong feelings on the matter. We cannot dismiss the fact that many have a real and often debilitating fear of needles - a fear that keeps those patients from seeking or keep dental appointments.
Options for gingival pain control
We practice in a time when needle-free options exist to make preventive care comfortable for sensitive and nervous patients. Depending on the type of sensitivity and the discomfort level of the patient, you can choose from pastes, varnishes, and topical anesthetics specific to the situation.
Research on professionally applied pastes at the time of hygiene treatment has shown a positive effect on dentinal hypersensitivity during nonsurgical periodontal treatment.2 While there was a decrease in dental hypersensitivity to air blasts immediately following application of the pastes, the studies also included daily use of a fluoride toothpaste at home to keep the sensitivity from returning post treatment.
Fluoride and strontium chloride3 varnishes have also been shown to be effective in decreasing dental hypersensitivity. Strontium chloride varnish such as Zarosen has a positive effect on dental sensitivity for up to 24 weeks after application. Fluoride varnish has shown to be effective in decreasing dental hypersensitivity with no significant difference in efficacy between the brands studied.4 Patient acceptance of varnish products is still being studied, and anecdotal comments from dental professionals indicate that acceptance is not high among adults.
Topical anesthetics are effective in decreasing gingival discomfort during nonsurgical periodontal treatment. In addition, these products are useful for routine prophylaxis in those patients with sensitivity. These products are easy to use and take little time to apply. Liquid anesthetic and periodontal gels for subgingival application provide comfort during gingivitis and periodontal treatment.
Gel anesthetic for subgingival use is available for treating gingival discomfort. Ultracare is a 20% benzocaine product which can be delivered into periodontal pockets by a syringe and plastic tip, and to surface of mucous membrane by a swab technique. It is indicated for minor irritation and pain associated with minor dental procedures. Benzocaine has a rapid onset, and the effect lasts for 8-10 minutes.
Oraqix contains a combination of prilocaine and lidocaine in a liquid state that becomes a gel after placement, extending the duration of anesthetic effect. Oraqix requires a special applicator with disposable cartridges and the applicator tip for this anesthetic gel is metal and somewhat wider than plastic tips. The combination of prilocaine and lidocaine creates an anesthetic effect with a fast onset (within 30 seconds) and duration of approximately 20 minutes. There is no added flavoring.
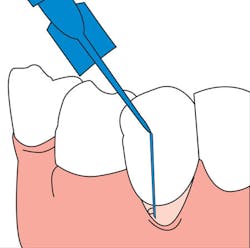
Cetacaine contains three active anesthetic agents and is available in liquid, spray, and gel forms. The liquid form is applied subgingivally into periodontal pockets by syringe and plastic tip (see illustration). Cetacaine Liquid provides quick relief for gingival sensitivity. The onset is almost immediate and the duration of effect is long enough to complete most nonsurgical treatments, such as SRPs (30 -60 minutes). Cetacaine in gel form is applied topically by swab to mucous membrane for pre-injections, or minor procedures that do not require injection. The spray form is indicated on-label for reducing the gag reflex. The flavor of Cetacaine is mild, and patient acceptance is favorable.
Patient selection for topical anesthetic
It is important to select the product appropriate for each patient being treated, making it necessary to keep the following in mind:
- The type of sensitivity - dentin or gingival
- The amount of time necessary to complete the treatment
- The level of anesthetic effect necessary for patient comfort
- Patient preference and acceptance
- Fears of needles or other concerns of the patient
When the sensitivity experienced by the patient is only dentinal in nature, a paste or varnish may be effective enough to make treatment comfortable. Pastes are shorter acting in duration and the effect is not always immediate, but may be more acceptable to the patient in taste or texture than a varnish. If longer duration of pain control is a goal, a varnish is a better choice than a paste. Strontium chloride varnish such as Zarosen goes on smoother and is thinner than most fluoride varnish and, therefore, may be preferred by the patient. Strontium chloride is also immediate in effect and lasts up to 24 weeks. Fluoride varnish should be considered for those with a higher caries risk. Pastes and varnish are most effective in areas of root recession where the surface is easily accessible for placement.
Typical gel anesthetic is appropriate for those who need supragingival sensitivity relief, such as pre-injection site numbing. The flavor of a gel anesthetic can be somewhat strong to cover the anesthetic taste, so patient acceptance also needs consideration. While allergic reactions are rare with topical anesthetics, it is important to note any possible allergies to the active ingredients.
Cetacaine Topical Liquid Anesthetic from Cetylite, Inc. has a mild banana flavor and is effective for nonsurgical periodontal procedures such as scaling and root planing or debridement. Cetacaine Liquid or Gel can also be used pre-injection and on any oral mucous membrane surface where topical anesthesia is needed, making it a good choice for supra- and subgingival use in decreasing sensitivity and creating a comfortable treatment experience for the patient.
The active ingredients in liquid Cetacaine are benzocaine, butamben and tetracaine hydrochloride at 14%, 2%, and 2% respectively. This combination allows for an almost immediate onset (approximately 30 seconds) and a duration of 30 to 60 minutes allowing time to complete most periodontal treatment appointments. It is effective for both quadrant nonsurgical treatments and preventive services where patient sensitivity is a factor.
Cetacaine in a liquid form is believed to have such a quick onset and long duration due to the unique combination of ingredients. Benzocaine provides a rapid onset of the anesthetic effect, but has a short duration of action. Tetracaine HCl has a slow onset but prolonged duration of effectiveness. These two ingredients are connected by the profound and intermediate onset and duration of butamben. This combination has been proven more effective than benzocaine alone.5
Patients who are fearful of needles yet need anesthetic for periodontal or preventive treatment are excellent candidates for liquid topical anesthetic. The ability to offer treatment that is comfortable and needle-free can also increase patient rapport and trust leading to more acceptance of recommended procedures in the future. Since it is easy to apply and cost effective, liquid topical is also a great choice for those sensitive to probing or exploring during periodontal examinations.
The needle-free delivery system of Cetacaine Liquid allows for accurate site-specific application, thus decreasing the amount of product needed for effective anesthetic benefit. The graduated 0.4 ml syringe and minimally invasive tip facilitate quick, precise, and comfortable application of product into the periodontal pocket. Patient acceptance of the product delivery as well as the consistency and taste are all favorable. Anxious patients appreciate the needle-free approach to anesthetic with the microcapillary plastic tip which is narrow and creates a stress-free subgingival application experience.
Benefits of Cetacaine Liquid include:
- Cost effectiveness - less than $2 to treat a full mouth
- Convenient - a luer-lock cap allows for ease dispensing into a syringe of choice
- Adjustable dosing - use only the amount of product needed for each situation
- Reduction of waste - each 30 gram bottle will facilitate up to 75 full mouth applications
- Acceptable taste - banana flavor is mild yet effective at covering the anesthetic taste
Precautions - The use of any prescription product should include knowledge of the precautions and contraindications included in the prescribing information and SDS form. Topically applied medicines rarely cause skin irritation, highlighting the advantage of a product which can be applied accurately to only the surfaces necessary. The clinician should adhere closely to dosing requirements and limits. The appropriate use of topical anesthetic agents during pregnancy vary so reading the prescribing information is essential.
Dental anxiety has long been a barrier in patients seeking or continuing treatment. Much of the anxiety experienced by nervous individuals is based on a perception of discomfort and/or a fear of needles. Products and techniques which allow us to offer more comfortable dental visits can decrease the number of broken appointments and increase the amount of dental care completed. Needle-free anesthetic options are a benefit in treating anxious or nervous dental patients.
By choosing the appropriate topical anesthetic agent, the dental professional can provide treatment with less discomfort for the patient leading to decreased anxiety about dental procedures. Prophy pastes, fluoride and strontium chloride varnishes, gel and liquid topical anesthetic agents are useful agents in decreasing root surface and/or gingival sensitivity. Care should be used in selecting the best needle-free pain relieving product for each patient circumstance.
Finishing the story
How did my experience with a fearful patient end? I was able to treat him with a combination of Cetacaine Liquid and low powered ultrasonic scaling. He was appreciative of the needle-free approach to care and even referred friends to our practice because of the “no stick” experience, suggesting they ask for the banana stuff in the dark bottle. The opportunity to work with this patient taught me valuable skills in comfortable care and gave him the reassurance that periodontal care can be a comfortable and needle-free approach to achieving periodontal health. RDH
Lory Laughter, RDH, MS, is an assistant professor at University of the Pacific, Arthur A Dugoni School of Dentistry in San Francisco. She is a paid clinical consultant for Cetylite.
References
1. Clay, R. Drilling down dental fears. Monitor on psychology. Vol 47, number 3. March 2016. Accessed on 7-17-17 http://www.apa.org/monitor/2016/03/dental-fears.aspx
2. Bekes K, Heinzelmann K, Lettner S, Schaller HG. Efficacy of desensitizing products containing 8% arginine and calcium carbonate for hypersensitivity relief in MIH-affected molars: an 8-week clinical study. Clin Oral Investig. 2016 Dec 21.] PubMed PMID: 28004247.
3. Kobler A, Kub O, Schaller HG, Gernhardt CR. Clinical effectiveness of a strontium chloride- containing desensitizing agent over 6 months: a randomized, double-blind, placebo-controlled study. Quintessence Int. 2008 Apr;39(4):321-5. PubMed PMID: 19081901.
4. Ritter AV, de L Dias W, Miguez P, Caplan DJ, Swift EJ Jr. Treating cervical dentin hypersensitivity with fluoride varnish: a randomized clinical study. J Am Dent Assoc. 2006 Jul;137(7):1013-20; quiz 1029. PubMed PMID: 16803829.
5. Adriani J, Mehta D, Naraghi M. Mixtures of local anesthetics: The Effectiveness of Combinations of Benzocaine, Butamben, and Tetracaine Topically. Anesthesiology Review. 1981; 12:15-19.