A room with a different view
How teledentistry is expanding and energizing practice settings
It’s vacation time! Spending time in the Big Apple has been on your bucket list for years. Now you’re standing right in the middle of the fabled Times Square. People of all sizes, ages, and nationalities are moving through the famous area. Some are old; others are young. Some are living on the streets; others live very comfortable lives. Some appear to be very healthy; others look frail and sickly. Times Square is a beehive of humanity.
The looming crisis
It takes a few minutes to soak in all the sights and smells. Glancing upward, your eye catches The Zipper, the famous New York Times news ticker. Headline after headline streams across the screen. The Zipper has been alerting crowds to breaking news headlines since 1928. Today is no exception. This moment’s visual sound bites are about oral health: Looming crisis—Lack of quality, affordable dental health affects millions in the US…Dental care: highest financial barrier of all health services…51 million lost school hours due to dental issues…Severe periodontitis associated with increased risk: stroke, heart disease, diabetes, chronic respiratory illness…50% of children age 5 to 9 have had one area of decay…RDH magazine reports Utah dental hygienist, Staci Stout, develops a sustainable business model that provides quality dental services to at-risk children and seniors. Stout works outside of a traditional dental office, harnessing the power of portable equipment and tele-dentistry communication platforms…
Your mind starts racing overtime. What? A dental hygienist who has figured out how to create her own business to provide care outside of a dental office? Who is she? Is her plan financially viable? Anxious to know the details, you click on your phone’s RDH magazine’s Facebook site. There it is, the whole article in the December 2017 issue!
Going in agonizing circles
Dental hygienists are charged with many duties beyond scaling and polishing. Often employers and administration look to staff to support patient retention efforts or help maintain a full, productive schedule. With tongue in cheek, consider the list of strategies we currently rely upon to fulfill retention and productivity goals.
An overworked recare system…seriously, how many messages can be left before it is legal to issue a restraining order?!
A series of inappropriately timed, guilt-based text messages?
Double booking and hoping that half of the patients don’t show up? Not a good plan for anyone’s blood pressure—operator or patient.
Charging patients a fee for a missed appointment? Throwing good money after bad money, requiring yet another employee to spend time trying to collect a fee that is never the financial equivalent of the original appointment…and risking a bad review online.
And finally, hoping and praying that every time the phone rings, the right person will miraculously be on the other end of the line, requiring the very services that the dental hygienist can offer at that particular time.
These resolutions are rarely effective…and just serve to antagonize the patient!
Staci’s strategic timeline
In 2015, the Utah state legislature approved changes to the Utah practice act that governs the activities of dental hygienists. The new law allows people in underserved populations and in a variety of different settings direct access care provided by a dental hygienist. Alternative practice settings include: assisted living facilities, subsidized senior housing, certified nursing homes, community health centers and school-based programs.
At the time, Staci was offering three evening clinics in an elementary school setting in collaboration with Sealants for Smiles, Utah’s first public health dental hygiene clinic. The focus was on families of students from the school.
Three months later, she launched Senior Smiles, an oral health program funded by an ADHA/Wrigley grant that provides services to residents at a Salt Lake City area assisted living facility.
In August 2016, Staci added MouthWatch’s TeleDent Exam Tab to the program for the seniors. In the same month, she helped a community health center, Utah Partners for Health, set up a Public Health Dental Hygiene Model.
In February 2017, Staci launched Happy Healthy Smiles, a mobile dental unit program, in collaboration with the Senior Charity Care Foundation. This new program, supported by funds from the ADHA/Wrigley grant, provides care for residents living in senior subsidized housing and utilizes MouthWatch’s TeleDent program and Dentimax’s cloud-based technology.
In May 2017, Utah’s governor signed legislation allowing telehealth exams. According to Staci, teledentistry legislation is not far behind and she fully expects to be able to bill for examinations by January 2018.
Not waiting for any grass to grow under her feet, Staci begins collaborating with Dr. Tanner Clark in August 2017 on a new project called Smart Smiles School-Based Oral Health Program. Dr. Tanner shares Staci’s passion for teledentistry, and his brick-and-mortar dental office is literally upstairs from the elementary school. Together, they are creating a model for school-based programs.
In October 2017, the Utah Dental Hygienists’ Association and the Senior Charity Care Foundation received funding from the Federal Grant for Certified Nursing Homes to provide oral health care in 10 nursing homes, allowing up to 600 residents to receive care over the next year. Dr. Tanner Clark is a collaborative provider dentist for the project, which will utilize teledentistry as part of the project.
The nuts and bolts
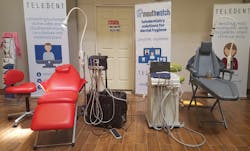
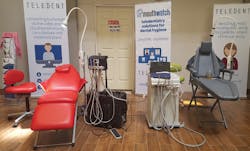
It takes a collective vision to put meaningful, sustainable programs together that are financially viable. Companies such as DNTLworks that specialize in portable and mobile dental equipment are joining forces with experts in teledentistry, such MouthWatch, to create opportunities that allow clinicians to deliver comprehensive evaluations as well as clinical care.
Dental hygienists are also collaborating with dentists to find ways to bring a full range of diagnostic and treatment services that include both dental hygiene and dental procedures to people who have been falling through the cracks. At times, all care is provided remotely, while in other circumstances diagnostic services are done off-site and then treatment is scheduled in a traditional office. Combining teledentistry technologies with portable equipment is creating new opportunities to improve access to care in Utah.
Staci said, “It’s an exciting time to be in dentistry. There are endless needs for oral care and we can make a huge difference to underserved populations by utilizing the technology that is available to us. As we work collaboratively with a dentist, it becomes critical to have a communication pathway that allows the hygienist to follow-up on patient needs with the dentist.”
Teledentistry, modeled on the success of telemedicine, has been the avenue to make that happen. By utilizing cloud-based dental software and an intraoral camera system, a dental hygienist can communicate patient needs in real time anywhere there is an internet connection. The cloud allows the collaborative dentist to view the patient’s intraoral photos and videos, review the medical and dental histories, and treatment records on a patient who may be miles away. The dental hygienist and the dentist work together to provide a treatment plan and discuss the best available options with the patient. Patients can ask questions, get answers, and have their concerns addressed. Care can often be provided on the same day. This real-time process is called synchronous teledentistry.
The MouthWatch/TeleDent software program that Staci uses allows her to provide care in multiple settings and still have access to a dentist who can provide consultation, if needed. If live communication between the two providers is not possible, she is able to store the patient information in a HIPAA compliant format that is available for the dentist review later. This store-and-forward process is called asynchronous teledentistry. Ultimately, the goal for either of these initial services is to help patients establish a relationship with a dentist and find a permanent dental home.
Young or old, one at a time
Dr. Tanner Clark is a young dentist with a big vision about how to best serve people. His thoughts are refreshing: “Teledentistry is very new to us and we are approaching it with eyes wide open. We have considered what others are doing in other places and we are incorporating some ideas of our own. Ultimately, our work, in collaboration as providers, is allowing us to reach out to, and physically go to people with the greatest need, people who are rarely capable of getting the care they need for themselves.”
His focus is on prevention—one patient at a time, a senior citizen, a child, or a disabled individual. Most of the patients have not had preventive dental care in over five years, or have only been to the dentist for emergencies.
Each patient receives a real-time, live digital exam, which is supplemented by the data that has been collected—x-rays, intraoral photos and videos, probing depths, mobility readings, and oral cancer screenings. On occasion, DIAGNOdent readings or CariVu images are also used. It is possible to compile and forward all data to any dental provider using the MouthWatch platform. According to Dr. Clark, combining these technologies creates better diagnostic results.
The remote digital exam allows a diagnosis prior to making a trip to a traditional dental office, where a comprehensive treatment plan is developed. This approach is more efficient when providing care for people with barriers: children, and aging populations with increasing health complications. Dr. Clark says, “Our target patients are those that don’t go to the dental office. We go to them!”
Old models not working well
Over the past 50 years, many dental schools have closed. While a handful of new programs have opened, there are many fewer dental graduates today than decades ago. In addition to fewer dental schools, approximately half of all dental students today are women. Most female dentists balance clinical time with family responsibilities. They tend to work fewer hours in the clinical setting than their male counterparts.
In addition to these demographic shifts, the debt load from a dental school education now exceeds well over $200,000. This creates a huge financial burden for a newly graduated dentist. For many, there is a big incentive to make as much money as possible to pay off student loans, an understandable goal.
In direct contrast to what is happening in the dentist community, dental hygiene programs are popping up everywhere. Graduating students are finding it increasingly difficult to find adequate employment in a traditional dental office. Today there is a pool of highly educated, experienced dental hygienists who need more employment options or who are burning out because of the accelerated pace expected many offices.
The size of the problem
“Houston, we have a problem” is an often-quoted remark from the 1995 movie, Apollo 13, and can be readily used to describe the burgeoning crisis in dental health-care delivery today. There are many contributing factors that are leading to a system that can no longer provide for the oral health needs of many in our nation.
Adult dental visits declining in all income groups.
Only 66% of adults had any kind of dental visit in last 12 months.
47% of adults age 30 or more has periodontitis.
Severe periodontitis and edentulous rates—twice as high in poverty.
49% of adults age 45-64 have untreated dental caries.
70% of adults 65-plus have severe periodontitis.
One quarter of all tooth decay is untreated.
#1 chronic disease in children is dental caries.
Dental caries in children are five times more common than asthma.
Oral pain is the #1 reason children visit school nurse.
After a nurse’s dental referral, only 5% seek treatment.
78% of all children have had one area of decay by age 17.
Children in poverty have twice the decay rate of others.
40% of poor adults have at least one untreated carious lesion.
Annual dental visit: Less than ¼ of Medicare recipients below poverty level.
According to a survey published in DentistryIQ by Mark Hartley in March 2017, 66% of dental hygienists express some degree of occupational burnout that ranges from “sometimes, too often, or always.” Subsequently, a PennWell survey in June 2017 reported that 76% would consider practicing in an off-site location, as an employee of a dentist, dental hygienist or physician, if all practice act obstacles were removed, and 52% of dental hygienists would consider owning their own dental hygiene practice.
The cost of providing care is rising, and so are treatment fees. To further complicate delivery models, most dental professionals live in large urban or suburban areas, leaving many towns and even whole counties without any dental facilities or enough health care providers—a dental desert, so to speak.
The maldistribution of dental health-care workers, along with increases in the cost of delivering care, is made more problematic by transportation and portability issues. When people are challenged to be seen in a traditional dental office, dental disease issues become more complex, resulting in more complicated treatment at higher fees in the future.
Teledentistry expands care delivery
While the programs that Staci Stout and Dr. Tanner have implemented are innovative and exciting, there are many other ways health care delivery can use teledentistry technology to serve more people, addressing many of the reasons for the current health-care crisis. It is important to understand a state’s practice act regarding supervision, as well as laws regarding telemedicine and teledentistry. What can and will work in one state may be entirely different in another. But practice acts are changing and expanding rapidly all over the country and telehealth models are quickly expanding to fill unmet needs.
Imagine a mobile health-care vehicle equipped to provide both medical and dental treatment to people in underserved parts of a state. Consider a mobile RV-type unit that could go from town to town. Teledentistry allows clinicians to conduct both real-time examinations and consultations in addition to being able to store valuable diagnostic data that can be accessed later by off-site dental specialists, activities that facilitate and streamline both diagnoses and treatment. This unique type of mobile unit can be equipped to offer a range of preventive and restorative dental treatments and also be set up to provide general medical needs.
The curriculum for second-year dental students at New York University now includes instruction on utilizing teledentistry concepts in the clinical setting. Students use the MouthWatch intraoral camera on a mannequin to document treatment needs and for writing up clinical notes and treatment requests on a tablet. The data and narrative are transferred via the cloud to another student who is taking the role of the dentist. A HRSA grant is funding this innovative educational program.
During the 2017-18 academic year, NYU launched another innovative approach to using teledentistry to widen the reach of dental services via live streaming to store-and-forward platforms. When there is a need for an oral health consultation, but no dental professional is available, non-dental professionals will now be able to conduct a visual screening using an intraoral camera paired with a tablet to record oral findings in settings like pediatric medical clinics, adult clinics, hospitals, and other settings. Patients will get the advice and treatment referrals from NYU dental faculty and fourth-year dental students who review the information to facilitate diagnosis, treatment planning and appointment coordination.
Outlook for rural care
More solo dental practices are facing some very dramatic changes when the owner contemplates retirement. The current trend is to sell the practice to a large corporate group, but that is less likely in more rural settings. Factor in the challenge a community faces when the only dentist in the county can’t find a buyer. Unless a creative solution is found, patients are left with the only option to drive hours to receive care, and the local dental hygienist will be out of work.
Every state in the US has at least one dental health shortage area, leaving 33 million patients underserved. Teledentistry can fill the gap.
While still maintaining a thriving practice in a nearby city, a Colorado dentist purchased a small practice from a retiring dentist in a remote area. He was able to keep the local hygienist on staff. As an employee, working alone, she treats residents in her small town. If needed, the doctor is available for a live consultation. In most cases, though, he reviews notes, clinical images, x-rays, and health histories through asynchronous teledentistry.
He is then able to diagnose, treatment plan, and schedule restorative patients for his visit one day a week to his secondary rural location.
If you entertain the thought that you are stuck providing care inside the four walls of your current office, think outside of the proverbial box. Depending on your state’s definition of general supervision, there may be ample opportunities to expand your options as an employee, contribute to the financial health of the practice, and increase your compensation by creating new revenue streams. While teledentistry and portable equipment are critical tools for those working in a more traditional public health role, these technologies can also play an exciting role in how dental hygienists deliver care as employees of a traditional dental office delivering care in non-traditional settings.
Hope is Not a Plan
Before you think your dentist employer will never entertain a new way for you to work, read the sidebar and consider how our minds can trap us into thinking change and expansion are not possible.
Instead of being a slave to an ineffective set of solutions that are put in place all too often, consider the option of actively reaching and treating new patients from outside the walls of the traditional treatment room. Imagine offering dental hygiene services with portable, live-streaming video options—making access to care, screenings, referrals, treatment planning and consultations more effective and easy to execute.
Teledentistry does not change the services that are offered to a patient. It is a communication tool that connects patients to dental professionals. It takes our world into their lives instead forcing patients to live with our hours, our traditional locations and our rules. The benefits of teledentistry are no longer limited to the public health sector of dentistry. Legislative changes are making these shifts possible and dental manufacturers have developed products and technologies that can benefit to private practitioners, as well. Those in private practice can learn from the flexibility and adaptability that has been a cornerstone of public health endeavors.
Staci said, ‘It’s an exciting time to be in dentistry. There are endless needs for oral care and we can make a huge difference to underserved populations by utilizing the technology that is available to us.’
The financial investment can be minimal or more complex as the demand or range of services grows. A basic portable dental unit can be the foundation for preventive services offered in a variety of locations: nonurgent health-care center, a local nursing home or senior center, after-school daycare, or concierge dental services at a local business renowned for its extensive dental insurance coverage for its employees. Services could range from screening and oral hygiene instruction, to full prophylaxis, to a live evaluation, or a share-and-forward evaluation that could lead to an immediate diagnosis and treatment plan.
Consider the benefits from a patient’s perspective. Patient-initiated visits will reduce patient time away from work and, more than likely, also reduce broken appointments. Providing services off-site might better mesh with a patient’s daily activities or potentially reduce travel time to secure initial evaluations or services. A preventive screening could expedite the diagnosis of a serious condition, possibly reducing future costs of dental or medical care or the need for an after-hours emergency room visit. Instead of “firing” a chronic no-show patient, why not offering them one more chance with an initial teledental encounter?
Many studies demonstrate patients are as satisfied with telemedicine appointments as they are with an in-person medical visits. There is no reason to believe that this will be any different for dentistry.
The current health-care model is strained. Health-care providers are clustered in urban areas. Costs are out of control, health care providers are stretched thin, and transportation to an appointment is a poor use of time and resources.
Shift is happening. Consider the impact of technology on retail purchases. Health care can learn a lot from that market segment. Millions of people now make purchases online, have interactive chats with companies, and then pick up their purchases at a local distribution center or have a product directly shipped to their doorstep.
It is only a short matter of time before dentistry will need to figure out how to restructure its delivery model. It may very well be that the future of all dental professionals is a hybrid of treatment in a traditional setting, supplemented by evaluations and care supported through the advances in teledentistry and portable dental equipment. What worked well 50 years ago for health-care delivery will not work in today’s world. While health care will never be able to mirror the retail sector model 100%, we need to be nimble and learn to deliver care in innovative ways that will serve the patients that need our care.
Anne Nugent Guignon, RDH, MPH, CSP, provides popular programs, including topics on biofilms, power driven scaling, ergonomics, hypersensitivity, and remineralization. Recipient of the 2004 Mentor of the Year Award and the 2009 ADHA Irene Newman Award, Anne has practiced clinical dental hygiene in Houston since 1971, and can be contacted at [email protected].
Cindy M. Purdy, RDH, BS, has 37 years of clinical dental hygiene experience. She is currently able to offer her clinical skills to her small rural community in Colorado, with the benefit of teledental technology. She holds an ergonomic certification from Colorado State University. In 2013, she earned her Certified Ergonomic Assessment Specialist credential, with emphasis on improving the health and performance of dental professionals by creating safe, in-office workstations. She also provides ergonomic programs for dental hygiene students throughout the country. Cindy can be reached at [email protected].
References
1. Lyuboslavsky V. Telemedicine and telehealth 2.0: a practical guide for medical providers and patients -
2. Cuyler R, Holland W. Implementing telemedicine: completing projects on target on time on budget. Xlibris Corp - 2012
3. Variation in dental hygiene scope of practice by state. http://www.oralhealthworkforce.org/resources/variation-in-dental-hygiene-scope-of-practice-by-state/
4. US Department of Health and Human Services. Oral Health in America: A Report of the Surgeon General--Executive Summary. Rockville, MD: US Department of Health and Human Services, National Institute of Dental and Craniofacial Research, National Institutes of Health, 2000.
5. Vujicic M, Nasseh K. A decade in dental care utilization among adults and children (2001-2010). Health Serv Res. April 2014; 49 (2): 460-480.
6. American Well 2015 Telehealth Survey: 64% of consumers would see a doctor via video. www.americanwell.com/press-release/american-well-2015-telehealth-survey-64-of-consumers-would-see-a-doctor-via-video
7. Eke P, et al. Prevalence of periodontitis in adults in United States: 2009 and 2010. J Dent Res 2012 Oct:91(10):914-20.
8. Personal contact. Staci Stout, RDH; Tanner Clark, DDS. October 4, 2017.
9. Study: Nearly half of referrals made to dental specialists go unfulfilled. Dent Econ. June 2008.
About the Author
Anne Nugent Guignon, MPH, RDH, CSP
ANNE NUGENT GUIGNON, MPH, RDH, CSP, has received numerous accolades over four decades for mentoring, research, and guiding her profession. As an international speaker and prolific author, Guignon focuses is on the oral microbiome, erosion, hypersensitivity, salivary dysfunction, ergonomics, and employee law issues. She may be contacted at [email protected].

Cindy M. Purdy, BSDH, RDH, CEAS
Cindy M. Purdy, BSDH, RDH, CEAS, has a passion for workplace wellness that has resulted in the creation of THRIVE, a dental-oriented wellness and therapeutic alternatives summit for dental professionals. THRIVE occurs three to four times annually at Glen Eyrie Castle in Colorado Springs, Colorado. Attendance information can be found at cindypurdy.com. In addition to multiple decades as a clinical dental hygienist, Cindy holds an ergonomic certification from Colorado State University, a certified ergonomic assessment specialist credential, and is certified in health-care ergonomics.