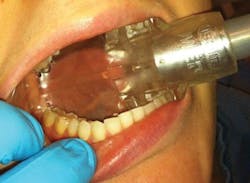
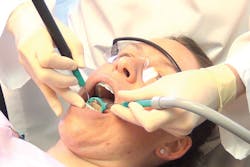
High-volume evacuation: Aerosols—it's what you can't see that can hurt you
By Laura Emmons, RDH, Cheri Wu, BDSc, RDH, and Tia Shutter
The time is now for HVE use. Recently, a dental hygienist contracted a virus at work, and an illness came on so quickly and aggressively that she ended up taking a whole month off at home to recover. Eventually, all of the other staff at her dental office, including the front desk and clinicians, contracted the same virus. After a month-long recovery, another hygienist described it as “the worst virus [she had] ever experienced.” She was concerned. The dental office required that clinicians use personal protective equipment (PPE), such as masks, gloves, eye protection, and proper lab coats; however, the office did not require a high-volume evacuator (HVE) as recommended in the CDC guidelines as a part of its safety protocol for working with powered instruments. Making matters worse, the vacuum pump lines were clogged with buildup that inhibited the airflow and limited the performance of the evacuation equipment at that office.
Illnesses are commonly shared in the workplace, but the risk of exposure is significantly higher for hygienists using powered instrumentation such as ultrasonics and air polishers.1 Bacteria and viruses can spread rapidly through splatter and aerosols produced by these types of treatments. The anecdote above was the firsthand experience of one of the hygienists at the clinic mentioned. While it can’t be proven that the viral infection she contracted was spread via contaminated aerosols resulting from powered instrumentation, this is certainly a hypothesis to explain the office-wide epidemic.
Powered instrumentation technologies are widely used in North America, but safety standards and regulations have not evolved with them. Only 24 out of 50 states in the United States claim to follow the Centers for Disease Control and Prevention (CDC) infection control guidelines.2 While HVEs are a recommended solution for controlling aerosols and reducing the risk of contamination,3,4 many clinicians are still allowed to choose any suction device they prefer. Saliva ejectors and isolation devices are a common choice, even though they offer no safety protection from contaminated aerosols.
Dental health-care professionals, educators, and governments are faced with urgency to improve health safety in dentistry. Some US states and Canadian provinces have already mandated that HVEs be used with all ultrasonic and air polishing procedures.2 Infection control guidelines, standards, and regulations are currently under review by the US Department of Health. We anticipate that this review will result in new and updated rules, including a mandate requiring the use of HVEs, across many more states. This needs to be a universal requirement, and it should be publicized with the same rigor as the antismoking campaigns that resulted in bans on smoking in public places in the 1990s.
What is HVE?
A high-volume evacuator is a suction device that draws a large volume of air over a period of time. This differs from a low-volume evacuator (LVE), which pulls a significantly lower volume of air. Air volume is measured in cubic feet per minute (CFM), and while both HVEs and LVEs maintain the same static vacuum pressure, the difference in air volume is due to the bore hole size, or the number of holes in the evacuator tip
HVE devices typically have large, single-bore or multiple openings, whereas LVE devices have a much smaller bore size. The standard HVE device used in dentistry has a large opening and is attached to an evacuation system that will remove a volume of air up to 100 cubic feet per minute.
Why do we need HVE?
Research shows that aerosols and splatter produced by ultrasonic and air polishing treatments contain saliva, blood, bacteria, and pathogens.5 Once airborne, aerosol particles can linger in the operatory for an hour or more while splatter lands on the surfaces immediately surrounding the treatment area. This poses a risk for the spread of the common cold and influenza viruses, herpes viruses, pathogenic streptococci or staphylococci, severe acute respiratory syndrome (SARS), and tuberculosis (TB).3
While vaccines for viruses such as the flu and H1N1 are available, neither the CDC nor the American Dental Association (ADA) mandate vaccinations as a preventive safety measure. For illnesses such as TB or SARS, these agencies recommend that patients avoid elective dental procedures altogether or have treatment done in a hospital.5 The number of tuberculosis cases in the United States rose in 2015 for the first time in 23 years, according to the Washington Post.6 Undiagnosed or undetected cases are of particular concern. A mandate for using HVEs as a preventative safety measure is urgently needed - now more than ever.
HVEs offer the best solution for controlling aerosol particles before they leave the mouth. Studies have shown that an HVE can reduce 90% to 98% of aerosols, regardless of source.1 As there is no single solution that will provide complete protection, a combination of protective measures - such as PPE, preprocedural rinses, prepolishing, an advanced air filtration system, and an HVE - offers the most effective and practical method of reducing the overall risk of infection.4
HVE devices also offer better assurance against potential liability claims and a compromised public perception of the dental industry as a whole. From epidemics to fatalities, a single infection can lead to disastrous results. Until regulations and monitoring are implemented and enforced, the burden lies with individual dental teams to ensure that they are taking every measure necessary to maintain safe and sanitary working environments.
What kinds of evacuation devices are available?
Evacuation devices on the market today vary by the function for which they are designed. For ultrasonic scaling or air polishing, the goal is not just water management; it is aerosol containment and controlling the risk of disease transmission. Saliva ejectors, isolation devices, and standard HVEs are among the most commonly used evacuation devices on the market today. Each of these has been studied for its effectiveness in reducing aerosols produced by powered instrumentation.
Compared to saliva ejectors, HVE devices can reduce up to 90% of particles reaching the clinician.4 The diameter of a saliva ejector is too small to be effective in removing aerosols. According to Stephen K. Harrel, DDS, “a saliva ejector does not qualify as a high-volume evacuator.”1 A Journal of the American Dental Association research report compared a saliva ejector to an isolation device and examined aerosol and splatter reduction during and after ultrasonic scaling.7 The study’s findings showed that neither device effectively reduced aerosols and splatter, nor was there a significant difference in the reduction of aerosols and splatter between the two devices.7 On the other hand, through his extensive research, Harrel concluded that a standard HVE tip could remove 90% to 98% of aerosols, regardless of the source, and that HVEs prove an effective solution for containing aerosols and reducing the risks of contamination.1
While the results of the HVE studies are impressive, the conditions when operating in a clinical environment can be quite different from test environments. In the field, hygienists must not only be able to efficiently use the device in patients’ mouths, but they also must be able to depend on the vacuum system and equipment provided at their dental clinics, where age and other conditions may impact performance. They also need to work steadily in patients’ mouths, ensuring their comfort, often while performing precise treatment with powered instruments for a prolonged period of time. These are variables, not necessarily present in test environments, that may challenge the performance of an HVE device.
How is evacuation measured?
Vacuum gauges on evacuation equipment show the level of airflow (cubic feet per minute, or CFM) set by the manufacturer or service technician. The setting range depends on the size of the evacuation motor, the clinic, and how far the air has to travel from the motor to the user end.
The only way to know whether an HVE device is working properly, however, is to test the volume of airflow coming out at the terminus or user end. Conditions such as age and strength of the equipment, buildup in the evacuation line, and the number of users on the system can significantly impact the airflow at the user end. Unfortunately, these variables are often overlooked. There are no testing standards to measure airflow at the user end.
So how can we tell if the power and volume of the HVE suction system are performing adequately? A simple timed water test is an easy way to test a device for suction performance at the user end.
Timed water test - Start with a straight-tip HVE and use a timer to measure how long it takes to pull up eight ounces of water. This will establish a control suction rate. Then measure the other devices against the control rate to get an idea of how different evacuation devices compare with the standard HVE device.
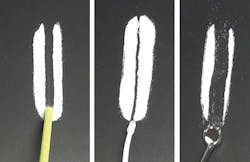
Scientific tests - To compare breadth of suction between instruments, we performed tests using equal amounts of salt and sifted talc powder to simulate small particles and determine how different suction devices perform as they draw in the mediums.
In Figure 1, we placed salt evenly across a smooth flat surface. Using a straight-tip HVE device, a saliva ejector (LVE), and an HV evacuation mirror, we drew up the salt, pulling each device through the salt at the same speed. In Figure 2, we repeated the process using talc powder.
The results were impressive. Due to the wider hole placement around the mirror head, the HV suction mirror was able to inhale a swath of particles that was two times wider than that left by the straight-tip HVE device.
Key Challenges in HVE Use
As suction is secondary to the dental procedure being performed, clinicians tend to choose devices that offer the greatest convenience and comfort so that they can focus on the primary task. Since saliva ejectors are widely used as handheld and hands-free, they are typically an easy option and a first choice for managing pooling water. However, as previously mentioned, saliva ejectors are a poor choice for use with powered instruments. While an HVE is a better option, three factors can affect acceptance and clinical application of this technology: performance, mobility, and ergonomics.
No. 1 Performance—Clinicians need to know whether the power and airflow volume of their HVE systems are performing safely. There are many devices on the market today that fit HVE ports but perform as LVEs. Because there is not a standard safety measurement for air quality and vacuum performance, clinicians must rely on data from independent tests and manufacturer tests to determine the effectiveness of their devices.
As previously noted, vacuum performance can vary depending on the conditions of the system. A system can have clean lines and exhibit adequate airflow yet also have an extremely low static measurement of vacuum pressure (mmHg). This is when backflow could be experienced. In another example, an evacuation system might show a high static reading but have clogged lines, resulting in low volume. When there are more users on the suction system loop, such as in large offices, it tends to lower the volume and pressure. Most office suction systems have enough strength to remove pooling water, but the lines can still get clogged, reducing suction volume performance.
No. 2 Mobility—In order to work properly, HVE devices need to be held approximately 6-15 mm away from the active ultrasonic tip or air polisher. For example, the device cannot be placed in the back of the mouth like a stationary device while the clinician works in the front of the mouth, and vice versa. Mobility is the key, and there are at least a dozen locations within the mouth that clinicians need to access with HVE. The straight, long shape of the standard HVE tip can be awkward to handle. Clinicians also need to pay careful attention to tip angulation to avoid getting the suction locked on a patient’s cheek or tongue. Ultimately, clinicians need to be able to move the suction device within the mouth without causing discomfort, all the while keeping focus on the treatment they are performing.
No. 3 Ergonomics—Ergonomic limitations can make the clinician’s job more time-consuming or difficult to perform, or they can cause long-term injury:
- A normal HVE hose weighs approximately one pound and feels very stiff to manage. Hygienists often complain of too much pull on the wrist and arm, which can lead to a repetitive strain injury.
- Because HVE devices are handheld, clinicians are unable to use their mouth mirrors for indirect viewing. Reliance on direct vision can cause excessive strain on the neck by stretching over the patient to see what they are doing as they work.
- Due to limited visibility, clinicians typically have to take extra time to put down the HVE device, check all areas with the mouth mirror, and then rescale the spots they missed. Better functionality and efficiency is important for completing tasks within the allotted time.
Ultimately, the question should be “Which HVE system is most effective for aerosol reduction while maintaining clinician ergonomics, ease of use, and patient comfort?”
How do we address these problems and encourage hygienists to use an HVE device as a safety standard for all ultrasonic treatments? In order to get hygienists to embrace HVEs for safety and efficiency with powered instrumentation, the following concerns must be addressed.
Device design
New HVE devices offer solutions to the ergonomic and mobility challenges of the standard straight-tip model. Beginning with performance, clinicians need to look for devices that operate at higher-velocity evacuation levels for reducing aerosols and splatter. From an ergonomics and mobility perspective, clinicians need to look for design elements that offer:
- Full mobility and easy handling in all areas of the mouth;
- Broad-sweep suction that inhibits the device from sucking up tissue;
- A lightweight design that reduces the risk of injury; and
- Multifunctional capabilities that eliminate the need to switch devices midprocedure.
One example of an HVE solution that meets the criteria listed above is the HV Evacuation Mirror System by Nu-Bird Inc.
Regulations and certification
Currently, the health and safety of hygienists, office staff, dentists, and patients are too loosely guarded. Tighter controls are needed. Dental health-care professionals must be made aware of the risks associated with aerosols and splatter produced by ultrasonics and other devices. With so much at risk, governments and the dental industry must take immediate action toward regulation and standards requiring the use of HVE devices as part of standard PPE and preventive safety measure with powered instrumentation:
- Mandatory use of HVE devices during ultrasonic, laser, and air polishing procedures should be universally enforced.
- Measurements for air quality and safe suction levels must also be defined, benchmarked, and standardized.
- Clinicians also need to know if the power and airflow volume of the HV evacuation system are performing to adequate safety levels chairside at the user end. In the same way that water lines and sterilization units are monitored at the user end, evacuation airflow measurements should be too.
- Dental office equipment should also be tested and certified to ensure that it performs as required for reducing aerosols and splatter. An annual user-end vacuum airflow and static pressure certification program would ensure that these systems are performing effectively.
Today’s hygienists need to apply themselves to learn about and use new technology that can offer better HVE performance and improved ergonomic benefits. It is imperative that the importance of using HVEs be taught at the fundamental level in dental hygiene and dental schools, and it should be enforced in general dental practice. Dental schools, manufacturers, and regulation enforcement agencies need to take steps to provide programs and material to advance clinical skills and compliance with upcoming changes in dental care safety.
It is vitally important for clinicians to use ultrasonic, air polishing, and laser technologies. Positive steps have been taken to support the evolving health safety needs in dentistry, as a few US states and Canadian provinces have mandated the use of HVEs with powered instrumentation.2 Dental hygiene schools have also taken steps to advance the clinical skills of their students in health and safety practices. However, there is still a road ahead for changes in industry regulations and standards for the health and safety of dental health-care professionals and their patients. Programs for testing, monitoring, and maintaining performance of vacuum systems in dental offices and HVE devices at the user end are still needed. The time is now to take the necessary steps to do better at managing aerosols to prevent the spread of disease in dental offices and to provide a safe and healthy environment for us all. RDH
Editor's note: Looking for information related to the coronavirus pandemic? Please visit our COVID-19 channel for the most up-to-date information for dental health-care professionals.
References
1. Harrel SK. Contaminated dental aerosols. Dimensions of Dental Hygiene. 1(6);2003:16-20.
2. Licensing requirements. In: The Composite. 28th ed. Chicago, IL: American Association of Dental Boards; 2017: 68-69.
3. Harrel SK, Molinari J. Aerosols and splatter in dentistry: A brief overview of the literature and infection control implications. J Am Dent Assoc. 2004;135:429-437.
4. Jacks M. Protecting yourself. Dimensions of Dental Hygiene. 9(8):26-29.
5. Centers for Disease Control and Prevention. Guidelines for Infection Control in Dental Health-Care Settings - 2003. MMWR 2003;52(RR-17).
6. Sun LH. TB cases increase in U.S. for first time in 23 years. Washington Post website. https://www.washingtonpost.com/news/to-your-health/wp/2016/03/24/tb-cases-increase-in-u-s-for-first-time-in-23-years/?utm_term=.6cd0839aabec. Published March 24, 2016.
7. Holloman JL, Mauriello SM, Pimenta L, Arnold RR. Comparison of suction device with saliva ejector for aerosol and splatter reduction during ultrasonic scaling. J Am Dent Assoc. 2015;146(1):27-33.
Laura Emmons, RDH, is a graduate of the Lake Washington Institute of Technology dental hygiene program who works as both a traditional and restorative hygienist in the Seattle area. Laura has conducted many continuing education workshops on the ergonomic use of HVE with ultrasonic therapy for dental schools, as well as for many private dental workshop events. You can contact Laura at (206) 380-3302 or visit her on Facebook.
Cheri Wu, BDSc, RDH, earned her degree in dental hygiene from the University of British Columbia. She has dedicated 25 years to clinical practice and education, including 10 years in nonprofit dental care. She has an independent dental hygiene clinic, Focus on Dental Hygiene, in Victoria, BC, and she holds a faculty position with Camosun College. With Dentsply Canada, she gives evidence-based presentations about ultrasonic instrumentation and air polishing. Other accomplishments include the 2012 Camosun College Distinguished Alumni Award and the 2014 Barbara Heisterman Award for Innovation and Commitment to Care. Contact her at [email protected].
Tia Shutter is a freelance copywriter and technical writer based in Seattle. She has recently launched a business to provide technical writing and marketing support to clients focusing on new technologies and public welfare. Reach Tia at [email protected] or visit her www.linkedin.com/in/tia-shutter-57355a3">LinkedIn profile.