No more bloody prophys: CDT code provide a guide for gingivitis, periodontitis, peri-implantitis
By Karen Davis, RDH, BSDH
Each year there are a few new coding opportunities that dental professionals should fully understand. Current Dental Terminology (CDT) 2017 is a resource owned and provided by the American Dental Association (ADA) to assist dental professionals with appropriate documentation.
This column is devoted to one goal: assist with easy implementation of the new code for gingivitis treatment and peri-implant inflammation so that patients can benefit from the treatment and receive appropriate insurance reimbursement. While not all inflammatory conditions in the oral cavity are plaque-induced, this decision guide reflects gingivitis, periodontitis, and peri-implant inflammation that are plaque-induced.
In essence, before a cleaning procedure is performed, clinicians must first determine whether or not inflammatory disease is present. If so, they must determine how involved it is, whether it involves implants, and what risk factors contribute to the diseased condition. An oral evaluation and recorded diagnosis should guide treatment decisions each visit. Gone are the days when bloody prophys were provided as a norm, or at least, they should be!
Let's begin with the ADA's description of these two new codes:
- "D4346 scaling in the presence of generalized moderate or severe gingival inflammation- full mouth, after oral evaluation. The removal of plaque, calculus, and stains from supra- and sub-gingival tooth surfaces where there is generalized moderate or severe gingival inflammation in the absence of periodontitis. It is indicated for patients who have swollen, inflamed gingiva, generalized suprabony pockets, and moderate to severe bleeding on probing. Should not be reported in conjunction with prophylaxis, scaling and root planing, or debridement procedures." (For ease of discussion in this article, I will refer to this procedure as "gingivitis therapy.")
- "D6081 scaling and debridement in the presence of inflammation or mucositis of a single implant, including cleaning of the implant surfaces, without flap entry or closure. This procedure is not performed in conjunction with D1110 or D4910." (For ease of discussion in this article, I will refer to this procedure as "peri-implant therapy.")
Wording of the gingivitis therapy code specifies that a diagnosis must be made prior to providing treatment. Applying that principle to treatment of all inflammatory conditions of the oral cavity will cover a multitude of sins, so to speak, in terms of continuity among clinicians, providing standard-of-care treatment, and clarity of treatment goals. The "Guide to Reporting D4346" is posted in the publications section of the ADA's website.
Wording of the peri-implant therapy code specifies therapeutic treatment per implant and can be used in conjunction with gingivitis therapy and localized or generalized periodontal therapy, but not in conjunction with prophylaxis or periodontal maintenance.
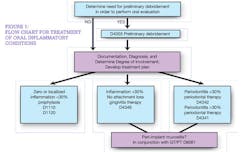
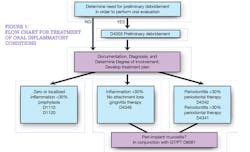
The following five "D" acronyms serve as a simple reference point to highlight key components for clinicians treating inflammatory conditions. The "Flow Chart for Oral Inflammatory Conditions" incorporates these acronyms, revealing a decision guide for preventive care, treatment of gingivitis, treatment of periodontitis, and treatment of peri-implant inflammation.
- 1. Determine whether or a not preliminary debridement is necessary due to excessive hard and soft accumulations that interfere with a complete oral evaluation. If so, that would be performed initially, with documentation, diagnosis, and therapeutic treatment to follow.
- Documentation that paints a clear picture of the clinical presentation and subsequent risk factors must be recorded. This includes but is not limited to systemic/medical risk assessments, full periodontal charting, assessment of tissue response, necessary radiographs revealing crestal bone support, photographs and salivary diagnostics to analyze pathogens, and/or genetic risk.
- Degree of involvement must be determined since code descriptions for treatment of gingivitis and periodontitis reflect the American Academy of Periodontology's definitions for localized (<30%) or generalized (>30%) disease that correspond to specific treatments. For example, a patient with 28 teeth would exhibit 50 or more sites bleeding for consideration of "full mouth" treatment corresponding to 30% involvement.
- Diagnosis of inflammatory conditions in this context correspond to gingivitis when no attachment loss is present and bone height equals 1.5 mm to 2 mm from CEJ to alveolar crest, or periodontitis when attachment loss is present. For inflammation and bleeding around an implant in the absence of bone loss, a diagnosis of peri-implant mucositis is made.
- Develop a treatment plan inclusive of gingivitis therapy or periodontal therapy, and peri-implant therapy, as indicated. There should be an emphasis on reducing risk factors and inflammatory conditions that include but are not limited to nutritional counseling, tobacco cessation counseling, oral hygiene instruction, motivational interviewing, and personalized counseling.
It is important to remember that code D4346 gingivitis therapy is not age-based and can be performed on children or adults. Following therapeutic treatment and resolution of gingivitis, appropriate ongoing care should be prophylaxis. D6081 peri-implant therapy can be performed in conjunction with D4346, D4342 localized periodontal therapy, or D4341 generalized periodontal therapy. Appropriate ongoing care would either be prophylaxis following gingivitis therapy, or periodontal maintenance following periodontal therapy.
Bottom line-to successfully implement these new codes, remember that treatment decisions are driven by diagnosis. This sounds simple enough, but what looks like per appointment will likely require a few paradigm shifts in traditional protocols and sequencing.
Appropriate use of these new codes should help clinicians fill the gap to provide treatment that corresponds with accurate diagnosis. Questions about these new codes are answered by Patti DiGangi, RDH, in DentalCodeology: A Gingivitis Code Finally! at dentalcodeology.com, by Charles Blair, DDS, in Coding With Confidence 2017 at practicebooster.com, or by the ADA CDT 2017 Companion at ada.org. I would encourage readers to access information from these experts to fully learn what you need to know. RDH
Karen Davis, RDH, BSDH, is the founder of Cutting Edge Concepts, an international continuing education company, and practices dental hygiene in Dallas, Texas. She is an independent consultant to the Philips Corp., Periosciences, and Hu-Friedy/EMS. She can be reached at [email protected].