From posture to oral pathology: The interconnected challenges of geriatric oral care
The quality of oral care provided to the older population is being silently compromised by an unexpected culprit: poor ergonomics in dental practices. This often-overlooked factor hinders our ability to accurately diagnose and effectively treat a wide range of oral pathologies beyond the well-known periodontal disease and root caries.
Aging, chronic diseases, and medications create unique oral health challenges for older adults. While common issues like periodontal disease and root caries are readily recognized, a hidden crisis looms as numerous other pathologies are frequently missed or underestimated due to ergonomic barriers that impede thorough exams and accurate diagnoses.1,2
By addressing ergonomic issues in dental settings and empowering practitioners with the tools and knowledge to provide optimal care, we can unlock a new era of comprehensive oral health for the aging population. This will enhance their quality of life and reaffirm our commitment to delivering the highest standard of care to this vulnerable group.
The link between poor ergonomics and undetected oral pathologies
With age, physiological changes occur that make individuals more prone to a variety of oral health issues. Frequently overlooked conditions include:3
- Oral candidiasis: While common in older adults due to weakened immunity, dry mouth, and denture use, this can be challenging to detect in its early stages without proper lighting and positioning. Poor ergonomics can impede a thorough examination, potentially delaying diagnosis and treatment.
- Burning mouth syndrome: This condition causes a burning sensation without visible signs. Proper patient positioning and a comfortable working posture for the practitioner are essential for conducting a thorough exam to rule out other potential causes.
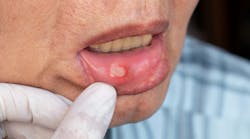
- Oral mucosal lesions: Conditions such as leukoplakia, erythroplakia, and lichen planus are more common in older adults. Accurate diagnosis relies on clear visualization and meticulous examination, which can be compromised by poor ergonomics that lead to fatigue and discomfort for the practitioner and patient.4
- Medication-related osteonecrosis of the jaw (MRONJ): This rare but severe condition requires early detection and intervention. Poor ergonomics can hinder the thorough examination of subtle signs of exposed jawbone or delayed healing.
Why are these crucial oral health conditions frequently overlooked?
Several factors play a role in this oversight. Ageism—the misconception that declining oral health is an inevitable part of aging—often leads to a dismissive attitude toward complaints or subtle signs of disease. Instead of investigating further, practitioners may attribute symptoms to "normal aging," which results in underdiagnosis and undertreatment.5
While cosmetic concerns are valid, some dental professionals may prioritize these over addressing underlying pathologies. This leads to neglecting severe conditions that may not be immediately visible but have significant implications on overall health. Limited time due to scheduling pressures can also hinder thorough exams, leading to missed diagnoses, especially for conditions that require careful observation or detailed questioning. Also, communication barriers between older adults and practitioners can lead to miscommunication or missed opportunities for diagnosis, especially if there’s a lack of rapport and clear communication.
Lastly, ergonomic challenges in dental settings present a significant barrier to effective geriatric oral care. Patient difficulties with positioning due to arthritis or stiffness, limited mobility, and sensory impairments can hinder thorough exams and treatment.
What can be done?
Addressing this multifaceted issue requires a comprehensive approach:
- Education and awareness: Enhanced training in geriatric oral health for dental professionals is crucial.
- Patient-centered care: Tailored treatment plans, clear communication, and addressing individual needs are paramount.6
- Collaboration: Collaboration among dentists, hygienists, physicians, and caregivers ensures holistic care.
- Research: Continued research into geriatric oral health needs and effective interventions is necessary.
- Ergonomic improvements: It’s essential to invest in adjustable equipment, use comfort aids, and provide ongoing training on ergonomic principles.7
We can significantly enhance geriatric oral care by acknowledging the impact of ageism, time constraints, communication barriers, and crucially, ergonomic limitations and implementing comprehensive solutions. Investing in education, fostering collaboration, and prioritizing ergonomic improvements will improve the quality of life for older adults and elevate the standard of care provided by dental professionals, ensuring a healthier and happier future for this vulnerable population.
References
1. Chan AKY, Tsang YC, Jiang CM, Leung KCM, Lo ECM, Chu CH. Diet, nutrition, and oral health in older adults: a review of the literature. Dent J. 2023;11(9);222. doi:10.3390/dj11090222
2. Ohlendorf D, Maltry L, Hänel J, et al. SOPEZ: study for the optimization of ergonomics in the dental practice–musculoskeletal disorders in dentists and dental assistants: a study protocol. J Occupa Med Toxicol. 2020;15:22. doi:10.1186/s12995-020-00273-0
3. Chen X, Kistler CE. Oral health care for older adults with serious illness: when and how? J Amer Geriatr Soc. 2015;63(2):375-378. doi:10.1111/jgs.13240
4.Pope-Ford R, Pope-Ozimba J. Musculoskeletal disorders and emergent themes of psychosocial factors and their impact on health in dentistry. Work. 2020;65(3):563-571. doi:10.3233/WOR-203110
5. MacDonald DE. Principles of geriatric dentistry and their application to the older adult with a physical disability. Clinics Geriatr Med. 2006;22(2):413-x. doi:10.1016/j.cger.2005.12.009
6. Nitschke I, Nitschke S, Haffner C, Sobotta BAJ, Jockusch, J. On the necessity of a geriatric oral health care transition model: toward an inclusive and resource-oriented transition process. Int J Environ Res Publ Health. 2022;19(10):6148. doi:10.3390/ijerph19106148
7. Crawford L, Gutierrez G, Harber P. Work environment and occupational health of dental hygienists: a qualitative assessment. J Occupa Environ Med. 2005;47(6):623-632. doi:10.1097/01.jom.0000165744.47044.2b
About the Author

Andreina Sucre, MSc, RDH
Andreina Sucre, MSc, RDH, is an international dentist, oral pathology, and oral surgery specialist practicing dental hygiene in Miami, Florida. A passionate advocate for early pathological diagnosis, she empowers colleagues through lectures focused on oral pathologies. Andreina is the founder of The Patho RDH, a published author for RDH magazine, and a selected speaker at RDH Under One Roof 2026. Committed to community outreach, she educates non-native English-speaking children on oral health and actively volunteers in dental initiatives.