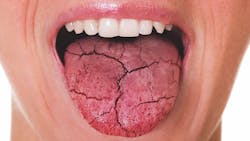
Dry mouth is everywhere, so why aren’t we talking about it? Saliva, systemic health, and dentistry’s next frontier
Key Highlights
- Reduced salivary flow is widespread, often overlooked, and frequently an early warning sign of broader oral-systemic dysfunction—not just an oral inconvenience.
- Saliva functions as a complex regulatory and diagnostic medium, reflecting inflammation, microbial balance, immune activity, and systemic health changes long before structural damage appears.
- Emerging salivary and oral microbiome testing tools are shifting dentistry beyond teeth alone, enabling earlier risk detection, better patient engagement, and more personalized preventive care.
Several years ago, someone close to me began experiencing severe pain on the tip of their tongue. It wasn’t subtle. It disrupted sleep, made swallowing difficult, and interfered with speaking. At the same time, other systemic symptoms appeared, such as fatigue and inflammation, vague discomforts that didn’t seem connected at first.
At the time, I didn’t yet have the language for what I now understand clearly: dentistry is entering an era where teeth alone no longer tell the full story.
They didn’t know what was happening or where to turn. I did.
I immediately recognized the signs of reduced salivary flow—not just as an oral issue, but as a breakdown in one of the body’s most important regulatory systems. As we know, long before we see structural damage to enamel or bone, we often see dysfunction in fluids, function, and inflammation. Saliva is frequently where those early signals appear.
What I didn’t realize then was that this moment would collide with another realization I was having myself. Shortly before this, I had begun noticing persistent dry mouth after starting clear aligner therapy. Then I picked up on something else: a noticeable decrease in salivary flow shortly after my daily coffee. Nothing dramatic—but consistent. Once I noticed it in myself, I started noticing it everywhere.
Patients. Colleagues. Friends. I noticed people complaining in small ways. Visible signs. Audible swallowing issues. Even subtle odor changes that signal reduced oral clearance. Decreased salivary flow wasn’t rare—it was everywhere.
And that raised a bigger question: if this is so common, why aren’t we talking about it more seriously in professional dentistry? And perhaps more importantly, how is this impacting the rest of the body?
What happens systemically when saliva begins to fail?
Saliva is not simply fluid. As licensed oral health-care professionals, we know it is a complex regulatory system responsible for buffering acids, modulating inflammation, controlling microbial populations, supporting remineralization, protecting soft tissue, aiding digestion, and serving as a first-line immune defense.
We know when salivary quantity or quality declines, the oral environment shifts rapidly, pH drops, microbial balance changes, tissue resilience weakens. But what we are only beginning to fully appreciate is how closely saliva reflects what is happening systemically.
The types of microorganisms and components of saliva are almost unbelievable—microorganisms, enzymes, cytokines, hormones, metabolites, and biomarkers that mirror physiological processes throughout the body. This is why prescription and recreational drugs can be detected in saliva for defined windows after use, and why salivary diagnostics are increasingly being explored in oncology, endocrinology, and infectious disease research.
Reduced salivary flow is not just an oral inconvenience. It is often an early signal of broader dysfunction.
Why did this lead me to the oral microbiome and saliva obsession?
Watching someone I love struggle with oral pain and declining quality of life pushed me beyond symptom management. I wanted to understand why this was happening, how quickly saliva dysfunction could alter the oral environment, and what tools existed to measure it objectively.
That curiosity turned into full immersion as I began exploring salivary and oral microbiome testing extensively and often on myself. I collected reports, measurements, biomarker data, inflammatory indicators, and microbial profiles. Over time, I accumulated a deep, longitudinal view of my own oral environment.
And then I encountered another problem we rarely address in diagnostics: we are generating enormous amounts of data, but we lack clarity on how to use it meaningfully. This is not unique to dentistry. Blood testing, wearables, genomics—we have information everywhere. The challenge is interpretation, integration, and action. Salivary testing sits directly in this tension point.
Is xerostomia becoming dentistry’s silent pandemic?
Research suggests that up to 30% of adults experience clinically significant dry mouth, with much higher prevalence among individuals taking multiple medications, undergoing cancer therapy, or managing autoimmune or metabolic conditions.¹ In my clinical and personal communities, I believe this number to be much higher.
We’ve known xerostomia to be associated with increased caries risk, periodontal breakdown, fungal infections, altered taste, difficulty speaking and swallowing, sleep disruption, and reduced quality of life.² More recently, we now understand salivary dysfunction has been linked to oral-systemic inflammatory pathways connected to cardiovascular disease, diabetes, and other chronic conditions.³
Yet patients often assume dryness is normal. Providers may view it as secondary. But it isn’t.
Dry mouth is a silent, progressive issue, and one we are underprepared to address comprehensively. However, recently, with the launch of
xerostomia-relief protocols, certifications, and lipid-based technologies, xerostomia is becoming an increasingly hot topic with patients in the clinical op.
How should we be thinking about oral testing today?
To make sense of the rapidly expanding oral testing landscape, I categorize tools into three functional questions.
- Is something happening right now? These are “assessment” salivary tools that assess real-time biological activity. Chairside salivary assessments that measure inflammatory biomarkers can help identify active tissue breakdown or inflammatory processes without diagnosing disease. In oncology, similar real-time salivary assessments are being explored to flag abnormal biomarker activity that warrants further investigation, supporting earlier referral and monitoring.⁴
- What is happening? These are “diagnostic” salivary aids, often lab-based, that help identify root causes when clinical signs persist or treatment fails. In cancer-related oral testing, this category includes lab assays that analyze specific salivary biomarkers associated with malignancy, viral load, or dysplastic changes, helping clinicians understand the underlying pathology.
- Could something happen in the future? “Risk” profiling using saliva samples evaluates susceptibility rather than active disease. Salivary-based cancer risk tests, genetic susceptibility panels, or microbiome risk profiles fall into this category. They do not diagnose disease, but they inform surveillance strategies and preventive planning.
What new salivary tools are changing clinical conversations?
Some of the newest tools entering the US market focus on measuring biomarkers released during inflammatory processes in oral tissues. These assessments are designed to answer simple but powerful questions: is tissue stable, or is it actively breaking down? And how rapidly?
Salivary tool workflows are becoming simpler, can take place chairside, and are commonly designed to produce a score rather than a diagnosis. The best part? These work best when integrated with other clinical findings, tools, and oral health data.
When used appropriately, they support earlier conversations, pattern tracking, patient education, and greater patient ownership of oral health, without overstepping diagnostic boundaries.
Why does 2026 represent a turning point for dentistry?
We are already seeing meaningful shifts. There are now professional certifications focused on xerostomia relief and therapy. Hands-on workshops and global symposiums dedicated to saliva, oral moisture, and function are becoming more common. Structured dry-mouth protocols exist that practices can adopt to create consistent, team-based care pathways. Most importantly, the conversation is moving beyond teeth alone.
The future of dentistry is not just about enamel and bone. It is about fluids, function, microbiomes, inflammation, early diagnostics, and prevention. Saliva may be the most powerful diagnostic and therapeutic tool we have been overlooking all along.
Dry mouth is not rare, it is not minor, and it is not isolated. When saliva fails, the dominoes begin to fall.
Stay tuned throughout the year as this saliva series will continue in an attempt for me to pass on everything I’ve learned during my extensive research over the last couple of years. We’ll explore methods, types, differentiators, and emerging salivary technologies. We’ll also examine how oral microbiome monitoring supports patient education engagement and behavior change, and how regular salivary monitoring enables truly personalized preventive care.
Editor's note: This article appeared in the March 2026 print edition of RDH magazine. Dental hygienists in North America are eligible for a complimentary print subscription. Sign up here.
References
- Villa A, Wolff A, Narayana N, et al. World Workshop on Oral Medicine VI: a systematic review of medication-induced salivary gland dysfunction. Oral Dis. 2016;22(5):365-382. doi:10.1111/odi.12402
- Dawes C, Pedersen AML, Villal A, et al. The functions of human saliva: a review sponsored by the World Workshop on Oral Medicine VI. Arch Oral Biol. 2015;60(6):863-874. doi:10.1016/j.archoralbio.2015.03.004
- Humphrey LL, Fu R, Buckley DI, Freeman M, Helfand M. Periodontal disease and coronary heart disease incidence: a systematic review and meta-analysis. J Gen Intern Med. 2008;23(12):2079-2086. doi:10.1007/s11606-008-0787-6
- Wong DT. Salivary diagnostics powered by nanotechnologies, proteomics and genomics. J Am Dent Assoc. 2006;137(3):313-321. doi:10.14219/jada.archive.2006.0180
About the Author

Melissa Turner, BASDH, RDHEP, EFDA
Melissa K. Turner, BASDH, RDHEP, EFDA, was honored as a 2024 Marquis Who's Who in America recipient. She is Senior Executive Consultant at Cellerant Consulting Group and spearheads the Cellerant Best of Class Hygiene Awards. She is a founding board member of the American Mobile & Teledentistry Alliance, cochair of the Oral Health Prevention Summit, and serves on the executive board of the Dental AI Association. Known as @thetoothgirl, she is the cofounder of The Denobi Awards and the National Mobile & Teledentistry Conference.