Silver diamine fluoride (SDF): Dental caries in older adult patients
Providing oral care for older adults with physical and medical impairments creates challenges for dental and other health-care practitioners. Older adults often have limited finances, restrictions in mobility, complex medical sequelae, and age-related cognitive issues that make dental treatment challenging.1 Currently, the adult population ages 65 and older accounts for over 13% of the United States population. Within this population, an estimated 96% of people have a history of dental caries, and 18.5% have untreated dental caries.2 This means that one in five adults aged 65 and older has untreated tooth decay, and two in three have periodontal disease.2 Furthermore, the Centers for Disease Control and Prevention predicts that by 2060, the number of US adults in this age group is expected to reach 98 million, or roughly 24% of the population, creating an oral health crisis among community-dwelling elders and medically frail patients.3
As we analyze this need, how do we as oral health-care providers address this disparity? The American Dental Association (ADA) recommends application of fluoride solutions to prevent and/or arrest dental caries, which provides a balance between protective and pathogenic factors.4 The application of fluoride changes the composition of plaque by altering its metabolism and decreasing the ability of the biofilm to transform dietary sugars and carbohydrates into acid.4 Dental practitioners have utilized sodium fluoride varnishes, chlorhexidine varnishes, prescription-strength fluoride toothpaste, and mouth rinses to help patients prevent and arrest decay. Recently, however, silver diamine fluoride (SDF), a relatively new formulation of topical fluoride using silver compounds, has gained global recognition as a noninvasive, nonrestorative treatment to arrest or prevent caries.4,5
What is SDF?
SDF is a dual-action solution that contains silver (25%) and fluoride (5%) stabilized by ammonia (8%). In 2014, the Food and Drug Administration (FDA) approved SDF as a class II medical device for use in dentistry to treat sensitivity, with an off-label use for arresting and preventing caries. In 2016, the FDA granted SDF its breakthrough therapy designation for the arrest of dental caries.6
A 38% solution of SDF contains 44,800 ppm fluoride, which is the highest fluoride solution available among dental medicaments.7 It is sold in the US by Elevate Oral Care under the brand name Advantage Arrest as a 38% SDF solution. In 2018, a second formulation of SDF became available in the US under the brand name Riva Star from SDI Inc. This product has a secondary application of potassium iodide, which minimizes the risk of staining. Riva Star can be purchased through your dental supply company, and Advantage Arrest is available directly from the manufacturer.
What makes SDF a better choice?
SDF boasts a dual action of the antimicrobial properties of silver and the remineralization properties of fluoride. Silver has been utilized in dentistry and medicine since the 1800s because of its outstanding anticaries, antimicrobial, and antirheumatic properties.8 SDF enters the dentinal tubules and forms a precipitate, which reduces hypersensitivity.9 The silver has been shown to be lethal to Streptococcus mutans and Actinomyces naeslundii, two of the bacteria responsible for the progression of caries.10 SDF reacts with saliva from the oral environment, forming fluorohydroxyapatite, which promotes the remineralization of teeth. It provides an insoluble layer or increased hardness that protects the enamel from the damaging effects of fermentable carbohydrates, dietary challenges, and other environmental factors. When caries is present in dentin, SDF prevents the diffusion of calcium and phosphate from the collagen matrix.11
Sodium fluoride and chlorhexidine varnishes require quarterly or biannual application for maximum efficacy, whereas SDF is effective with annual applications. Combined with oral hygiene educational programs, SDF’s effectiveness increases.5
How can SDF benefit older adults?
Older adults face multifactorial challenges, which put them at a higher risk for untreated dental caries and other oral manifestations. Changes in salivary flow due to age and medications, poor diet, and exposure of root surfaces in areas of recession place older adults at a greater risk for developing caries than younger patients. The incidence of root caries increases with an increase in medical conditions and age.1
SDF can provide a safe and effective treatment option for use in community-living facilities and medically compromised patients. Application is simple and requires no special equipment or infrastructure support. For patients in ambulatory or palliative care, SDF can prevent the progression of carious lesions without adding additional stresses that often occur when transporting these patients to a dental facility for treatment. Patients with advanced dementia or mental illnesses do not fully understand dental and medical procedures, making it difficult to treat them safely. In cases such as these, SDF can be an alternative treatment option.
Dental and medical providers should understand that even though SDF can be used to successfully arrest a carious lesion, it is not a final restoration. Composite resin or glass ionomer materials may be placed on a lesion to fill the cavitation, with glass ionomer as the material of choice for root surface lesions in older adults.
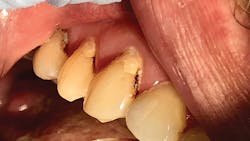
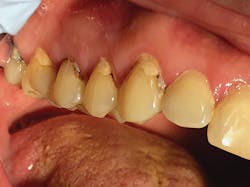
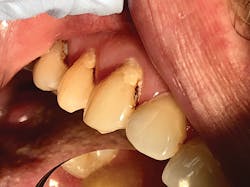
Adverse effects of SDF are rare and mostly limited to the dark brown or black staining that occurs when SDF contacts a carious lesion. SDF will not stain healthy tooth structures. Contraindications include patients with allergies to heavy metals (specifically silver or fluoride allergies), ulcerative gingivitis, or stomatitis; those undergoing thyroid gland therapy; and on teeth that show signs and symptoms of irreversible pulpitis.
Application protocol
To place SDF, make sure the surface is clear of debris and plaque, isolate with cotton rolls, dry the area to be treated, and place SDF with a cotton-tipped applicator. Allow the SDF to dry before removing the cotton rolls. Patients describe the taste as bitter and metallic, so rinse after allowing the area to dry. SDF will become milky white where it encounters saliva. Staining of gingival areas may occur, but this will typically go away within 48 hours.
A dentist’s perspective of SDF success
As previously stated, SDF has a place in our office tool kit for patients who are mentally, medically, and/or physically challenged. It has demonstrated its ability to arrest and prevent caries in clinical trials, thus clearing the way for successful uses in clinical dentistry. When utilizing SDF, dental practitioners must understand that it is not a replacement for definitive treatment. If the determination is made that a patient cannot tolerate conventional dental treatment, SDF followed by a modified atraumatic restoration (ART) is an acceptable technique.
Placement of a restorative material following SDF application is optimal. For older adult patients with root surface caries, resin-modified glass ionomers (Fuji II by GC America or Geristore by DenMat) are ideal to fill the arrested cavitation. This will assist the patient and caregiver in keeping the area clean, because a smooth surface is much easier to keep clean than a dimpled one.
Once a restoration is placed, the patient/caregiver should continue to be diligent with applications of a prescription-strength fluoride (e.g., Prevident 5000 by Colgate), as well as timely hygiene appointments to prevent caries from reactivating and progressing rapidly. Carefully monitor the patient to determine whether the carious lesion is arrested or progressing, in which case alternative treatment would be in order.
How to code for reimbursement
In January 2018, the ADA updated the Current Dental Terminology (CDT) to cover placement of SDF. CDT code D1354—Interim caries arresting medicament application, per tooth—was added. If SDF is placed to aid with sensitivity, use CDT code D9910—application of desensitizing medicament. Currently, 37% of Medicaid plans offer reimbursement for SDF applications; however, many states do not offer adult Medicaid coverage, which leaves a larger number of older adults with a financial burden.
Even though most dental insurance companies do not currently reimburse for SDF applications, continual claims filing will help increase the likelihood of employers picking up these codes for coverage under their dental plans. The more a code is utilized, the more it is included in dental insurance plans.
The cost of SDF is much cheaper than a hospital or ambulatory visit, which could be required to provide care for a medically compromised patient. The average cost of SDF application for a single-tooth treatment ranges from $20–$25.
Successful use of SDF in clinical practice
We use SDF in our office as an alternate treatment option for medically challenged patients and older adults. As our heavily restored older patients become more restricted in their ability to perform daily hygiene routines, such as brushing teeth and flossing, we start to see more marginal and root surface caries. The cause of this can be twofold: lack of proper plaque removal and poor diet. When interviewing patients in this age group or their caregivers, we find patients tend to experience dry mouth and often find relief from sipping on sugary beverages or sucking on hard, sugary candies. In a dry mouth, these habits accelerate tooth decay. Compromised medical situations often prevent patients from undergoing dental treatment.
As dental providers, it is our responsibility to educate patients and their caregivers and provide treatment options. For a patient who is in the last stages of dementia, it is neither ethically nor morally appropriate to put them through extensive restorative procedures or extractions. In our office, we place SDF at the initial diagnosis of decay after removing food debris and plaque, and then we reapply it at subsequent appointments. If the caregiver requests, we can follow up with treatment at the assisted living facility. SDF shows success with annual applications, but in our practice, we have seen greater benefits if SDF is reapplied at six-month intervals during the first two years. We attribute this to the difference in home-care plaque removal, habits, and diet, which are often uncontrolled in real-life situations, as compared to clinical trials.
Conclusion
SDF is a cost-effective medicament for arresting and preventing caries in older adults, in addition to those who are in ambulatory care, dementia patients, and the mentally and physically challenged. As dental practitioners, it is our responsibility to be aware of and use alternative technologies to assist our patients in all stages of life to achieve optimal oral health.
Authors’ disclosure: While several products are named in this article, neither of us receives any royalties or funding from these companies. Mentioning these products is not an endorsement.
References
1. Griffin SO, Jones JA, Brunson D, Griffin PM, Bailey WD. Burden of oral disease among older adults and implications for public health priorities. Am J Public Health. 2012;102(3):411-418. doi:10.2105/AJPH.2011.300362
2. Dye B, Thornton-Evans G, Li X, Iafolla T. Dental caries and tooth loss in adults in the United States, 2011–2012. NCHS Data Brief, no 197. Hyattsville, MD: National Center for Health Statistics; 2015. https://www.cdc.gov/nchs/data/databriefs/db197.pdf
3. Oral health for older Americans: facts about older adult oral health. Centers for Disease Control and Prevention. Updated May 22, 2019. https://www.cdc.gov/oralhealth/basics/adult-oral-health/adult_older.htm
4. Slayton RL, Urquhart O, Araujo MWB, et al. Evidence-based clinical practice guidelines on nonrestorative treatments for carious lesions: a report from the American Dental Association. J Am Dent Assoc. 2018;149(10):837-849.e19.
5. Horst JA, Ellenikiotis H, Milgrom PL. UCSF protocol for caries arrest using silver diamine fluoride: rationale, indications, and consent. J Calif Dent Assoc. 2016;44(1):16-28.
6. Breakthrough therapy designation for the arrest of early childhood caries. Elevate Oral Care. The Silver Bulletin. 2017;1. http://www.elevateoralcare.com/Landing-Pages/silverbulletinv1
7. Tracy S, Weyant RJ, Anselmo TT, et al. Topical fluoride for caries prevention: executive summary of the updated clinical recommendations and supporting systematic review. J Am Dent Assoc. 2013;144(11):1279-1291. doi:10.14219/jada.archive.2013.0057
8. Lansdown ABG. Silver in health care: antimicrobial effects and safety in use. Curr Probl Dermatol. 2006;33:17-34. doi:10.1159/000093928
9. Sarvas E. The history and use of silver diamine fluoride in dentistry: a review. J Calif Dent Assoc. 2018;46(1):19-22.
10. Rosenblatt A, Stamford TCM, Niederman R. Silver diamine fluoride: a caries “silver-fluoride bullet.” J Dent Res. 2009;88(2):116-125. doi:10.1177/0022034508329406
11. Zhao LS, Gao SS, Hiraishi N, et al. Mechanisms of silver diamine fluoride on arresting caries: a literature review. Int Dent J. 2018;68(2):67-76. doi:10.1111/idj.12320
About the Author

Joseph R. Hendrick Jr., DDS
JOSEPH R. HENDRICK JR., DDS, is a licensed dentist with more than 35 years of experience in providing clinical dental care. He is active in organized dentistry in North Carolina as a past president of his local dental society, and as a current board of trustee member of the North Carolina Dental Society. He enjoys sharing his knowledge of dentistry with new dentists and hygienists and serving as a mentor to new graduates. He may be reached at [email protected] or josephrhendrickjr.com.

Lori Gordon Hendrick, PhDc, MS, RDH, CDA, CDT
Lori Hendrick, PhDc, MS, RDH, CDA, CDT, is working toward a PhD in public administration and policy with a concentration in health policy at Old Dominion University. In addition to practicing dental hygiene, she owns Athena Dental Solutions and teaches clinical hygiene and professional development at Central Piedmont Community College. She’s a past president of the North Carolina Dental Hygiene Association, a consultant on the North Carolina Dental Society Work Force Task Force, and on the board of directors for North Carolina Caring Dental Professionals. Email Lori at [email protected].
Updated February 4, 2022