Mini Dental Implants:
Life-Changing Options For Denture Patients
By AGNES DEZAK, RDH
Almost any hygienist who works with denture patients has stories about treating people who are unhappy and uncomfortable with their dentures or partials. While these devices are an improvement over the total or partial edentulism that patients would face without them, many patients still experience discomfort or self-consciousness, and many are sad that the prosthetics cannot perform like their natural teeth did.
It is not just a few isolated denture patients that feel this discomfort and sadness. Research shows that it is very common for edentulous patients to have negative feelings about their condition. One study of 50 edentulous people found that their responses to tooth loss included “bereavement, lowered self-confidence, altered self-image, dislike of appearance, an inability to discuss this taboo subject, a concern about prosthodontic privacy, behaving in a way that keeps the tooth loss secret, altered behavior in socializing and forming close relationships, premature aging, and lack of preparation.”
This is quite a list of issues, but experienced hygienists likely understand its truth. The researchers conclude, “Tooth loss can be disabling and handicapping.” To offer an additional, perhaps more poignant perspective, another study examined the experiences of getting dentures and losing teeth as compared to other life experiences. Research subjects in this study ranked getting dentures as a more significant life adjustment than retiring from work, getting married, or having a child.
Findings such as these underscore why it’s important for every member of the dental team to provide support and guidance for denture patients, and to help educate them on the options available for improving their comfort and confidence. In some cases, patients may be helped with simple measures such as denture relines. But the dental community also has more powerful options for patients who seek added stability and retention for their dentures.
Options For Dental Implants
Dental implants for denture stabilization have become increasingly popular in recent years. Data shows that placing two implants in the anterior mandible can make a major difference in the quality of life for patients, and can help maintain bone in the jaw that would otherwise resorb following teeth loss. In 2002, McGill University issued a consensus statement on overdentures, which stated in part, “Mandibular two-implant overdentures have been shown to be superior to conventional dentures in randomized and nonrandomized clinical trials that ranged in duration from six months to nine years.”
The only problem is that for many patients, traditional dental implants are not a viable option. This is due to a number of factors. First, patients must have adequate bone levels to anchor the implants. While bone levels are often not a problem for patients who have only recently become edentulous, long-time denture wearers often have ridges that have resorbed too much for implant placement. This resorption can be treated with bone grafting, but this treatment adds a layer of expense and medical complexity.
The expense of traditional implants, whether or not bone grafting is required, is also a major hurdle for many senior-aged patients. Many of these patients are on fixed incomes and have a hard time accommodating an expense that is many thousands of dollars. Finally, the invasiveness and time involved in the placement of traditional implants can dissuade many patients from pursuing this treatment. The placement procedure can be very traumatic for patients and may require significant healing time. Because the procedure is so invasive, people who are not in optimal health may not qualify for it even if they want to proceed with it. The procedure requires coordination from multiple health-care professionals to ensure that new medications are compatible with existing prescriptions, and that patients are healthy enough to undergo surgery.
Therefore, while many in the dental industry acknowledge that implant-retained dentures can serve patients better and alleviate many of the common problems patients have with dentures and partials, the treatment may not always be feasible. The expense and time commitment can be disheartening for patients who want a solution for their ill-fitting dentures.
Attractive Alternatives To Traditional Implants
The good news is that traditional implants are no longer the only option for these patients. Over the past five to 10 years, mini dental implants have emerged as an attractive alternative to traditional implants. These implants range in size from 1.8 mm to approximately 3 mm versus the traditional implant diameter of 3.75 mm. MDI Mini Dental Implants by 3M ESPE represent a good example of a mini implant system. These mini implants (originally known as the IMTEC Sendax MDI System) were the first on the market approved for the long-term use of denture stabilization.
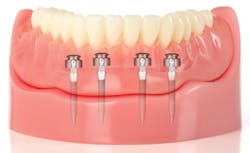
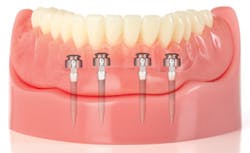
The placement procedure for mini implants is quite different from that of traditional implants. They can be placed and loaded in a one-day appointment with a general dentist who is certified in the procedure. In a typical denture stabilization procedure, four mini implants are placed in the lower mandible. With the assistance of diagnostic imaging tools, the dentist marks the proper locations for the implants on the patient’s ridge, and then uses a pilot drill to create a small hole in the tissue. The implants are then inserted into the pilot holes and tightened into place with a series of drivers and wrenches. This minimally invasive procedure is a stark contrast to the procedure for traditional implants, which involves cutting a flap in the tissue and requires significant healing time before loading.
Once the implants are placed, the patient’s denture is fitted with metal housings that allow it to snap onto the o-ball shaped heads of the mini implants. In some cases a new denture is fabricated for this procedure, but it is also possible to retrofit the patient’s existing denture if it is in good condition. After the denture is fitted with the housings, the patient is instructed on proper care and sent home. In just one day, it is possible for patients to experience a dramatic change in denture retention.
As might be inferred from this description of the procedure, mini dental implants are quite different from traditional implants, and can help address many of the hurdles that patients face when they consider implant treatment. Because a general dentist places them in a minimally invasive procedure, mini implants are significantly more affordable than standard-diameter implants. As mentioned, in some cases the patient’s existing denture can be used, which adds to the affordability.
While many edentulous patients do not have adequate bone levels for standard implants, the bone requirements for mini implants are significantly lower. Additionally, patients who are turned off by the time required for traditional implants are often very excited to hear that mini implants often can be placed and loaded in just one day.
The Hygienist’s Role In Implant Treatment
The dentist is typically the member of the practice responsible for sharing treatment plan information with prospective patients, but it is very helpful for hygienists to have an understanding of the placement procedure and the benefits of mini implants so they can share a brief overview with interested patients. Because hygienists often hear complaints from denture patients about discomfort, sore spots, and trouble eating, this can provide a natural opening to discussing implant treatment and directing the patient to ask the dentist more questions. While the dentist will explain the clinical details of the treatment, hygienists in practices that place mini implants should feel comfortable sharing their own perspective about how exciting and life changing the treatment can be.
While hygienists typically are not involved in the placement procedure, they are a very important part of the care team after mini implant placement. Proper care begins with brushing, which can be a challenge for edentulous patients out of the habit of brushing, who were likely not good brushers when they had natural teeth. Proper brushing can also be an issue simply due to someone’s age. For these reasons, use of an electric toothbrush is strongly encouraged. This can be a great help for patients with dexterity issues, and toothbrushes with built-in timers can help ensure that patients achieve an adequate duration of brushing. Patients should be instructed to brush throughout the mouth and pay particular attention to the implants, as plaque can build up on them just as it does on natural teeth, potentially compromising the long-term success of the implants.
Patients should return to the dental office for checkups every six months following implant placement. This helps the dental team ensure that the implants remain stable and that patients care for them properly. Many hygienists have likely faced challenges with motivating denture patients to take good care of their appliances, and this can continue to be an issue for some implant patients. However, many implant patients do regain motivation to take good care of their dental health once they experience the stability and confidence of mini implants. Being able to eat foods such as steak, corn on the cob, and apples gives patients a tangible motivator to maintain their implants.
Another reason that patients must return to the office regularly following implant placement is that the o-rings in the denture require periodic replacement. The o-rings wear out over time, and we recommend changing them once a year, or as needed according to the patient’s comfort level. Patients who experience slight mobility with their dentures often find that changing the o-rings brings them back to a level of stability they prefer.
Improving Quality Of Life
It is very difficult to see patients suffer from discomfort and insecurity caused by loose dentures. Patients not happy with their dentures lose confidence when socializing and eating, and can even have trouble with important rituals such as blowing out birthday candles. Problems like these take a toll on people, more so than they may disclose to their dental teams.
The good news is that hygienists, by virtue of their role as teachers and listeners, have a great opportunity to help educate patients about denture stabilization options. While some patients may have written off the possibility of dental implants due to their cost or other reasons, they may not be aware that mini dental implants give them another option for regaining confidence and function with their dentures. The emotional impact that denture stabilization has for these people makes it very rewarding to work in a practice that places mini implants. RDH
References
1. Fiske J, Davis DM, Frances C, Gelbier S. The emotional effects of tooth loss in edentulous people. Br Dent J. 1998 Jan 24;184(2):90-93.
Bergendal B. The relative importance of tooth loss and denture wearing in Swedish adults. Community Dent Health. 1989 Jun;6(2):103-111.
ADA Council on Scientific Affairs. Dental endosseous implants: an update. J Am Dent Assoc. 2004 Jan;135(1):92-97.
Christensen GJ. The ‘mini’ implant has arrived. J Am Dent Assoc. 2006 Mar;137(3):387-390.
AGNES DEZAK, RDH, currently provides dental hygiene and periodontal therapy at Concierge Dental Group where they focus on implant dentistry. She is a member of the American Dental Hygienists’ Association, the Dental Hygienists’ Association of the State of New York, the Buffalo Dental Hygienists’ Association, and the International Congress of Oral Implantologists. DeZak is also the owner of Western New York Dental Sharpening, servicing dental offices and clinics throughout Western New York.
Past RDH Issues