Untangling the insurance web
Turn the perceived limitation into a benefit for both clinician and patient
by Kimberly R. Miller, RDH, BSDH, RDHMP
Over the last 18 years as a consultant, I have pushed many dental professionals out of their comfort zone by asking them to adopt new behaviors or change existing ones. In my experience, the shortest route to behavior modification starts with thought. In other words, effective behavior change begins with what you think. Change the way you think about a situation, and you can change the way you behave when dealing with that situation.
In writing this article it occurred to me that, for the most part, dental professionals give dental insurance companies a bad reputation. We view dental insurance as an entity that discourages the patient from obtaining treatment due to policy limitations and restrictions.
In fact, the opposite is true.
Many patients would not receive any dental care if it were not for the dental insurance benefits they accrue. That being said, there are times in the dental workday when we pull our hair out over dental insurance issues and the time it takes to resolve them. Sometimes it is a patient’s misunderstanding over the amount of reimbursement provided by their insurance plan. At other times, the patient or even a team member may have a perceived limitation of available care when a procedure is not covered. We often hear, “If my insurance does not cover it, I’m not going to do it.”
Regardless of the obstacles dental insurance presents, it’s in our best interest to think about insurance as a benefit or an advantage for the patient. Our best interest (as well as the patient’s) also includes having a good understanding of the American Dental Association (ADA) procedure codes most commonly billed by dental hygienists. As hygienists, we must also understand the application of these treatment codes, which will assist us in choosing the correct codes for individual procedures in order to maximize the patient’s insurance benefits.
The most commonly billed code from the dental hygiene chair is 1110, or Adult Prophy. In fact, according to the JP Institute, most general dental practices bill an average of 80% to 90% 1110s annually. This statistic should give every clinician pause, since the research tells us that about 80% of our patients have some form of periodontal disease:
- In 2002, the Academy of General Dentistry estimates 74% of the U.S. population had periodontal disease.
- In 2005, the American Academy of Periodontology stated 90% of patients ages 55 to 64 had moderate to severe periodontal disease.
- In 2006, the American Dental Association estimated 80% of the U.S. population had mild to moderate periodontal disease.
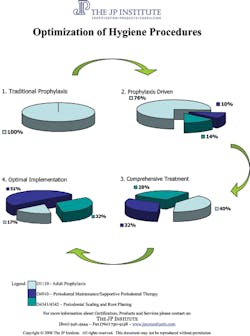
Since this is the case, you might be asking yourself some questions. Shouldn’t we be billing about 80% for therapeutic services? Are we undertreating our patients? Are we trying to correct disease in an appointment designed for prevention or maintenance? Let me suggest that you calculate your own percentages so that you know exactly what percentage of your patients are being treated under each treatment code. Independent of production awareness, you will be able to see how many of your patients are receiving preventive and maintenance procedures vs. therapeutic care. Once you have calculated your own percentages, compare them to the charts featured.
To calculate your percentages, list the number of adult patients in each treatment category (typically, pediatric procedures are not factored into this calculation). You can easily access this information by running a computer report. Look for the report that gives you “procedures by provider by treatment code.” The title of this report varies a bit from software to software.
Once the report is generated, view it before printing to be sure you have the correct data. Down the left side of the page, the ADA procedure codes will be listed; tracking across the page to the right you will see the numbers for that procedure provided for the date range you have selected. This report usually shows you production generated from the use of that code as well. Initially, you will want to run this report for the previous 12 months and then monthly after that to track your progress.
The formula is:
1110: ____________
4910: ____________
4341 / 4342 / 4355: + ____________
Total adult patients seen: ____________
# of 1110 ___ ÷ # of adult patients ___ x 100 = ___% 1110
# of 4910 ___ ÷ # of adult patients ___ x 100 = ___% 4910
# of 4341 ___ ÷ # of adult patients ___ x 100 = ___% 4341/2/4355
Compare your hygiene department percentages to the JP Institute pie charts. These pie charts have been created from the percentages reported to the JP Institute by clients over the last 30 years. Once you know your current percentages, you can begin an action plan to shift your percentages to the next pie chart. If you would like to take advantage of a complimentary practice profile to determine your growth potential, please call the JP Institute.
Dental insurance benefits
It goes without saying that every patient who has the blessing of dental insurance has a different policy with a unique set of rules. While there are some basic similarities, even policies issued from the same company can have varied benefits, limitations, and exceptions. Most often, employers purchase plans that are financially manageable for them. The employee must then choose one of those available options. Some companies now implement “health care spending” options, allowing the employee to pledge a certain amount of dollars per year. In many cases, this amount is matched by the employer and can be spent on any dental or medical needs without limitation or approval process. With this option, the employee typically is issued a “debit card” of sorts for easy payment at the time of service.
Traditional dental insurance, on the other hand, usually assists the patient with 100% of preventive services, as long as the dentist’s fee matches the specific fee schedule for that policy. When the fee charged by the dentist exceeds the “allowed” amount, the provider, assuming they are participating with that insurance company, must discount their fees to match the insurance company’s fee schedule. In other words, the dentist writes off those dollars.
Therapeutic services may fall under the “basic benefits” of the insurance policy and are usually assisted at 80% after the annual deductible has been met with the same set of rules when the “allowed” amount is exceeded. On the other hand, some insurance companies refer to any therapeutic services as a “major benefit” and usually assist 50% to 80% after the annual deductible has been met. It’s a small wonder most patients don’t have a full understanding of how their dental benefits actually work. Therefore, they rely on us to know the details. I have been in dental offices where there are upwards of 20 different types of dental benefit packages that the team must be familiar with.
An interesting new development
Some dental insurance companies have started imposing a little known and undisclosed six-week waiting period between the following treatment codes:
- 1110 and 4341/2
- 4355 and 4341/2
- 4910 and 4341/2
Basically, if you bill an adult prophy, a periodontal maintenance procedure, or a full mouth debridement, the insurance will not assist the patient with any benefit toward therapeutic procedures (4341/2) for six weeks. This “waiting period” is not typically disclosed; you must ask if it is in effect. With this being the case, I highly recommend that, when verifying insurance benefits for new or existing patients, you ask if there is a waiting period between the above codes. In addition, ask if there is a benefit for 0180 (periodontal evaluation). If so, inquire about frequency limitations when using 0180 and 0150.
When you run across a patient whose policy has these parameters, and you use the D1110 or the D4910 as a transitional appointment between recall and therapy (as many offices do), you may want to consider the option of using the billing code D0180 for the current recall appointment. Under the umbrella of the D0180 code, you can include a recall procedure as long as you follow the descriptor (see below).
There are no insurance rules that limit the dentist from providing services for the patient that they do not submit to the insurance company for reimbursement or benefit. So, once you have established that your recall patient has an active periodontal infection, you can provide the service the patient was scheduled for today, educate the patient, and collect the data included in the D0180, as well as avoid having the patient wait six weeks for periodontal treatment to begin.
To be clear, billing the insurance company for a procedure that you did not do is considered fraudulent. Providing a service for which you do not bill the insurance company, or the patient, is simply generosity.
Procedure code applications
As you read through these definitions, let me encourage you to think with me and identify the opportunities for care these descriptors offer, rather than how they may limit treatment.
- The ADA CDT (Current Dental Terminology) descriptor for D1110 prophylaxis reads: “Removal of plaque, calculus, and stains from the tooth structures in the permanent and transitional dentition. It is intended to control local irritational factors.”
The last phrase translates to: If the patient has a generalized condition, or bleeding in more than localized areas, additional procedures should be considered. For example, when our patients present with generalized moderate bleeding, with or without calculus, and we provide a “cleaning” and reappoint them for another recall, we are sending a patient with an active periodontal infection out the door. This happens routinely even though the current standard of care does not support this protocol. This is just one of the reasons the percentage of D1110 is commonly so high.
The current body of science and research indicates a strong link to periodontal bacteria that impacts the systemic health of our patients. Patients who smoke, have diabetes, or previous personal histories of periodontal disease, as well as those with autoimmune disorders, are considered at high risk for the progression of periodontal disease. We could add pregnancy to this high-risk group due to the increase in progesterone, which is a proinflammatory hormone. For these reasons, we should be diagnosing periodontal treatment for these patients even in the absence of pocketing, bone loss, and subgingival calculus deposits.
Please note that most insurance companies will not provide a benefit for patients with pockets of 3 mm or less, (some insurers designate 4 mm or less) with treatment coded 4341 or 4342. Even though there is a lack of insurance assistance, as health care providers we should be diagnosing therapeutic treatment for those patients with bleeding gums.
- The ADA CDT descriptor for a D4910 periodontal maintenance reads: “This procedure is instituted following periodontal therapy and continues at varying intervals, determined by the clinical evaluation of the dentist, for the life of the dentition or any implant replacements. It includes removal of the bacterial plaque and calculus from supragingival and subgingival regions, site specific scaling and root planing where indicated, and polishing the teeth. If new or recurring periodontal disease appears, additional diagnostic and treatment procedures must be considered.”
This procedure differs significantly from the D1110. Where the prophy is designed to control local irritational factors and prevent disease, the periodontal maintenance procedure is designed to maintain disease remission for a patient who has a previous history of periodontal disease and/or any other risk factors.
Continues at varying intervals refers to the obligation of the clinician to customize the frequency of the maintenance visit. When determining the best interval for each patient, the clinician should consider risk factors, systemic links, compliance, home care and dexterity, contributing restorative factors, and genetic susceptibility.
In 1993, the Journal of the American Dental Association published an article titled, “Periodontics in General Practice.” The article commented on the importance of customizing the periodontal maintenance interval, noting, “A recall appointment should include complete periodontal exam, response diagnosis, professional supra- and subgingival tooth cleaning and recommendations for any additional treatment. From a legal standpoint, both the patient and the practitioner have acquired new duties. The professional is obligated to inform the patient that professional plaque control is necessary on a two to three months basis (60 to 90 days) and to provide professional tooth cleaning, examination, and diagnosis. Providing periodontal treatment without accompanying periodontal maintenance should be considered negligent care by the practitioner.”
The customized interval should be set to help the patient reach and maintain their “biofilm threshold” or “balance point,” which is defined as the length of time a patient can go between professional subgingival biofilm disruptions and maintain disease remission. The JP Institute recommends weeks rather than months when determining the interval.
This procedure includes site specific scaling and root planing where indicated. Site specific refers to localized areas only. The JP Institute offers the additional guideline of no more than four sites to be treated (rather than maintained) at this visit.
I am sure you can see the wisdom in limiting the amount of site specific treatment during this visit due to time constraints. Attempting to treat new or recurrent disease in this appointment is contraindicated. The patient should be diagnosed during this procedure with a recurrent or new infection and given a treatment plan for therapeutic treatment.
Years ago this procedure included an exam. That is no longer the case. It is very appropriate for the doctor to provide an exam for an additional fee, typically twice per year.
In my observation, many offices include oral irrigation during periodontal maintenance — most commonly, chlorhexidine, povidone iodine, or a bleach and water solution.
- The ADA CDT descriptor for a D4341 periodontal scaling and root planing (four or more teeth per quad) and D4342 (one to three teeth per quad) reads: “This procedure involves instrumentation of the crown and root surfaces of the teeth to remove plaque and calculus from these surfaces. It is indicated for patients with periodontal disease and is therapeutic, not prophylactic, in nature. Root planing is the definitive procedure designed for the removal of cementum and dentin that is rough, and or permeated by calculus or contaminated with toxins or microorganisms. Some soft tissue removal occurs. This procedure may be used as a definitive treatment in some stages of periodontal disease and/or as part of presurgical procedures in others.”
Since this is a therapeutic service and not a preventive service, the only criterion necessary to use this code is the presence of disease. The descriptor indicates the removal of plaque (biofilm) and calculus and is indicated for patients with periodontal disease. The descriptor does not mention depth of pocket as a criterion. However, in my experience, most insurance companies will only assist the patient if they have pockets of 4 mm or greater.
The D4342 code is very appropriate to use for a periodontal maintenance patient who needs to go back through some isolated areas of treatment. Most insurance will not assist unless 18 to 24 months have passed since the patient’s last treatment, or use of the 4341 or 4342 codes. We, of course, should still diagnose the treatment and give the patient the opportunity to pay for it as fee-for-service treatment.
- The ADA CDT descriptor for a D4355 full mouth debridement to enable comprehensive evaluation and diagnosis reads: “The gross removal of plaque and calculus that interfere with the ability of the dentist to perform a comprehensive oral evaluation. This preliminary procedure does not preclude the need for additional procedures.”
If you cannot determine the periodontal case type of a patient due to the amount of calculus present, this is the procedure code to use. This is not a subgingival gross scale, however. This procedure indicates the removal of enough calculus to allow comprehensive periodontal charting. Overtreatment can occur very easily, causing pockets to heal, sealing off calculus on the root surfaces followed by abscess formation. Often, there are limitations to this code; typically, the patient has a once in a lifetime benefit.
- The ADA CDT descriptor for a D0180 comprehensive periodontal evaluation – new or established patient reads: “This procedure is indicated for patients showing signs or symptoms of periodontal disease and for patients with risk factors such as smoking or diabetes. It includes evaluation of periodontal conditions, probing and charting, evaluation and recording of the patient’s dental and medical history and general health assessment. It may include the evaluation and recording of dental caries, missing or unerupted teeth, restorations, occlusal relationships, and oral cancer evaluation.”
Keep in mind that this code is a diagnostic code and may be billed from the hygiene chair only when the doctor does an exam. The hygienists may do the evaluation of periodontal conditions, probing and charting, evaluation and recording of the patient’s dental and medical history, and general health assessment. When these steps are included, billing this code is perfectly appropriate, even if other procedures were provided.
As you apply your understanding of these insurance codes and their parameters, you will be able to assist your patients in receiving the appropriate care while maximizing their insurance benefits. The more we can think of dental insurance as a benefit rather than a limiting factor, the more our patients will perceive their insurance as a benefit as well.
Kimberly R. Miller, RDH, BSDH, RDHMP, is a partner of the JP Institute and a cofounder of PerioFrogz. A graduate of Loma Linda University in 1981, she received a bachelor’s degree in dental hygiene.