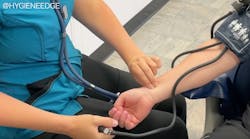
On the “pulse” of cardiovascular wellness through dental treatment
As dental professionals know, systolic blood pressure (SBP) represents the maximum pressure exerted on arterial walls during cardiac contraction (systole), whereas diastolic blood pressure (DBP) reflects the minimum pressure on arterial walls during cardiac relaxation (diastole).
SBP and DBP are essential markers of cardiovascular function, reflecting the heart's pumping ability and the resistance of peripheral arteries, respectively. Hypertension's role as a significant risk factor for various health conditions, including cardiovascular diseases, renal diseases, metabolic disorders, neurological disorders, autoimmune disorders, and obstructive sleep apnea, is well-established.
While much attention is given to systolic and diastolic blood pressure individually, pulse pressure (PP) provides unique insights into arterial health and cardiovascular function. PP is the difference between systolic and diastolic blood pressure and an essential parameter in cardiovascular physiology. PP reflects the dynamic interaction between the heart and the arteries, representing the force exerted by the heart during systole and the resilience of the arterial system during diastole. A wider PP indicates increased arterial stiffness and reduced arterial compliance, whereas a narrow pulse pressure suggests better arterial elasticity. However, a PP less than 25% of the systolic pressure is inappropriately narrow.
The clinical relevance of PP
Normal PP is in the range of 40–60 mm HG. A low or narrow pressure could indicate decreased cardiac output and is often observed in patients with heart failure. Elevated or wide pressure exceeding 60 mm Hg may stem from factors such as atherosclerosis or hypertension, and its likelihood tends to increase after the fifth decade of life.
Disorders such as iron deficiency anemia and hyperthyroidism can lead to an increase in PP.1 Research has shown that wider PP is associated with an increased risk of adverse cardiovascular events, including coronary artery disease, stroke, and heart failure, and serves as an independent predictor of cardiovascular risk.2
Arterial stiffness, reflected by elevated PP, is a hallmark of vascular aging and atherosclerosis. Prolonged exposure to high pulse pressure can lead to structural changes in the arterial walls, promoting the development of arterial plaque and contributing to cardiovascular disease progression. PP provides valuable hemodynamic insights into cardiovascular function and influences myocardial oxygen demand, left ventricular afterload, and coronary perfusion.
Wide PP may strain the heart, particularly in individuals with preexisting cardiac conditions, leading to adverse remodeling and impaired cardiac function. Some cardiovascular patients’ physicians may already be targeting both systolic and diastolic blood pressure to reduce pulse pressure for the prevention of end-organ damage and cardiovascular events.
Pulse pressure and periodontal disease
The relationship between periodontitis and blood pressure is nothing new. In a meta-analysis of observational studies, we know that periodontal disease can lead to an increase in blood pressure. In observational studies periodontal disease was significantly associated with the 20% higher risk of unsuccessful antihypertensive treatment.3
While PP may not have received as much research attention as other cardiovascular indicators, there are several mechanisms that could elucidate the relationship between periodontal disease and PP. Periodontal inflammation can trigger systemic inflammation, leading to endothelial dysfunction and arterial stiffness. Inflammatory mediators released from periodontal tissues can impair endothelial function, causing vasoconstriction and increased arterial stiffness.
Moreover, extended exposure to periodontal pathogens may activate the immune system, inducing an inflammatory response that disturbs vascular homeostasis and worsens arterial stiffness. In 2022, data was analyzed for 3,496 Korean adults 20 years of age and older showing that periodontal disease was positively associated with high pulse point in the adults with hypertension, but not in those who did not have hypertension.4
Managing PP is necessary, as a higher PP indicates increased strain on the heart, reduced arterial flexibility, or both. These conditions heighten the risk of heart and circulatory issues, particularly heart attack or stroke. Therefore, monitoring and addressing PP levels wide or narrow is essential for maintaining cardiovascular health and preventing adverse outcomes.
Health-care providers can use PP as part of their assessment to identify patients at risk for cardiovascular issues. Our role is not just recording numbers; it's to understand what the numbers mean and empower our patients to take proactive steps in managing their well-being.
References
1. Jobbé-Duval A, Bézard M, Moutereau S, et al. Prevalence and determinants of iron deficiency in cardiac amyloidosis. ESC Heart Fail. 2022;9(2):1314-1327. doi:10.1002/ehf2.13818
2. Wang M, Su W, Jiang CY, Li WP, Chen H, Li HW. Association between pulse pressure with all-cause and cardiac mortality in acute coronary syndrome: an observational cohort study. Front Cardiovasc Med. 2022;9(7). doi:10.3389/fcvm.2022.930755
3. Surma S, Romańczyk M, Witalińska-Łabuzek J, Czerniuk MR, Łabuzek K, Filipiak KJ. Periodontitis, blood pressure, and the risk and control of arterial hypertension: epidemiological, clinical, and pathophysiological aspects-review of the literature and clinical trials. Curr Hypertens Rep. 2021;23(5):27. doi:10.1007/s11906-021-01140-x
4. Yoon H, Seong JM. The relationship between pulse pressure and periodontal disease in Korean populations with or without hypertension. Appli Sci. 2022;12(10):4973. doi.org/10.3390/app12104973
About the Author

Anne O. Rice, BS, RDH, CDP, FAAOSH
Anne O. Rice, BS, RDH, CDP, FAAOSH, founded Oral Systemic Seminars after over 35 years of clinical practice and is passionate about educating the community on modifiable risk factors for dementia and their relationship to dentistry. She is a certified dementia practitioner, a longevity specialist, a fellow with AAOSH, and has consulted for Weill Cornell Alzheimer’s Prevention Clinic, FAU, and Atria Institute. Reach out to Anne at anneorice.com.