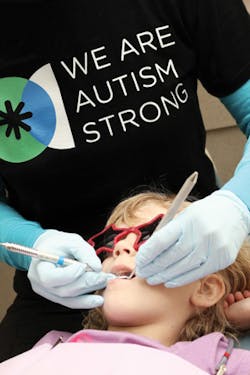
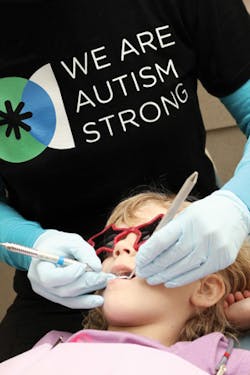
The autism challenge
In some cases, anesthesia is needed. For the rest, the motto is: Stop needless sedation
BY Josalyn Sewell, RDH, OMT
Have you ever felt so strongly about something that it kept you up at night? Has there ever been something so important to you that you were moved to action? For me that issue is working with and advocating for individuals affected by autism.
This is the first in a series of articles about autism as it relates to the field of dental hygiene. Future articles will be more scientific in nature and will discuss the diagnosis, medical comorbidities, and associated behaviors of autism, as well as strategies for the dental hygienist.
In this introduction I will present a case study that appropriately demonstrates a devastating trend in the dental management of patients with special needs-the overuse of sedation and general anesthesia simply because a child has a diagnosis.
The author's buddies
I would like to introduce you to three of my special friends: Sunni, Levi, and his little sister, Khloe, who all have autism spectrum disorders. Although the children are between the ages of five and nine, no dental professional had ever seen any of them before January of this year. This is not uncommon for children affected by autism because their parents have a hard time finding professionals trained to work with autistic children. Oral health takes a back seat to the host of other therapy appointments a child with autism requires - speech therapy, behavior therapy, occupational therapy, eating therapy, play therapy, music therapy, and physical therapy, to name a few.
In general, oral care for children with autism can be particularly difficult, and parents fear a dental appointment will be excessively challenging.
In these particular cases, the children had not visited a dental professional because they had written off the children as incapable of behaving, and had recommended general anesthesia before the children even stepped foot in the office. Both mothers had called numerous dental offices in search of a dental home with professionals trained to work with children with autism.
Top row from left: Samantha Sam, Josalyn Sewell, Kaitlin Harris, Kelly Foutz. Bottom row: Khloe, Levi, and Sunni
The conversation typically went something like this, "Hello, I have a child with autism. She's never seen the dentist and I'm not sure how she will react. Do you have anybody trained to work with children with autism?"
The reply was usually, "We would love to help you! We absolutely have training and we do it all the time. We just sedate them."
Neither mother felt an overwhelming desire to traumatize her child, expose the children to general anesthesia, or incur the steep cost, especially when the children did not have obvious signs of pain or dental disease.
I received word of their frustration and volunteered to help the children overcome their fear of the dental environment. San Juan Community College generously allowed me to use their facilities on a Friday morning when the students were not in clinic. I was assisted by three senior dental hygiene students, Kaitlin Harris, Kelly Foutz, and Samantha Sam, who volunteered to learn more about working with children on the spectrum.
The first appointment was set up as simply an introduction to the dental environment, much like a happy visit is for small children. Each child allowed me to polish, floss, and place fluoride varnish. We met the following week to add the more difficult aspects of a hygiene appointment. I allowed the students to work as the clinicians, and I sat chairside to assist and intervene if we faced any unseen challenges.
All three children had radiographs (a pano and four bitewings), a prophy that included scaling and polishing, flossing, fluoride varnish application, and a dental exam. They all required minimal support. Levi and Khloe covered their ears when the suction was on during the first appointment, but not during the second. Sunni had to be reminded to keep her hands on her belly, but she never grabbed or hit at the instruments. The dental exams revealed no pathology, not a single carious lesion. We did find that Levi is congenitally missing No. 10.
Now, stop here to take in what this means for these families. If they had gone with what the dental offices recommended for these children, they would have been subjected to general anesthesia and the trauma associated with IVs, needle sticks, heavy medication, recovery, and time off work and school for preventive services. That is not OK! The children were seen by dental hygiene students, not a highly trained, highly experienced clinician. Instead, we took a minimally invasive approach, and I feel confident saying that all three children can now approach dental appointments without anxiety.
The families had a good experience, the children know what to expect and how to behave, and they will be excellent patients for any clinician lucky enough to work with them in the future. Not all children with autism will have such an easy time. Behaviors and sensory challenges can make dental appointments challenging, but there are plenty of individuals with autism who are completely capable of visiting the dental office without the use of sedation and general anesthesia. I'm suggesting that you try not to get hung up on the autism diagnosis.
The trouble with general anesthesia and sedation
I am not against the use of general anesthesia or sedation when the risks truly outweigh the benefits. We have used general anesthesia for my son Ethan, who has moderate-severe autism, when he needed to have two interproximal caries restored. While he was under we made sure to take radiographs, place sealants, and give him a thorough prophy. He allows me to scale his teeth, but only for a very short time and not all at once.
I find that even when a child requires anesthesia for restorative procedures that there is a lack of follow-through in getting the child back to the office for preventive services. Please don't let this happen in your office. General anesthesia is not without risks, most of which are temporary. Autism is a multifaceted disorder that is not all neurological, as I will point out in the next article. A portion of the autistic population also experience metabolic challenges or dysfunction, which means that it can be more difficult for their bodies to metabolize medications, and anesthesia can affect them differently. When small children undergo general anesthesia, they generally return to normal activity levels by the end of the day or by the next day, depending on the medications used, the duration of the anesthesia, and the procedure completed.
Josalyn Sewell with Khloe, Levi, and Sunni.
Following general anesthesia, Ethan was not himself for nearly four days. Communication is difficult for him. He is nonverbal but uses his iPad or single words to express several requests. After anesthesia, he did not communicate anything, had a hard time understanding things I asked him to do, and was generally in a fog. When I discussed this with the dentist and anesthesiologist, I was told that they see this phenomenon in children with autism all the time. They feel like it takes children with autism about three times longer than the average child to overcome the effects of general anesthesia due to potential metabolic challenges. Understand that this not a hard and fast rule and I could not find the scientific data to back that claim. I'm simply sharing my personal experience in an effort to shed light on the challenges your patients face. Take time to understand the potential risks and side effects, and do all you can to complete dental hygiene services in the office.
A complicated problem
I think it is important to discuss the different practices that are contributing to the problem, and some potential solutions.
1. Dental professionals and parents are unaware of the potential dangers of repeated use of general anesthesia. More research needs to be conducted on the effects of general anesthesia on a fragile brain such as those with autism.
2. Dental professionals lack adequate training. Working with individuals with autism often requires more than the simple tell-show-do approach with children. It is important to seek quality continuing education specific to autism spectrum disorders.
3. People have preconceived notions. We should not assume that a child with special needs is incapable of learning or overcoming fear and sensory challenges.
4. Front-desk staff should be trained in how to gather more information. If a patient calls to make an appointment for someone with autism, rather than assuming the individual will not cooperate and recommending sedation, front-desk staff should ask questions like, "Has the child ever been to a dentist? Does the child communicate? How does the child behave in doctors' offices? Does the child have a hard time brushing and flossing at home?" I do not expect general practices to see severely affected patients, but with the prevalence of autism, it is not realistic to leave the work to pediatric and special-needs dental offices.5. Sometimes parents omit the truth. They bring a child to the dentist without alerting dental professionals that their child has autism. The child struggles to behave, we think they are just "naughty" and we push for appropriate behavior, the child melts down, and it usually ends pretty ugly. But can you blame parents? They might have been turned down for services based on a diagnosis and not on actual ability. This is not fair to the dental professional, the family, and especially the patient.
6. If a child requires anesthesia once, parents may assume it must always be done that way. As children mature and are exposed repeatedly to the dental environment, they will learn to behave appropriately. Coach your patients to return for preventive services, even if restorative has to be done with sedation.
7. Dental offices should develop protocols, including whether or not they want to treat individuals with special needs. If the clinicians do not enjoy children or are afraid of individuals with special needs, then refer to another office. If you choose to treat them, develop a method to help patients with autism, such as making them the first appointment of the day, or set aside an afternoon a month when the office is slow and more time can be given to these patients. Be sure to get some training to support you in your efforts.
8. General anesthesia is expensive. Even when insurance is available, there can be large out-of-pocket expenses, not to mention time off work and school.
Sunni, Levi, and Khloe's story is not unique. As an avid blogger about autism and oral health, I often receive emails from families all over the country that have faced similar problems - dental offices recommend sedation and anesthesia before a child steps into the office. I hear desperate pleas for help finding dental professionals trained to work with individuals with autism.
I have one foot in both worlds. As a hygienist I see how difficult it is to find the time in a busy hygiene schedule for happy visits and acclimation programs. I see the turmoil of wanting to help and knowing what to do, but not knowing what to bill and what to charge.
As an autism mom, I need help, and I want access to professionals who can help me. As an advocate for my special friends, I cannot ignore the burning in my heart that moves me to action. If you will take the time and open your heart and practice to individuals with autism, I can assure you that you will not walk away from the experience unchanged. You have the power, the talents, and the ability to make a real difference in the lives of these patients.
I strongly encourage you to work harder to avoid sedation and general anesthesia and do more to help teach the patients appropriate behavior. Once they learn the behavior, most individuals with autism will strictly adhere to the rules and become some of your best patients. Don't be stumped by a diagnosis and don't be blocked by a label. As hygienists, we have a gift for working for people and this area is no exception. Kindness matters and goes a long way. Fight the good fight. Make a difference. Stop sedating needlessly. RDH
Josalyn Sewell, RDH, OMT, enjoys many aspects of a dental hygiene career, including clinical work, teaching, speaking, writing, and sales. She is a member of both the ADHA and CareerFusion. Josalyn's full-time position is in domestic management (stay-at-home-mostly-mom) in a rural town in the mountains of eastern Arizona. She blogs about what it is like to raise a child on the autism spectrum. You can find her blog at: autismaintforsissys.blogspot.com or on Facebook: Autism Ain't for Sissys.