Lumps and bumps belong in bottles!
by Nancy W. Burkhart, BSDH, EDD
"Lumps and bumps belong in bottles!" Does this sound familiar? Most practitioners remember their original oral pathology course, and the professor using this exact phrase. I certainly do! Most pathologists still use this sentence and truly believe that if a diagnosis cannot be established clinically, a biopsy is warranted. Lumps and bumps do not belong on the oral structures and are removed for diagnostic purposes to establish an etiology and to rule out malignancy.
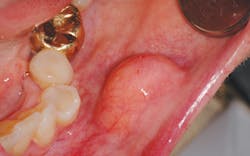
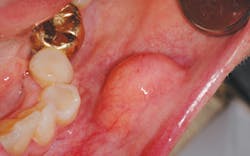
One such entity that is often perplexing to the clinician is the lipoma. (see Figure 1) It is one of the most common total body tumors, yet it is also a rare benign neoplasm not often found intraorally. In order of occurrence when found intraorally, these growths may occur on the buccal mucosa (because of the abundant fatty tissue), the tongue, the floor of the mouth, buccal sulcus, palate, lips, and gingiva (Kumaraswamy et al.2009). They have also been found in the oral pharyngeal area and may interfere with swallowing. This is another excellent reason to critically examine the tonsillar and pharyngeal areas since tonsillar cancer is a prime concern as well.
Lipomas are slow growing, painless, soft, smooth-surfaced, palpable masses, and are noted as having a yellow hue. They are unlike the fibroma, which does not normally present with a yellow-tinged surface and presents a more firm and flesh-toned appearance.
Lipomas are usually discovered by the dental practitioner unless they become large enough to be detected by the patient. Eyewear and illumination give dental professionals an edge on detecting small growths. Most are discovered in a less than 3 cm diameter size, but large lipomas have been documented as well and may exceed 11 cm as reported by Chidzonga, et al. 2006, who documented a gigantic tongue lipoma. When they are left untreated and continue to grow, larger lipomas occur. In a retrospective study of 207 patients with intraoral lipomas conducted by Taira, et al. 2012, the most frequent size was reported to be 10-19 mm with a finding of 57.5% males and 42.6% females.
One to four percent of lipomas occur intraorally and they may be confused with the fibroma when found in some locations of the mouth -- especially in areas where friction may occur. A combination of a fibroma and lipoma is documented and is referred to as the fibrolipoma. The fibrolipoma has characteristics of both fibrous connective tissue and adipose tissue when viewed microscopically. Although the lipoma is benign, the malignant counterpart to the lipoma is the liposarcoma. The need to confirm that the entity is truly benign is crucial for a definite diagnosis.
Some researchers and clinicians believe that the lipoma may be more common than those documented, but they are often not reported or noted in most instances. The tumors are rarely reported in children and the mean age in adults is the fifth through seventh decade (Taira, et al. 2012). Often, lipomas may be noticed for years by the patient before they are clinically identified or removed in a dental practice.
The lesions are broad-based and composed of adipose tissue with an unknown etiology. Some authors report an occurrence of blunt force or soft tissue trauma to the area preceding the development of external lipomas (Aust, et al., 2007). Microscopically, the tissue is covered by a thin layer of epithelium and appears to be normal adipose tissue. The lobules of mature fat cells are circumscribed and thinly encapsulated by a fibrous covering, and are found in a loose fibrous stroma. There is little to no inflammatory component in the lipoma specimen. As evidenced by the tissue found within a container in Figure 2, the specimen will float within the fixative agent giving the pathologist a heads-up on what the submission may contain.
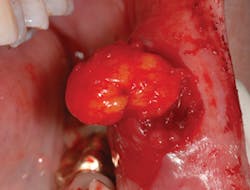
The treatment for a lipoma is excision, and recurrence is usually not a factor (see Figure 3). When examining a patient who has had a previous lesion of any type, the practitioner has more reason to suspect and to monitor the person for either the development of a future neoplasm or the recurrence of a previous growth. Follow up and evaluation are always needed for early discovery and treatment. The dental hygienist can be instrumental in detection of early lesions of any kind because of the continuity of patient maintenance appointments and the length of time that the hygienist spends with the patient. The dental practitioner becomes very familiar with his/her patients and the tissue of each individual. Intraoral images are always the ideal way to monitor any suspected area for tissue changes.
As always, keep asking good questions and always listen to your patients.RDH
References
Aust MC, Spies M, Kall S, Gohritz A, Boorboor P, Kolokythas P, Vogt PM. Lipomas after soft tissue trauma:are they real? Analysis of 31 cases. Br J Dermatol. 2007 Jul; 157(1):92-9.
Burkhart, NW. Lipoma. RDH. 2007; 27:9: 90-92.
Chidzonga MM, Mahomva L, Marimo C. Giagantic tongue lipoma: A case study. Med Oral Patol Oral Cir Bucal. 2006;11:E437-9.
DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. 2nd ed. Lippincott Williams & Wilkins, Baltimore. 2012.
Kumaraswamy SV, Madan N, Keerthi R, Shakti S. Lipomas of oral cavity: case reports with review of literature. J Maxillofac Oral Surg 2009; 8(4): 394-397.
Lee SH, Yoon HJ. Bilateral asymmetric tongue classic lipomas. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012; 114(1):e15-8. Doi: 10.1016/j.tripleo.2011.07.045. Epub 2012 Jan 27.
Taira Y, Yasukawa K, Yamamori I, Lino M. Oral lipoma extending superiorly from mandibular gingivobuccal fold to gingival: a case report and analysis of 207 patients with oral lipoma in Japan. Odontology. 2012;100 (1): 104-108.
Relevant Internet Articles
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3177381/
Past RDH Issues