Back to Basics
By B. Michelle Strange, RDH, MSDH
I have witnessed numerous ways of scaling teeth over the years, both teaching in dental hygiene clinics and during volunteer programs where I helped assist colleagues. I have observed an array of techniques -- some light-handed, some awkward, some aggressive and slightly scary, and some downright impressive. Hygienists love to stop at the product exhibit booths and handle the latest instruments that companies have to offer.
However, even with the most innovative instruments, we sometimes just need to remember our basic techniques for instrumentation and root debridement, especially when we encounter a patient who requires advanced instrumentation. When patients present with moderate to advanced periodontitis, instrumentation in these deep periodontal pockets can be a challenge. Remembering advanced fulcrum techniques, root morphology, and types of strokes, as well as being knowledgeable about new instruments, are crucial in treating our patients.
While writing this article, I was approached concerning two different incidents regarding scaling technique. A former student was let go from her office because she did not feel comfortable going subgingivally. A week later, a referring office contacted my private practice asking if the two full-time hygienists could shadow me for an afternoon, because they felt unsure about seeing periodontal patients.
-----------------------------------------------------------------------
Other articles of interest:
- How not to overwork your hands: Use a little leverage during periodontal instrumentation
- CAMBRA and caries detection technology
- Using your dental hygienist for laser periodontal care
-----------------------------------------------------------------------
We can get spoiled in our practices by seeing children who do not require advanced techniques and our "easier" patients who do not struggle with disease and inflammation. We can lose our confidence or skills to treat the more advanced areas. Some hygienists, of course, are not lucky enough to have access to the new instruments or technology and must make do with what they have such as advanced fulcruming and knowledge of root surfaces. Regardless of whether graduation was last year or 30 years ago, it is important to stay current with the newest technology, remembering what we learned in school and in continuing education classes.
So, let's get back to the basics and review the five Ws and the how of advanced instrumentation.
What
Advanced instrumentation entails use of fulcrums that require us to move from our more common same-arch finger rest nearest the tooth we are instrumenting to a fulcrum that can be extraoral, on the chin or cheek, cross arch, opposite arch, or finger-on-finger (my favorite for the extremely tenacious calculus).1 Advanced instrumentation also involves having excellent knowledge of root morphology and understanding where root concavities and depressions -- as well as the occasional root fissures -- occur, and using the correct strokes to remove calculus from these areas.
Gingival or soft-tissue curettage can occur when seeing a patient who requires advanced instrumentation. Not every state allows hygienists to perform gingival curettage, so be sure to check your state laws. The American Dental Hygienists' Association has a great resource that breaks down each state with its allowed functions for dental hygienists.2 I hope to see a day when all states allow dental hygienists to provide soft-tissue management. My years in a periodontal office have shown me that it takes more than just cleaning the root surfaces. Removing the diseased tissue that exists along the root surface is just as important and always gives the best healing results.
Who
Determining the need for advanced instrumentation requires hygienists to thoroughly assess their patients and determine the state of their periodontal health. Advanced instrumentation can be performed on patients with generalized or localized and moderate to advanced chronic periodontitis. Moderate periodontitis can be classified as bone loss past the crest to one-third of the supporting structures with attachment loss of 3 to 4 mm, with a class I furcation present.3
When identifying more advanced cases, a hygienist may find greater than 4 mm of attachment loss, with bone loss affecting more than one-third of the supporting structures, including furcations greater than class I and possibly mobility.3 Identifying the chronic periodontally involved patient and effectively performing advanced instrumentation for subgingival debridement is the most reliable way of improving the disease activity and improving the attachment level of our patients.4
When and Where
Ideally, treating areas affected by periodontal disease with advanced instrumentation as soon as possible is best. This can be when we see our patients initially in our office or on recall when we may find isolated areas of inflammation. If this procedure cannot be done during the normal recall, then bringing the patient back for scaling and root planing (and gingival curettage, if possible) would be best.
Having the time to perform the techniques involved in advanced instrumentation, as well as the time to review home-care techniques, and then arranging the appropriate recall appointment are key. One study found "that professionally delivered and frequently repeated supragingival tooth cleaning, combined with careful self-performed plaque control, had a marked effect on the subgingival microbiota of moderate to deep periodontal pockets."5
This evidence is a great reminder that having knowledge and the skills for advanced instrumentation is important, but they are not the sole reasons for improvement in a periodontal patient. We also must keep in mind that frequent supragingival plaque removal is extremely important. We could have the newest instruments on the market and the best technology but, if we are not educating our patients about proper home-care techniques, then advanced instrumentation will only benefit the patient temporarily.
This concept can be lost in the hustle of a busy schedule. Maybe we don't have the time to explain home-care regimens or have openings in our schedule to reappoint for more frequent recall appointments. If this is the case, we must evaluate our scheduling in order to generate the best results for our patients. After initial therapy involving advanced instrumentation and appointing the patient to the appropriate recall frequency, we may have to perform advanced instrumentation during those recall appointments. This is not uncommon in order to treat areas that are chronically inflamed and difficult for the patient to clean.
When assessing our patients, we must decide on the appropriate treatment and not just go about our normal routines. If the patient requires irrigation with an electronically-powered instrument, such as the ultrasonic or piezoelectric scalers, or using instruments with longer shanks or miniature working ends, then it is our responsibility to treat accordingly.6 Using the appropriate instrument with the proper working stroke is crucial to the success of our periodontal patients.
Why
The reason we perform advanced instrumentation is pretty straightforward: Periodontitis causes bone loss, and the effective removal of the biofilm is necessary to achieve the best results for our patients. Now, why do we choose certain types of fulcrums and strokes vs. others? Would using a combination of strokes and fulcrums we learned prove more successful?
Choosing multiple strokes and adjusting our fulcrums to access the area during our scaling and root planing would increase the chances of eliminating the biofilm that resides in the deep periodontal pockets along the root surfaces. Scaling every aspect of the tooth, however, cannot be done without advanced instrumentation. Having a strong understanding of advanced instrumentation is fundamental. When biofilm and calculus go undetected, disease progression is very likely. Seems like Hygiene 101, right? Yet sometimes we fall into such a routine or run behind in our schedules that we don't take the time to correctly assess our patients and their needs.
How
If we do not have access to the newest instruments, then we need to fall back on what we know: fulcruming, lateral pressure, and using the appropriate strokes in order to access the deep pockets and perform advanced instrumentation. The pressure we apply to the side of the instrument, or lateral pressure, should be used no matter where our fulcrum is placed.7 This method allows you to make adequate strokes without gliding off of the tooth and causing trauma to soft tissue. I often tell my students that you should hear the strokes. When I show them a root planing stroke, the first observation they makes is that you can hear the strokes I am making to debride the root surface.
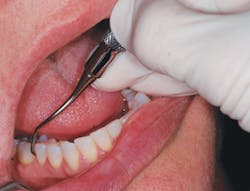
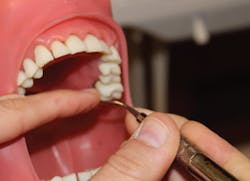
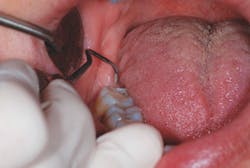
Finding the best fulcrum, in addition to lateral pressure, is important to advanced instrumentation. Moving from our basic intraoral fulcrum to a modified intraoral fulcrum can be useful for instrumenting the maxillary posterior teeth. Cross-arch fulcruming occurs when you rest the ring finger on a tooth on the opposite side of the arch from where you are instrumenting6 (see Figure 2). Opposite-arch fulcruming is an excellent way to access deep pockets while continuing to have parallelism to the proximal root surfaces. For example, when trying to access the mesiolingual of No. 14, you may fulcrum on the lower anterior teeth in order to keep the instrument parallel to the root surface (see Figure 5). I commonly use an extraoral fulcrum to achieve the best position for my instrument in deeper periodontal pockets. A knuckle-rest technique can be used by placing the clinician's knuckles on the patient's chin or cheek6 (see Figure 4). The hand can also be placed in a cupping position on the patient's chin when fulcruming (see Figure 1).
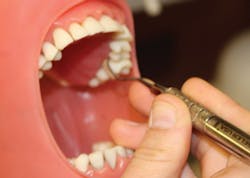
You must keep in mind that these fulcrums will not allow you to grasp the instrument in the same way as if you were using a typical intraoral fulcrum. You will have to slide your hand away from the shank in order to reach the deeper pockets and establish a modified intraoral or extraoral fulcrum. One of my personal favorites for removing tenacious calculus, especially in the posterior, is the finger-assisted fulcrum (see Figure 3). The index finger of your nondominant hand will press against the shank of the instrument to help apply lateral pressure, and your working hand can use an intraoral or extraoral fulcrum. I find that this method helps control my working strokes and keeps my hand from being overworked.
If you have graduated from a dental hygiene program, it is assumed that you know how to properly adapt your instruments subgingivally without causing harm to the patient. Now it is time to be creative with your instrument placement. I remember the first time I told a student that she could use the posterior instrument in the anterior. You would have thought I told her she was allowed to break a law. But it is true; we know how our instruments should be used, but thinking outside of the box is a part of advanced instrumentation.
This can mean flipping your instrument to the opposite working end, using a toe-down position and making a horizontal stroke. Imagine that I need to access the distal of No. 31. I would use my Gracey 13/14 or 17/18 (one of my personal favorites) and, instead of using the "appropriate" working end, I will flip my instrument, insert the curette with the toe-down and make horizontal strokes from the lingual to the facial of the distal of that tooth (see Figure 6). This is one of my favorite ways to reach the distal of the last molars. Horizontal strokes, or channeling strokes, are needed in order to be successful with advanced instrumentation.
When seeing your patients who have deep pocketing, clinicians must take into account that we cannot stick with the basic instrumentation. We have to move toward a more advanced technique to properly debride the root surfaces and properly treat the patient. Yes, this means that we must go subgingival and change our routine depending on our patients' needs.
Periodontal disease occurs in all of our offices. We need to diagnose properly and then provide the appropriate level of care. If we are not able to obtain the newest instruments, we can still use these advanced techniques to provide care for our patients.
B. Michelle Strange, RDH, MSDH, is a practicing clinician in a private periodontal office, as well as adjunct faculty at Trident Technical College in Charleston, S.C., and is an education consultant for TePe Oral Health Care Inc. She can be reached at [email protected].
References
1. Sanz I, et al. Nonsurgical treatment of periodontitis. J Evid Based Dent Pract, 2012. 12(3 Suppl): p. 76-86.
2. American Dental Hygienists' Association. Dental Hygiene Practice Act Overview: Permitted Functions and Supervision Levels by State. Available at: http://adha.org/ resources-docs/7511_Permitted_Services_Supervision_Levels_ by_State.pdf. Accessed July 17, 2013.
3. Parameter on chronic periodontitis with advanced loss of periodontal support. American Academy of Periodontology. J Periodontol, 2000. 71(5 Suppl): p. 856-8.
4. Heitz-Mayfield LJ, et al. A systematic review of the effect of surgical debridement vs nonsurgical debridement for the treatment of chronic periodontitis. Journal of Clinical Periodontology, 2002. 29 Suppl 3: p. 92-102; discussion 160-2.
5. Hellstrom MK, et al. The effect of supragingival plaque control on the subgingival microflora in human periodontitis. J Clin Periodontol, 1996. 23(10): p. 934-40.
6. Nield-Gehrig JS. Fundamentals of periodontal instrumentation and advanced root instrumentation. 2004. Philadelphia Lippincott Williams & Wilkins.
7. Pattison A, Pattison G. Extraoral fulcrums. Dimensions of Dental Hygiene, 2004. 2(10): p. 20-23.
Past RDH Issues