Hydrogen peroxide in dentistry
Tray delivery helps hydrogen peroxide deliver its punch to biofilm
by Jeanne Bosecker, BSN, RDH
When most of us think of hydrogen peroxide, we envision a brown bottle in the medicine cabinet or first aid kit. Hygienists and dentists may also have some memory of "black hairy tongues" as a side effect of oral rinsing with hydrogen peroxide.
The truth is that hydrogen peroxide is used safely and effectively in dentistry today. While its most common application involves tooth whitening, significant health benefits are documented using hydrogen peroxide to treat gingivitis and periodontitis.
The first use of hydrogen peroxide in dentistry was in 1913, used to decrease plaque formation and to control "pyorrhea" or gum disease. The now known mechanism of antimicrobial action is the release of oxygen, and pathogenic effects are seen in gram-positive as well as gram-negative organisms.₁ Another mechanism of antimicrobial action is the effect the hydrogen peroxide has on the debridement of bacterial call walls. A 10 minute exposure to a 1.7% hydrogen peroxide gel penetrates the biofilm slime matrix and debrides the cell walls of in vitro S. mutans biofilms. Microbiologists have also hypothesized that peroxide delivered and maintained in the sulcus or periodontal pocket releases oxygen and changes the subgingival micro-environment, making it harder for anaerobic bacteria to survive.2,5 , 6
Oxygen therapy has been shown to greatly reduce or eradicate pathogens in acute necrotizing periodontal disease, the most aggressive form of periodontal disease.3
In order to treat periodontal disease, the problem is getting the hydrogen peroxide into the periodontal pocket and holding it there long enough for it to work. Studies have shown that while rinses and dentrifices with hydrogen peroxide can help, they are not sufficient to deliver the medication deep into periodontal pockets where the infection is localized.1 A customized prescription tray (Perio Tray, Perio Protect, LLC, St. Louis, Mo, USA) is designed to deliver a solution such as hydrogen peroxide deep into periodontal pockets against the force of crevicular fluid flow. If the tray with the peroxide is worn for 15 minutes, the peroxide is shown to reach the bottom of deep pockets >7mm.2,5 , 6
It is important to hold the medication in place. Hydrogen peroxide has been shown to penetrate the slime matrix covering that protects a biofilm and then to debride the bacterial cell walls, but studies show that the peroxide needs approximately 10 minutes to do so. When biofilms were treated with 1.7% hydrogen peroxide for five minutes and examined using the Live/Dead technique, only a small proportion of cell walls were compromised. After 10 minutes, however, virtually all of the bacterial cell walls were disrupted. For a control group exposed to a gel with no hydrogen peroxide, the results were the same as the group that received no treatment at all. These results demonstrate that a 10 minute exposure to 1.7% hydrogen peroxide aqueous gel can debride bacterial cell walls within a typical dental biofilm.2
When hydrogen peroxide is delivered deep into the pocket and held in place, data indicate that the bacterial loads are reduced and so are periodontal probing depths. One study followed four patients with periodontal disease presenting at different clinical levels. Dosages were 10 minutes two times a day (Type I periodontal disease); four times a day for five weeks (Type II periodontal disease); and six times a day for 15 minutes times for two weeks (Type IV). The patients did not receive SRP or any other treatment for their periodontal disease except for the prescription tray delivery of medication.
Biofilm samplings were performed using absorbent paper points held in place in the sampled periodontal pockets for 10 seconds before Perio Tray treatment began and again two to five weeks after the daily treatment began. The points were scanned with electron microscopy. The colonies were counted, morphotypes of bacteria were defined and averaged at three standard areas of 100 µg² and averaged. After the initial SEM analysis of the paper points, the periodontal pockets were treated with 1.7% hydrogen peroxide and a sub-clinical dose (three drops per tray) of Vibramycin syrup, topically placed by prescription Perio Trays. The paper point analysis was repeated after two to five weeks of daily Perio Tray delivery of medication.2
The first patient presented with Type II periodontal disease with bleeding on probing. After five weeks of treatment wearing the Perio Tray four times a day, there was no bleeding on probing and a 1-2mm pocket depth reduction. One of three sites had no bacteria found after five weeks. The second patient presented with Type I periodontal disease. After wearing the Perio Tray two times a day for 10 minutes each time, no bleeding on probing was detected and there was a 2-3 mm reduction in pocket depth. No bacteria were found in three of four of the sites sampled after five weeks.
The third patient presented with Type IV periodontal disease. After wearing the Perio Tray six times a day for 15 minutes each time for 2 weeks, no bleeding on probing was detected, pocket depth was reduced 1-5 mm and no bacteria were found in three of the five sites sampled after two weeks. The fourth patient had Type IV periodontal disease and was treated six times a day for 15 minutes for two weeks. No bleeding on probing was found in three of the six sites sampled, pockets were reduced 0-5 mm, and two sites had no bacteria after two weeks of treatment.2
The in vitro and in vivo evidence indicate that the custom formed Perio Tray can place medications in periodontal pockets at sufficient concentration for the medications to have a significant therapeutic effect. Theoretical calculations indicate that hydrogen peroxide is capable of reaching deep periodontal pockets, even against gingival crevicular fluid pressure, and that the mechanism of action is the peroxide's oral debriding action.2
Putt et al. did a study with 30 patients with moderate to advanced periodontitis, who were randomized to SRP alone or SRP combined with the prescription custom-tray application (Perio Tray) of 1.7% hydrogen peroxide gel (Perio Gel) for a period of three months. In this examiner-blind clinical trial, clinical assessments of pocket probing depth (PPD) and bleeding index (BI), were conducted at baseline and after two, five, and 13 weeks of peroxide applications; SRP was performed three weeks after baseline. The adjunctive use over three months of 1.7% hydrogen peroxide gel, administered using prescription customized trays in the treatment of subjects with moderate to advanced periodontitis, demonstrated statistically significant clinical improvements in pocket depths and bleeding when compared to SRP alone.4
A potential problem with the prescription tray delivery system for hydrogen peroxide is that it requires daily use to be effective. Patient compliance is always a concern with any oral hygiene instruction. However in the Putt et al. study, subjects were receptive to using properly fitted trays, especially after observing rapid improvements in their oral condition.4 Several limitations are associated with the use of local delivery agents for periodontal disease, such as home care restriction around the sites, microbial overgrowth, bacterial resistance to antibiotics, patient drug allergies and sensitivities, and retention problems. The prescription tray system such as Perio Tray overcomes most of these problems and offers some potential advantages:
- Patients can use the system at home in between office visits
- It is non-invasive
- There are no restrictions on brushing or flossing around treatment sites
- Full arch treatment is beneficial for patients with significant numbers of deep pockets
- Adjunctive intervention is possible earlier than with other time-released delivery agents
- It can place medication into periodontal pockets of all depths, theoretically allowing for adjunctive care at the earliest stages of disease progression when the disease is easier to control
- It can deliver low-concentration hydrogen peroxide gel, which is a safe, well-known oral debriding agent and wound cleanser.4
As hygienists, we are pretty well aware of the use of hydrogen peroxide in teeth bleaching. As an agent to treat periodontal disease, however, most of us may not have known hydrogen peroxide to be an option. We treat a lot of patients regularly with varying levels of periodontal disease, and many patients are uncomfortable with or may even refuse treatments such as SRP or surgery.
The prescription tray delivery of hydrogen peroxide is a great option to help these patients who are reluctant to accept SRP or surgery. The tray delivery of medication is non-invasive and reportedly comfortable, Although it is best used as an adjunct to conventional therapy methods, it has been shown to have beneficial effect alone. Reducing the biofilm bacterial load in the pockets will keep the tissue healthier, reduce bleeding, and may keep the patient healthier even if he or she refuses SRP or surgery.
When patients whose gum diseases are not as advanced as to require surgery, the prescription tray delivery of hydrogen peroxide can be used at the earliest onset as an adjunctive therapy. There are no pocket depth restrictions with the prescription tray delivery, so infected tissues in 3-5 mm pockets can be successfully addressed before the disease gets worse, and there is no concern about medication being dislodged from a pocket. This can be an important preventative treatment step, especially for those patients who have a long history with you fighting the disease, or with generalized 4-5 mm infected pockets on whom we want to keep a very close eye.
Talking with hygienists who have used the prescription tray delivery, it just makes sense that this technique makes our work as hygienists easier and better. We love our work being easier and better. The benefit of having the patient be healthier makes it a winning situation for everyone. RDH
References
1. Marshall MV, Cancoro LP, Fischman SL. Hydrogen Peroxide. A Review of its uses in dentistry. J. Periodontol. 1995; 66:786-96.
2. Dunlap T, Keller DC, Marshall MV, Coserton JW, Schaudinn C, Sindelar B, Cotton JR. Subclinical Delivery of Oral Debriding Agents: A proof of Concept. J. Clin Dent. 2011;22:149-58.
3. Gaggl AJ, Rainer H, Grund E, Chiari FM. Local Oxygen Therapy for treating Acute Necrotizing Periodontal Disease in Smokers. J. Periodontol. 2006; 77:31-38.
4. Putt MS, Proskin HM. Custom Tray Application of Peroxide Gel as an Adjunct to Scaling and Root Planing in the Treatment of Periodontitis: A Randomized, Controlled Three-Month Clinical Trial. J. Clin Dent. 2012; 23:48-56.
5. Schaudinn C, et al. Manipulation of the Microbial Ecology of the Periodontal Pocket. World Dental. 2010 Feb-Mar; 2(1): 14-18.
6. Schaudinn C, et al. Periodontitis: An Archetypical Biofilm Disease. J. Am Dent Assoc. 2009 Aug; 140(8): 978-86.
Jeanne Bosecker, BSN, RDH, is a registered dental hygienist living in the northwest suburbs of Chicago. She completed a bachelor's degree in nursing, but found her passion in dentistry working as a dental assistant. She loves the day-to-day patient contact and takes every opportunity to educate her patients. She is currently working in two general dental offices six days a week. She is a three-time graduate of CareerFusion, a one-time RDH Under One Roof attendee, and a two-time delegate to the Illinois Dental Hygiene Association through her component the West Suburban Dental Hygiene Society. She can be reached at [email protected].
Hydrogen Peroxide
Hyperbaric oxygen therapy has been used in medicine to help treat poorly healing wounds in soft tissue and bone.3 An oxygen-rich milieu always inhibits the growth of anaerobic microorganisms, effectively supporting antibiotic and surgical therapy.3 In addition, an oxygen-rich milieu enhances the function of leukocytes, activating or supporting the body's local defense mechanisms in areas that are already frequently poorly perfused, which in turn speeds up the healing process.3
Hydrogen peroxide is a naturally-occurring substance made in the human liver, breast milk, and white blood cells as part of the body's immune response system. It is officially listed as an over-the-counter (OTC) oral debriding agent and oral wound cleanser. OTC concentrations of hydrogen peroxide (≤3%) come in liquid and gel formulations. 10% Carbamide (urea) peroxide breaks down into approximately 3% hydrogen peroxide and urea.
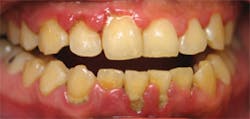
Patient presented with 100% BOP and 74% pockets measuring 4-7mm. Perio Tray delivery of 1.7% hydrogen peroxide gel was started, and full mouth debridement was completed a month later. Courtesy of Dr. Craig Buntemeyer.
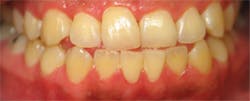
Appearance after four months during post-scaling recall visit. Courtesy of Dr. Craig Buntemeyer.
Image taken one week after full mouth debridement and four weeks of Perio Tray delivery of 1.7% hydrogen peroxide. No scaling completed at this point. Courtesy of Dr. Craig Buntemeyer.
Appearance after six months. Patient continued to use prescription Perio Tray delivery of 1.7% hydrogen peroxide gel (Perio Gel). Courtesy of Dr. Craig Buntemeyer.
Side Effects
The black hairy tongue is a rare side effect of rinsing with hydrogen peroxide. When use of hydrogen peroxide in confined to trays for periodontal therapy, the black hairy tongue is rare. Little information is available regarding hydrogen or carbamide peroxide use for teeth bleaching as causing this side effect.
The concentration of peroxide for adjunctive periodontal therapies should be low. Higher concentrations can have side effect of tooth sensitivity. For this reason, teeth bleaching agents that have much higher concentration of peroxides, ranging up to 35% in carbamide peroxide gels, are used in trays that keep the agents away from the gum tissue. These products are thus not advised for any periodontal therapy.1 When peroxide gels are used in lower concentrations in specially formed prescription trays that are designed to deliver and maintain the agents in the sulcus or pocket, (for example the Perio Tray with a 1.7% concentration of hydrogen peroxide), reports of sensitivity are minor4 and can be easily addressed with a fluoride product delivered with the special tray.
One well known side effect of peroxide use is tooth whitening. Patients using prescription tray delivery of low concentration of hydrogen peroxide products to treat gingivitis or periodontitis report whiter teeth. While these results are not as profound as whitening treatments relying on higher concentrations of peroxide, there are no food or drink restrictions with the 1.7% gel use as there are with high dose exposures, and the lower concentration is not as likely to cause sensitivity as the higher concentrations.1
Hydrogen peroxide in oral use is extremely safe. Toxic effects of hydrogen peroxide are noted for ingestion of the peroxide, not with topical use. With carbamide peroxide, few data are available. No significant deleterious genotoxic effects were observed in animals or mammalian cells.1 Acute toxicity was seen in rats at 5mg/kg of a tooth whitener containing 35% carbamide peroxide when given by gavage.1 A subsequent study indicated that carbamide peroxide-containing products were not genotoxic, nor were they any more toxic than dental materials currently in use.1 For oral uses not involving ingestion of the peroxide materials, toxicity does not appear to be a problem.
Past RDH Issues