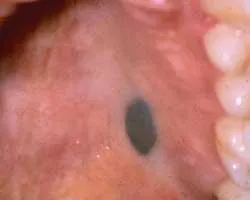
The blue nevus
by Nancy W. Burkhart, RDH, EdD
[email protected]
Your patient today is Mannie, a 25-year-old male who has recently moved to your city. He has not been in a dental office for a number of years because of frequent moves and the lack of dental insurance.
His health history is excellent with no medications other than over-the-counter medications for seasonal allergies. He consumes two to three beers on a daily basis. As you question him, he tells you that he noticed a blue area in the palate and asks about the lesion during the exam. After seeing recent advertisements regarding oral cancer, he was concerned and made the appointment for an exam (see Figure 1).
You note that the lesion he is concerned about on the palate is blue-black, measuring approximately 5x3x1mm. The patient does not know the length of time the dark area has been present, but noticed it himself about six months ago.
The patient is referred to an oral surgeon. A biopsy is performed and the pathology diagnosis is a blue nevus.
Etiology: The blue nevus is often referred to as the pigmented nevus, melanocytic nevus, or nevomelanocytic nevus. Nevi may be either congenital or developmental. The most common intraoral type of nevi is the intramucosal nevi followed by the blue nevi.
The blue nevus is usually asymptomatic, with color variations of gray, brown, slate-blue, and blue-black in color (Tyndall effect) and rarely measures over 6 mm (see Figure 2). In the early stages, the lesion may have characteristics similar to the deadly melanoma.
There is a genetic predisposition to the nevus in general, and the lesions are often seen on external skin surfaces, but they are uncommon intraorally. Several types or variants of the blue nevus such as the plaque-type blue nevus (Fistarol and Itin, 2005) and the epithelioid blue nevus (Pinto et al., 2003) versions have been documented in the literature.
Method of transmission: The nevus is not transmitted from one person to another in either external skin or intraoral forms.
Epidemiology: The intramucosal nevus is the most commonly occurring nevus in the mouth, followed by the blue nevus that accounts for 19 to 36% of all oral nevi. The blue nevus is most frequently discovered in young adults. However, literature on the subject indicates that the intraoral nevus occurs in all age groups. The blue nevus is most often found on the hard palate with the buccal mucosa being the second most common site. The intramucosal nevus is usually found on the buccal mucosa.
Pathogenesis: The nevus occurs from nevus cells in the epithelium, the basement membrane, connective tissue, or in combination from these sites. Depending upon the location in tissue layers, several classifications of a nevus are possible: the intramucosal type, the blue nevus, compound nevus, or junctional nevus.
The nevus originates from the proliferation of melanocytes. And within the classification of the blue nevus, several types are recognized and diagnosed by the pathologist:
- Common (most frequently occurring)
- Cellular forms
- Sometimes a combined nevus.
Common forms of the blue nevus are benign and rarely recur. Cellular forms may behave aggressively and may recur.
Perioral and intraoral characteristics: The blue nevus is well-circumscribed and slightly raised. The blue-black color of the lesion makes its appearance very noticeable when viewed in the palate. When found on the buccal mucosa, the possibility of an amalgam tattoo is more probable and must be considered. Radiographs will often confirm the presence of amalgam fragments.
Extraoral characteristics: Blue nevi occur on the skin of the hands, feet, and buttocks. Generally, all types of nevi occur externally on skin surfaces and are rarely found intraorally.
Distinguishing characteristics: The location is a key factor when found in the palate region. The smooth, circumscribed, and slate-blue color are also considerations. Microscopically, the blue nevus is readily diagnosed and classified with key characteristics. In all cases, a microscopic evaluation is needed to confirm a suspicion of a blue nevus.
Significant microscopic characteristics: Tissue specimens exhibit proliferation of oval-shaped and spindle–shaped melanocytes with dendritic extensions that are heavily pigmented. The cells are seen deep within the lamina propria and parallel to the surface epithelium (see Figure 3).
Dental implications: When a blue nevus is suspected, the clinician would remove the lesion because of the rare possibility of malignant transformation or confusion with the deadly melanoma. The lesion is always recorded and documented in a three-dimensional format such as 5x3x1mm. Intraoral photographs are an additional documentation for the lesion before removal.
Differential diagnosis: Several other lesions should be considered along with the blue nevus. Confusion may occur with satellite metastases from malignant melanoma; therefore, a correct diagnosis is crucial. Diascopy (using a glass slide with applied pressure) is beneficial to rule out vascular type lesions.
Additional considerations: Amalgam tattoos, malignant blue nevus, melanoma, Kaposi’s sarcoma, or hemangioma.
Treatment and prognosis: Surgical removal with histological evaluation is always performed with these lesions. The dental health-care provider may be the first and only person to recognize a blue, pigmented area in the mouth. Swift and accurate diagnosis is extremely important for the long-term health of the patient.
References:
Pinto A, Raghavendra S, Lee R, DeRossi S, Alawi F. Epithelioid blue nevus of the oral mucosa: A rare histologic variant. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2003;96:429-36.
Delong L, Burkhart N. General and Oral Pathology for the Dental Hygienist. Lippincott, Williams & Wilkins, Baltimore. 2007.
Eisen D, Lynch D. The Mouth: Diagnosis and Treatment. Mosby, St. Louis. 1998.
Fistarol S, Itin P. Plaque-type blue nevus of the oral cavity. Dermatology 2005;211:224-233.
Ojha J, Akers J, Akers J, Hassanein A, Islam N, Cohen D, Bhattacharyya I. Intraoral cellular blue nevus: Report of a unique histopathologic entity and review of the literature. Cutis 2007;80:189-192.
Neville B, Damm D, Allen C, Bouquot J. Oral & Maxillofacial Pathology. W.B. Saunders Company, Philadelphia. 1995.
Regezi J, Sciubba J, Jordan R. Oral Pathology: Clinical Pathologic Correlations. 4th ed. Saunders, St. Louis. 2003.
Fistarol S, Itin P. Plaque-Type Blue Nevus of the Oral Cavity. Dermatology 2005;211:224-233.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor in the department of periodontics at Baylor College of Dentistry and Texas A&M Health Science Center in Dallas. Nancy is also a co-host of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She is the coauthor of General and Oral Pathology for the Dental Hygienist.