Going the extra mile
Does subgingival irrigation help patients with gingivitis or periodontal disease? The answer depends on several factors. In this case, hygienist and patient persistence won the day!
Dianne D. Glasscoe, RDH, BS
Over the past few years, various studies have been conducted to determine the effectiveness of subgingival irrigation for patients with gingivitis and/or periodontal disease. For example, in an article titled "Mechanism of Irrigation Effect on Gingivitis," in the November 1994 issue of the Journal of Periodontology, the author stated that, when used consistently, oral irrigation:
(1) Improves breath
(2) Eliminates gingivitis
(3) Removes toxins from gingivitis
(4) Reduces bacterial concentration
Since gingivitis does not include loss of bone, pathogens that cause inflammation are easily accessible. However, in situations where bone loss has already occurred and periodontal pockets have formed, would irrigation be beneficial for these patients? We know that pathogens that elicit the inflammatory response reside deep in the sulcular areas where toothbrush or floss will not reach. These pathogens require an anaerobic environment to survive. Can these same pathogens be brought under control when they are attacked daily by a suitable irrigant, as well as a delivery method that places the irrigant where the pathogens reside?
What follows is an irrigation success story about a patient I have been able to follow over a 13-year period.
This is not meant to be a scientific study. However, the results for this particular patient with periodontal disease have been truly amazing and certainly worth sharing.
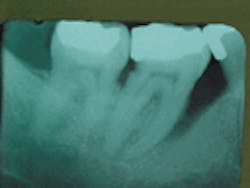
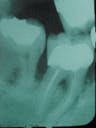
When Mr. Davis first came to our office in 1987, he had a 6 mm pocket on the mesial of tooth #30. Radiographs showed evidence of caries on the distal of the tooth. The patient was subsequently referred to a periodontist for evaluation.
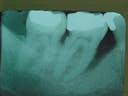
In early 1988, a tri-calcium phosphate bone graft was done on #30 at the mesial and in the furcation. The radiograph shows excess graft material at the margin that was later reduced to a more acceptable height. The patient returned to our office with no sign of disease and a 3 mm pocket at #30 mesial.
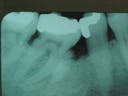
In 1989, I made the decision to stay at home with my children, so I lost contact with Mr. Davis. However at his recare visit in 1991, slight evidence of graft deterioration is visible. In the interim period between 1989 and 1991, he had undergone endodontics and had a PFM crown placed on the tooth.
At this visit in 1993, further evidence of graft breakdown is evident.
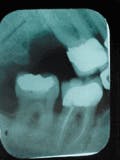
In 1994, I returned to private practice on a part-time basis, and I saw Mr. Davis early in 1995. At this visit, I asked if he was experiencing any dental problems. He told me that when he pressed his right cheek with his hand, he felt pain. When I retracted his right cheek, I saw that the area around #30 was severely inflammed. Suppuration and tissue tenderness were obvious. However, the tooth did not hurt on percussion, nor was it mobile. The radiograph revealed that the bone graft that was placed in 1988 was completely obliterated. Probing at #30 mesial was 11 mm. Upon examination, the doctor recommended immediate extraction. This patient had done everything possible to save this tooth, and now it appeared that we were out of options.
Mr. Davis was not happy! He exclaimed that he had spent a small fortune on this tooth and did not want to have it extracted. He reiterated that his tooth was not loose, and he still could chew with it. He felt that there must be something else that could be done. Mr. Davis was not going to give up this tooth without a fight!
One final try
Suddenly, it occurred to me that there might be one more thing that we could try ... and that was irrigation. Two months earlier, a speaker - Dr. Larry Burnett - had shown some slides of presumably hopeless teeth that had been saved through daily home irrigation and frequent preventive care.
I explained to Mr. Davis that there was something we could try, but there were no guarantees it would work. With a plastic syringe and irrigating cannula, I then demonstrated how he should insert the irrigating cannula into the mid-lingual and mesial aspects of tooth #30 and flood those areas with chlorhexidine. I was adamant about emphasizing to Mr. Davis that this needed to be done every day without fail!
One month later, Mr. Davis returned for a tissue check. Before he sat down in the chair, he told me that his cheek no longer hurt when he pressed against it with his hand. I was pleasantly surprised to see that the tissue was much less inflammed and generally looked better. No suppuration was evident.
Mr. Davis told me he had faithfully irrigated this area twice each day. When the doctor checked Mr. Davis, he was cautiously optimistic about his improvement. Based on the progress, we decided to stay the course for two more months. I gave Mr. Davis another plastic syringe and irrigating cannula - he had worn the other one out!
Two months later, still more improvement was evident. The tissue appeared pink and firm, even though the defect in the bone was very deep. I decided to debride the area with the ultrasonic scaler using a Slim-Line tip. We decided at this point to switch the irrigant from chlorhexidine to Listerinea and set his recare visit at three months.
In three more months, the area appeared to be stable with no inflammation or suppuration and only slight bleeding at probing. The pocket measured 9 mm.
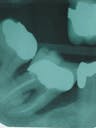
In 1997, the radiograph showed something amazing - the formation of new bone in the furcation and at the base of the pocket. Never in our wildest dreams did we expect to see this!
In 1998, the radiograph showed the area to be stable.
The key to success
The traditional home-care methods (such as brushing and flossing) do not address the problem of periodontal pathogens that reside in deep sulcular areas. Actually, supra-gingival plaque control is of little value in treating established periodontitis.
However, in this particular case, we were able to devise a method of delivering the irrigant to the base of the pocket. By using a plastic syringe with an irrigating cannula, the patient was able to flood the entire bony defect and reach the most remote crevices of the pocket.
I believe the major reason for success was patient compliance. Part of his motivation came from the fact that he had invested a considerable sum of money in retaining this tooth - i.e., bone graft, endodontics, and a crown. But even without the monetary considerations involved, I think he still would have been compliant simply because we had a great rapport. It is a fact - if your patients like and trust you, they are more likely to do what you ask of them.
Granted, what I asked him to do was not an ordinary task. Thankfully, his manual dexterity was adequate to carry out the task of subgingival irrigation. Even though it was not an anterior tooth, it was fairly accessible.
As dental professionals, we possess exceptional dexterity in maneuvering small, sharp instruments in the oral cavity by virtue of our clinical and educational experience. However, what may seem like a small benign task to us may be extremely difficult to a patient.
For example, I remember a woman who had an isolated 11 mm pocket at #22 mesial. This was certainly an easily accessible area. However, this patient related to me that she "couldn`t stand the thought of sticking a needle in my gum." She could not grasp the concept of the space between her tooth and the side of the gum being a hiding place for periodontal pathogens. Neither would she agree to go to a periodontist for treatment.
Another factor that contributed to Mr. Davis` success was his understanding of the problem at hand. I took time to explain the bone loss, the action of the "bad bugs" living in the pocket, and the ineffectiveness of traditional methods of plaque control. What I presented to him was a logical way of controlling those pathogens over a period of time, thereby bringing the inflammatory response under control and eliminating the infection. Mr. Davis took possession of his disease.
Mr. Davis basically has a healthy pocket. After all, we should consider that a pocket is merely a scar in the bone left from the destructive action of the host resistance in response to virulent pathogens. He has gained several millimeters of attachment, going from 11 mm in 1995 to 6 mm now. The new bone that is evident on the radiograph far exceeded my expectations. My goal was merely to bring the infection under control and retain the tooth. However, our anti-infective therapy has been quite successful in this case.
At present, the patient is irrigating every other day with a diluted Listerine solution and is maintaining well. He is being seen for professional care every four months, and the pocket and furcation are debrided with Slim-Line ultrasonic inserts on medium power.
Types of irrigants
Many offices are privileged to own irrigating devices that allow the clinician to cool the ultrasonic tip with something other than water. This allows the pocket environment to be debrided and disinfected at the same time.
Also, many different types of irrigants have been tested. An article titled "Povidone Iodine`s Effects and Role in the Management of Periodontal Disease: A Review," states, "There is evidence to indicate that povidone iodine delivered via an ultrasonic device achieves better results in deep pockets than ultrasonic debridement when water is the irrigant." Povidone iodine is a safe antiseptic that does not appear to impede wound-healing or induce resistant bacteria.
Some clinicians report good results with chlorhexidine, Listerine, or salt water irrigation. Others like the stabilized chlorine products, such as Oxyfresh.
The success or failure of any irrigant probably has to do with exactly what pathogens are at work in the pocket and the patient`s ability to irrigate effectively and consistently over a period of time.
In everyday practice, we may not have the systems in place to do a culture. However, we do have the freedom to try another irrigant if what we are using does not seem to be working. A simple one-time office irrigation probably does little to control established periodontal disease.
A final thought
It is an established fact that periodontal disease is site-specific and progresses in bursts of activity and periods of quiescence. It is in the active stage when supporting structures are destroyed. It has been speculated that the bursts of activity may be triggered by a dip in the patient`s host resistance. Some factors that contribute to decreased host resistance are stress, physical illness, and lack of proper nourishment and/or sleep. Also, certain systemic changes related to glandular function can cause changes in the host immunity.
While it is not always possible to pinpoint the contributing factors in our patients` lives that lead them down the periodontal-destruction path, we can increase their professional care by instituting shorter recare intervals and utilizing site-specific treatment modalities when possible. Patient dexterity and compliance always will be issues. However, subgingival irrigation should be considered as an additional weapon in our arsenal against periodontal disease.
For those motivated patients who are willing to establish a partnership with their hygienists and comply to the letter with the required home-care therapy, the rewards can be quite fulfilling!
Dianne Glasscoe, RDH, BS, is a writer, speaker, and consultant based in Lexington, N.C. For more information, visit her Web site at www.professionaldentalmgmt.com.
1987
1988
1991
1993
1995
1997
1998