‘Double teeth' leads to differential diagnosis
by Nancy W. Burkhart, RDH, EdD
[email protected]
Jason, a 15-year-old high school student, is a new patient in your office and is scheduled for an exam and prophylaxis.
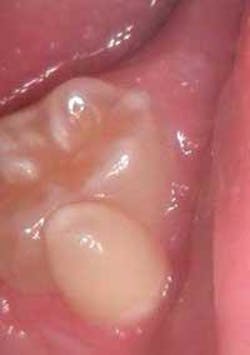
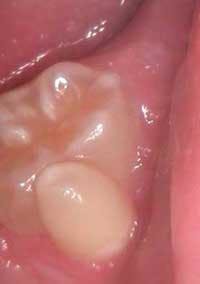
Jason is a healthy teenager with no complaints, and his health history ends with no significant findings. As you examine his mouth, your attention is drawn to his left, second mandibular molar #18 (see Figure 1). You ask Jason if anyone has mentioned the small cusp on the facial side of his molar. He tells you that he is aware of the tooth. His mother, who is with him, states that a previous dentist had questioned her about some multiple deciduous teeth that were discovered during an exam years ago. However, she did not have any other details on the dentist's prior questions; nor was the current tooth in question a concern at that time.
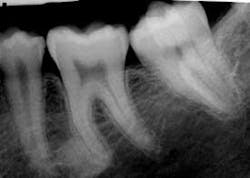
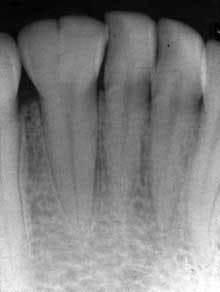
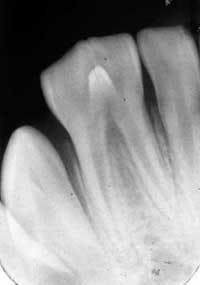
As you take his radiographs, you also make a PA of the tooth (see Figure 2). You confer with the dentist, to determine her opinion concerning the etiology of the odd molar. As you both view the clinical slide and radiograph, the diagnosis is unclear. You are confused about whether a separate root system is present.
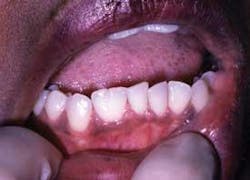
Figure 1: Clinical slide of tooth #18 with additional adjoining tooth in question. Photo courtesy of Kathryn Jendrasik-Savitsky, DDS. Figure 2: The radiograph vaguely supports two separate root canal systems. Also noted in the radiograph is a small focus of dense, radiopaque bone between the bicuspid and the first molar. This was diagnosed as “as a small zone of idiopathic osteosclerosis.” Photo courtesy of Jessica Huffman, RDH. Figures 3, 4: Gemination. Photos courtesy of Lippincott Williams & Wilkins from “General and Oral Pathology for the Dental Hygienist.” and Dr. Harvey Kessler. Figure 5: Fusion. Photo courtesy of Lippincott Williams & Wilkins from “General and Oral Pathology for the Dental Hygienist” and Dr. Harvey Kessler.
Since you can see two crowns clinically, there are several possible findings. You are able to make a differential list of considerations, and the most likely findings would be gemination, fusion, a supernumerary tooth, concresence or an accessory cusp. Or, another possibility would be a combination of the above mentioned items.
Differential diagnosis: Considerations for this case would include:
• Gemination — In gemination (see Figures 3, 4), a single-tooth germ tries to produces two teeth. The root system appears as one and then the tooth splits as the two crowns become visible. In other words, two crowns appear to arise from a single root. The maxillary incisors are most commonly affected. The incidence is dramatically decreased in the molar region, and a hereditary tendency is noted. The terms “twinning” and “double teeth” have been noted in the literature as well.
• Fusion — Fusion (see Figure 5) occurs during dentinal matrix formation, and two tooth buds are joined at the crown. The root systems are separate and the tooth count indicates that a tooth is missing. Since the correct number of teeth appears present in this case, fusion could be a possibility if the tooth in question is really a third molar.
A familial tendency occurs in only 1% of the population. Just to add more confusion, the tooth in this case does not clinically appear as a molar. The other possibility is that the visible tooth is a supernumerary tooth (a “paramolar”) in this particular case. This would mean that a supernumerary tooth is fused to the second molar. Paramolars are supernumerary teeth situated lingually or buccally to a molar tooth.
• Concrescense — Concrescense is very similar to fusion, but the teeth are joined at the root surface by an overproduction of cementum. It's usually found in the maxilla more often than the mandible. The tooth in question appears to be joined by the crown as well and not limited to the root area. Since the tooth in this case appears to be fused to the crown as well, concresence may not be likely.
• Accessory cusps — The cusp of Carabelli is found on the maxillary first molars on the palatal surface of the mesiolingual cusp.
Talon cusps are located on the cingulum area of an incisor or canine tooth extending to at least half the distance from the cemento-enamel junction to the incisal edge.
Doak's cusp is normally located on the facial surface of maxillary molar teeth.
Dens evaginatus is normally located in the central groove on the occlusal surface of posterior teeth or root and is lined by enamel. Premolars are affected most often with molar teeth being only occasionally involved. Mandibular teeth are affected more often than maxillary teeth.
Accessory cusps are not supported by the radiographic findings in this case. But, clinically, due to the shape of the tooth in question, this would be a possibility in only a clinical inspection. The tooth is noted and merely monitored when the diagnosis is accessory cusp. In the case of accessory canals such as Doak's cusp, there is a risk of caries in the grooves of the cusps where they join the abutting tooth. A pulp horn often extends into the cusp and this could make any restorative efforts difficult.
Perioral and intraoral characteristics: The intraoral characteristics and the tooth anatomy vary with the location of the gemination or fusion. In the case presented, the tooth in question that is on the labial of #18 is peg-like and certainly not the usual anatomy of any of the teeth in the patient's mouth. Gemination has a propensity for the maxillary incisors and decreases in occurrence from the anterior to the posterior. Fusion usually affects the incisors.
Significant radiographic features: Radiographic diagnosis is the key factor in distinguishing gemination and fusion, and a variety of appearances may be noted in both gemination as well as fusion. With gemination, the root canal system will appear normal, but will split as it moves toward the crown.
The pulp chambers may appear noticeably large. In this case, the pulp chamber does appear somewhat separate (see Figure 2). Also noted in the radiograph is a small focus of dense, radiopaque bone between the bicuspid and the first molar. This was diagnosed “as a small zone of idiopathic osteosclerosis.”
Discussion: This case was unusual in that the diagnosis is not as clear as we would like to see in the dental community. Two oral pathologists, one radiology specialist, one general dentist, one dental educator, and two dental hygienists reviewed the case. The case caused considerable discussion, and the final consensus was that this was probably a small supernumerary tooth (a paramolar) that was fused to the second molar.
Sometimes dental terminology and definitions can be difficult to apply accurately in all situations. In this particular case, the third molar is not evident in this 15-year-old, and the tooth in question does not appear to be a third molar based on the clinical appearance of the tooth.
The crowns appear to be separate, the root canal system appears separate, and the tooth appears fused to the second molar.
Technically, the definition of gemination requires the tooth count to be normal when the tooth in question is counted as one tooth. In this case, since the third molar is not present, the definition for gemination is fulfilled as well. However, also with the definition of gemination, the teeth would share the same root canal system. In this case, that aspect is in question since the radiograph vaguely supports two separate root canal systems.
Conclusion: Although this case is very interesting, sometimes all entities do not fit a neat final diagnosis. This case brings to mind the concept of Occam's razor for those with an interest in philosophy. Sometimes the simplest idea is the best with as few assumptions as possible.
Upon initial inspection, gemination was thought to be the diagnosis. However, on closer inspection, other considerations became apparent. This is one of the cases that does not clearly conform to all “textbook” findings. Sometimes, “double teeth” may be the better diagnosis, rather than neatly trying to fit this finding into a clear set of terminology — particularly since the treatment would be the same (just monitoring the affected area).
Likely diagnosis: The consensus was that this was most likely a supernumerary tooth (a paramolar) that was fused to the third molar. The patient will be monitored to assess the development of a third molar.
Finally, keep listening to your patients and asking good questions!
References
Delong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. First Edition. 2008. Wolters Kluwer, Lippincott Williams & Wilkins.
Grammatopaulos E. Br Dent J. Aug 11 2007, 203:3.119-20.
Neville BW, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. W.B. Saunders Co. 1995.
Langlais RP, Miller CS, Nield-Gehrig JS. Common Oral Diseases. 4th Ed. 2009. Wolters Kluwer, Lippincott Williams & Wilkins.
A special thank you to:
Kathryn Jendrasik-Savitsky, DDS, Charlotte, North Carolina
Jessica Huffman, RDH, Charlotte, North Carolina
Brad W. Neville, DDS, Charleston, South Carolina
Harvey Kessler, DDS, Dallas, Texas
Leslie DeLong, RDH, MHA, Beaumont, Texas
Terry Rees, DDS, MS, Dallas, Texas
About the Author
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and co-host of the International Oral Lichen Planus Support Group http://www.bcd.tamhsc.edu/outreach/lichen/ and coauthor of General and Oral Pathology for the Dental Hygienist. Her Web site for seminars is www.nancywburkhart.com.