Monster in the Shadows
The painful presence of carpometacarpal arthritis of the thumb
by Colene W. House, RDH
There's a monster out there, lurking in the shadows ... waiting for just the perfect moment to pounce on any unsuspecting hygienist or assistant, stripping her of the ability to perform her daily duties. This monster has a name — many names actually, just as other mythical monsters such as Big Foot, El Chupacabra, and the Loch Ness Monster. But this monster is no myth. It's very real and afflicts many hygienists, coming on very quietly until, alas, it is too late to recover. This monster is known among hand specialists as carpometacarpal arthritis of the thumb, or in layman's language, arthritis of the base of the thumb.1
Can surgery be performed to correct this problem? Sure. But here's the catch ... fine motor skills are gone. The ability to grip a scaler and use it with precision is gone. Along with that loss goes the ability to continue in the clinical field of dentistry. This in itself can be totally devastating for any hygienist who truly loves her job. I know this for a fact, for I am one of those unfortunate hygienists who has been affected by this particular monster.
What causes this type of arthritis? According to many of the articles that are available, not much is known about the true cause.2,3 What are the predisposing factors? One theory is a hypermobile joint at the base of the thumb. Or perhaps there was an incident involving an injury such as a sprain or fracture in the past.2 Joint stress, heredity, muscle weakness, and repetitive motions play a large part in the development of this type of arthritis.1
Another observation is that the primary form of arthritis of the base of the thumb is most common in women over 40.3 According to my hand specialist, it is fairly common among long–practicing dental hygienists. The constant pinching action that a hygienist applies at the tips of her fingers transfers up to 10 times its force by the time it reaches the base of the thumb.6 In other words, one pound of pressure applied at the tips of your thumb and forefinger equals 10 pounds of pressure at the base of the thumb. That's a lot of pressure! There's no telling how much pressure we apply during the course of a day's work, often for several minutes up to more than an hour at a time. Imagine a mortar and pestle, grinding herbs or chemicals, and you will have a basic idea of the shape and actions of the bones in the base of the thumb. The constant grinding that occurs when one is gripping a scaler while attacking some hard deposits of calculus day after day is going to take its toll. Gradually, the cartilage that cushions the joint is worn away.3
The most common and early symptom that occurs is pain at the base of the thumb when grasping or pinching an object such as opening a jar or turning a key.5 In our case, instruments are the objects. Also, swelling and tenderness at the base of the thumb can occur.1 Looking back, the first symptom I noticed was a soreness when I would attempt any act of placing my hands on a flat surface while attempting a push–up, the Yoga position such as "downward facing dog," or "the plank" in Pilates. I also noticed weakness in my hands after a particularly tough day of scaling teeth, a day when I am left wondering if anyone flosses his or her teeth! Other times, I would be turning the steering wheel of my car and would get a sharp pain radiating up from my wrist. The symptom that got my attention was soreness in the muscle at the base of my thumb. Thinking that this was a sign that I was wearing the wrong size of surgical gloves, I spent at least two years looking for a better–fitting glove. I tried a cortisone shot, which worked great for about three months, only to have the symptoms return. That's when I finally got an appointment with a hand specialist.
Let's go a bit further back in time for a moment. Several years ago, probably around 1986, I began feeling a numbness in my right hand. Having no knowledge of the symptoms of carpal tunnel syndrome, I went for three years thinking I was just feeling the effects of gripping too hard while scaling. I would sit back and have a brief chat with my patient, masking the fact that I was shaking my hand back to life behind my back. I'm not sure when I finally heard of the symptoms of CTS, but believe me, a light of recognition blinked on in my brain. I did my homework by picking the brains of the surgeons who came in as patients to find out who would be the best one to handle the surgery. The answers I got were collective.
The surgery was very simple and the local orthopedic surgeon would be able to handle the CT release without any difficulty. So in December 1989, I finally had the surgery done. The recovery time would be six weeks. Six weeks! How would I help pay the bills that were due, buy groceries, and take care of our children's needs without putting a strain on our household? My husband was already working two jobs. True to form, my husband offered total support, calmly stating that God hadn't let us starve yet. Surely we would find a way through this together just as we had weathered other storms and bumps in the road of life.
On the other side of the story, what would happen at work? My boss was just as supportive. He even created a position for me as "office assistant." He figured that surely I would be able to develop X–rays, pull charts, help answer the phone, and anything else that needed doing with one hand. Believe me, was I ever grateful! Through the whole ordeal, I knew that I would eventually be able to return to my duties within six weeks.
It was still scary sitting down with my first patient after the surgery. In the back of my mind, I was scared silly that I might slip. Even though I had been doing my exercises diligently to strengthen my hand, I still could not make a good fist. Time was up; it was time to go back to work as a hygienist. So, with lots of trepidation, I picked up the instruments and miraculously my hand performed just as it used to. Only later would I find that I had lost the strength to split wood. But hey, I didn't want to do that anyway! And sadly, I found that it was painful to play the piano. Trying to reach the large chords was just not comfortable anymore. Playing the piano had been a major part of my life since I was 5 years old. Eventually, I sold my piano, a baby grand that I had bought for myself in celebration of graduating from dental hygiene school. It was a sad parting, but there were other things I still had that I held near and dear to my heart. One of those things was the ability to clean teeth and to continue in a field that I love and felt that I was pretty good at. By this time, I had been a hygienist for almost 20 years.
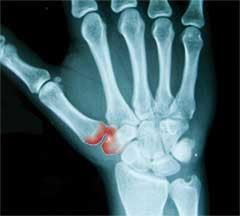
Now here I am again, faced with the inevitability of having to turn away from the security of being able to make a living, save for retirement (which was not supposed to be for another 10 years), and then be able to travel comfortably with my husband when I do retire. Standing there with my doctor looking at my X–rays, he asked me that dreaded question: "Do you plan on retiring soon?" I bravely answered that I wanted to work chairside until I was at least 60. "You're not going to make it," he replied. I felt the ground slip away from under my feet. I was like a child being dropped off at kindergarten on the first day of school, clinging to my mother's skirt. Looking up into her eyes, I was silently begging her not to leave me in this strange, new place. I didn't want to be left there by myself! But pride wouldn't let me show my despair.
It wasn't until later as I was describing to my husband what had happened at the doctor's office that I finally broke down. How could this be happening again? Not now! I'm just hitting my stride, still learning new things, still having fun, and heck, I'm finally getting the hang of digital X–rays! I'm only 56 years old. Far from considering myself old, I'm not nearly ready to hang up my scalers. I have patients who have come to depend on me to be there, to take care of them, to laugh with them at the corny jokes we tell each other, or to cry with them when life isn't going so well. These people have become my friends over the last 20 years or more. I ask you, what better job can you have when your friends come to see you every day ... all day long?
The next day I went in to work. I had told my boss that I would be going to the hand specialist, so the first thing he asked me that day was how things went. I didn't want to tell him, basically because I couldn't trust myself to hold it together. Finally I agreed to go to lunch with him to tell him of my hand specialist's prognosis. I think he was as devastated as I was. In his eyes, I was supposed to be a part of his team for many years to come. Ultimately, the decision was made to go to a part–time schedule. Surely, working in clinical dentistry just two days a week will prolong the necessity of having to make that final leap into the unknown. I never knew that reinventing myself would be so scary. Every so often the monster in the shadows sneaks up on me and I have a meltdown — scared, because I can't see the future as clearly as I used to, and intensely sad to lose a part of my life that was as comfortable and loved as a favorite pair of jeans.
As a seasoned hygienist with close to 37 years under my belt, what changes would I make in the way I practice dental hygiene? A few. I would be absolutely adamant about not working with dull instruments. Instead, I would make sure I had a sharp set (or three or four) at the ready. The very second you feel that an instrument is not effortlessly effective, put it down! The more dull an instrument is, the more tightly you have to grasp it. Ultrasonics? Oh, absolutely, use them as often as you can. But remember, there will be patients who just cannot tolerate them. Even when I use ultrasonic scalers, I always go back with hand scalers to double–check myself. Call me old–fashioned, but I feel that my tactile sensitivity is better with a light grip on that scaler. Large–handled instruments are an absolute must. I wish they had been around far longer than they have been! Believe me, I was happy to get them, especially after going through carpal tunnel surgery. My hand surgeon recommended taking breaks during the day by doing other duties around the office. This is a great idea, but as we all know, we feel pressure if we are not being "productive" every moment of the day.
At this point in time, I am still working chairside, but only two days a week. The other two days I am learning about the administrative side of our practice, slowly segueing over to the front desk. I am also learning the new skill of reimaging smiles (which is way cool!) on our Dentrix software for patients who are hesitant to begin any cosmetic treatment to change their smiles. But my heart will always belong in clinical dentistry. After all, I have spent the last 36 years refining my skills, caring for patients, truly loving what I do. Being the optimist that I am, I'm forcing myself to see this change as a door opening instead of a door closing. I will take this time to educate others out there about what carpometacarpal arthritis of the thumb is, and what its symptoms are as I remember them, as well as researching any possibility to prevent it. And so ... I write.
I can only look forward now ... no furtive glances over my shoulder, knowing the monster is there, silently hiding in the shadows behind me. But being the strong–minded woman I am, I am determined to prevail. I will somehow find a way to stay involved in dental hygiene — the world that I love and of which I am so intensely proud to be a part.
References
1 MayoClinic.com. Tools for healthier lives. Section 1 Thumb Arthritis, March 31, 2006.
2 Mayo Clinic.com. Tools for healthier lives. Section 3, Thumb Arthritis, March 31, 2006.
3 American Society for Surgery of the Hand, Arthritis of the Base of the Thumb. Who gets arthritis at the base of the thumb? Nov. 28, 2007.
4 MayoClinic.com. Tools for healthier lives. Section 4 Thumb arthritis, Risk factors, March 31, 2006.
5 MayoClinic.com. Tools for healthier lives, Section 2 Thumb arthritis, Causes, March 31, 2006.
6 Osteoarthritis, 4th Edition, Diagnosis and Medical/Surgical Management, Section IV: Surgical Considerations in Osteoarthritis, By Roland W. Moskowitz, Roy D. Altman, Marc C. Hochberg, Joseph A. Buckwalter, and Victor M. Goldberg.
About the Author
Colene W. House, RDH, is a 1971 graduate of Central Piedmont Community College in Charlotte, N.C. She has spent the majority of her time in clinical dentistry, and has helped design soft–tissue management programs for the offices where she has worked. Being actively involved with the Eblen Foundation Sealant Program, House helps to provide free sealants for first– and second–grade children from schools throughout the county in the dental clinic at Asheville–Buncombe Technical Community College. After 36 years in dentistry, House now pursues her love of writing. She may be contacted at [email protected].