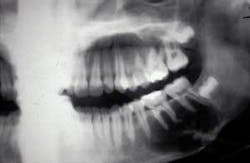
Traumatic Bone Cyst
By Nancy Burkhart, RDH, EdD
Jonathan, a 15-year-old male, is a new patient. He is in for a routine appointment and has not been seen for a dental appointment in more than two years. Jonathan is on the wrestling team at the local school and competed in a national tournament with his school approximately one year ago.
He explains that he took a hard blow to the mandible during the tournament, and he has complained of a dull pressure sensation in his mandibular region for a few weeks. He was evaluated by the sports medicine providers at the event and was told that there did not appear to be any ill effects except for some bruising.
Jonathan is in good health, works out at the school gymnasium, and claims to eat a healthy diet supplemented by multiple vitamins with protein shakes.
In order to establish a permanent record for Jonathan, you proceed to first examine his mouth and take a full-mouth set of radiographs. The intraoral exam results in an area of concern for you since the right apical areas of the molars appear to be somewhat elevated. The radiographs that you subsequently take reveal a true area of concern in the mandible.
The related radiograph depicts a radiolucent lesion around the mandibular molar teeth extending from the second premolar to the distal of the second molar. The border of the radiolucent lesion may be described as scalloped and reaching to the inferior border of the mandible. The scalloping in between the roots follows the nature of the traumatic bone cyst.
Diagnosis: Traumatic bone cyst
Etiology: The traumatic bone cyst may also be called the simple bone cyst. Trauma is the usual cause of this type of cyst and as stated in the case above, a blow to the region in question is usually reported by the patient. This cyst does not have a true epithelial lining and is not considered a true cyst, but rather a pseudocyst.
Epidemiology: The traumatic bone cyst is usually found in the 10 to 20 year age range, but they may occur in any age group. There is no gender predilection. Since most contact sports with high impact involve males, the odds of being affected by trauma may be greater in males. Most commonly, the mandible is the site of the cyst.
Pathogenesis: Pooled blood is found in the cavity and may be released when the lesion is opened. The cyst is thought to be a hematoma, which is caused by the initial trauma and ultimately liquifies. Another implication of the etiologies that have been suggested is the possibility of a calcium deficiency in some individuals.
Extraoral characteristics: Some swelling may occur if the size of the lesion is large enough to cause expansion of the tissue.
Perioral and intraoral characteristics: Pain is usually not reported by the patient and the traumatic bone cyst may be routinely found during a Panorex or intraoral radiograph examination. The cyst exhibits scalloping with very sharp margins that may extend in between the teeth. The lesion may also have the characteristic “soap bubble” appearance of other cysts such as the ameloblastoma.
Distinguishing characteristics: When the cyst is opened, the lesion is found to be blood-filled in a liquid form. With the drainage and release of blood, the lesion can begin to heal with bone formation.
Significant microscopic features: Blood and bone are the composition of the traumatic bone cyst. No epithelial lining is present, which helps in differentiation when viewed microscopically.
Dental implications: The lesion that is detected early may be small in size and easily managed. However, if undetected, the lesion may have expanded, covering a large area of bone and tissue. The larger lesions may take much longer to heal.
Differential diagnosis: Depending upon the location, various types of cysts may be suspected along with florid cemento-osseous dysplasia. A true confirmation is usually made by submitting a small tissue sample of bone and blood from the wall of the cyst for a definitive diagnosis.
Treatment and prognosis: Recurrence is very rare, once the lesion is drained and curetted. Over time, the bone will fill in the cavity and return to a normal state. Since Jonathan is in a contact sport, he may suffer other injuries and may damage the same site again. Depending on where the lesion occurs, protective mouth wear or protective headgear may offer some additional benefit.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor in the Department of Periodontics at Baylor College of Dentistry and Texas A & M Health Science Center in Dallas. Nancy is also a co-host of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She is the co-author of General and Oral Pathology for Dental Hygienists, published by Lippincott Williams & Wilkins in Baltimore, which will be released in October 2007. She can be contacted at [email protected].
References:
Dvori S, Shohat Y, Taicher S. Simple bone cyst in the mandible: A rare occurrence in an elderly patient. Refuat Hapeh Vehashinayim 2006;(1):27-30, 69.
Neville BW, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. 2nd ed. Philadelphia: WB Saunders, 2002.
Regazi J, Sciubba J, Jordan R. Oral Pathology-clinical pathologic correlations, 4th ed. St. Louis: WB Saunders, 2003.
Sciubba JJ, Fantasia JE, Kahn LE. Atlas of tumour pathology: tumors of the jaw. Third series. Fasciole 29, Washington DC: AFIP, 2001:49.
Shear M. Cyst of the oral regions. 3rd ed. Oxford, Wright, 1992.