Endoscopy dreamin’
As many of you know, I live in Georgia. Yesterday was a gloomy, rainy day, so I decided to watch a movie that is considered a “sleeper.” “Midnight in the Garden of Good and Evil” was filmed in Savannah, Ga., at Christmastime. Regarded as “The Belle of the South,” the port city of Savannah exemplifies antebellum grandeur complete with ornate architectural details and public squares with sprawling oaks draped with Spanish moss.
The movie’s appeal to me was the photography and the wonderful characters that include well-bred ladies and gentlemen, and a voodoo priestess who works her magic at a local graveyard. The movie is basically a “whodunit,” and much of the plot revolves around the death of a young “redneck” local. A writer comes to town to try to unravel the truth, and spends many late nights at the graveyard with the voodoo priestess. She warns him not to become obsessed with death and advises, “Don’t commune with the dead so long, you might forget how to live.”
Who among us has been a part of mediocrity for so long that we’ve forgotten what’s best for patients? How many of us are goal-oriented and remain focused on what’s important in the services offered to patients? Are you practicing in the way you once dreamed of, or are you practicing at what you don’t want to become? Are you content with the tools that are provided to you to get the job done, or are you continually frustrated with having to beg for modern equipment and technologies?
“Want a dream job?” That’s what I was asking after visiting the periodontal practice of John Kwan, a periodontist in Oakland/Berkeley, Calif. Do you want to be practicing technology-enhanced, evidence-based nonsurgical periodontal therapy with an employer who is totally supportive of this goal? I already knew quite a bit about Dr. Kwan’s commitment to excellence in the nonsurgical treatment of periodontal infection, so I was excited to learn more and “shadow” him and his team for a day.
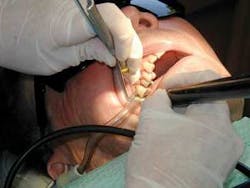
On the day I visited, Dr. Kwan and two hygienists, Mari and Kris, were scheduled to see patients. I was immediately drawn to Kris’ operatory, mainly because she was booked to perform periodontal endoscopy-enhanced nonsurgical periodontal therapy from 8 a.m. to 1 p.m., whereas Mariwas scheduled to see periodontal maintenance patients. Kris (Kristine Wood, RDH) was very friendly and welcomed my intrusion (with digital camera in hand) into her bright and sunny operatory. Even Dr. Kwan’s wife, Deborah, popped in to say hello while tending to the beautiful potted orchids that adorn each operatory.
In between shadowing Dr. Kwan and Kris, I viewed microsurgical videos and watched a fascinating one of a connective tissue graft performed to treat damage from oral piercing. About 70 percent of Dr. Kwan’s practice is dedicated to different types of surgery, and about 50 percent of the surgery is devoted to implant placement.
Kris, Mari,and Dr. Kwan use a manually-tuned ultrasonic unit with a variety of precision-thin ultrasonic inserts that Dr. Kwan refers to as “micro ultrasonic”inserts. Don’t expect to see any hand curettes on their instrument trays. Dr. Kwan and the team rely exclusively on micro ultrasonic inserts to remove biofilm and calculus, and they combine microultrasonic instrumentation with periodontal endoscopy to magnify the root surface. Micro ultrasonic inserts, including diamond-coated inserts, come in various shapes and sizes to reach inaccessible areas such as furcations and root grooves.
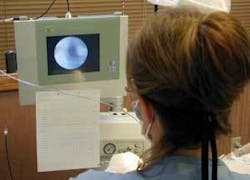
Kris is incredibly enthusiastic about scope-enhanced nonsurgical periodontal instrumentation. She describes the endoscope’s function as “striking gold,” and insists that clinical outcomes can’t be compared with and without the endoscope. “Being able to see on the roots of bicuspids and molars makes all the difference,” she said. “You can see how much you need to position the insert to maximize calculus removal.” One striking point Kris made while I was watching was, “Seeing is believing, that’s for sure!” After spending a full day observing Kris, Mari and Dr. Kwan, I admit that I, too, believe that nonsurgical periodontal instrumentation without a periodontal endoscope is incomplete.
Kris, Mari and Dr. Kwan insert the endoscope (a probe with a camera attached) with their left hand and the ultrasonic insert with their right hand. They position the endoscope subgingivally while instrumenting with the right hand, and it all seems so easy as they instrument and view at the same time! Kris confessed that it took her weeks of continuous use to become proficient with the endoscope. A two-handed technique (probe in one hand and micro ultrasonic insert in the other) for full or split mouth can be accomplished in 90 to120 minutes.
Most of the subgingival calculus does not show up on radiographs, and many studies show that anywhere from 17 and 69 percent of root surfaces show some residual calculus.1 So, you ask, why do we need to remove as much subgingival calculus as possible? Subgingival calculus may or may not be harmful in some instances, but its presence as a foreign body in association with dental biofilm/plaque is biofilm-retentive and may act as a reservoir for endotoxins and bacterial antibodies.2 Many clinicians have observed that just about all bleeding sites (sites that bleed after conventional scaling and root planing) have residual calculus. The pieces can be as small as a millimeter or not tactilely detectable. In addition, the formation of a long junctional epithelium is generally not possible under these conditions. The calculus has to go, so why not “scope” around the pocket to find out where the calculus is hiding?
Why doesn’t every practicing hygienist own or rent a periodontal endoscope? For starters, it’s expensive. But according to Dr. Kwan, it will quickly pay for itself if periodontal diseases are diagnosed consistently. There’s only one periodontal endoscope on the market, andthe manufacturer is working on a newer version that will have better water control and improved imagery. It may also be smaller and cost less. Some companies offer other calculus detection devices, and I recently read about a German company that has developed a calculus detection device built into an ultrasonic insert.
There’s a huge disconnect between periodontal practices that offer conventional nonsurgical debridement followed by pocket reduction surgery, and those that focus on minimally invasive nonsurgical approaches
to periodontal therapy with adjunctive use of systemic antibiotics or locally applied antimicrobials. Dr. Kwan calls his technique “cleaning and disinfecting,” and describes his procedure through a brochure that details the process.
So why are Dr. Kwan and his hygiene team so far ahead of the pack, so to speak? Why do Dr. Kwan’s hygienists have manually tuned ultrasonic units and inserts and a periodontal endoscope for routine use, while other hygienists are still begging for the best technology?
Dr. Kwan is an avid reader of periodontal literature and considers all the evidence when making decisions at the clinical level. His nonsurgical protocol is less invasive and less expensive, and he has sought outside validation of his protocol through clinical studies and publications, including one in the Journal of Periodontology, and presentations at the American Academy of Periodontology and the International Association of Dental Research.
I knew I had stumbled on a very special periodontal practice when I walked through the front door. There on the bulletin board for all patients to read was a copy of an article from The New York Times' science section dated Jan. 21, 2003. The title was “Experts Debate the Best Way to Fix Ailing Gums,” and the content was highlighted in Dr. Kwan’s handwriting. The question “Can cleaning and antibiotics take the place of surgery?” is answered in Dr. Kwan’s handwriting: You bet!
The article mentions that standard periodontal care is to cut back the gums, clean the pockets and remove tartar from the enamel below the gum line. Dr. Kwan added another comment at the top of the article: We have been doing this (cleaning and disinfecting) for 12 years! Everyone else is so far behind!
Let’s go back to my initial thoughts about communing with mediocrity and practicing at what we don’t want to become. Dr. Kwan stepped out of his comfort zone when he moved beyond the norm and challenged the routine need for periodontal surgery. Let’s follow his lead and challenge ourselves to master this new technology, and recognize that it will improve with each generation of endoscopes. Make a commitment to yourself to think and do things differently. Insist on being treated with respect, not only as a team member, but as a dental provider with support that is on equal footing with the dentist. Stay true to your dreams and remember: If you always do what you’ve always done, you’ll always get what you’ve always got.
References
1 American Academy of Periodontology. World Workshop in Periodontics - Annals of Periodontology. 1996. Vol. 1: 1-947.
2 Tan TK, et al: Study of bacterial viability within human supragingival calculus. J Periodontol. Jan 2004: 23-29.