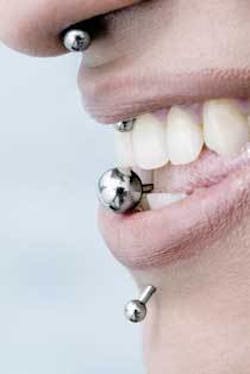
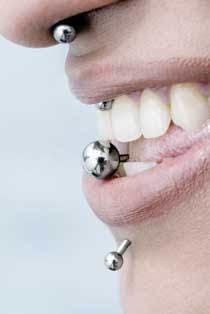
the perils of oral piercing
Oral piercing is a growing phenomenon in Western culture. Hygienists must be aware of the risks and possible consequences associated with oral piercing to educate patients who are considering the procedure.
Oral piercing, a smaller part of body piercing (also called “body art”) is not a new phenomenon, and it’s growing. In fact, history points to the Mayans, some of whom pierced their tongues to demonstrate courage and virility. The Aleuts and Eskimos sometimes pierced the lips of female infants as part of a purification ritual and the mandibular lips of boys to signify part of the passage into puberty. Items used for piercings included stones, bones, or ivory. In some Third World countries, oral piercings (using ivory, wood, pottery, or metal) are customs that continue to be practiced for religious, sexual, tribal, or marital significance.
The Surma tribe of Ethiopia wears large plates on their lower lips. Married men and widowers of the Suya tribe of Brazil adorn their mandibular lips with painted wood disks. Other tribes wear plugs on the maxillary lip or rings in the mandibular lip. And some inhabitants of Southern India pierce the tongue with a skewer to maintain a vow of silence. (Ouch!)
What's up in Western culture with oral piercing?
In Western culture, body piercing is most often considered a personal statement that reflects fashion, risk, daring, independence, or sexuality. Other motivations patients give include:
• Because they felt like doing it
• The desire to assert individuality
• The intense need for acceptance into a peer group or athletic team
• As a means to enhance perceived body image
• Spiritual reasons
The trend has been supported by sports stars and popular media, which display oral piercing as an acceptable form of body art. Statistically, women are more likely than men to undergo oral piercing; athletes more likely than nonathletes.
The most common age people undergo an oral or body piercing is between 18 and 30. This figure is supported by the hygienists we interviewed. Said Patti Schwenk, who practices in Coxsackie, N.Y., “In the 21 years in this practice, I have seen about 10 oral piercings. The age that seems to pop up is 16 to 30 - mostly college students.”
Another appeal to subjects who undergo intraoral piercings is the ability to conceal it in situations where piercings would be deemed inappropriate, such as in the parents’ home or the workplace. Reversibility with oral and body piercings, as compared with tattoos, has also added to their growing popularity. This may support the reason why many piercings are done as the result of an impulsive decision, especially peer pressure. Among impressionable youth, some piercings are performed on a whim, or dare, and may be done by unskilled peers of the adolescent being pierced, referred to as “peer-piercing.”
The most popular sites of oral/perioral piercing preferred by Westerners include the tongue, lips, frenum, cheeks, and uvula.
According to Patti, most of the piercing jewelry she has observed in her practice was located on the tongue. She notes that she has had two patients with piercings just below the lower lip. The jewelry was either a stud or barbell.
This is backed up by Mona Bumpers, a hygienist working in a general practice in Delmar, N.Y., who concurred, “The piercings I’ve seen were of the tongue and on the lower lip.”
Kelly Schest, who practices hygiene in Phoenix, Ariz., also concurred, noting the areas of oral piercing to be the tongue, lip, and cheek, with the tongue the most common site. Hygienist Nancy Genung, of Delmar, N.Y., has observed barbells and labrettes in her patients with oral piercings.
How is oral/perioral piercing performed?
The majority of oral piercings are referred to by “body modification artists” as “straight piercing”; that is, they do not require the boring needle to be bent as is required with other body piercing sites, for example, the navel. The piercer first assesses the anatomy of the site, the majority of which are chosen based on the statistical absence of major vessels or nerves, such as the midline of the tongue or lip.
Once the site it chosen, it is marked and the tissue grasped with sponge forceps. The most common initial piercing uses a 14-gauge boring needle to pierce the tissue. Once the tissue has been pierced, an identically sized piece of jewelry is used to push the boring needle through the tissue so that only the jewelry remains. No local anesthesia is used during oral piercing.
Immediate complications following oral piercing
Complications may result immediately following piercing or may result long-term.
Local inflammation of the tongue - When swollen, the tongue can affect speech, mastication, and deglutition. The submental and/or submandibular lymph nodes may also become enlarged and tender. Effects can last from three to five weeks. The oral cavity can be treated with a saline soak or rinse to reduce swelling. Persistent symptoms must receive professional attention.
Localized infection - The moist, warm environment of the tongue is an inviting breeding ground for bacteria, especially when the fingers are introduced into the oral cavity. Infection can most readily be prevented with meticulous aftercare following piercing. If infection should occur, chlorhexidine rinses or systemic antibiotics and local debridement can hasten healing and resolve infection. Any infection that does not respond within one to two days should receive professional attention because such infections can quickly become life-threatening.
Kelly noted that infections were a common occurrence in the tongue piercings she’s seen.
Trauma to the lingual gingiva - Edema and erythema of the gingiva is caused by the tendency to play with the tongue ball by rubbing it against the lingual gingiva. This can occur from placement of the dorsal ball against the maxillary lingual tissue or the ventral ball against the mandibular lingual tissues. According to Nancy, “I have found [gingival] recession on the labial of Nos. 24 and 25 in four patients; a couple of patients were referred to a periodontist for a graft.”
Bacteremia - A systemic infection can result from bacteria introduced during the piercing, or it can spread from a localized infection that could occur at any time. If symptoms such as fever, chills, shaking, or a red streaked appearance near the piercing site occur, a health-care provider must be consulted.
Ludwig’s angina - This condition involves an inflammation of connective tissue in the body. It spreads rapidly to involve submandibular, submental, and sublingual spaces. Signs and symptoms of Ludwig’s angina include painful tongue swelling, difficulty in speaking, and a compromised airway. This is a serious condition that demands immediate professional intervention because a compromised airway could be fatal.
Hyperplastic tissue - Tissue hyperplasia around oral jewelry may occur at the piercing site and may be accompanied by edema and pain. For most types of jewelry this will approximate the outline of the jewelry resting against the tissue. Severe tissue hyperplasia has been reported with jewelry engulfed in tissue to the point that surgical excision was the only viable option to release the jewelry.
Depending upon the degree of hyperplasia, generally the tissue can be excised, the wound treated, irrigated, and then followed with reinsertion of a sterile barbell. The tissues can become repeatedly hyperplastic following excision.
Dehiscence - The ball of the labrette or the lip barbell rubbing against the mandibular anterior facial gingiva can create a dehiscence. This could occur in any oral location where metal continually abrades or rubs against soft tissues. Should dehiscence occur, a periodontal consultation is advisable.
Cracked/fractured teeth - Damage to teeth can result from parafunctional oral habits related to biting the barbell, careless jewelry insertion, or talking, swallowing, or eating. Damage to the teeth is most likely to occur after swelling has diminished and the barbell fits loosely in the tongue. Either maxillary or mandibular teeth can sustain chipping from the ventral or dorsal ball on the tongue.
According to Patti, “One patient had chipped a posterior tooth while chewing food. The chipping occurred from a barbell inserted into the tongue.”Kelly also noted tooth fractures as a side effect of piercing. Nancy has seen fractured molars on some oral piercing patients.
Symptoms associated with cracked or fractured teeth include sensitivity to sweets and cold, and pain upon biting pressure. When a mandibular block injection is administered while the patient is still anesthetized, jewelry in the numbed tongue can readily result in cracked or chipped teeth during loss of tongue control.
Gingival recession/tooth abrasion - The habit of repeatedly pressing the tongue barbell against the mandibular lingual gingiva may lead to slight, moderate, or severe recession of oral soft tissues. Labrette or lip piercings may cause recession in the mandibular facial tissue. Likewise, the dentition can become abraded by the jewelry.
Aspiration or ingestion of the jewelry - In one type of oral jewelry a metal bar connects two balls of the barbell. One side of the rod has threads that screw the ball into position; this side is placed on the dorsum. If the ball becomes loose, there exists the potential to swallow or aspirate it into the lung. Also, during removal or insertion, the ball can inadvertently slip down the throat. Aspiration or inhalation of oral jewelry parts can occur any time after a piercing.
Choice of oral jewelry also a concern
If the individual should decide to undergo oral piercing, selection of proper jewelry is important. Oral jewelry should be made of inert nontoxic metal such as 14k or 18k gold, surgical stainless steel, titanium, or niobium. While the piercing procedure may cost from $15 to as much as $50, the purchase of jewelry is an additional cost that may range from $35 to $100. Because some individuals do not anticipate the cost of the jewelry when considering a piercing, the investment of proper jewelry for the procedure may be seen as an additional, unnecessary expense. Thus, the individual may elect to use costume jewelry or a safety pin in the opening instead. Because silver plating and other finishes on costume jewelry wear off quickly, they leave abrasive brass that predisposes the pierced site to infection and/or allergic responses.
The hygienist's role in patient education
It is important that the hygienist be aware of the risks and possible consequences associated with oral piercing to take the opportunity to educate patients seeking advice prior to undergoing oral piercing. This includes advising the patient on safety and health issues, as well as maintaining optimal oral hygiene both during and after the piercing procedure.
According to Kelly, “I advise patients that clicking or tapping mouth jewelry on teeth can lead to fractures in their teeth ... which sometimes are visible; other times they can be tiny hairline fractures in the enamel.” She noted that her practice dispenses oral piercing literature.
Nancy said, “I explain what I have observed with other patients, the risks and stress, the risk of septicemia, and death.” Her office also dispenses oral piercing literature.
Two sources of information to dispense to patients are brochures produced by the Association of Professional Piercers (which can be downloaded from the association’s Web site at http://www.safepiercing.com/) and the American Dental Association [Oral Piercing: Is It Worth It? brochure #W284; call (800) 947-4746 or visit www.adacatalog.org].
When giving information about oral piercing to a prospective piercee or concerned parent, the hygienist can take the opportunity to advise the person and emphasize the following:
• The need for maturity/responsibility on the piercee’s part because “upkeep” is required with the piercing site.
• Careful evaluation of the piercing studio, focusing on sterilization and infection control, as well as credentialing of the piercer.
• That during the initial four- to six-week healing period the tongue will be swollen, which may affect speaking, eating, drinking, and swallowing.
• The possibility of infection always exists, as well as the potential for fractured teeth and gingival recession, which may require professional intervention by the dentist.
• Quality of jewelry of the appropriate size is essential.
Post-piercing home care
Despite the best attempts of the well-intentioned hygienist to dissuade patients seeking oral piercing advice from doing so, any number of patients may elect to go ahead and have the piercing performed (by an outside business). In this case, the hygienist may elect to give post-piercing home-care instructions to prevent any number of immediate, short-term, or long-term complications associated with oral piercing.
➊ Rinse the mouth three to four times daily with an antibacterial mouthwash. Alcohol-free over-the-counter mouth rinses are acceptable. Chlorhexidine may be prescribed.
➋ Avoid hard and/or spicy foods for the first five to seven days. Adequate fluid intake (excluding alcoholic beverages) is advised.
➌ Suck on ice for the first three to five days to help reduce swelling.
➍ Tighten threaded piercings once or twice daily.
➎ Always wash the hands before handling mouth jewelry. Rinse with mouthwash after handling oral jewelry.
➏ Downsize the jewelry as soon as the swelling has subsided (two to four weeks).
➐ Avoid oral contact of any kind (e.g., kissing) for four weeks after initial piercing.
Kelly advises her new piercees to clean their oral jewelry frequently and to make sure their hands are clean when handling it. She also advises them to rinse with an antibacterial mouthwash and to change their toothbrushes frequently. “A new toothbrush is very important initially when piercing is done,” she concludes.
Management of the patient with an oral piercing
Most often, a patient who presents with an oral piercing will not require any special considerations by the oral health-care team during routine treatment. However, sometimes removal of oral jewelry is indicated.
During exposure of radiographs, it is often necessary to ask the patient to remove his or her oral jewelry. For panoramic radiographs, all jewelry should be removed above the neck. Cheek and labrette jewelry should be removed for exposing periapical and bitewings radiographs due to their location in relation to film placement and the tube head.
In some cases, oral jewelry must be removed under local anesthesia, with the administration of a mandibular block. When the tongue is anesthetized, patients should be cautioned that there is increased possibility for tooth damage or accidental biting of the tongue until the anesthesia has completely worn off.
Where do we stand? Where do we go from here?
The American Academy of Pediatric Dentistry has issued a policy statement “strongly opposing the procedure of piercing intraoral and perioral tissues and the use of jewelry in intraoral and perioral tissues due to the potential for pathological conditions and sequelae associated with this procedure.”
The American Dental Association opposes the practice of intraoral/perioral piercing and supports legislation requiring parental consent of minors (who want to be pierced) because of the potential for numerous negative sequelae.
According to hygienist Colleen Schmidt of the American Dental Hygienists Association, “The ADHA currently has no policy statement regarding oral piercing.”
Each state has the opportunity to individually consider legislation regarding the issue of minors and regulation of piercing parlors; they could have the power to mandate the use of sterile equipment, as well as submission to OSHA guidelines and inspections.
Currently 13 states have enacted regulations on tattooing and body piercing. Of them, only six exercise authority over body piercing establishments. New Jersey adopted regulations that require the licensing and inspection of these facilities, as well as setting standards for the sterilization and disinfection of instruments. These regulations also require the written consent of a parent or legal guardian before piercing the ears, nose, tongue, or other body part of a person under the age of 18. The parent or guardian must be present during the procedure.
While many in the health-care profession may view intraoral piercing as a fad that they hope will eventually go away, it is currently increasing in popularity and, therefore, must be addressed by the dental community. The best professional advice to give a patient who is contemplating intraoral piercing is to avoid the procedure entirely, given the potential for complications that range from minimal to life-threatening. If an individual desiring oral piercing cannot be dissuaded from undergoing the procedure, the hygienist can best advise him or her to seek out a reputable facility where universal precautions, including the use of sterile gloves and sterile instruments, are followed. In addition, the patient’s medical history should be evaluated prior to the piercing procedure to rule out a history of bleeding disorders, conditions that make a patient immunocompromised, keloid formation, and the need for antibiotic prophylaxis.
References available upon request at [email protected].
Different types of oral piercings
There are a number of oral piercings, with tongue piercing the most common site.
✴Dorsoventral - There are two types of tongue piercing, dorsoventral and dorsolateral. The safer and most common is dorsoventral. In dorsoventral piercing, the jewelry is inserted from the dorsal to the ventral tongue surfaces. This piercing is most commonly done in the middle of the tongue; major blood vessels are located in this area and must be avoided during the piercing. Some individuals have multiple dorsoventral piercings. Barbells are the most commonly used forms of jewelry inserted into the dorsoventral piercing. Tongue rings may also be used when the piercing site is located near the tip or lateral borders of the tongue.
Dorsolateral piercing is not a safe procedure because of the vascularity of the tongue. During this piercing procedure, both spheres of the jewelry are on the dorsum of the tongue at the lateral borders and located approximately halfway in an anteroposterior direction. The barbell is placed dorsally, curves down toward the ventral side of the tongue, and resurfaces at the dorsal aspect.
✴ Labrette - Another popular type or oral piercing is the labrette, which refers to piercing sites on the lip(s). One style is placed above the labiomental groove, centered below the vermillion border. The jewelry placed at the location can contribute to gingival recession at the anterior facial surface of the mandibular region, caused by physical trauma to the tissues.
Lip piercings can be placed anywhere around the vermillion border. The most common site is the side of the mandibular lip near the commisure. The piercing extracts through the lip extraorally and inserts into the oral cavity. A ring is often worn encircling the edge of the lip.
Other, less common oral/perioral piercing sites include the cheeks, lingual frenum, and the uvula. Cheek piercings are also called “dimples” because the bilateral placement corresponds to common locations of dimples. The intraoral placement of the ball of the oral jewelry at the buccal mucosa can lead to gingival recession and/or abrasion or chipping of the teeth.
The lingual frenum site is sometimes referred to as a “web” piercing. The uvula is an uncommon piercing site due to the inherent difficulties involved in performing the piercing and placing the jewelry. Functional issues associated with uvula piercing include gagging, throat irritation, and deglutition problems. In individuals with several oral piercings, the effects on speech, mastication, and deglutition are compounded.
Complications: what the dental hygienist should know
Complications associated with oral/perioral piercing can occur either during the initial procedure or at any time thereafter. It is important for the hygienist to be aware of these sequelae to inform both the potential and current piercers; also so that complications can be recognized during the oral examination. The following effects can happen during piercing, shortly afterward, or long after the piercing procedure.
✴ Hemorrhage - The tongue is highly vascularized, served by the deep lingual artery and vein. It will bleed - sometimes profusely - during the piercing procedure. This bleeding should soon be well controlled. Extreme hemorrhaging can occur and must receive immediate attention.
✴ Trigeminal nerve damage - It is possible to puncture a portion of the mandibular division of the nerve during the piercing procedure because the tongue is highly innervated by the trigeminal facial, hypoglossal, and glossopharyngeal nerves. Nerve damage is more common with the dorsolateral than with the dorsoventral tongue piercing, but can occur with either. If nerve damage occurs, there can be sensory or motor effects, depending on the nerves affected.
✴ Communicable diseases - Many types of communicable diseases can result from improper sterilization or disinfection of piercing equipment or supplies. Universal precautions must be utilized throughout the piercing procedure because blood and body fluids are involved during oral piercings.
Piercing has been identified by the National Institutes of Health as a possible vector for the transmission of bloodborne viruses, such as HIV, hepatitis (B,C, D, and G), herpes simplex, and Epstein-Barr. Tetanus may also occur.
A number of factors have been hypothesized to influence the development of an infection resulting from body piercing. These include the blood supply to the site, intrinsic healing capacity of the affected tissue, and the environment in which the tissue heals (including hygiene), in addition to the aseptic technique used during the initial puncture.
Purulent bacterial infections have been described in association with tongue piercing. The exact frequency with which pierced tongues will eventually become infected is yet undocumented. Although the tongue heals relatively quickly, it has the unique feature of being in a warm, moist environment, constantly bathed in saliva. This allows constant exposure to potential aerobic and anaerobic pathogens. And although the incidence of tetanus in the United States has been progressively declining, it may be resurfacing due to the practice of body piercing.Cephalic tetanus occurs most commonly as a result of injuries to the head or dental or middle ear infections. This rare form of tetanus commonly manifests as facial nerve palsy and trismus. Although facial musculature weakness occurs most commonly, evidence of other cranial nerve dysfunction frequently occurs.
Risks Associated With Oral Piercing
The hygienist should calmly and frankly explain the possible current, immediate, and long-term complications associated with oral/perioral piercing , which include:
✴ Pain
✴ Swelling
✴ Infection (bacterial, viral, or fungal)
✴ Airway obstruction
✴ Bleeding
✴ Trauma to teeth and mucosa
✴ Speech impediment and swallowing problems
✴ Hypersalivation (salivary incontinence)
✴ Lingual nerve damage
✴ Swallowed or inhaled (aspirated) jewelry
✴ Foreign body incorporated into the piercing site
✴ Radiographic artifact
✴ Calculus formation on metal surface
✴ Galvanic and hypersensitivity to metal
Adapted from Theodosy. Complications of tongue piercing: a case report and review of the literature. Br Dent J 2003; 194:551-552.