Case #9
by Joen Ianucci Haring
A 40-year-old female presented to a dental office for evaluation of a gingival swelling.
History
The patient first noticed the swelling one month earlier and stated that since it first appeared, the tiny lump had a tendency to "come and go." When questioned about symptoms, the patient claimed that whenever the swelling appeared, it was accompanied by moderate pain. The patient also stated that as the lesion disappeared, she noticed a bad taste in her mouth and the pain would subside.
At the time of the dental appointment, the patient appeared to be in an overall good state of health. At the time of the dental appointment, the patient was not taking any medications. The patient's past dental history included sporadic dental examinations and routine dental treatment. The patient's last dental appointment was approximately two years earlier.
Examinations
Physical examination of the head and neck region revealed no enlarged or palpable lymph nodes. The patient's temperature was not elevated and the vital signs were all within normal limits. No significant extraoral findings were noted.
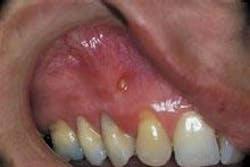
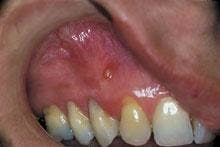
Intraoral examination revealed an elevated yellowish papule near the mucogingival junction and apical to tooth #6 (see photo). The lesion measured three millimeters in diameter and was fluctuant when palpated. A smooth surface without ulceration or hemorrhage was noted. A periodontal probe was used to identify one small opening on the surface of the lesion. Teeth #5 and #6 were pulp tested for vitality; tooth #5 tested vital and tooth #6 tested non-vital. Further examination of the oral cavity revealed no other lesions present. A periapical radiograph of the area was exposed. The radiograph demonstrated a well-defined radiolucency at the apex of tooth #6.
Clinical diagnosis
Based on the clinical and radiographic information presented, which of the following is the most likely diagnosis?
o periodontal abscess
o gingival cyst
o parulis
o peripheral giant cell granuloma
o pyogenic granuloma
Diagnosis
• parulis
Discussion
The parulis, also known as the "gum boil," is an extremely common oral lesion. The parulis is a localized collection of pus in gingival soft tissue. The pus is produced as a result of necrosis of non-vital pulp tissue, or occlusion of a deep periodontal pocket. In this case study, parulis formation was caused by a non-vital tooth.
Parulis formation as the result of a non-vital tooth can be described as follows:
• Pulp tissue becomes infected, dies, and undergoes necrosis.
• The necrotis tissue (pus) accumulates at the apex of the non-vital tooth.
• The pus drains peripherally and produces a "fistula," which is an abnormal channel in body tissue.
• A parulis forms at the end of the draining fistula.
Clinical features
The parulis may be seen in any individual with a non-vital tooth or occluded periodontal pocket. When seen with a non-vital tooth, the location of the parulis is typically apical to the offending tooth on or near the mucogingival junction. When seen with a periodontally involved tooth, the lesion occurs adjacent to the deep periodontal pocket.
The clinical appearance of the parulis is fairly characteristic. The lesion appears as a yellowish gingival swelling surrounded by erythema. The parulis is fluctuant when palpated and usually measures less than five millimeters in diameter. When examined with a periodontal probe, a small opening into the adjoining fistulous tract can be identified. A purulent exudate can be expressed from this small opening.
The symptoms associated with a parulis may vary. The lesion may be painless or cause considerable pain. The pain, when present, typically persists until pus escapes at the surface opening. The drainage of pus relieves the pain and often causes a bad taste in the patient's mouth.
Diagnosis
On a clinical basis, the parulis may be confused with a number of other lesions including the pyogenic granuloma, the peripheral giant cell granuloma, the abscess, and the gingival cyst. The parulis can be differentiated from such lesions by identifying the production of pus and determining the source of infection (for example, non-vital tooth vs. occluded periodontal pocket).
The diagnosis of a parulis can be made on a clinical basis; no biopsy is necessary. Diagnostic aids include pulp testing and periodontal probing of the teeth adjacent to the lesion. The dental radiograph can also be used as a valuable diagnostic aid.
A sterile gutta percha point can be placed into the surface opening of the parulis and inserted into the fistulous tract. Following insertion of the gutta percha point, a periapical radiograph can be exposed. The proximity of the gutta percha point to the apex of the non-vital tooth can be evaluated on the dental radiograph.
In addition, the periapical region of the tooth can be examined for evidence of an increased widening of the periodontal ligament space or a well-defined radiolucency.
Treatment
The treatment of the parulis involves treating the underlying condition. In cases of a non-vital tooth, endodontic procedures or extraction is indicated. In cases of an occlusion of a deep periodontal pocket, periodontal therapy is indicated. Once the underlying cause is treated, the parulis resolves and does not recur.
Joen Iannucci Haring, DDS, MS, is a professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.