Case #7
By Joen Iannnucci Haring
A 29-year-old male visited a dentist for evaluation of a large growth on the gingiva near his upper front teeth.
History
The patient first noticed the pinkish-red growth in front of his upper anterior teeth several months earlier. The patient claimed that the lesion appeared as a small lump and had gradually increased in size. When questioned about any change in color or texture, the patient stated that, when the lump first appeared, it was soft, reddish in color and had a tendency to bleed. The patient noted that, with time, the lesion became firm and pinkish-red in color. The patient denied any pain or discomfort associated with the lesion. The patient reported no history of trauma to the affected area.
At the time of the dental appointment, the patient appeared to be in an overall good state of health. The patient's medical history was reviewed; no significant positive findings were noted. At the time of the dental visit, the patient was not taking medications of any kind. The patient's dental history included regular dental examinations and routine dental treatment. The patient's last dental appointment was approximately two years earlier for a dental prophylaxis.
Examinations
Physical examination of the head and neck region revealed no enlarged or palpable lymph nodes. The patient's vital signs were all found to be within normal limits. No significant extraoral findings were noted.
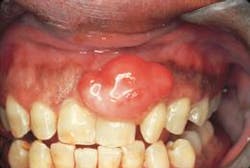
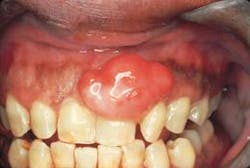
Intraoral examination revealed an elevated, pinkish-red nodule involving the marginal gingiva and located in the interdental papilla area between teeth #9 and #10 (see photo). The lesion appeared to be a firm, well-defined, broad-based growth that measured approximately 1.5 centimeters in diameter. A smooth surface without ulceration or hemorrhage was noted. The teeth adjacent to the lesion were pulp tested for vitality; all tested vital. Further examination of the oral soft tissues revealed no other masses present.
The patient was referred to an oral surgeon for biopsy and removal of the lesion. Histologic examination revealed a cellular connective tissue proliferation with plump fibroblasts, a delicate stroma, and scattered calcifications.
Clinical diagnosis
Based on the clinical and histologic information presented, which one of the following is the most likely diagnosis?
o peripheral ossifying fibroma
o peripheral giant cell granuloma
o pyogenic granuloma
o irritation fibroma
o giant cell fibroma
Diagnosis
• peripheral ossifying fibroma
Discussion
The peripheral ossifying fibroma (POF) is a relatively common reactive lesion. This lesion appears as a "bump on the gums" and is believed to arise from the periodontal ligament. The term "ossifying" refers to the calcifications that are seen when the POF is examined histologically.
Clinical features
Although the POF may be seen at any age, it typically affects young people ranging in age from 10 to 19. Females are affected more frequently than males. The location of the POF is characteristic. This lesion is only found on the free margin of the gingiva in the interdental papilla area and is always seen in association with teeth. It usually occurs anterior to the molar area. The gingival tissues of the anterior maxilla are affected more frequently than the gingival tissues of the mandible.
The clinical appearance of the POF is also fairly characteristic. The lesion usually appears pale pink to pinkish-red in color. The POF may be broad-based (sessile) or appear pedunculated. The surface may be smooth or may exhibit ulceration if traumatized. When palpated, the POF feels slightly firm and usually measures less than 2 centimeters in diameter. When a POF first forms, it may have a vascular, reddish appearance and bleed easily. With time, the lesion becomes more firm and fibrous and appears pale pink in color. The POF is asymptomatic. Typically, the intraoral radiograph is not useful in the evaluation of a POF. Only in rare instances does the POF exhibit a cup-like erosion of underlying bone.
Diagnosis
The POF may clinically resemble the irritation fibroma, the pyogenic granuloma, the peripheral giant cell granuloma, or the giant cell fibroma. The pale pink color of a mature POF is similar to that of the irritation fibroma, peripheral giant cell granuloma, or the giant cell fibroma. The reddish color of an early POF is similar to a pyogenic granuloma. A biopsy and histologic examination of the tissue is necessary in order to establish a definitive diagnosis.
When examined histologically, the POF appears as a hyperplastic connective tissue growth that exhibits a proliferation of plump fibroblastic cells along with scattered calcifications. The calcifications may represent cementum or bone.
Treatment
The POF is reactive connective tissue lesion; this lesion is not contagious and does not have malignant potential. The POF does not spontaneously disappear or regress with time. The treatment of choice for the POF is surgical excision. Surgical removal should include the base of the lesion and extend to the bone; curettage of underlying bone is recommended. If properly removed, the POF should not recur. If removal is incomplete, a recurrence may be seen; approximately 16 percent of peripheral ossifying fibromas recur following treatment.
Joen Iannucci Haring, DDS, MS, is a professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.