Effective, Conservative, Contemporary, Non-surgical Periodontal treatment
by Teresa Barjenbruch, RDH, Lisa O'Connor, RDH, and David P. Reichwage, DDS
Our practice finds it disturbing that there is such a high prevalence of periodontal disease — almost to epidemic proportions — in an era of medical and dental technological advances. It is the philosophy of our practice to be patient-centered, and it is our mission to diagnose and treat periodontal disease, including its earliest form — gingivitis. The methodology to accomplish this is conservative, non-surgical treatment with active patient involvement. We use a systemic approach to patient care, and the model we have created is based on our standard of care. Since we use it daily on every patient, our model is continually tested and evaluated, based on predictions of treatment outcome as well as direct observations of its effectiveness. The first step of this system is to perform a comprehensive clinical and diagnostic evaluation. This evaluation includes:
• Occlusal evaluation and anterior guidance
• TMJ exam and muscle palpitation
• Head and neck exam, and oral cancer screening
• Charting of existing restorations and missing teeth
• Diagnosing areas of caries
• Taking a full-mouth series of periapical films, bitewings and panoramic X-ray
• Ascertaining the patient's concerns
• Establishing goals for treatment
• Consideration of motivating factors, as well as personality profiles
Our periodontal evaluation form also becomes an educational tool for each patient. We record six-point pocket depths for each tooth, bleeding points, recession, furcations, mobility, tissue contour, tissue color, plaque scores, and calculus present. We explain to them that this is the most efficient way to determine their progress and periodontal health at a glance. We also point out to the patient all of the etiological factors that affect periodontal health and may compromise treatment. This includes genetics, general systemic health, hormonal changes, diet, oral hygiene, occlusion, tobacco use, and stress.
It becomes evident to the patient that they can develop a "barometer" to measure their periodontal health and susceptibility to disease. All of the data and variables are used as instruments to map the course of treatment. This "map" is developed with patients' input based on their own treatment goals. They become actively involved in their treatment recommendations.
Co-diagnosis and treatment planning with the patient set the stage for the next step — providing conservative treatment. This includes the number of therapy appointments to be scheduled, the sequence in scheduling, and the actual clinical modalities that are to be used. The ultimate goal of periodontal therapy (PT) is to stop disease progression and to stabilize and improve tooth attachment. Treatment includes the use of hand instruments for scaling and root planing. We use micro-ultrasonics for debridement and irrigation. The unit we use is Dual Select by Dentsply.
Dr. Reichwage uses a diode laser to remove diseased epithelium and for bacterial decontamination. Local antimicrobials, such as Atridox, are used when pocket depths are five millimeters or greater. Lastly, Periostat is used at 3, 6, 9, or 12-month intervals, depending on the patient's progress. This subantimicrobial dose of doxycycline (20mg), used twice daily, is approved by the FDA for enzyme suppression to manage periodontitis.
Regardless of the treatment modalities used, the purpose is to achieve a gradual healing process and continue treatment until the disease process is controlled. Co-therapy by the patient is critical. Our recommendations for this include daily use of a power toothbrush, floss, and a chlorine dioxide toothpaste and rinse, such as Oxyfresh. Follow-up after periodontal therapy is crucial. Our system involves re-evaluation after six weeks and again after three months. Maintenance intervals of supportive periodontal therapy (SPT) are determined by the progress patients achieve. Our typical recommendation is a three-month cycle, but can be as short as eight weeks.
First case report
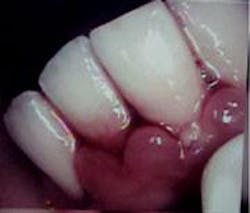
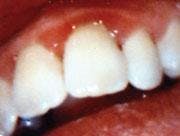
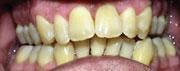
A 26-year-old male patient presented with a desire to alleviate generalized bleeding, inflammation, and sore gums. It had been more than 10 years since his last dental visit. We started by conducting a comprehensive clinical and diagnostic evaluation. We performed co-diagnosis techniques with the patient by using a hand mirror, radiographs, and intraoral camera in order to have the patient involved in the clinical data process and understanding the findings as we presented them. It was noted that his medical history was negative and presented no contributory data. The following were findings from his complete clinical evaluation: hyperemic bulbous tissue, heavy supragingival and subgingival calculus, probe depths from four to seven millimeters and 109 bleeding points. He was diagnosed with Moderate Periodontitis Type III, with light to moderate generalized bone loss (see Figure 1).
Treatment plan — We reviewed our findings, the etiology behind our concerns, and the treatment necessary to achieve perfect tissue health. Treatment would consist of four to six PTs, which include scaling and root planing, micro-ultrasonics with chlorhexidine for irrigation, soft tissue laser to reduce and contour the bulbous infected tissue, and decontamination of the periodontal pockets. Following the last PT, a six-week SPT would be needed to evaluate healing and determine if additional PTs were necessary. The patient would then be placed on a supportive recare schedule based on his needs.
Procedure — At the initial periodontal therapy (IPT), the patient was disclosed and was given manual and power brushing and flossing instructions. Treatment began the next day and started with local anesthesia on the lower arch with 4 percent Citanest Plain and Carbocaine 2 percent Neo-Cobefrin.
Once profound anesthesia was obtained, treatment began by using the micro-ultrasonic to remove supragingival and subgingival calculus. Next, scaling and root planing were performed to fine scale and remove any residual calculus. Scaling and root planing were followed up by using the micro-ultrasonic with chlorhexidine to flush out and irrigate the pockets.
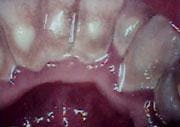
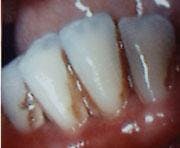
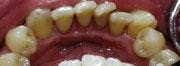
The last step consisted of the doctor using the soft tissue laser. The laser was set at 3.5-4.5 continuous wave (CW) and Touchtips were used to contour the tissue. The laser was then set at 1.2 CW and used to decontaminate the pockets. Once the laser was completed, vitamin E was placed and a gel was dispensed as a soothing and healing agent. Post-operative instructions were also given. Two weeks later, this same procedure was repeated on the upper arch (see Figure 2).
Results — Six weeks after the last PT, the patient returned for an SPT to evaluate the healing process, as well as his home care and plaque control. During this appointment, we also re-treated with micro-ultrasonics and chlorhexidine for irrigation.
At that time, a marked decrease in inflammation was noted and the gingival tissue was responding well to the therapy. The tissue was generally pink and no longer bulbous. Some marginal redness was noted on the upper arch. The patient was given a Braun 3-D Excel Electric Toothbrush and Oxyfresh toothpaste and fluoride rinse. He was placed on a three-month SPT continuing care cycle.
Twelve months post-treatment, the patient's tissue is no longer bulbous and is generally pink. He has generalized one to four millimeters pocketing with 16 bleeding points (originally 109 bleeding points). The patient commented on how good the tissue looked and felt, and how it was no longer bleeding.
Second case report
A 46-year-old male presented with a desire to alleviate chronic pain he was experiencing on the upper left side. He stated that it had been more than seven years since his last dental visit. The patient admitted that he had a fear of dental procedures and was uncomfortable in a dental environment. He also stated his goal was to keep his natural teeth and bring his needed dentistry up-to-date.
We conducted a comprehensive clinical and diagnostic evaluation. The patient presented with red, swollen gingivae that were tender to the touch and the tissue contour was irregular in several areas. Upon disclosing, moderate plaque was present. Calculus, both subgingival and supragingival, was described as moderate to heavy. The patient had generalized recession of one to two millimeters. Probe depths ranged from 2-12 mm, with heavy, profuse bleeding upon probing. Radiographically, moderate to severe bone loss was noted. No mobility was present in any of the teeth. The diagnosis was Advanced Periodontitis Type IV.
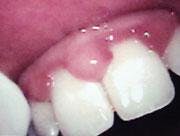
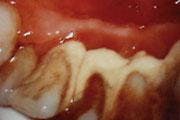
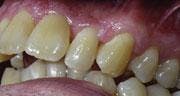
Disruptive occlusal patterns and prematurities cannot be discounted as contributing etiologies in this case. Our clinical findings showed posterior cross bite, anterior open bite, and 80 percent overbite. We performed co-diagnosis techniques with the patient by using a hand mirror, radiographs, and intraoral camera in order to have the patient involved in the clinical data process and to understand the findings as we presented them to him. It was noted that his medical history was negative and presented no contributory data (see Figure 3).
Treatment plan — At the treatment plan consultation appointment, we reviewed our findings, the etiology behind these concerns, and the treatment necessary to restore carious lesions and achieve perfect tissue health. Short-term goals were to treat active decay that was causing the patient chronic pain. Our first recommendation was to refer the patient to a periodontist due to the severity of the pocketing. The patient declined and requested to be treated at our office.
The treatment recommendation consisted of six to eight PTs at two-week intervals with the repetitive placement of Atridox and the use of the diode laser. The goal was to achieve a reduction in pocket depth, inflammation, and bleeding points. The patient would also need a six-week SPT to evaluate healing and to decide if he required more periodontal therapy or could be placed on a recare interval.
Long-term treatment goals include the possibility of a referral to a periodontist if there is not enough pocket reduction to achieve health and stability. The final phase of treatment will be to take the necessary bite registrations for mounted models and perform an occlusal analysis to diagnose and treat premature contacts and lateral interferences.
Procedure — At the IPT, the patient was disclosed and was given both manual and electric brushing instructions as well as flossing instructions. The patient was also instructed to dry brush for at least 10 minutes per day and to use a rubber tip stimulator to massage and help re-contour the tissue. The patient was placed on doxycycline (100 mg) twice a day during PTs to help get the infection under control and to avoid periodontal abscesses due to the severity of the pocketing. He was also placed on Gel-Kam stannous fluoride to help with root sensitivity.
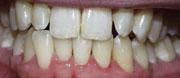
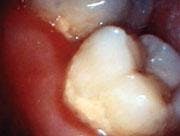
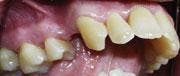
At each PT, scaling and root planing were performed in conjunction with micro-ultrasonics and irrigation with chlorhexidine. Dr. Reichwage used the soft tissue laser for removal of necrotic epithelial lining decontamination, and then placement of Atridox was performed. Periodontal therapies were performed approximately two weeks apart and included ongoing monitoring of oral hygiene progress and healing (see Figure 4).
Results — The patient was brought back for a six-week SPT. At this time, he was re-treated with micro-ultrasonics and chlorhexidine for irrigation. He was also evaluated for healing and plaque control. The patient was placed on an eight-week SPT interval to closely monitor healing. When the patient returned for his six-week SPT, there was a significant improvement in pocket depths, but heavy bleeding was still present. Tooth and tissue sensitivity had been resolved. Three months after the PTs, the patient had a pocket reduction of one to five millimeters.
Six months later, periodontal progress had been tremendous, but periodontal health was still not ideal, so the patient was placed on Periostat. Seventeen months post-op, Atridox was placed in pockets of five millimeters and greater. At this appointment, the patient was found to have dramatic improvement with pocket depths ranging from two to seven millimeters (previously 2-12 mm), bleeding light, tissue pink, and contour normal.
The patient was encouraged with the results. He was relieved that at this point he could be maintained without seeing a periodontist. The patient is aware that, in the future, Atridox will need to be placed sporadically to control the disease and maintain health. The patient is also aware of the importance of SPTs to maintain and control the disease process. These significant results could not have been achieved without the commitment and determination of both the patient and the hygienist.
The identity that our team desires for our practice is one of dedication to excellence. Our method to achieve this identity is to offer each patient customized, comprehensive, state-of-the-art care. This includes complete and accurate periodontal diagnosis and treatment planning with the ultimate goal of perfect tissues. The benefit of this for our patients is that they have active participation in selecting the level of care that is best for them, which is to restore their mouths to comfort, health, aesthetics, and function.
The authors acknowledge that this article incorporates both conservative and nonsurgical periodontics as taught by JP Consultants Institute, as well as occlusal and restorative principles taught by Drs. Ronald D. Jackson and William Dickerson at the Las Vegas Institute for Advanced Dental Studies.
Lisa O'Connor, RDH, is a 2000 graduate from Indiana University-Purdue University. Teresa Barjenbruch, RDH, is a 1990 graduate from Indiana University at South Bend. Both dental hygienists have attended the Pacific Esthetic Continuum and completed an advanced anterior esthetic courses and laser certification courses. Barjenbruch is a graduate of the JP consultants Institute in the advanced diagnosis and treatment of periodontal disease. David Reichwage, DDS, has practiced family dentistry in Fort Wayne, Ind., for 29 years. He has completed courses in laser dentistry, and advanced cosmetic, periodontal, and restorative dentistry.