The Oral Cancer Exam
by Diana Burnham, RDH
In recent years, there have been no significant changes in the statistics related to oral cancer. The term oral cancer includes cancers of the mouth, throat, pharynx, lips, cheeks, gums, and tongue. Oral and pharyngeal cancers continue to account for 2 to 3 percent of cancer deaths in the United States.12 It is estimated that 32,000 new cases are diagnosed each year, and approximately 8,000 people will die annually.1,3 Oral is the sixth most common cancer and continues to be more prevalent than cervical cancers, melanoma, and Hodgkin's lymphoma.4
The prognosis depends on the stage of the cancer and when it is diagnosed. Patients diagnosed with localized tumors have a five-year survival rate of 80 percent, whereas patients diagnosed with regional metastasis have a five-year survival rate of 40 percent, and less than 20 percent with distant metastasis. Surgery, which is often part of the required treatment, can be extensive, complex, and result in disfiguration. Of all the diseases of the oral cavity, oral cancer remains the most serious, and early detection and prevention continues to be the primary focus in reducing the morbidity and mortality rate.
Oral cancer examination/screening
What exactly is an oral cancer examination? Many patients ask this question and are unaware of the oral exam's existence. Studies have shown that less than 15 percent of those who visit a dental practice regularly report having an oral cancer screening.5 Are dental professionals dropping the ball, or are patients simply unaware that a screening had been done? One dentist concerned with these statistics wrote to the Journal of the American Dental Association: "After examining 50 patients [for oral cancer], I asked them if they realized they had just had an oral cancer examination. Forty-three out of 50 told me they were not aware I had just done an oral cancer examination."3 If this is the case, then dental professionals must tell patients exactly what they are doing and its purpose.
An exam consists of a thorough visual and manual examination. A logical sequence should be maintained to ensure that no areas are overlooked. The vermilion border, the labial and buccal mucosa, tuberosities, retromolar pads, and the hard and soft palate should be looked at and palpated for any abnormalities. The uvula, anterior and posterior tonsillar pillars should be checked using a tongue depressor or mouth mirror to maximize visibility. A 2" x 2" gauze square helps maintain a secure grasp when checking the tongue. The ventral and lateral borders of the tongue are high-risk areas and should be thoroughly examined. Using the gauze allows the clinician to manipulate the tongue and access those hard-to-see places. When lifting the tongue, examine the floor of the mouth for abnormal red, white, or red/white speckled lesions, then bimanually palpate the area for any lumps or nodules.
This may all seem like a lot for a one-hour appointment; however, a thorough exam takes only 60 to 120 seconds. This is little time to sacrifice if practitioners can add many years to a patient's life because of early detection.
Educating patients
Patient education is the foundation to increasing awareness. Dental professionals should use their patients as a pipeline of communication to the outside world. Information obtained during a dental visit may be passed along to patients' colleagues, family, and friends.
Dental providers must maintain a standard of care and are professionally responsible for determining which patients are at risk of developing oral cancer. Characteristics of a patient such as age, sex, ethnic background, and occupation should be evaluated and considered in the assessment. Patients' social habits should be evaluated in order to properly educate them on the seriousness of any of risk factors in which they participate. Questions should be addressed on the medical history forms, or even better, a separate form addressing their habits in more detail could be available. Patients who have disclosed that they use tobacco, drink, are outdoors frequently, etc., should learn how to do their own oral cancer screening since all of these factors place them in a high-risk category. Show them where the high-risk areas are and educate them on what to look for. It is important to point out that many times initial cancer lesions are painless. Advise them to come in if any of the following occur and do not resolve in 14 days.5
• A red, white, or red/white speckled patch that cannot be wiped off and won't go away
• A sore that bleeds easily and won't heal
• A lump or thickening anywhere in the mouth or neck
• Pain, tenderness, or numbness anywhere in the mouth or on the lips
• A change in the way the teeth fit together
• Trouble chewing, swallowing, speaking, or moving the jaw or tongue
Although the exam may be negative, the patient's awareness has increased. The patient can continue routine checks and share this information with someone else who is at a high risk for oral cancers. This is how awareness increases.
A safe alternative?
Although public awareness of an oral cancer examination is lacking, people recognize the risk factors of oral cancer. A consortium led by the New York University College of Dentistry conducted a three-day oral cancer screening. In addition to the screening, subjects were given a survey about their oral cancer knowledge. Nearly 76 percent of the subjects knew that tobacco was a major risk factor for oral cancer.2
However, when people associate tobacco as a risk factor, the first thing that comes to mind is cigarette smoking. In an effort to cut back on smoking, people will often search for an alternative. Some people are under the impression that a "smokeless" substance is less harmful than a "smoked" tobacco product. This is exactly what the United States' producers of smokeless tobacco wants the public to believe. In fact, they have gone as far as to ask the Federal Trade Commission for permission to advertise that smokeless products could be a safer way to consume tobacco than cigarettes. The U.S. Surgeon General disagrees with this statement and reports that snuff "is not a safe substitute" for cigarettes.6
Each year 10 to 16 million Americans use smokeless tobacco. Their risk for some types of cancer can be as much as 50 times greater than those who use no tobacco products.7 There are two forms of spit tobacco: chewing tobacco and snuff. Chewing tobacco is usually sold as leaf tobacco (in a pouch) or plug (in brick form). It is placed between the cheek and gums and kept there for several hours to maintain a continuous high from the nicotine being released.
Snuff is a powdered tobacco that is usually sold in cans. It is placed between the lower lip and gums. The nicotine is absorbed quickly into the bloodstream and results in a quick high.
Holding chew in the mouth for 30 minutes gives a person as much nicotine as three or four cigarettes. Using two cans of snuff each week equals the amount of nicotine inhaled by someone smoking a pack and a half each day.8 While this decreases the risk for lung cancer, it increases the risk for cancer in the oral cavity. Changes in the oral mucosa can be seen microscopically as soon as seven days after using smokeless tobacco. People need to be educated to understand how this product contributes to oral cancer.
Role of the dental professional
Members of the dental profession not only need to participate in increasing the awareness of the patients in their private practice, but they also need to become strong advocates of community education. This is their area of expertise, and as members of this profession they ought to take charge and become more involved with organizations that support the same cause. Organizations such as the Oral Cancer Foundation and the National Cancer Institute recognize the importance of early detection and are launching public awareness campaigns to instill the importance of annual screenings. Unfortunately, the messages have not been successful enough to cause public concern.
Other cancer organizations have partnered with those in the medical community to emphasize the seriousness of cancer of the breast, prostate, and cervix. They have devoted endless hours getting the public involved, which has led to an increase in annual PAP smears, prostate exams, and mammograms. Dental professionals need to put forth this kind of effort to get the attention of the public on the issue of oral cancer. Only a well-financed, ongoing national campaign about annual oral cancer exams will move this issue from the shadows into the forefront of health education.3
Discovery and diagnosis
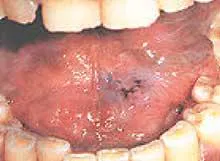
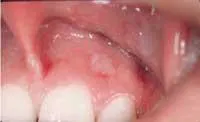
Many dentists and dental hygienists agree that it is often difficult to determine whether the discovery of abnormal tissue is worthy of concern. The average individual presents in the office with various changes in the oral tissue that can resemble a precancerous lesion. For example, the photo at right is a typical lesion that may be easily overlooked. It proved to be precancerous or cancerous.4
There are two products on the market — the brush biopsy and a chemolucent ViziLite — that can provide additional information about whether or not the lesions found at chairside are benign or should be sent for a scalpel biopsy. The brush biopsy is performed chairside in the dental office using a brush biopsy similar to the brush biopsies used to detect cancer in other organs. The sample is sent to CDx Laboratories Inc. in New York for computer analysis and review by pathologists.4 The biopsy is minimally invasive and generally painless, so no topical or local anesthetic is required. Results can be faxed directly to the office as early as three days after the lab has received the sample.
The ViziLite test is also completed at chairside. The procedure is simple, noninvasive, and painless. The patient must rinse with a raspberry-flavored one percent acetic acid solution for one minute. The clinician can then activate the ViziLite capsule and assemble it with the ViziLite retractor to create the device used for the examination. The lights are dimmed and the examination of the suspicious lesion and the rest of the oral cavity are checked using the ViziLite device. Normal tissue will absorb the wavelength of illumination delivered from the ViziLite. Abnormal tissue will reflect back the light and allow it to stand out from surrounding tissue, making it easy to identify.
These tests are beneficial to both the dental provider and the patient. Oftentimes dental providers find a lesion that is somewhat questionable and they elect to watch it rather than biopsy it. The result is that when it is finally diagnosed, the tumor is more advanced. For patients, it provides a noninvasive, painless way to assure that a suspicious lesion is truly benign.
Paying attention to oral cancer is long overdue, and it is the responsibility of all dental health professionals to commit themselves and deliver the optimum in quality care. This means educating patients about the risk factors, prevention, self-examinations, and what to look for. Awareness increases one patient at a time, one day at a time.
Efforts have been made to increase the public's awareness, but more attention needs to be focused on getting the public to acknowledge the seriousness of this disease and how early detection can be imperative to their life. One excellent example is the early prevention and detection of breast cancer. For many years this was placed on the front line of cancer organizations. One of the major goals of the campaign was self-examination. Information was made readily available at doctor's offices, hospitals, clinics, school health centers, etc. Patients were taught how to properly conduct their own exam, then were sent home with illustrated pamphlets containing step-by-step instructions.
There is currently a national effort by multiple foundations, charities, and medical institutions to raise the awareness of oral head and neck cancer.9 The campaign includes weeks that have been designated for oral cancer awareness, and will include media coverage, free screenings, lectures, seminars, continuing-education courses, and other events. The "Oral Cancer Awareness Weeks" are:
• 2005 — April 4-10
• 2006 — April 17-23
• 2007 — April 16-22
• 2008 — April 7-13
• 2009 — April 13-19
• 2010 — April 12-18
This is a wonderful opportunity for hygienists to provide free screenings, show people how to conduct their own exam, and share informational booklets. Campaigns held by the American Dental Association, American Dental Hygienists' Association, or cancer foundations use billboards, taxi signs, and bus shelters to get the message out. Placing an emphasis on self-examinations will get more people involved with their health and increase early detection.
Diana Burnham, RDH, is a dental hygienist who is undergoing a degree completion program at the University of New Mexico.
References1 Horowitz A., Drury T., Goodman H., Yellowitz J. "Oral Pharyngeal Cancer Prevention and Early Detection" Journal of the American Dental Association 2000 April Vol. 131; pg. 453-462
2 Cruz G., Le Geros R., Ostroff J., Hay J., Kenigsberg H., Franklin M. "Oral Cancer Knowledge, Risk Factors and Characteristics of Subjects in a Large Oral Cancer Screening Program" Journal of the American Dental Association 2002 August Vol.133; pg.1064-1071
3 Meskin, Lawrence "One More Time" Journal of the American Dental Association 1999 July Vol.130; pg. 910-915
4 Gurenlian, JoAnn. "The Brush Biopsy: A Chairside Technique for Early Detection of Oral Cancer" Acess. The American Dental Hygiene Association 2003 Sept.-Oct. Vol. 17 (8): pg. 32-36
5 Oral Cancer Foundation "The Role of the Dental Profession" www.oralcancerfoundation.org
6 National Cancer Institute "Smokeless Tobacco and Cancer: Questions and Answers" May 2003 www.nci.nih.gov
7 National Center for Chronic Disease Prevention and Health Promotion "Chronic Disease Notes & Reports" Fall 2000 Volume 13(3)
8 Mayo Clinic Staff "Smokeless Tobacco: As Harmful As Cigarettes" Mayo Clinic www.mayoclinic.com
9 The Oral Cancer Foundation "Oral Cancer Related Events Calendar" www.oralcancerfoundation.org