The pandemic has made dry mouth products more important
Like so much in our lives, dry mouth has taken on a new complexity and urgency during the COVID-19 pandemic. The dental hygiene profession has been one of the foremost advocates for awareness of how dry mouth can decimate oral health. Ironically, dental professionals are now reporting symptoms of dehydration, including dry mouth, from wearing enhanced personal protective equipment (PPE). Many hygienists have also shared with me that they are seeing increased levels of dental disease in patients (including health-care professionals) since the onset of the pandemic.
This trend has many causes—increased access to decay-promoting foods while staying home, stress, medication, drug abuse, financial hardships, access to care issues, and so on, and the profession will not have peer-reviewed studies pinpointing the precise issues for some time. However, as clinicians in the trenches, dental professionals are currently faced with helping patients (and one another) navigate these new challenges and preventing an oral health disaster. The mouth is a complex ecological system, and changing one aspect—in this case, the amount of saliva present—can be disasterous.
First, a note on what exactly the term dry mouth syndrome means. Xerostomia is the patient’s perception of dry mouth, while hyposalivation is the pathological condition of decreased or absent saliva flow.1 It is also important to note that by the time a patient notices that his or her mouth is feeling dry, saliva flow may have already been reduced by as much as half.2
Stress
The salivary reflex is modulated by the central nervous system (CNS), and influenced by signals from other things happening within the CNS. Anxiety is the most well-known emotional state associated with hyposalivation.3 The circadian rhythm also influences the flow and composition of saliva.3
Sustained levels of high stress and loneliness are among the most heartbreaking aspects of the pandemic. The American Psychological Association (APA) says that “the negative mental health effects of the coronavirus will be serious and long-lasting.”4 In May, they found that the largest increases in pandemic-related stress were found among parents and people of color, although a universal increase in stress levels was found across geographic locations, political lines, and ages.4
Prescriptions for antidepressants have risen significantly during the pandemic,5 and in June, the Food and Drug Administration added sertraline (Zoloft) to its list of drugs experiencing shortages; the shortage is due to both increased demand and manufacturing difficulties caused by the pandemic.6 At press time, the drug was still listed as in shortage on the FDA website.
Dry mouth is a common side effect of antidepressants,7 although second-generation antidepressants have been shown to cause less severe dry mouth.8 Because patients are often lax in updating their health histories with dental clinicians, it is important to remind them that any drug they are taking can affect the oral cavity, even if they do not associate it with dentistry.
Anxiety is the most well-known state associated with hyposalivation . . . The American Psychological Association says that “the negative mental health effects of the coronavirus will be serious and long-lasting.”
Alcohol and drug use
Alcohol use has risen in the United States as a result of the pandemic and associated government measures.9 Alcohol is a diuretic and can increase dry mouth,10 and alcohol use can exert long-lasting influence on the brain. An April 2020 correspondence published in The Lancet Public Health stated that “stress is a prominent risk factor for the onset and maintenance of alcohol misuse. For example, chronic alcohol use results in neuroadaptations in stress and reward pathways . . . in turn, these neuroadaptations lead to increased cravings for alcohol in response to stress.”11 Put differently, alcohol changes the brain and increases the likelihood that a person will crave alcohol when stress is experienced in the future (in the case of the pandemic, the very, very near future).
Isolation and stress have also fueled an increase in opioid abuse, a crisis the United States was already facing. Factors related to a surge in opioid abuse include stress, social isolation (which increases the risk of relapse), cancellation of support meetings, and difficulty in obtaining substance use disorder care.12 Opioids, whether prescribed or not, also cause dry mouth.13
The pandemic has caused significant disruptions to diet and sleep, which are both important to overall saliva health. Dental health-care professionals are experiencing dehydration and dry mouth problems due to increased PPE use,14 but many clinicians are also reporting that prolonged mask wearing is also causing decay in the general population.
Fortunately, clinicians and patients do not have to accept dry mouth and decay as yet more collateral damage from the pandemic. There are many high-quality products available to help with dry mouth, but there are also many products on the market that can damage, rather than promote, oral health. To help understand how dental hygienists are recommending dry mouth products to patients, the RDH editors recently conducted an informal survey of approximately 380 dental hygienists on their practices for recommending dry mouth products.
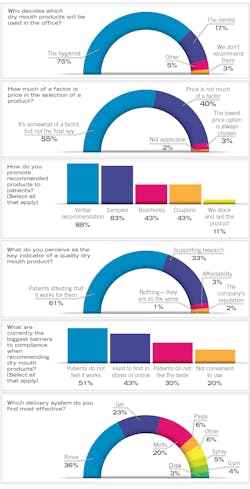
The vast majority of dental hygienists (92%) are discussing and making recommendations for dry mouth products, and 74% of respondents reported that hygienists are the ones deciding which dry mouth products will be used and recommended in the office. “The relative success of any product or protocol is very personal,” writes Anne Guignon, MPH, RDH, CSP, after many years of researching and writing about the topic.15 This was borne out in our survey results: 61% responded that the key indicator of a quality dry mouth product was patients attesting that it worked for them, with only 33% answering that supporting research was the most important. Fifty-one percent cited “patients do not feel it works” as the biggest barrier to compliance, with “hard to find in stores and online” (43%) and patients not liking the taste (30%) coming in after. Respondents most often selected Biotene, Xylimelts (Orahealth), and ACT as the top companies selling dry mouth products.
RDH will continue to publish more about the effects of the pandemic on oral health, and you can take advantage of the many articles about xerostomia in our web archives to learn more.
References
- Guignon AN. Treating dry mouth: What’s the point? RDH. July 1, 2018. Accessed August 12, 2020. https://www.rdhmag.com/patient-care/article/16408127/treating-dry-mouth-whats-the-point
- DiGangi P. Finding the right dry mouth fit. RDH. February 1, 2019. Accessed August 12, 2020. https://www.rdhmag.com/patient-care/xerostomia/article/16408893/finding-the-right-dry-mouth-fit
- Proctor GB. The physiology of salivary secretion. Periodontol 2000. 2016;70(1):11-25. doi:10.1111/prd.12116
American Psychological Association. Stress in America 2020. May 2020. Accessed August 12, 2020. https://www.apa.org/news/press/releases/stress/2020/report - Berger M. Shortages of antidepressant Zoloft reported in the midst of COVID-19 pandemic. Healthline. June 4, 2020. Accessed August 12, 2020. https://www.healthline.com/health-news/shortages-of-antidepressant-zoloft-reported-in-the-midst-of-covid-19-pandemic
- Drugmakers report Zoloft shortage amid COVID-19. FDAnews. June 3, 2020. Accessed August 12, 2020. https://www.fdanews.com/articles/197425-drugmakers-report-zoloft-shortage-amid-covid-19
- Antidepressants: Get tips to cope with side effects. Mayo Clinic. September 12, 2019. https://www.mayoclinic.org/diseases-conditions/depression/in-depth/antidepressants/art-20049305
- Cappetta K, Beyer C, Johnson JA, Bloch MH. Meta-analysis: Risk of dry mouth with second generation antidepressants. Prog Neuropsychopharmacol Biol Psychiatry. 2018;84(Pt A):282-293. doi:10.1016/j.pnpbp.2017.12.012
- Collins LM. Pandemic drinking shows alcohol misuse can be a problem at any age. Deseret News. July 12, 2020. https://www.deseret.com/indepth/2020/7/12/21317903/covid-19-pandemic-alcohol-drinking-addiction-alcohol-use-disorder-niaaa-george-koob-odyssey-house
- Dry mouth. Mayo Clinic. Accessed August 12, 2020. https://www.mayoclinic.org/diseases-conditions/dry-mouth/symptoms-causes/syc-20356048
Clay JM, Parker MO. Alcohol use and misuse during the COVID-19 pandemic: a potential public health crisis? Lancet Public Health. 2020;5(5):e259. doi:10.1016/S2468-2667(20)30088-8 - Weiner S. COVID-19 and the opioid crisis: When a pandemic and an epidemic collide. American Association of Medical Colleges. July 27, 2020. Accessed August 12, 2020. https://www.aamc.org/news-insights/covid-19-and-opioid-crisis-when-pandemic-and-epidemic-collide
- Safe use of long-acting opioids. University of Michigan Medicine. Accessed August 12, 2020. https://www.uofmhealth.org/health-library/abo7833
- Guignon AN. Respiratory PPE, dry mouth, and COVID-19: Why you need to know your own CAMBRA score. DentistryIQ. July 9, 2020. Accessed August 12, 2020. https://www.dentistryiq.com/dental-hygiene/infection-control/article/14179240/respiratory-ppe-dry-mouth-and-covid19-why-you-need-to-know-your-own-cambra-score
- Guignon AN. Evaluating a new dry mouth product system: Valuable insider experiences. RDH. July 1, 2020. Accessed August 12, 2020. https://www.rdhmag.com/patient-care/xerostomia/article/14179284/evaluating-a-new-dry-mouth-product-system-valuable-insider-experiences
About the Author
Amelia Williamson DeStefano, MA
Amelia Williamson DeStefano, MA, is group editorial director of the Endeavor Business Media Dental Group, where she leads the publication of high-quality content that empowers oral-health professionals to advance patient well-being, succeed in business, and cultivate professional joy and fulfillment. She holds a master's in English Literature from the University of Tulsa and has worked in dental media since 2015.
Updated May 16, 2023