How food insecurity affects families: What can be done and who can help
The United States is often considered the “greatest country in the world.” However, is it really when millions of Americans are food insecure? The US Department of Agriculture (USDA) reports that 11% of all households and 13% of households with children experience food insecurity.1 One in seven, or 11 million, children in America live in households without consistent access to adequate food.2
Being food insecure means more than not having enough money to buy food. In fact, there are two levels of food insecurity: low and very low. Low food insecurity is recognized as having a reduced quality, variety, or desirability of diet, while having little or no indication of reduced food intake.1 Very low food insecurity involves disrupted eating patterns and reduced food intake.
You might also be interested in ...
Fluoride and sealants: How these preventive tools are helping our pediatric patients
Examples of Americans having low or very low food insecurity could include unemployed individuals,3 those with health or mobility issues, elderly,4 single-parent5 and single-income households, and homeless populations.6 But don’t be fooled—there are many Americans in affluent areas who experience food insecurity. Each scenario could have been food secure, and one simple event, such as a global pandemic, could have been the tipping point to becoming food insecure.
Low food insecurity
Let’s break down “having a reduced quality, variety, or desirability of diet, while having little or no indication of reduced food intake.” In this case, families may have monetary resources, Supplemental Nutrition Assistance Program (SNAP), or Women, Infants, and Children (WIC) benefits, but they are unable to obtain foods that are considered nutrient rich and support an active, healthy lifestyle, which is the goal of the USDA.7
Often, decisions must be made to purchase lower-quality foods to ensure sustainability throughout a paycheck cycle. As well, some families may be without reliable transportation, which limits their ability to reach lower priced “big box” stores which allow for stretching food budgets and acquiring more nutritious food options. These families may only have a neighborhood market option, which offers limited nutritious inventory. In fact, most times, these scenarios offer many processed foods, which should be some of the last options consumed due to the increased risks they pose of obesity, diabetes, dental caries, and periodontal conditions.4
Very low food insecurity
It is critical to understand disrupted eating patterns and reduced food intake when analyzing very low food insecurity. A disrupted eating pattern means that families may not be able to consume breakfast, lunch, and dinner, let alone choose nutritious food options to support the healthy, active lifestyle recommended by the USDA.7 It’s often a challenge to have access to food in general, which equates to reduced food intake.
Because research indicates the need for a nutrient-rich diet to achieve optimum health, families with very low food insecurity may likely also have higher risks for sickness and disease.4 When faced with these roadblocks to a healthy, active lifestyle, individuals, especially children, could face a cascade of life’s turmoils—e.g., decreased attendance at work or school,6 equating to reduced pay and fewer days of learning,6 which can stunt upward mobility in society. When individuals experience these situations, they are usually consistently working to “dig themselves” out of ruts that are difficult to maneuver.
Dental effects from food insecurity
Considering that early childhood caries (ECC) is the most common chronic disease among youth in the US, it is crucial that dental professionals investigate food security when offering nutritional counseling. More than 45% of American children between the ages of 2 and 19 experience tooth decay in their primary or permanent dentition.8 Food insecurity affects these outcomes on many levels: increased processed food/drink intake, decreased vitamin/mineral consumption (calcium, vitamin D, and fluoride), decreased access to nutritious foods, socioeconomic status, awareness, and infant/toddler feeding scenarios.4 Periodontal outcomes can likewise be affected by similar circumstances. Additions could involve deficiencies in protein, vitamin C, and zinc.4
Effects from the global pandemic
The COVID-19 global pandemic affected food security in incredible ways. A study of more than 3,200 respondents conducted in Vermont early in the pandemic suggested that respondents experiencing a job loss were at higher odds of experiencing food insecurity due to the effects of the pandemic. Some statistics from the study indicated new food insecurities, in addition to increased food insecurities of those who were previously food insecure, and two-thirds of responding households in Vermont with food insecurity during COVID-19 were already eating less to stretch their food.3 Note: While this research focuses on Vermont, it is safe to speculate many, if not all, states experienced similar issues.
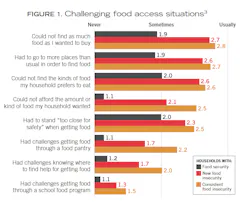
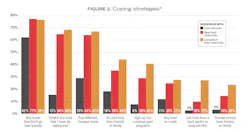
Every aspect of food insecurity was affected by the pandemic: economic, physical access, availability, utilization, and stability. Figure 1 indicates limited food budgets, safety standing near others (in the earliest times of the pandemic), and access to food were a few of the issues respondents experienced. Some of the coping strategies (figure 2) respondents enacted were stretching food to last longer, choosing more long-lasting food sources, buying cheaper foods, and borrowing money and receiving food from friends and family.3
The study’s results indicated that more research was needed. Increasing funding for food programs, expanding food pantries and mobile pantry services, increasing access to fruit/vegetable programs, preparing for national and global emergencies (from an access-to-food perspective), and removing stigmas associated with use of government programs would help lessen the effect of another challenging situation, especially for those new to food insecurity.3
Who can help?
As health-care professionals, we need to know about a variety of outreach programs and resources available to those who are experiencing food insecurity on any level. Pediatric primary care screenings within private practice or community health centers can be an incredible resource to point parents in the right direction. These health-care professionals can offer referrals, such as SNAP benefits and WIC,1 which can get the ball rolling. Mediating institutions such as religious communities, educational communities, and nonprofit organizations can also bridge gaps9 that are not being met via paychecks, SNAP, and WIC benefits.
Religious communities may house food pantries and soup kitchens,9 as well as youth programs that may offer meals or snacks. Educational communities have offered free and reduced-cost breakfasts/lunches for years to families who qualify.9 The state of Colorado recently voted (55% in favor) to offer free meal programs for all students! They are joining California and Maine, two states that have already been following this path.10 A large variety of food security nonprofits are available across the nation—the Hunger Project, Feeding America, and Feed the Children, to name a few. Check the internet for more suggestions.
Conclusion
Food insecurity is not new and should not have to be a constant in the US or across the globe, but unfortunately it is. No matter the economy, there will always be people in need of sustenance due to circumstance—job loss, health matters, lack of resources and education, broken homes/families, single-income families … you name it; it can affect outcomes. Health-care professionals tend to have knowledge about available resources, which may assist those in need. If they don’t, it’s likely they know someone who can help. Advocacy for patients in this arena can most definitely affect oral health outcomes. Creating awareness of food insecurity is a crucial first step in offering guidance to families.
Editor's note: This article appeared in the March 2023 print edition of RDH magazine. Dental hygienists in North America are eligible for a complimentary print subscription. Sign up here.
References
- Banks AR, Bell BA, Ngendahimana D, Embaye M, Freedman DA, Chisolm DJ. Identification of factors related to food insecurity and the implications for social determinants of health screenings. BMC Public Health. 2021;21(1):1410. doi:10.1186/s12889-021-11465-6
- School meal statistics. School Nutrition Association. https://schoolnutrition.org/about-school-meals/school-meal-statistics/
- Niles MT, Bertmann F, Belarmino EH, Wentworth T, Biehl E, Neff R. The early food security impacts of COVID-19. Nutrients. 2020;12(7):2096. doi:10.3390/nu12072096
- Sroda R, Reinhard T. Nutrition for Dental Health: A Guide for the Dental Professional, Enhanced Edition. 3rd ed. Jones & Bartlett Learning; 2018.
- National Single Parent Day: March 21, 2022. United States Census Bureau. March 21, 2022. Accessed October 6, 2022. https://www.census.gov/newsroom/stories/single-parent-day.html
- The facts. Stop Child Homelessness. Accessed October 6, 2022. https://stopchildhomelessness.org/the-facts/
- Zhang J, Wang Y, Yen ST. Does supplemental nutrition assistance program reduce food insecurity among households with children? Evidence from the current population survey. Int J Environ Res Public Health. 2021;18(6):3178. doi:3390/ijerph18063178
- Something to smile about: a Children’s Dental Health Month guide. American Dental Hygienists’ Association. 2021. https://www.adha.org/resources-docs/ncdhm/NCDHM_Guide_2021.pdf
- Klimon WM. Mediating institutions. Religion & Liberty. 2010;2(3).
- Prothero A. Colorado voters say yes to universal free school meals. Will other states follow? Education Week. November 9, 2022. https://www.edweek.org/policy-politics/colorado-voters-say-yes-to-universal-school-meals-will-other-states-follow/2022/11
About the Author
Angela Grover, MA, BASDH, RDH
Angela Grover, MA, BSDH, RDH, graduated from Central Community College in 1996, obtained her BASDH from the Community College of Denver in 2018, and received her MA in organizational leadership from Buena Vista University in 2022. She is the founder of 360 Dental Navigations, which utilizes her expertise to create unique content for dental presentations and published articles for the dental industry. Angela is a webinar professional educator for Water Pik in the central time zone. Contact her at [email protected].
Updated January 20, 2022