Helping dental patients quit tobacco through interprofessional collaboration
As dental hygienists, we see patients as often as three to four times per year. According to the Canadian Dental Hygienists Association (CDHA), hygienists see a larger client population than other medical professionals. Some of our patients see us more often than their family physician. As disease prevention specialists, we have skills in health promotion, disease prevention, health education, and behavioral motivation that allow us to provide effective tobacco cessation counseling. Since we have a high frequency of interaction with our patients, we’re able to deliver tobacco cessation support with repeated reinforcement, which is essential for all tobacco users.1
However, delivering tobacco cessation in a clinical setting is easier said than done. Of the 340 dental hygienists surveyed in 1996, 35% stated that patient resistance was a significant barrier when trying to deliver tobacco cessation. Twenty-nine percent of hygienists felt adequately trained to deliver tobacco cessation, but 26% felt that lack of time was a barrier.2
The 5 As to help patients quit
To deliver motivation in the dental setting, use these 5 As to help patients quit:
- Ask about use, history, and smoking habits
- Advise about health risks and encourage quitting
- Assess willingness to quit status
- Assist in creating an action plan
- Arrange follow-up care
The 5 Rs to increase motivation to quit
In conjunction with the 5 As, use these 5 Rs to increase patients’ motivation
to quit:
- Relevance: Quitting is personally relevant
- Risks: Negative consequences of smoking
- Rewards: Benefits of smoking cessation
- Roadblocks: Identify barriers to quitting
- Repetition: Repeat every time during a patient’s visit
Interprofessional collaborative care offers clinicians the opportunity to engage patients in tobacco cessation treatment that is coordinated and comprehensive. Hygienists are well-trained to get the process started and remain engaged with patients as they move toward better health.
You may also be interested in ... White lesions of the oral cavity and oral-systemic health: A review for the dental hygienist
Clients will be more likely to entertain smoking cessation, or reduce harm, when engaging with a health professional who they perceive as empathetic and nonjudgmental. As you build a trusting rapport with clients, the conversation becomes easier. Repetition over time is key to keep the conversation going.
The 3-legged stool of addiction
Tobacco addiction is much like a three-legged stool with the legs being addiction, psychological dependence, and behavior. Recognizing the stage of change your patient is in will help guide a meaningful conversation.
- Addiction: Nicotine addiction is the physical dependence involved even if the person wants to quit. Addiction leads to physical withdrawal symptoms.
- Psychological dependence: The “feel good” addiction/dependence of nicotine works on the dopamine receptors in the brain. For example, even if the patient thinks nicotine “lowers my stress,” it physically raises blood pressure and increases the stress response.
- Behavior: Refers to the habitual part of smoking. For example, the patient may brew coffee and then light a cigarette automatically.
The behavioral change process
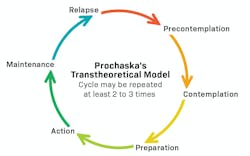
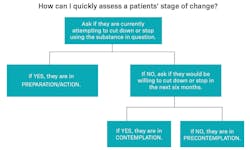
Encompassing the 5 As and 5 Rs into a three- to five-minute interaction, we can break it down by behavioral stage (figure 1) and assess patients’ stage of change (figure 2):
Precontemplation: Denial of the problem—the cons to change outweigh the pros for change. The client may say, “Yes, but …” or may express anger when the subject of cessation is raised. Ask how the patient feels about their smoking or say, “Help me understand why you feel that way.” Depending on the patient’s reaction, stopping the conversation until next time may be best.
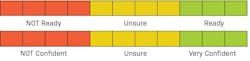
Contemplation: Some ambivalence/low confidence for change—the pros equal the cons. Using the readiness ruler (figure 3) as a guide, inquire how ready and confident the patient is to make the change. Anything above a 7 on the ruler means the patient is ready to discuss further. Say, “On a scale of 10, where 0 means you aren’t ready and 10 means you’re very ready, how ready are you to make a change today to quit smoking?” Using the same scale say, “How confident are you that you can quit?” At this stage, build on the pros for change. Inquire what would make your patient shift higher on the readiness scale. Ask if they would like to learn more about treatment options.
Preparation/action: The pros outweigh the cons, so the patient is getting ready to change. Define the obstacles and find strategies that will help the patient take action. Use the readiness scale strategy, but now you can help arrange access to care and/or delve deeper into how to use nicotine replacement products, depending on your comfort/knowledge level.
Interdisciplinary collaboration
Tobacco addiction can be complex. While some patients will be able to self-manage with nicotine replacement therapy products (NRTs), most require ongoing counseling and support. Collaboration between health-care providers is a key to success. Patients may be more open to discussion with a different professional rather than their family physician.
You may also be interested in ... Vaping and oral health: Unveiling the hidden risks
Collaboration can be direct communication with the patient’s primary care practitioner, or it can involve building relationships with other tobacco cessation professionals to help you know when and where to refer.
In Ontario, Canada, we have several options to collaborate, including but not limited to:
- Ask a direct peer.
- Contact your local public health unit and ask about local support programs.
- Enroll patients at the Centre for Addiction and Mental Health (CAMH). CAMH offers the STOP program (Smoking Treatment for Ontario Patients). Patients are enrolled for one year, during which they receive counseling and up to six months of free NRT products. This program is offered through some hospital outpatient programs, primary care, and pharmacies.
- Seek online support from CAMH through their Quit Smoking with STOP and nicotine dependence services
We work with patients who have complex medical histories, and they often present with risk factors that require an interdisciplinary approach. Collaboration between the dental team and other members of the interprofessional team can help increase patient awareness about oral health and its effects on overall systemic health.
Editor's note: This article appeared in the January/February 2024 print edition of RDH magazine. Dental hygienists in North America are eligible for a complimentary print subscription. Sign up here.
References
- Tobacco use cessation services and the role of the dental hygienist — a CDHA position paper. Canadian Dental Hygienists Association. Accessed September 28, 2023. https://www.cdha.ca/pdfs/Profession/Resources/1004_tobacco.pdf
- Monson AL. Barriers to tobacco cessation counseling and effectiveness of training. American Dental Hygienists’ Association. Accessed September 28, 2023. https://jdh.adha.org/content/jdenthyg/78/3/5.full.pdf
- Fundamentals of addiction: motivation and change. Influencing motivation to change. The importance of assessing motivation to change. Centre for Addiction and Mental Health (CAMH). Accessed October 9, 2023. https://www.camh.ca/en/professionals/treating-conditions-and-disorders/fundamentals-of-addiction/f-of-addiction---motivation-and-change
Fatima Foster, RRT, CRE, has 30 years of experience as a registered respiratory therapist and certified respiratory educator. She implemented the STOP program at the Firestone Institute for Respiratory Health, St. Joseph’s Healthcare Hamilton, Ontario, Canada. She currently works for Asthma Research Group Inc. (ARGI) Best Care, where she provides education and case management support in primary care.
Whitney Foster, RDH, has worked in various roles in the dental field. With a passion for oral health care and its relationship to overall health, She strives to support and mentor fellow dental hygienists on the subject. Whitney is currently creating a continuing education course that will focus on interprofessional collaboration.
About the Author

Fatima Foster, RRT, CRE
Fatima Foster, RRT, CRE, has 30 years of experience as a registered respiratory therapist and a certified respiratory educator. She implemented the STOP program at the Firestone Institute for Respiratory Health, St. Joseph’s Healthcare Hamilton, Ontario, Canada. She currently works for Asthma Research Group Inc. (ARGI) Best Care, where she provides education and case management support in primary care.
Updated December 13, 2023

Whitney Foster, RDH
Whitney Foster, RDH, has a demonstrated history of working in various roles in the dental field. In the last year, Whitney has been published in various publications within the industry and developed a continuing educational course that focused on interprofessional collaboration. With her passion for oral health care and the relationship to overall health, Whitney continues to support, mentor, and advocate on the subject for fellow dental hygienists.