Heberden's Nodes: Chronic arthritic disease can impact oral health
By NANCY W. BURKHART, BSDH, EdD
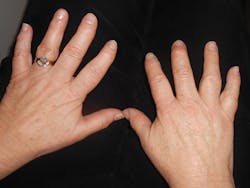
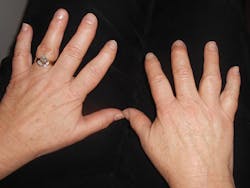
The patient that you are seeing today is a patient that you have treated for a number of years. She is 62 years old and in good health. Angie usually has very little plaque, virtually no calculus, and she is a very conscientious patient. As you begin your assessment, you ask her about any changes in her health or dental status. She tells you that she has an appointment with an orthopedic specialist to evaluate some nodules that she has noticed on her fingers and proceeds to show you the largest growth on her right hand.
Angie asks for your opinion about the etiology (see Figures 1). As a dental professional, it is rare that a patient will ask about any problems with the hands, and you are unsure about what the nodules may indicate. Since you have not seen these before in a patient that you have treated, you are unsure exactly how to respond. Have you heard of Heberden's nodes?
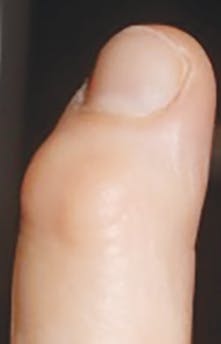
Etiology: Heberden's nodes are small, pea-sized areas of exostosis or bony outgrowths that are seen in the joints closest to the tip of the fingers. When the middle joint is affected, the nodes are referred to as Bouchard's nodes. The nodes are an indication of a destruction of the cartilage covering the surfaces of bones in the synovial joints. Segments of bone or cartilage break off and float around the joints (DeLong & Burkhart, 2013). These nodes are found in patients with osteoarthritis (sometimes referred to as degenerative arthritis or OA) and also in rheumatoid arthritis.
Rheumatoid arthritis affects many systems in the body and is much more serious. However, both are considered multifactorial degenerative disease processes. Both genetic and environmental factors are associated with OA.
Trauma is primarily associated with osteoarthritis and the development of Heberden's nodes. The Arthritis Foundation also reports that there may be a rare defect in the body's production of collagen, the protein that makes up cartilage. Some individuals may have the misfortune to have slight defects in the bone and the way that the bones fit together.
Epidemiology: Osteoarthritis is the most common type of arthritis. Approximately 27 million Americans are affected with OA and are usually over the age of 65 years old. However, younger individuals can be affected as well. According to the Arthritis Foundation, one in two adults will develop OA of the knees and one in four will develop symptoms of hip OA by age 85. One in 12 people over 60 years old have hand OA.
Courtesy of Carol Perkins, RDH
In general, there are over 100 types of arthritis and related conditions. It is the leading cause of disability in America. More than 50 million adults and 300,000 children have some type of arthritis.
Pathogenesis: Trauma is the prime cause of OA with cumulative wear of the joints over time. With osteoarthritis, destruction of cartilage covering the articular surfaces of bones in synovial joints may result in the opposing bones rubbing against each other when significant cartilage is lost. This is especially seen in the knees and hips causing limiting of motion with pain and inflammation. The spine and the lower lumbar regions may be affected as well.
With advancing age, the replacement of chondrocytes and chondroblasts in joints is slowed, and there is much less turnover. The fibers work longer and become susceptible to fatigue (Neville, 1995).
Excess fat produces inflammatory chemicals (cytokines) that promote inflammation and joint damage. Patients may complain of stiffness, swelling, and limited range of motion. Pain and "cracking" of joints is also often reported. Bone spurs and crystals as in Heberden's nodes occur with OA.
Intraoral characteristics: The TMJ may suffer damage and destruction of cartilage as well. Asking patient about crepitus, deviation, deflection, and limitations on opening is suggested. The patient may have other indications of osteoarthritis but may not have perceived the connection with the Heberden's nodes.
Diagnosis: The joints such as the knees, fingers, and hips are usually assessed through radiographs or magnetic resonance imaging (MRI). The cartilage is assessed, and the physician will look for "bone spurs" or evidence of crystals and joint deterioration. A thorough health history is taken to determine risk factors, previous injury, and lifestyle. Rheumatoid arthritis may have some similar traits but, of course, is a far more serious disorder involving the immune system.
Treatment: In severe cases, rehabilitation may be needed with surgery and NSAIDs to reduce inflammation. Sodium hyaluronate is used as a lubricant and is injected directly into the joint areas. This mimics the synovial fluid that has been lost. Treatment includes a clear diagnosis by an orthopedic specialist, rheumatologist, or someone knowledgeable in the skeletal system and bone disorders. Recommendations to limit the effects and lessen the destruction of joint damage have been suggested (see related sidebar).
Dental implications: In severe osteoarthritis, the cartilage destruction may make holding a toothbrush or dental floss difficult. With more severe cases, the brush may need modification, and flossing may be more time consuming or difficult. Special flossing devices may assist the patient and more frequent appointments may be necessary. The TMJ may be affected in both osteoarthritis and in rheumatoid arthritis, limiting opening and mobility of the jaw.
Oral medicine: We often treat patients who have signs of an array of systemic disease processes that may be overlooked unless the clinician is paying close attention to the patient. Patients come in at various times of the year and may be clothed from head to toe depending upon the season. Many times skin surfaces are not visible. At other times, we may notice lesions, nodules, skin patches, and discolorations. Sometimes this may indicate a skin cancer, early signs of systemic diseases, or the development of a chronic type of disease such as osteoarthritis. Early intervention does make a difference.
We may see a patient more often than any other clinician and referrals to a physician may be indicated more often than we realize. Providing patient education is needed to assist patients in preventing chronic disease. Paying attention to all visible areas on the body and a careful health history review is always warranted. This concept is part of a total wellness concept in the dental office.
It is well documented that we have an obesity problem in the United States. With obesity, we continue to see chronic disease states at an increasing level. Many of these chronic issues are occurring at younger ages and will expand with time. Although we do not know all the causes of osteoarthritis, we do know that the loss of one pound of body fat can reduce the joint pressure of the knees by four pounds and the hips by up to six pounds.
Arthritis is the leading cause of disability in America. As osteoarthritis increases in the population, limited activity may occur as well, and this places the patient at a higher risk for other diseases such as diabetes. Patients with osteoarthritis are also more likely to fall and have fractures.
This is a real issue of concern for the elderly population since hip fractures significantly decrease longevity in this population. With the increase in knee and hip replacement being on the rise in the United States, a substantial shift in wellness needs to occur. Hygienists and dentists are in a perfect position as health-care providers to assist patients in maintaining healthy lifestyles. Remember, you really do have a captive audience!
As always, keep asking good questions and continue to listen to your patients. RDH
What are the risk factors for osteoarthritis?
- Females are more affected than males.
- Increasing age. At the age of 75, most men and women show some signs of osteoarthritis even in milder forms. This is usually due to wear on the joints with years of use.
- Trauma or injury to the joints.
- Genetic risk factors: Osteoarthritis tends to run in families.
- Obesity. The loss of just one pound of extra weight will decrease pressure on the knees by four pounds, and hip pressure by six pounds.
- Diabetes: High glucose levels speed the formation of molecules that make the cartilage stiffer. Diabetes triggers total body inflammation.
- Repetitive use of a body part. For example, the fingers used repetitively in computer keyboards or multiple sports injuries that occur over time.
Recommendations to limit osteoarthritis:
- Exercise-Development of muscles in the legs. Increase strength training to develop all muscles in the body. If possible, a personal trainer is very helpful to begin an exercise routine and the recommendation of specific exercises.
- Lose weight-The loss of just one pound of body weight decreases pressure in the knee joint by four pounds and a decrease of six pounds in the hips.
- Limit inflammation in the body-A Mediterranean diet is known to limit inflammation and is recommended by many physicians.
- Acetaminophen relieves pain; NSAIDs target inflammation and pain. These are used by patients when needed for pain. Medications may be discontinued or decreased when weight loss and strength training are successful in many cases.
- Hyaluronic acid injections are alternatives to surgery and work well for many patients.
- Ice packs when needed for soreness or pain.
- Walking, swimming (especially water aerobics), and yoga keep joints limber.
References
1. Arthritis Foundation http://www.arthritis.org/about-arthritis/types/osteoarthritis/symptoms.php
2. http://www.arthritis.org/about-arthritis/types/osteoarthritis/what-is-osteoarthritis.php
3. Delong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. 2nd ed. Wolters Kluwer: Lippincott, Williams & Wilkins, Baltimore 2013.
4. Neville B, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. WB Saunders Co. Philadelphia 1995.
5. Web MD http://www.webmd.com/osteoarthritis/news/20050629/small-weight-loss-takes-pressure-off-knee
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics/stomatology, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was awarded a 2016 American Academy of Oral Medicine Affiliate Fellowship (AAOMAF). She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. She can be contacted at [email protected].